Fig. 27.1
Graphic representation of the findings from RRM. Right side of the nose, red; left, blue. Light-colored curves: before decongestion of the mucosa. Dark-colored curves: after decongestion of the mucosa. Upper graph: nasal airway resistance. Lower graph: turbulence flow behavior of the nasal airstream. x-axis: left of the midline: inspiratory flow in ml/s. right of the midline: expiratory flow in ml/s. y-axis: upper graph: resistance in sPa/ml. lower graph: turbulent flow behavior: lam. laminar, turb. turbulent
The graph enables us to evaluate nasal airway resistance for each side of the nose “at a glance”: the higher the path of the curve, the greater the nasal obstruction. In Fig. 27.1, the right side of the nose is obstructed prior to decongestion.
In addition, by examining the distance between the curves before and after decongestion, we can differentiate between the portions of nasal airway resistance due to congestion and due to skeletal narrowing. In Fig. 27.1, a decongestant effect can be seen on the right side. At the measurement before decongestion, there was mucosal congestion on the right side of the nose (e.g., during a resting phase in the nasal cycle). After decongestion, resistance is low on both sides of the nose. Thus, there is no obstruction related to skeletal narrowing on either side of the nose.
Figure 27.2 shows rhinoresistometric resistance curves in a nose with mucosal congestions and skeletal obstruction on the right.
After decongestion, nasal resistance improves (the mucosal component), but the resistance still remains elevated (the skeletal component).
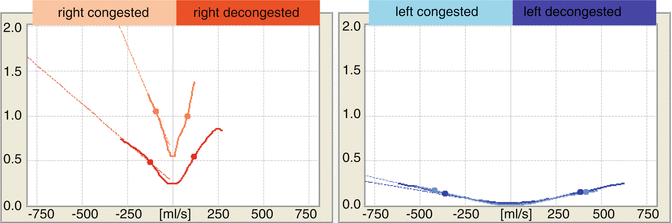

Fig. 27.2
Rhinoresistometry resistance curves from the right side of a nose obstructed by mucosal congestion and skeletal constriction with normal findings on the left
Besides detecting obstruction at a glance, it is also possible to establish the diagnosis of inspiratory nasal valve collapse (NVC) by looking at the graph. In the graphical presentation of nasal airway resistance, the inspiratory arm includes a calculated curve as an interrupted line, which indicates the flow-dependent increase in airway resistance in the presence of a stable vestibular wall (without collapse resulting from suction and the Bernoulli effect). Deviations of the measured (continuous line) curve from the (interrupted) straight line indicate abnormalities in the width of the flow channel, such as those resulting from NVC (Fig. 27.3).
The measured and calculated curves will be congruent if the nasal valves are not sucked in during inspiration as a result of the Bernoulli effect (Fig. 27.1, right prior to decongestion; Fig. 27.2, all curves; Fig. 27.3, right prior to decongestion). The greater the extent of NVC, the more sharply the measured curve will deviate from the calculated curve (Gruetzenmacher et al. 2005a). Slight deviation at high flow velocities (>500 ml/s) indicates physiological collapse of the nasal valves (Fig. 27.1, right prior to decongestion and left before and after decongestion; Fig. 27.3, right after and left prior to decongestion). One can identify pathological collapse of the nasal valves on the basis of a large deviation of the measurement from the calculated curves (Fig. 27.3, left after decongestion).
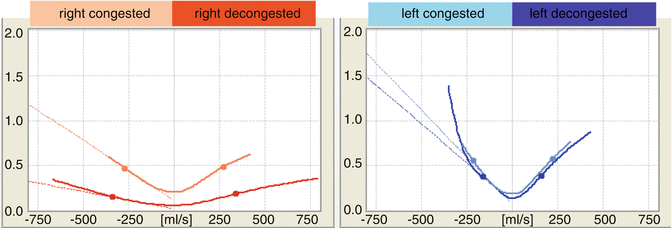

Fig. 27.3
Resistance curves measured by rhinoresistometry (continuous lines) and resistance curves calculated with a stable lateral vestibular wall (dotted lines on the inspiratory side of the curve). Right before decongestion: no NVC. Right after decongestion and left before decongestion: physiological NVC. Left after decongestion: pathological NVC
The graphical representation allows us to estimate the proportion of the increase in nasal airway resistance caused by collapse of the nasal valves. It also makes it possible to establish an initial assessment of how much improvement in nasal airway resistance might be expectable as a result of surgical stiffening of the lateral vestibular wall.
27.2.1.1.2 Lower Graph: Inspiratory and Expiratory Turbulence Behavior in Relation to Airflow Velocity
In the RRM, the lower graph (Fig. 27.1) displays the turbulence behavior of nasal airflow in relation to airflow velocity. The level on the x-axis corresponds to pure laminar flow, and the upper blue-gray bars correspond to marked turbulence.
At very low flow velocities, flow is laminar in any flow channel (Mlynski and Loew 1992) and thus in the nose as well. In inspiration and expiration, as the velocity of flow increases, laminar flow portions transition into turbulent flow portions. This “transitional zone” is important for the respiratory function of the nose. It creates the optimal situation for conditioning the air. It provides for adequate mucosal contact by the streaming air without leading to drying out or cooling of the mucosa. At very high airflow velocities, nasal airflow becomes purely turbulent (Mlynski and Loew 1992; Churchill et al. 2004; Sawyer et al. 2007; Chen et al. 2009, 2010; Leong et al. 2010). Pure turbulence hardly ever occurs in a normal nose. When high airflow velocities are required to provide adequate oxygen supplies during heavy physical activity, oral bypass breathing is unconsciously switched on so that the nasal airstream decreases (see above: zone of “physiologically required nasal airflow”).
Nasal airflow should become more turbulent when the mucosa is in a decongested state (corresponding to the working phase of the nasal cycle) as a condition for sufficient mucosal contact than in the congested state (corresponding to a resting phase in the nasal cycle). In the resting phase (decongested mucosa), the flow character should not become purely turbulent up to an airflow velocity of 250 ml/s (Fig. 27.1, bilaterally; Fig. 27.4, right side of the nose).
In pathological turbulence behavior, there is a rapid transition to pure turbulence so that pure turbulence will already develop in the nose at a flow rate <250 ml/s (Fig. 27.4, left side of the nose).
Excessive turbulence in the nose can be the cause of elevated airway resistance, and it can also cause a sense of stuffiness and sicca symptoms at low levels of airway resistance.
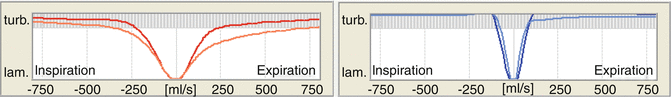

Fig. 27.4
Turbulence curves from rhinoresistometry. x-axis: left of the y-axis: inspiratory flow in ml/s. right of the y-axis: expiratory flow in ml/s. y-axis: degree of turbulence. The x-axis corresponds to pure laminar flow (lam.), and the upper blue-gray bars correspond to marked turbulence (turb.). Right nose (red): typical of physiological transition from laminar to turbulent flow behavior. Left nose (blue): typical of pathological turbulent flow behavior
27.2.1.2 Numerical Values
Besides using the graphical representations to establish a “diagnosis at a glance,” the numerical values make it possible to precisely estimate the extent and the causes of obstruction. Different individuals with the same degree of nasal obstruction may have quite varied levels of symptoms depending on their age, gender, body mass index, level of physical fitness, and associated illnesses. Therefore, the reference values presented here should not be applied rigidly. They are simply benchmarks for the purpose of orientation. The values were determined through studies on both rhinologically healthy patients and patients with nasal obstruction (Marschall 1997; Enßen 2005; Fiebig 2007; Gogniashvili et al. 2011).
Nasal air resistance (R) is numerically reported at a flow velocity of 250 ml/s before and after decongestion. As presented in Sect. 27.2.1.1, the maximum flow velocity still within the zone of physiologically required flow is around 500 ml/s. If we assume that with moderate physical activity, both sides of the nose will enter the working phase of the nasal cycle (which is known as the “in-concert” cycle), at this level of activity, each side of the nose should have a flow rate of about 250 ml/s. No mouth-bypass breathing should occur with moderate physical activity (Olson and Strohl 1987). This is the reason that for a total flow rate = 500 ml/s, there must be no nasal obstruction present. Thus, for the practical evaluation of nasal obstruction, the resistance measured at 250 ml/s is an important value (Gehring et al 2000; Sawyer et al. 2007).
The extent of nasal obstruction can be estimated according to the reference values in Table 27.1.
Table 27.1
Standard values for nasal resistance at 250 ml/s for evaluating nasal obstruction
Resistance at 250 ml/s | Extent of obstruction on one side of the nose |
|---|---|
<0.17 sPa/ml | No obstruction |
0.17–0.35 sPa/ml | Slight obstruction |
0.36–0.70 sPa/ml | Moderate obstruction |
>0.70 sPa/ml | Severe obstruction |
Hydraulic diameter (d h ) is a measure of the width of the nasal cavum. The nasal cavity is a space with irregular cross sections. Therefore, its width cannot be defined simply by its diameter as with a round tube. In technological science, the usual practice when dealing with an irregular cross section is to use the “hydraulic diameter.” This is the diameter of a tube of the same length with a round cross section that has the same resistance to flow as the irregularly shaped flow channel. The figures shown in Table 27.2 can be used as reference values for estimating the width of the interior of the nose.
Table 27.2
Standard values for hydraulic diameter for determining the width of the nasal flow channel
Hydraulic diameter | Width of the nose |
|---|---|
<5.5 mm | Too narrow |
5.5–6.5 mm | Normal width |
>6.5 mm | Too wide |
Hydraulic diameter is shown before and after decongestion. Using these values, one can identify a mucosal swelling and a skeletal narrowing as the cause of nasal obstruction. The increase in magnitude of the hydraulic diameter by decongestion is an index of mucosal swelling. If the hydraulic diameter remains low after decongestion, this is evidence of skeletal stenosis. A very large hydraulic diameter indicates a nose that is too wide.
Numerical values for NVC are calculated before and after decongestion. To objectify the extent of NVC, a calculation is made of the percentage increase in resistance (∆R) caused by suction at a flow velocity of 500 ml/s (Fig. 27.5, left). If this flow velocity cannot be achieved, the calculation is performed at maximum inspiration (Fig. 27.5, right).
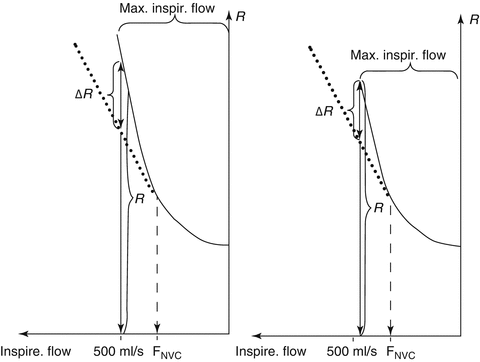

Fig. 27.5
Schematic representation of the inspiratory arm of an RRM curve during NVC for calculating the increase in resistance ΔR caused by sucking in the lateral wall of the nasal vestibulum. Left: calculation with maximum inspiratory flow >500 ml/s. Right: calculation with maximum inspiratory flow <500 ml/s. ____ Measured RRM curve, …….. Calculated curve for a stable lateral vestibular wall, F NVC Flow rate at which NVC begins, R Resistance at flow rate = 500 ml/s or at maximum inspiratory flow, ΔR Percent increase in resistance as a result of NVC
The numerical value for the increase in resistance from NVC (ΔR) allows us to estimate the magnitude of the suction phenomena as well as to differentiate between physiological and pathological NVS, in accordance with Table 27.3.
Table 27.3
Standard values for the increase in resistance (ΔR) as a result of NVC for differentiating between physiological and pathological NVC
ΔR | NVC |
|---|---|
<25 % | Physiological |
>25 % | Pathological |
In addition, the nasal airflow velocity at which suction/collapse begins (F NVC) is quantified. The nasal valves should not be significantly collapsed/sucked in (ΔR < 25 %) at airflow velocities up to the maximum physiologically required nasal airflow of 500 ml/s.
The friction coefficient λ is reported during inspiration and expiration, both before and after decongestion. This index characterizes the configuration of the inner nasal wall in relation to its degree of “streamlining,” that is, its impact on the development of turbulent flow, which is important for the warming and humidifying function of the nose (Keck and Lindemann 2010). A low λ-value suggests an internal configuration that causes few turbulent regions of flow. High λ-values indicate greater turbulence formation.
Using the reference values in Table 27.4, the interior of the nose can be evaluated with respect to its tendency to trigger turbulence.
Table 27.4
Standard values for the friction coefficient λ as an index for the tendency of the inner nasal walls to create turbulence
Friction coefficient λ | Turbulence |
|---|---|
Up to 0.30 | Normal tendency for turbulence |
<0.30 | Severe tendency for turbulence |
In the nose, the λ-value changes over the nasal cycle: it increases after decongestion in the working phase. This promotes the mucosal contact with the flowing air that is required for thermal and humidity exchange. In the resting phase, the friction coefficient becomes lower, and the airflow becomes more laminar (Lang et al. 2003).
Values over 0.030 indicate severe turbulence, which can cause elevated airway resistance, sicca symptoms, and/or a feeling of stuffiness.
Figure 27.6 presents rhinoresistometry graphs and numerical values from a patient with right mucosal congestion, right skeletal narrowing, and left pathological turbulence behavior.
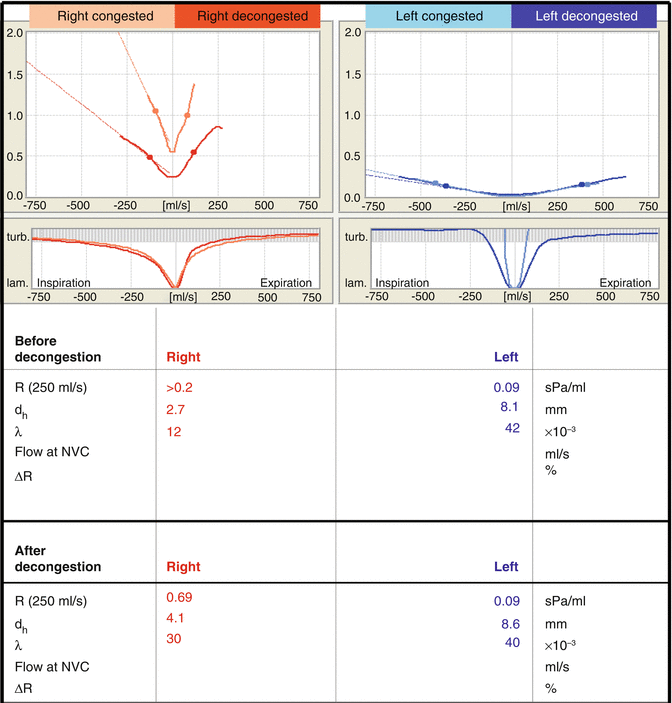

Fig. 27.6
Results of rhinoresistometry measurements in a patient with severe nasal obstruction as a result of mucosal congestion and skeletal stenosis as well as pathological turbulence on the left side from an excessively wide nose
Figure 27.7 shows RRM findings from a patient with “empty nose syndrome” (Beule 2010; Scheithauer 2010), with post-decongestion values on both sides that are characteristic of an excessively wide nose (hydraulic diameter after decongestion >6.5 mm) with marked turbulence (λ > 0.03), in the graph prior to and after decongestion, there is pure turbulence at a flow <250 ml/s.
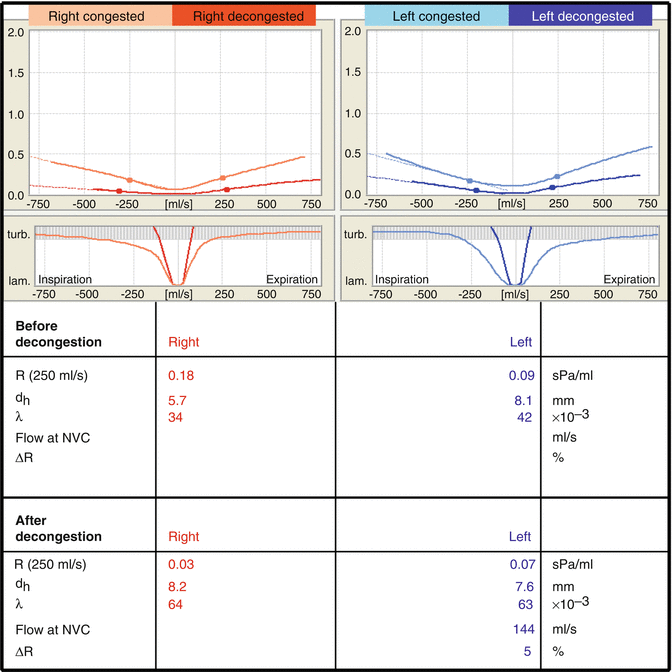

Fig. 27.7
Results of rhinoresistometry measurements in a patient with “empty nose syndrome”
27.2.2 Measuring the Nasal Diffuser Using Acoustic Rhinometry (ARM)
ARM is presented in detail in Chap. 26 Here, we will describe in addition how acoustic rhinometry can be used to obtain evidence about the causes of pathological turbulence in the nose (Fig. 27.8).
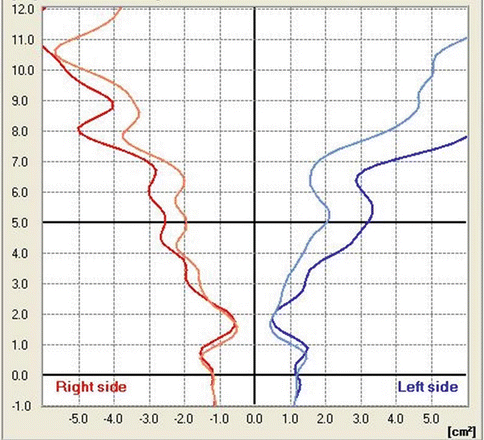

Fig. 27.8
Results of ARM. The nasal diffuser is marked in color on both sides (right, red; left, blue; before decongestion, light; after decongestion, dark)
The occurrence of turbulence in a diffuser rises directly in proportion to increases in the cross-sectional area and to decreases in the size of the diffuser entry opening (see Sect. 23.4).
The entry opening in the nasal diffuser corresponds to the inner nasal valves and thus to MCA1 as calculated by acoustic rhinometry. It is only when there is a ballooning phenomenon present that the diffuser starts out already at the external nasal ostium.
Increases in cross-sectional area along the nasal diffuser are evaluated by measuring the diffuser opening angle φ. This indicator is used in fluid physics in order to characterize cross-sectional expansion in circular diffusers (Fig. 27.9).
In accordance with this principle, the opening angle φ is calculated for the nasal diffuser (anterior cavum) using the cross-sectional area measured by ARM (Fig. 27.10). The angle φ indicates the occurrence of turbulence in the nose in the inspiratory flow direction.
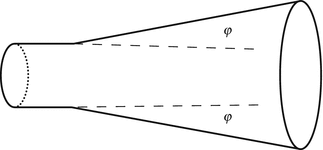
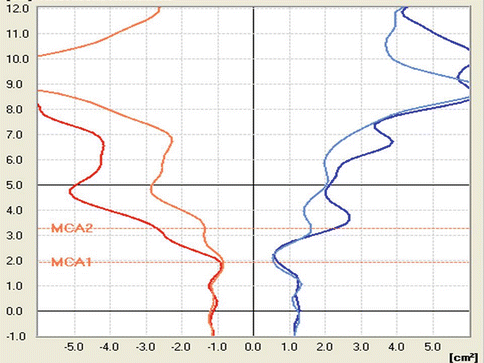

Fig. 27.9
Schematic representation of the diffuser opening angle φ in a circular diffuser

Fig. 27.10
Results of acoustic rhinometry measurements with a deformed diffuser on the right (marked in red). With the help of a regression scale (………..), the diffuser opening angle φ can be calculated
The diffuser angle in relation to triggering nasal turbulence can be assessed using the reference values in Table 27.5.
Table 27.5
Reference values for the diffuser opening angle φ in relation to triggering turbulence in the nose
Turbulence in the nose | Diffuser opening angle φ |
|---|---|
Slight turbulence formation | <7° |
Moderate turbulence formation | 7°–9° |
Severe turbulence formation | >9° |
In the presence of a pathological friction coefficient λ > 0.03 as measured by RRM, the diffuser opening angle provides information about one possible cause of the high level of turbulence. Figure 27.10 shows the results of ARM with a large diffuser opening angle on the right, especially after decongestion.
It has to be considered that even if the opening angle in the nasal diffuser plays the principal part in the occurrence of turbulence, structures other than a narrow diffuser entry opening (e.g., a deformed nasal vestibule, bands, or spurs) may also increase the level of turbulence in the nose.
27.2.3 Long-Term Rhinoflowmetry (LRM)
LRM was developed because RMM, RRM, and ARM only allow for estimating nasal obstruction at a certain time point of the measurement (Lang et al. 2003). Some patients complain about symptoms that occur at other times of the day. LRM makes it possible to measure nasal flow separately for each side of the nose, along with heart rate to serve as an index for physical activity over a 24-h time period under the patient’s everyday conditions of life. Nasal flow is measured using standard commercial nasal oxygen cannulas and the heart rate using standard EVG electrodes. Recording is performed by means of a battery-powered portable device (Fig. 27.11).
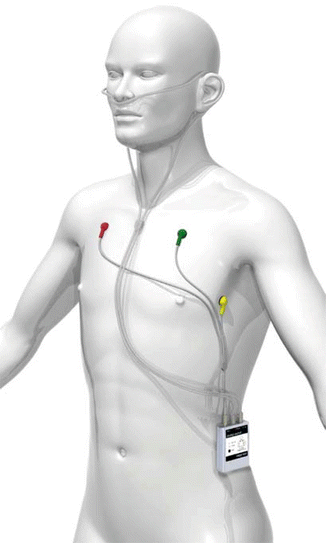

Fig. 27.11
Measurement system for long-term rhinoflowmetry
Figure 27.12 illustrates the graphical curves resulting from an LRM examination. The upper graph presents the maximal nasal flow values during inspiration separately for each side of the nose in relation to time. The lower graph shows the heart rate for estimating physical activity, respiratory rate, as well as nasal minute ventilation in relation to time.
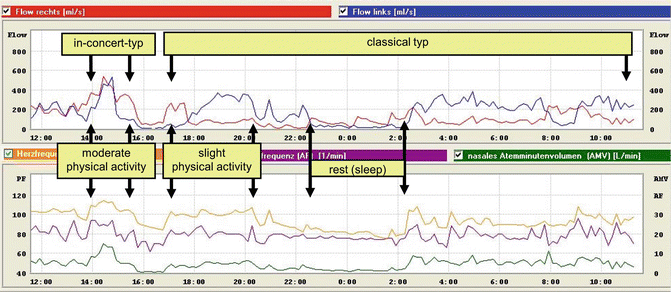

Fig. 27.12
Findings from LRM in a person with normal nasal breathing. To better grasp the relation between physical activity and mucosal congestion in the nose, in this figure the type of cycle and the amount of physical activity were marked. x-axis: time of day in hours. y-axis: upper graph, nasal respiratory velocity at maximal inspiration in ml/s (red right nose, blue, left nose). Lower graph: orange, heart rate (HF); green, nasal respiratory minute volume (NMV) in l/min; purple, respiratory rate (AF)
27.2.3.1 Upper Graph (Figs. 27.12 and 27.13)
The flow-time curves allow for the visual assessment of the nasal cycle at a glance. At physical rest or light physical activity, a “classical type” of nasal cycle should occur, with reciprocal alternation between the two sides of the nose in working and resting phases. With increasing physical activity, the simultaneous transition of both sides of the nose into the working phase (the “in-concert” cycle) may be seen as a physiological response to increased oxygen demand. In this situation, the nasal flow in both sides should reach between 250 ml/s and 500 ml/s, as shown in Fig. 27.12. These flow velocities could not be reached in the presence of increased nasal air resistance with the deployment of mouth-bypass breathing. An example is shown in Fig. 27.13.
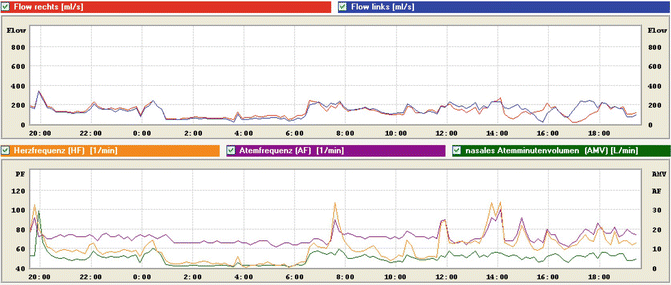

Fig. 27.13
Findings from LRM with bilateral nasal obstruction. The nasal respiratory minute volume (green curve) suggests mouth-bypass breathing during the day (values under 10 l/m, with the exception of the 8:00 PM value) and complete mouth breathing at night between 1:00 AM and 6:00 AM as a result of nasal obstruction
27.2.3.2 Lower Graph (Figs. 27.12 and 27.13)
27.2.3.2.1 Heart Rate (Orange Curve)
Heart rate is used as an index of physical activity.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


