Fig. 18.1
The concept of a “tetrapartite” gliapse modulating synaptic strength based on the anatomical relationships between astrocytes, glia and neurons has superseded the previous synaptic model
18.3 Migraine/Chronic Tension Headache
Current migraine theory centres on sensory processing dysfunction of the brain stem or diencephalic nuclei. Neural events in the brain stem result in ensuing dilation of blood vessels, which in turn results in pain and further neural activation (Goadsby et al. 2002). Brain imaging studies using positron emission tomography show that the brain stem, particularly the periaqueductal grey matter (PAG), is activated at the beginning of a migraine attack (Weiller et al. 1995). The PAG is a major gateway to the limbic system and other sensory systems. The amount of light or sound coming into the body does not change during an attack; the brain’s sensory response does. As well as during an attack, the sensory processing mechanisms in the brain stem and limbic system in migraine patients are often hypersensitive both before and after an attack, reflecting an ongoing central sensitisation (Welch 2003; Woolf 2011).
Many patients who present with symmetrical frontal or temporal headache have a tension-type headache. However, facial pain can also be lateralised to one side, usually to the left (Min and Lee 1997). Mid-segment pain, where patients present with normal sinus CT scans and pain over the maxillary sinuses, also has many features consistent with central sensitisation. It represents a version of tension-type headache affecting the mid-face (Jones 2004). Chronic tension headache is associated with pain and increased tenderness in the head, neck and shoulder muscles (Figs. 18.2 and 18.3). A common assumption has been the pain in the head and neck muscles causes the headache. However, the neck muscles can also be painful because of central sensitisation in the spinal cord or brain stem. People with chronic tension headache are often more sensitive not only around the head, neck and shoulder muscles, but also elsewhere such as in the low back and calves, indicating an overall central sensitisation (Fumal and Schoenen 2008; Woolf 2011).
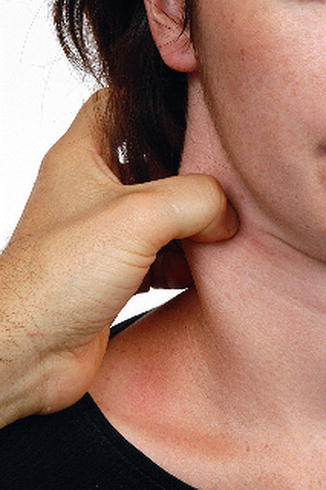
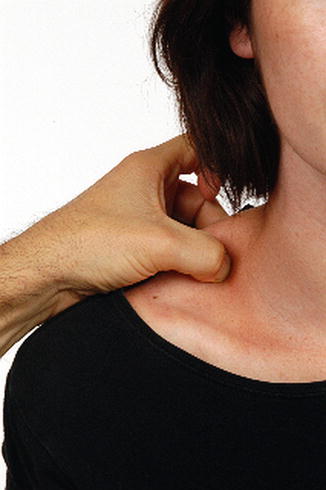

Fig. 18.2
To examine the sternocleidomastoid muscle for tenderness, the muscle needs to be examined up and down its length in a gentle pincer-like grip between thumb and forefinger

Fig. 18.3
A tender area in the superior midpoint of the shoulder in the upper trapezius muscle can be located if one palpates the superior aspect of the muscle between thumb and forefinger
The underlying pathophysiology behind migraine and tension headache is central sensitisation.
18.4 Medication Overuse Headache
In some people, the overuse of medication to treat their headache can make their headaches worse. It is important to take a medication history. If a person complains of daily headaches requiring regular pain medication (more than twice a week), the headache could be caused by the medications and, if so, will improve or disappear when the medications are discontinued. Medication overuse headache (MOH) can be a significant clinical challenge. The reality is almost every medication used to treat headache and migraine can cause MOH (Cupini et al. 2010). The general recommendation is patients come off these medications while under medical supervision.
18.5 Sinusitis
According to the diagnostic criteria of the 2004 International Headache Society, “chronic sinusitis is not validated as a cause of headache and facial pain unless relapsing into an acute stage” (Lipton et al. 2004). On the other hand, the American Academy of Otolaryngology – Head and Neck Surgery considers that facial pain or pressure is an important, although not exclusive, consideration in the diagnosis of CRS (chronic rhinosinusitis) (Levine et al. 2006; Meltzer et al. 2006). These views are the consensus opinion of experts in their respective fields. Many clinical studies show that the majority of patients presenting with “sinus headache” fulfil the diagnostic criteria for either migraine or tension headache (Silberstein 2004; Jones 2009).
While many patients with “sinus headache” may fulfil the criteria for tension headache, this does not exclude sinus infection contributing to central sensitisation.
While the patients may fulfil the criteria for tension headache, this does not exclude sinus infection contributing to central sensitisation, which is the underlying pathophysiology of these conditions. A review of recent advances in our understanding of pain pathophysiology indicates that a chronic infective process such as sinusitis can induce a central sensitisation (Scholz and Woolf 2007; Milligan and Watkins 2009). TLRs, particularly TLR2 and TLR4, which have been implicated in glial cell activation (Fig. 18.1), recognise and respond to endogenous danger signals such as lipopolysaccharide that are released by damaged and dying cells associated with active bacterial infection (Milligan and Watkins 2009; Liu et al. 2012).
Clinical evidence of central sensitisation is seen in CRS patients. The well-known physical finding of tenderness to palpation or percussion over the affected sinuses that is experienced by patients with sinusitis may be indicative of either excessive peripheral or central sensitisation. Increased muscle tenderness in CRS (Figs. 18.2 and 18.3) has been measured (Naranch et al. 2002). The quality of clinical evidence supporting the role of sinus surgery in helping patients with facial pain is not of a high quality. However, the majority of prospective studies looking at the results of endoscopic sinus surgery for facial pain/headache indicate that there is a group of CRS patients whose facial pain benefits from surgery (Tarabichi 2000; Moretz and Kountakis 2006; Phillips et al. 2007; Soler et al. 2008; Chester et al. 2009).
However, there are major limitations to these studies, and some of the improvement can be explained using other mechanisms. Some of these patients may have been suffering from medication overuse headache. The surgery, by itself, was an incentive to come off these medications. The natural history of these facial pain/headache conditions is also not known, and regression to the mean is also a potential mechanism. The breathing cycle is divided into inspiratory and expiratory phases. Nasal breathing slows the respiratory rate increasing the length of the expiratory phase (Ayoub et al. 1997). Increasing the expiratory phase of the respiratory cycle is known to increase the body’s relaxation response (Cappo and Holmes 1984). Improving nasal breathing could thus facilitate relaxation techniques which are effective treatments for both migraine (Campbell et al. 2009) and tension headache (Carlson 2008).
Many patients with purulent secretions visible at nasal endoscopy have no headache or facial pain (Jones 2004). When many so-called “sinus pain” patients present acutely with symptoms, many have no evidence of infection (Jones 2004). There is also no correlation between the severity and location of the pain with the extent or location of mucosal disease (Tarabichi 2000; Levine et al. 2006). These observations can be explained using a central sensitisation model. Sinus infection does not cause pain by itself; it simply influences sensory thresholds. In many, but not all, patients, this is insufficient to cause pain. In other patients, the inflammation will be such that pain processing is influenced.
Sinus infection does not cause pain by itself; it simply influences sensory thresholds.
The otolaryngologist has to be aware that sinus infection is but one possible contributor to a lowering of the sensory thresholds; other pathologies can also be responsible for exactly the same symptoms. Patients diagnosed with fibromyalgia and tension headache, who also have nervous system sensory and pain regulation abnormalities, can report exactly the same sinus symptoms (Naranch et al. 2002). The key to successful nasal and sinus surgery in “sinus pain” patients lies not only in the surgery itself but in careful patient counselling and selection. One should not be operating if the CT scan shows no evidence of sinus disease. One should be careful about operating on CRS patients in the absence of significant infective symptoms or signs. Co-morbidities reflecting other potential pathologies such as anxiety, depression, fibromyalgia, irritable bowel symptoms and neck and low back pain should make the surgeon very wary of attributing “sinus pain” to sinus disease (Woolf 2011).
18.6 Contact Points and Nasal Obstruction
The theory that contact points within the nose could cause headache reflects specificity theory thinking. The prevalence of a contact point has not only been found to be the same in an asymptomatic population as in a symptomatic population. In symptomatic patients with unilateral pain when a contact point was present, it has been found on the side contralateral to the pain in 50 % of patients (Abu-Bakra and Jones 2001). The relationship between nasal obstruction and headache is controversial. Schonsted-Madsen et al. (1986) showed that relief of headache (pain localised to the forehead, glabella or above or around the eyes) was strongly related to relief of nasal obstruction (Schonsted-Madsen et al. 1986). A potential reason as to why improvement in the nasal airway might lead to improvement in tension headache has previously been described (Sect. 18.5).
The weight of evidence supports the view that chronic temporomandibular joint pain is not due to occlusal abnormalities.
18.7 Temporomandibular Joint Disorders
The weight of evidence supports the view that chronic temporomandibular joint (TMJ) pain is not due to occlusal abnormalities (Koh and Robinson 2004). Psychophysiological forces are important (Suvinen et al. 2005; Carlson 2008). The TMJ is lubricated by synovial fluid, which also nourishes the avascular cartilage and cartilaginous disc in the middle of the joint. Whenever the joint is compressed, the blood supply to the joint is reduced and the joint has difficulty manufacturing lubricating fluid. The friction within the joint increases, and the cartilaginous disc in the middle of the joint begins to stick (Nitzan 2001). In times of stress, people tend to breathe using their upper chest, which tends to lead to a forward head position and increased pressure on the joint or clench and grind their teeth. Increased pressure in the TMJ can lead to clicking and sticking of the cartilage disc. If the friction increases, the ligaments holding the disc in place stretch and the disc moves off the condylar head (Bartley 2011). In the absence of any major external trauma, before addressing any structural changes within the jaw joint, underlying psychosocial stresses, breathing re-education as well as musculoskeletal issues need to be addressed (Carlson 2008; Aggarwal et al. 2010).
18.8 Causes Removed from the Orofacial Area
A history of neck injury can often be overlooked. The nerve supply to the upper neck and head overlaps in the upper spinal cord. Using first principles, neck pain could be referred to the head. Alternatively, by sensitising the spinal cord to incoming pain messages, neck pain could lower the pain threshold to other sensory messages being received from the face and head. After a whiplash injury to the neck, areas well away from the original injury site – from the head to the feet – can be shown to be hypersensitive to normal sensory messages (Woolf 2011).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


