We thank the correspondent for her comment on our recent publication reporting that total posterior vitreous detachment (PVD) by ultrasound was associated with 3 times as many cases of dry age-related macular degeneration (AMD) as cases with wet AMD (69% vs 21%; P = .002). An attached posterior vitreous cortex by optical coherence tomography (OCT) was associated with 4 times as many cases of wet AMD as dry AMD (38% vs 10%; P = .008). We agree with the proposal that one of the plausible mechanisms by which PVD may be salubrious and vitreomacular adhesion may be deleterious is that oxygenation of the macula is enhanced in the absence of an attached posterior vitreous. Indeed, in our original publication, the third sentence of the fifth paragraph of the discussion states that: “ The presence of the posterior vitreous cortex attached to the macula could prevent oxygen and perhaps nutrients from diffusing from the ciliary body into the macula. The resulting state of relative ischemia could promote choroidal neovascularization via the action of VEGF .”
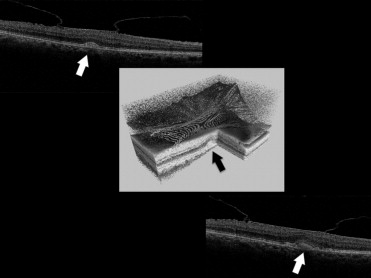
There are reasons, however, to suspect this is not the only explanation. A recent study (Binder et al, IOVS 2009;50: ARVO E-abstract 5245) has shown that in most cases of exudative AMD with vitreomacular adhesion, there is a positive correlation between the site of vitreous adhesion to the macula and underlying choroidal neovascularization (CNV). In 72% of these eyes, traction of the posterior vitreous cortex onto the macula was visible and the traction lines were directed towards the CNV, as visualized in 3-D and longitudinal OCT images ( Figure ). Vitreous was adherent to the fovea in 52.4% of cases and was juxtafoveal in 47.6%. In 93% of the juxtafoveal adhesions, a retinal angiomatous proliferation (RAP) was present, and the area of the adhesion corresponded with the localization of the “hot spot” on ICG angiography.