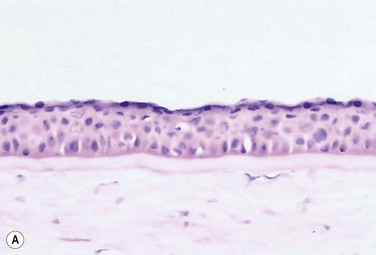
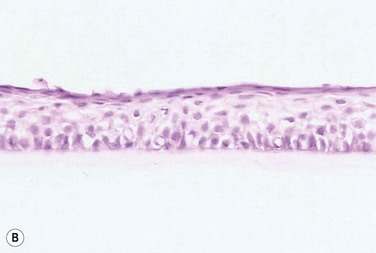
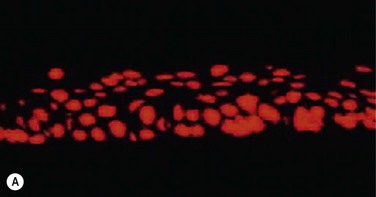
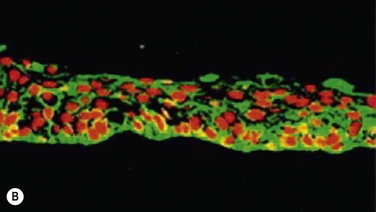
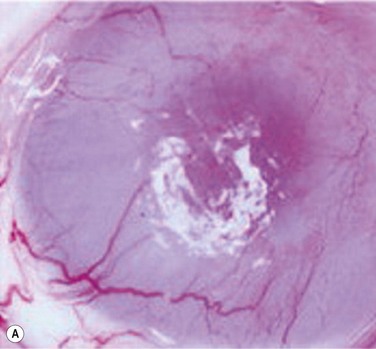
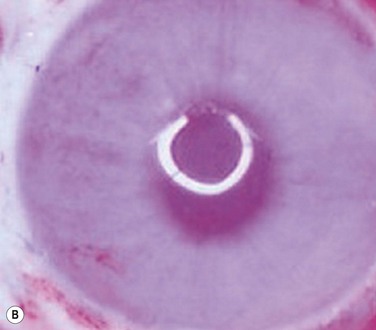
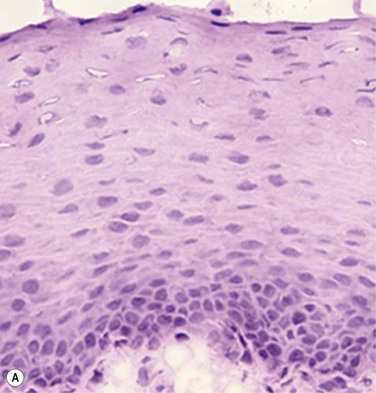
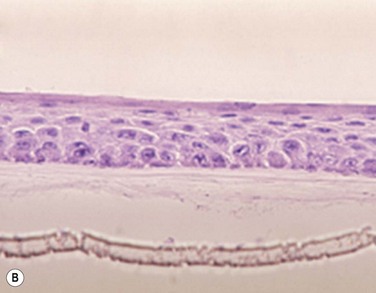
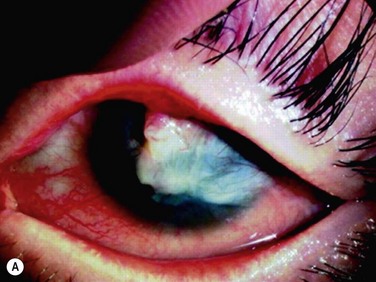
45 The Successful Culture of Rabbit Oral Mucosal Epithelial Cells The problem of allograft rejection is the main reason that we decided to develop a new method of autologous oral mucosal epithelium transplantation for OSR.1 In our laboratory experiment, epithelial cells from the oral mucosa began to form colonies on the denuded AM within 3 days. At 3 weeks, the cultivated oral epithelial cells showed 4–5 layers of stratification, were well differentiated (Fig. 45.1A), and appeared very similar to in vivo normal corneal epithelium (Fig. 45.1B).1 Cytokeratins play an important structural and protective role in maintaining the integrity of the epithelium of the anterior segment of the eye. Defined subsets of individual cytokeratin pairs are characteristically expressed, depending on the type of epithelial cell tissue and level of differentiation. In this study, we used immunohistochemistry to demonstrate that the keratin 1/10 pair, which is involved in the physiological keratinization process in the epidermis, is not expressed in any layers of the cultivated oral epithelial sheet. We also found that the keratin 4/13 pair, which is observed in nonkeratinized, stratified epithelia, is expressed in the superficial and intermediate layers of the cultivated oral epithelial cells. These results led us to believe that the oral epithelial cells cultivated on AM have the characteristics of nonkeratinized mucosa, not keratinized mucosa. Immunohistochemical examination revealed no cornea-specific keratin 12 expression in any layers of the cultivated oral epithelial sheets (Fig. 45.2A), whereas cornea-specific keratin 3 was expressed in all epithelial layers of the cultivated oral epithelial sheet (Fig. 45.2B). Even though the cells of the cultivated oral epithelial sheet are not able to become corneal epithelial cells, we suggest that they might have the potential ability to become cornea-like epithelial cells under proper in vitro culture conditions. Electron microscopic results of the cultivated oral mucosal epithelial sheet are of particular interest. Examination by use of a scanning electron microscope (SEM) revealed that rabbit oral epithelial cells appeared healthy and well formed with tightly opposed cell junctions (Fig. 45.3). The cultivated oral cells were similar in size and appearance to rabbit corneal epithelial cells. Transmission electron microscopy (TEM) confirmed that the cultivated oral epithelial sheet was very similar in appearance to that of corneal epithelium, and very different from conjunctiva and oral mucosa. Like corneal epithelium, it had 4–5 layers of stratified cells which were differentiated into columnar, wing, and squamous cells (Fig. 45.4). Both our SEM and TEM results show clearly that our oral mucosal cells, cultivated on AM, resemble normal corneal epithelial cells more closely than any other cell type. After the successful culture of rabbit oral mucosal epithelial cells on AM, we tried to reconstruct the damaged corneal surfaces by transplantation of autologous cultivated oral mucosal epithelial cells in order to test the viability of using these cells as a substitute for cultivated corneal epithelial cells. At 48 hours after surgery, most of the area of the transplanted cultivated oral mucosal epithelial sheet possessed intact epithelium. At 10 days after transplantation, the ocular surface covered by the transplanted epithelium was intact and without defects, thus suggesting that the autologous transplantation of cultivated oral mucosal epithelia is a viable procedure for ocular surface reconstruction (Fig. 45.5). Histological examination of the transplanted sheets at 10 days after surgery revealed that the sheets were well adhered to the host corneal stroma, with no evidence of subepithelial cell infiltration or stromal edema. Superficial cells of the transplanted sheets had nuclei, indicating that they were indeed nonkeratinized mucosal epithelial cells. We next focused our attention on cultivating human oral mucosal epithelial cells using our previously reported culture methods for rabbit oral mucosal epithelial cells, yet with several modifications. It should be noted that it was quite difficult to cultivate human oral mucosal epithelial cells using the previously reported culture technique for rabbit oral epithelial cells, and therefore, the culture process did require some modification. In the end, and as a result of the modification, we were able to successfully generate a well-stratified and differentiated human cultivated oral mucosal epithelial sheet (Fig. 45.6). Light microscopy revealed that the human cultivated oral mucosal epithelial cells were very similar in appearance to normal corneal epithelial cells. Moreover, immunohistochemistry confirmed the presence of keratins 4/13 and 3 in the human cultivated oral mucosal epithelial cells, similar to those found in the rabbit model. In the past, several researcher groups investigated the possibility of using oral mucosa for OSR. Ballen reported that oral mucosal grafts which included both epithelium and subepithelial tissues, heavily vascularized with early fibrosis.2 In addition, Gipson et al. reported that in vivo oral epithelium, freed of underlying connective tissue, was not maintained in the central avascular corneal regions.3 We investigated the possibility of reconstructing the human ocular surface using autologous mucosal epithelium of non-ocular-surface origin. Using rabbits, we have already established a surgical method for transplanting cultivated autologous oral mucosal epithelial cells.1 We next applied this method in six eyes of four patients with severe OSD.4 At 48 hours post transplant, the entire corneal surface of all six eyes was free of epithelial defects, indicating complete survival of the transplanted cultivated oral mucosal epithelium. Visual acuity was improved in all eyes. During follow-up (13.8 ± 2.9 months), the ocular surface remained stable, although all eyes showed mild peripheral neovascularization. Therefore, autologous cultivated oral mucosal epithelial sheets can be transplanted to treat severe OSD (Fig. 45.7). This initial clinical study represents a first step toward assessing the feasibility of transplanting autologous cultivated epithelial transplants of non-ocular-surface origin.
Non-Ocular Sources for Cell-Based Ocular Surface Reconstruction
Development of Cultivated Oral Mucosal Epithelial Transplantation (COMET, Preclinical Trail)
Cell Biological Characteristics of the Rabbit Cultivated Oral Mucosal Epithelial Sheet
Morphological Characteristics of the Rabbit Cultivated Oral Mucosal Epithelial Sheet
Successful Transplantation of the Rabbit Cultivated Oral Mucosal Epithelial Sheet
The Successful Culture of Human Oral Mucosal Epithelial Cells
Transplantation of Cultivated Oral Mucosal Epithelial Cells in Patients with Severe OSD (Clinical Trial)
Non-Ocular Sources for Cell-Based Ocular Surface Reconstruction