Purpose
To determine whether pretreatment (baseline) optical coherence tomography (OCT) features can be used as predictors of visual acuity outcome at 12 months in eyes with neovascular age-related macular degeneration treated with intravitreal ranibizumab and to assess whether baseline OCT features can predict a change in visual acuity from baseline to 12 months.
Design
Retrospective, observational study.
Methods
We retrospectively evaluated the serial cross-sectional images of the macula obtained using the Spectralis OCT (HRA+OCT; Heidelberg Engineering) in 100 eyes of 94 patients attending a single center and undergoing treatment with intravitreal ranibizumab for neovascular age-related macular degeneration. The baseline OCT characteristics and visual acuity were correlated to the final visual acuity (Early Treatment Diabetic Retinopathy Study letters) and change in visual acuity after 12 months of monitoring and treatment. Univariate and multivariate analyses were carried out to correlate these morphologic features with the final visual acuity and the change in visual acuity.
Results
Intact ellipsoid zone ( P = .0001) and external limiting membrane in the subfoveal area ( P < .0001) at baseline were the only 2 independent good prognostic indicators of final visual acuity at 12 months. However, none of the morphologic features at baseline could predict the change in visual acuity by 12 months.
Conclusions
The results suggest that integrity of the outer retinal layers at baseline is crucial for determining final visual acuity at 12 months in eyes undergoing treatment with ranibizumab for neovascular age-related macular degeneration.
The development of intravitreal ranibizumab, a monoclonal antibody directed against all isoforms of vascular endothelial growth factor A (VEGF-A), represents a major therapeutic shift from existing therapies for neovascular age-related macular degeneration (AMD). Randomized clinical trials have shown that monthly dosing with ranibizumab is effective in preventing visual loss and is capable of significantly improving visual acuity (VA) in up to one third of patients with subfoveal neovascular AMD. These results have raised the expectations of both the physicians and patients regarding the extent of visual loss that can be prevented or reversed in neovascular AMD.
The Prospective Optical Coherence Tomography Imaging of Patients with Neovascular Age-Related Macular Degeneration Treated with Intraocular Ranibizumab study showed that after the first 3 monthly intravitreal ranibizumab injections, time-domain OCT-guided retreatment provides similar outcomes to monthly dosing. However, in real life, many subsequent reports have indicated that the outcomes of pro re nata dosing are variable. Approximately 20% to 30% of patients do not respond to the treatment (defined as a loss of ≥5 Early Treatment Diabetic Retinopathy Study [ETDRS] letters). However, there are very limited surrogate markers for good response. It therefore is important to identify accurate prognostic indicators to define the responders better.
The advent of spectral-domain OCT with better axial resolution, faster acquisition time, real-time tracking of eye movements, and real-time averaging of scanning laser ophthalmoscopic images have reduced the signal-to-noise ratio of the images. Thus, the significant improvement in image quality has allowed precise analyses of the retinal microstructures. The aim of this study was to evaluate the predictive value of the morphologic features of the macula on OCT at baseline in assessment of visual prognosis at 12 months.
Methods
This was a retrospective, observational study that involved case notes and serial OCT scan reviews conducted in the Laser and Retinal Research Unit of King’s College Hospital, London, United Kingdom. The study was approved by the Research and Development department of King’s College Hospital, NHS Foundation Trust, as a retrospective study not requiring Ethics Committee approval or informed consent. The study adhered to the tenets of the Declaration of Helsinki.
Patients
Patients with treatment-naïve subfoveal neovascular AMD of any lesion subtype, with lesion size of less than 12 disc areas and VA between 24 (Snellen equivalent, 20/320) and 73 (Snellen equivalent, 20/32) ETDRS letters at baseline were included. All eyes were required to have clear media that permitted OCT imaging with good signal strength (signal-to-noise ratio, >20 dB). Patients with choroidal neovascularization (CNV) membranes secondary to causes other than AMD, previous laser photocoagulation or photodynamic therapy, and other retinal diseases in the study eye, including diabetic retinopathy or hereditary retinal dystrophies, were excluded.
Baseline Examination
As part of routine care, each patient underwent VA measurement with ETDRS charts at 2 m. Before slit-lamp examination, the pupils were dilated with 1% tropicamide and 2.5% phenylephrine. Spectralis OCT (HRA+OCT; Heidelberg Engineering, Heidelberg, Germany) scans were obtained using defined protocols (as detailed below). Lesion characteristics were defined by fundus fluorescein angiography (FFA). Indocyanine angiography was performed to confirm retinal angiomatous proliferans and polypoidal vasculopathy in clinically suspicious cases. Four angiographic membrane subtypes of the CNV were identified in the patients. Predominantly classic CNV membranes showed an early lacy filling pattern on FFA, which increased in mid phase with leak in the late phase. The second group consisted of patients with occult membranes that showed a stippled filling pattern in mid phase with leak in the late phase. Minimally classic lesions had a classic component occupying less than 50% of the entire lesion area by FFA. The fourth group included patients with retinal angiomatous proliferans, confirmed by indocyanine angiography. Retinal angiomatous proliferans was characterized by early hyperfluorescence at the tip of a retinal vessel on FFA with an associated hot spot on indocyanine angiography.
Retreatment Criteria
Follow-up assessments of VA were carried out by trained personnel in a busy clinic setting, and refraction was not repeated. Biomicroscopy and OCT examinations were carried out at each monthly visit. Fundus fluorescein angiography was repeated only if a new hemorrhage was noted on slit-lamp biomicroscopy with no significant changes on OCT compared with the previous visit.
Criteria for retreatment included recurrence of any subretinal fluid or intraretinal fluid on OCT, a decrease of 5 ETDRS letters associated with fluid on OCT, new hemorrhage, angiographic evidence of increase in lesion size, or a combination thereof. The presence of pigment epithelial detachments (PEDs) was not considered as a retreatment criterion.
Optical Coherence Tomography Acquisition
The Spectralis (HRA+OCT), combines high-resolution spectral-domain OCT with a scanning laser ophthalmoscope. The OCT volume scan was performed on a 20 × 20-degree cube, with 49 raster lines, each containing 1064 pixels, separated by 125 μm. The morphologic features on OCT at baseline and at 12 months were assessed.
Morphologic Features on Optical Coherence Tomography
The integrity of the retinal layers was analyzed in the subfoveal area (1 mm) at baseline and at 12 months of follow-up. The OCT characteristics of the eyes specifically noted were the presence or absence of the external limiting membrane (ELM), ellipsoid zone presumed to represent the inner segment of photoreceptors, subretinal thickening (SRT), intraretinal fluid, subretinal fluid, hyperreflective dots in the retinal layers, outer retinal tubulations, vitreomacular traction (VMT), epiretinal membrane (ERM), PED, and outer segment stalactites ( Figure ).
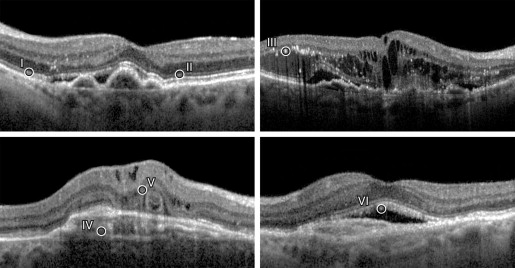
The ellipsoid zone was identified as the second HRB layer above the hyperreflective band of the retinal pigment epithelium (RPE). The hyperreflective layer between these 2 bands, termed the interdigitation zone , was not always visible in all the scans, and so it was not considered as a prognostic feature for this study. The ELM was seen as a less dense hyperreflective line anterior to the ellipsoid layer.
Subretinal thickening is a spindle-shaped or fusiform, uniformly dense, hyperreflective band that straddles the RPE. Fluid accumulation was defined as hyporeflective areas within the inner retina, intraretinal fluid, or between the retina and RPE, subretinal fluid. Pigment epithelial detachment was identified as an elevation of the RPE overlying a hyporeflective or optically empty area. Hyperreflective dots are small particles scattered throughout the retinal layers, more frequently in the outer retina. Outer retinal tubulations were defined as rounded, ring-like, hollow structures with a hyperreflective border, noted in areas with disruption of the outer retina. They usually were seen overlying areas of RPE damage or SRT or at the junction between the preserved and lost ellipsoid zone. Outer segment stalactites were defined as hyperreflective elongated areas that overhang an area of subretinal fluid.
Vitreomacular interface changes were classified as ERM, VMT, and posterior vitreous detachment. ERMs were deemed to be present if 1 or more of the following conditions were met: a macular pseudohole, a difference in optical reflectivity between membrane and retina, or a visible membrane tuft or edge. VMT was considered to be present when a highly reflective band was observed on the surface of the retina at specific sites and was elevated off the surface elsewhere, whether continuous or not with the posterior vitreous surface.
All the morphologic features were dichotomous variables, classified as being present or absent, if any of these structures could not be identified reliably. Discontinuities of the ellipsoid zone and the ELM were classified as the presence or absence of these layers in the subfoveal area. The OCT features were evaluated at baseline and on the 12-month visit after commencement of treatment.
Grading Procedure
All digital OCT image sets on Spectralis were assessed independently by 2 graders (R.M. and M.R.). They were masked to the VA recordings. Differences were adjudicated by the senior author (S.S.), after discussion.
Statistical Methods
Sample size was based on the calculation suggested by Flahault and associates. For a sensitivity of 0.95, with a 0.95 probability of the lower 95% confidence limit of 0.85, the approximate number of cases required was 93. Analyses were conducted using MedCalc software version 12.3.0.0 (Mariakerke, Belgium). Univariate analysis was carried out to evaluate the association of each OCT feature at baseline with the 12-month VA. Multiple linear regression was performed on the variables taken into account on univariate analysis to detect independent prognostic indicators, after which a parsimonious model of VA was performed using the significant predictors. Statistical significance was set at P < .05 for all analyses. The equation derived from this model was validated further on eyes of another 25 patients being treated with ranibizumab for neovascular AMD.
The reliability of the grading of each OCT feature was determined using weighted κ statistics and intraclass correlation coefficients. κ statistics were interpreted using ranges suggested by Landis and Koch: 0 to 0.20, slight agreement; 0.21 to 0.40, fair agreement; 0.41 to 0.60, moderate agreement; 0.61 to 0.80, substantial agreement; and more than 0.80, almost perfect agreement. The intraclass correlation coefficient was considered reliable if the values were between 0.4 and 0.75, and values over 0.75 were considered excellent.
Results
Baseline Characteristics
The study included 110 eyes of 97 patients. After excluding the eyes with uncertainty regarding the OCT features, there were 100 eyes of 94 patients, with 22 men and 78 women. The average age of the patients was 79.1 ± 1.7 years. The CNV subtypes included 5 cases of predominantly classic CNV (5%), 2 cases of minimally classic CNV (2%), 73 cases of occult CNV (73%), and 20 cases of retinal angiomatous proliferans (20%). All the patients had a minimum follow-up of 12 months, with a mean follow-up of 18 months (range, 12 to 24 months). The mean VA at baseline was 56.7 ± 12.7 and that at 12 months was 64.3 ± 7.24 ETDRS letters.
Univariate Analyses
The mean VA at 12 months, based on the presence or absence of each OCT feature at baseline, is shown in Table 1 . The integrity of the ellipsoid zone and the ELM and outer segment stalactites were found to be positive predictors of VA, whereas outer retinal tubulations and intraretinal fluid were negative predictors of VA. The comparison of VA at baseline and 1 year between the various membrane subtypes is shown in Table 2 . The VA gain was statistically significant only in occult CNV.
| Variable at Baseline | Mean VA at 12 Months ± SD | P Value | Pearson Correlation Coefficient | |
|---|---|---|---|---|
| OCT Feature Absent | OCT Feature Present | |||
| Ellipsoid zone | 57.2 ± 26.2 | 71.9 ± 6.3 | .0000 | 0.490 |
| ELM | 44.1 ± 19 | 68.1 ± 8.5 | .0001 | 0.589 |
| SRT | 65.8 ± 15 | 59.8 ± 14 | .075 | −0.178 |
| PED | 66.5 ± 13 | 62.5 ± 27 | .178 | −0.132 |
| SRF | 62.4 ± 15 | 65.1 ± 15 | .419 | 0.100 |
| IRF | 69.4 ± 12.7 | 61.2 ± 16.9 | .004 | −0.266 |
| HRD | 65.3 ± 18.5 | 63.7 ± 13.3 | .624 | −0.047 |
| ORT | 65.9 ± 14.2 | 47.7 ± 5.6 | .0004 | −0.348 |
| OSS | 62.4 ± 15.5 | 72.5 ± 9.2 | .017 | 0.264 |
| ERM | 64.1 ± 15 | 68.5 ± 4.2 | .737 | 0.057 |
| VMT | 64.7 ± 15 | 59.8 ± 18.4 | .447 | −0.090 |
| No. | Baseline VA ± SD | 1 Year VA ± SD | P Value | |
|---|---|---|---|---|
| Occult | 73 | 55.4 ± 12 | 62.9 ± 14 | .0015 |
| PCCNV | 5 | 58.2 ± 10 | 64.4 ± 18 | .5326 |
| MCCNV | 2 | 67 ± 12 | 77.5 ± 14 | 1.0000 |
| RAP | 20 | 58.8 ± 13 | 67.36 ± 15 | .0818 |
Multivariate Analyses
A multivariate analysis using the variables at baseline and VA at 1 year revealed that the positive predictors were the integrity of the ellipsoid zone and ELM at baseline. None of the other OCT parameters showed an association with the VA at 1 year ( Table 3 ). More importantly, none of the morphologic features at baseline could predict a change in VA from baseline to 1 year (data is not shown).
| Independent Variables | Unstandardized Coefficients | Standardized Coefficients: Beta | P Value | |
|---|---|---|---|---|
| Beta | Standard Error | |||
| (Constant) | 53.042 | |||
| Ellipsoid zone | 7.564 | 2.571 | 0.304 | .004 |
| ELM | 18.570 | 3.740 | 0.474 | <.0001 |
| ORT | −5.394 | 5.947 | −0.098 | .367 |
| IRF | −4.974 | 2.875 | −0.184 | .087 |
| SRF | −8.037 | 3.165 | −0.266 | .013 |
| SRT | −0.602 | 2.936 | −0.022 | .838 |
| ERM | 7.756 | 6.057 | 0.138 | .204 |
| OSS | 4.939 | 3.177 | 0.166 | .124 |
| PED | −2.285 | 2.559 | −0.096 | .375 |
| VMT | −6.546 | 5.131 | −0.137 | .206 |
| HRD | 2.003 | 2.642 | 0.082 | .451 |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


