Fig. 22.1
Anatomy of the nasal valve
22.3.1.2 What Is the External Nasal Valve?
The “external nasal valve” is located in the nasal vestibule, and it is an area bound by the alar rim and columella, including the medial crus, nasal spine, and soft tissues covering the nasal sill and floor. As with the internal nasal valve, the external valve either may be narrowed at rest (i.e., vestibular stenosis) or may have a floppy and weak lateral component (i.e., alar rim) which narrows under the influence of negative pressure associated with nasal inspiration (Constantian 1994).
22.3.1.3 Influences on Nasal Valve Strength
22.3.2 Internal Nasal Valve Collapse
22.3.2.1 Static Internal Valve Compromise
Internal nasal valve collapse may be categorized as static or dynamic (Apaydin 2011; Park 1998). Static internal nasal valve collapse is a narrowing of the middle third of the nose at rest – that is, the angle between the upper lateral cartilage and nasal septum is anatomically small and the resultant area of the valve is similarly reduced. Static collapse is often seen as a result of nasal trauma or previous rhinoplasty in which a weakening of nasal support structures leads to an overly narrowed angle between the upper lateral cartilage and nasal septum (i.e., this may result from simple surgical maneuvers such as skin elevation, mucosal elevation, separation of the upper lateral cartilages from the septum). Static internal valve collapse may also result from scarring of the medial segment of the upper lateral cartilage to the nasal septum following the separation of those structures along with their intervening mucosa. Elevation of the skin-soft tissue envelope, damage to the nasal dilator muscles, and weakening of the mucosal support of the middle third cartilages all contribute to a weakening of nasal valve support.
22.3.2.2 Identifying Static Internal Valve Compromise
Middle third narrowing at rest, that is, static internal nasal valve collapse, may be seen upon simple external inspection of the nose in which a pinched middle third may be visible. This often results in a discontinuity along the brow-tip aesthetic line as the middle third is pinched and narrowed, while the upper third, which is supported by bone, remains wide. Classically, the inverted V deformity has been linked to the separation of the upper lateral cartilages from the overlying nasal bones during rhinoplasty, but it is actually seen more commonly either in patients with internal nasal valve collapse who have never undergone previous rhinoplasty or in patients who have had a standard dorsal reduction rhinoplasty without disarticulation of the upper lateral cartilages from the nasal bones (Fig. 22.2). Static internal nasal valve collapse may appear clinically as scar tissue, strictures, or webbing in the valve angle (as might occur after separation of the upper lateral cartilage and mucosa from the septum without sparing the mucosal attachments between the two structures). Congenital or traumatic weakness or absence of the upper lateral cartilages or other deformities (thickening, twisting) of the upper lateral cartilages may result in static narrowing of the middle third of the nose. Additionally, in patients with an overprojected tension-type nasal deformity, overgrowth of the nasal septum causes the angle between the upper lateral cartilage and the nasal septum to be excessively narrowed. Such patients may also frequently be found to have thin and weak upper lateral cartilages, which tend to add a dynamic component to the internal nasal valve collapse.
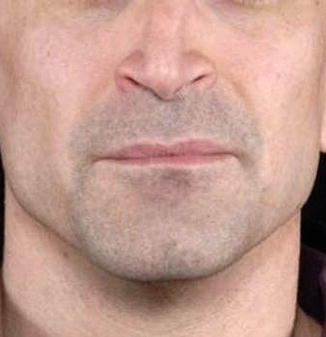

Fig. 22.2
Static internal nasal valve collapse visible in the middle third of the nose
22.3.2.3 Dynamic Internal Nasal Valve Compromise
Dynamic internal nasal valve collapse is an active narrowing of the upper lateral cartilage and middle third of the nose which occurs only with nasal inspiration through a valve which, at rest, appears of normal size (Fig. 22.3a–d). Dynamic nasal valve collapse, in which the middle nasal third appears normal at rest but narrowed upon gentle nasal inspiration, often results from an inherent weakness of the nasal sidewalls (Fig. 22.4). Thin, weak, detached, or absent upper lateral cartilages cannot provide the necessary strength along the nasal sidewall to withstand the negative pressures created by inspiratory nasal airflow – as a result, the sidewalls of the nose fall in as the negative pressure created by nasal inspiration draws them inward. Previous rhinoplasty in which the upper lateral cartilages have been weakened or detached from the nasal septum, congenitally or developmentally thin upper lateral cartilages, and absent upper lateral cartilages may all contribute to such structural weaknesses of the nasal sidewall. In such cases, the patient may not have obvious findings suggestive of nasal valve collapse upon inspection at rest, such as an inverted V deformity or a pinched middle third, but when asked to inspire gently through the nose, there is an active narrowing of the middle third which becomes obvious to the examining physician. In order to appreciate dynamic nasal valve collapse and its effects on nasal breathing, it is often helpful for the examining physician to apply gentle lateral traction on the cheek adjacent to the nose (i.e., Cottle maneuver) to assess for improvements in nasal breathing that might occur with stiffening of the lateral nasal wall by digital traction. Additionally, in order to pinpoint the precise location of the collapse, it is helpful to introduce a cotton tip applicator or ear curette into the suspected area of collapse and observe improvements in nasal obstructive symptoms when the precise site of obstruction is stiffened with the examiner’s help. Application of external nasal dilation devices further helps identify internal nasal valve collapse.
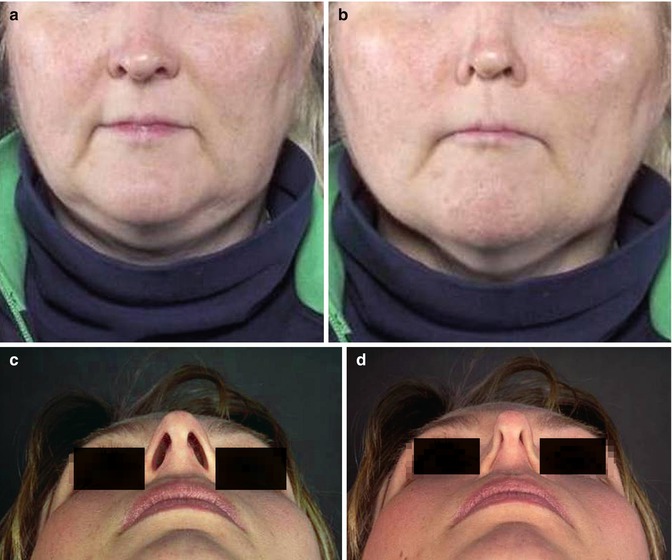
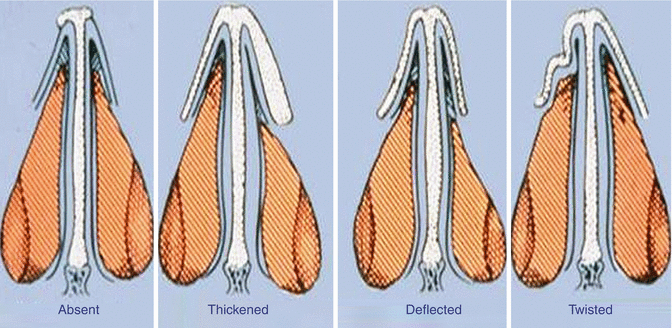

Fig. 22.3
(a, b) Dynamic internal nasal valve collapse. The nasal sidewalls collapse inward under the force of negative inspiratory pressure. (c, d) Dynamic external nasal valve collapse on gentle nasal inspiration

Fig. 22.4
Variability of inherent structure of upper lateral cartilage
22.3.3 External Nasal Valve Collapse
The external nasal valve is an area primarily supported by the lower lateral cartilages and their overlying skin and soft tissue covering and is defined anatomically by the region between the columella and the alar rim. The size, shape, and strength of the lower lateral cartilages create the nasal vestibular aperture that defines the external nasal valve. Static narrowing of the external nasal valve (vestibular scarring and stenosis, alar rim collapse) may be seen with trauma, soft tissue triangle injury, reconstruction of nasal skin cancer defects, cleft lip repair, alar base narrowing procedures, significant caudal nasal septal deformities in Cottle area 1, or secondary to a variety of other causes. Functionally unfavorably shaped lower lateral cartilages may narrow the external nasal valve aperture and contribute to nasal obstruction simply due to the shape of the cartilages (concave lower lateral cartilages that impinge on the airway, lateral crural cephalic malposition with resultant concavity along alar rim, etc.). For example, in the case of tension-type nasal deformities in which the vestibular aperture at the level of the nasal rim is narrowed and pinched, we see the shape of the lower lateral cartilage affecting the size of the nasal vestibule – a tent-pole-like overprojection of the tip results in a narrow nasal vestibule secondary to “slit-like nostrils.”
Dynamic external nasal valve collapse occurs when the valve appears normal at rest, but upon inspiration through the nose, there is collapse of the alar rims. Primary weakness of the lower lateral cartilage and malposition of the lower lateral cartilage (as with vertically oriented lower lateral cartilages) often lead to dynamic external valve collapse – in both situations, the lower lateral cartilage malposition and inadequate soft tissue support at the rim lead to an inability to support or withstand the negative inspiratory forces generated by nasal breathing. In examining a patient with external valve collapse, it is best to simply observe the nose during quiet breathing and watch the nasal vestibule for narrowing of the alar rim on gentle nasal inspiration. As with internal valve collapse, application of lateral traction with the examiner’s hand, a cotton applicator or wax curette, or with an external nasal dilator will help to identify the precise area of weakness and may further help demonstrate to the patient what may be achieved with surgical correction of the external nasal valve weakness.
22.3.4 The Aging Nose
A common and increasingly more prevalent clinical scenario in which we find nasal obstruction associated with both internal and external nasal valve collapse is in the aging patient. The aging nose undergoes structural changes that result in various weaknesses that lead to nasal valve collapse and nasal obstruction. A significant loss of nasal support occurs with thinning of the nasal bones and skin, thinning and weakening of the upper lateral cartilages, laxity in the supportive attachments between the upper and lower lateral cartilages at the scroll region, weakening of the lower lateral cartilages, and laxity in the supportive fibrous attachments between the lower lateral cartilages and the nasal septum and maxilla. Additionally, just as in the rest of the body, the nasal muscles likely atrophy with age, which may add to the collapsibility of the nasal sidewall. The structural changes associated with aging contribute to the drooping of the nasal tip (tip ptosis), narrowing and weakening of the internal valve, and narrowing and weakening of the external nasal valve – all of which contribute to both functional breathing problems as well as to the aesthetic changes that are typical of the aging nose. As we face a global aging of the population, nasal surgeons around the world will likely see increasing numbers of patients for surgical correction of nasal breathing (Toriumi 1996; Guyuron 1997; Rohrich and Hollier 1999).
22.4 Treatment
Over the past 10–15 years, there has been an increased awareness of the nasal valve as a contributor to nasal airway obstruction, resulting in a flurry of scientific publications on the matter, innovations in therapeutic options, and increasing applications of a multitude of both surgical and nonsurgical treatments to correct the nasal valve contribution to nasal obstruction (Park 1998; Kern 1978; Gassner et al. 2006; Friedman et al. 2004; Paniello 1996; Akcam et al. 2004; Vaiman et al. 2005; Guyuron et al. 1998; Toriumi et al. 1997; Sen and Iscen 2007; Mendelsohn and Golchin 2006; Ng et al. 1998; Sheen 1984; Clark and Cook 2002; Stucker et al. 2002; Stucker and Hoasjoe 1994; Menger 2006; Rohrich et al. 2002; Andre et al. 2006; Byrd et al. 2007). Evaluation of the patient begins with a thorough history, eliciting signs that may hint at nasal obstruction and nasal valve collapse. Does the patient mouth breathe, snore, awaken tired? Has the patient used breathing dilator devices in the past or had prior nasal surgery? The answers to these questions will help guide the patient and surgeon in deciding whether there is a nasal valve component to the nasal obstruction and whether nasal surgery might be of benefit.
Many of the surgical techniques that have been described for nasal valve repair have focused on secondary nasal surgery to improve nasal function following rhinoplasty (Sheen 1984; Clark and Cook 2002; Stucker et al. 2002; Stucker and Hoasjoe 1994). Armed with a better understanding of the nasal valve, recent refinements in surgical techniques, and an accompanying thorough preoperative evaluation, findings of internal and/or external nasal valve collapse may often be identified in previously unoperated individuals who complain of nasal obstruction. Such patients often have improvements in nasal breathing with the Cottle maneuver or with the application of external nasal dilator devices. Treating the patient with nasal breathing devices at home allows the patient to experience the quality of life improvements associated with correction of nasal valve obstruction. In this way, it helps to communicate to the patient what they might expect from surgical nasal valve intervention. Patients are then better able to make informed decisions about the desirability of surgical intervention for nasal valve obstruction. Additionally, the application of such breathing devices helps in defining the site of obstruction more precisely in order to optimize surgical outcomes (Gruber et al. 2011). Primary and secondary functional nasal surgery with correction of the dysfunctional nasal valve has been previously shown to significantly improve quality of life in patients complaining of nasal obstruction who have preoperative findings of nasal valve collapse (Rhee et al. 2005; Younes et al. 2006; Most 2006).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


