Infectious Diseases
Alex V. Levin
Thomas W. Wilson
Nasrin Najm-Tehrani
Virtually every infectious disease may affect the eye either through direct infection, hematogenous spread, contiguous spread, or complications related to a primary infection at another site. This chapter focuses on ocular complications of systemic and remote infection. Diagnosis of the ocular manifestation might require culture from a site remote from the eye or, less commonly, sampling of intraocular fluids or tissues. Given the difficulty in obtaining intraocular tissues for culture, careful attention to remote sites for diagnostic culture or titers becomes essential.
Suspicion of an infectious cause for an ocular abnormality might stem from the presence of systemic signs such as fever, shock, or other more localized indicators. The presence of infection in the cerebrospinal fluid or blood is particularly worrisome with regard to potential ocular involvement. Transplacental spread of infection to a fetus may present with multiorgan system involvement or even malformations. Taking a careful history is another powerful diagnostic tool and should include queries regarding contacts and exposures, course of the illness, other systemic indicators of infection, treatment with antibiotics or other agents, contact with pets and other animals, travel, and, in the case of suspected fetal infection, pregnancy history. Diagnostic studies on family members (e.g., the mother in a case of suspected fetal infection) may be appropriate in some circumstances.
Some ocular complications of systemic and remote infectious disease are treated by topical or intraocular agents, whereas others require systemic treatment. When diagnostic tissue culture is not obtainable, broad-spectrum antibiotic coverage may be appropriate. The American Academy of Pediatrics Red Book is a particularly useful reference for diagnosis and treatment guidelines.
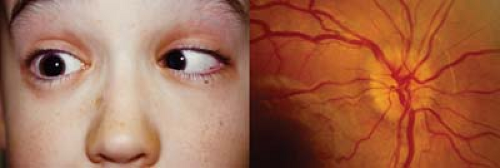 Figure 19.1 Gradenigo Syndrome Aggressive bacterial otitis media can lead to involvement of the petrous bone and mastoid. Cranial nerve VI runs over the intracranial petrous bone on its way to the ipsilateral lateral rectus muscle. Inflammation in the intracranial space can result in an abduction deficit, as shown in this child’s right eye (Chapter 1: Strabismus, Fig. 1.51). Other diagnostic findings include otitis media, papilledema from increased intracranial pressure, signs of systemic illness (in particular pain, fever, and headache), and diagnostic inflammatory signs in the region of the petrous bone with or without mastoiditis on computed tomography scan or magnetic resonance imaging. |
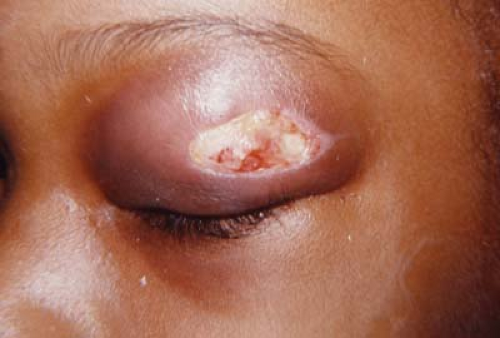
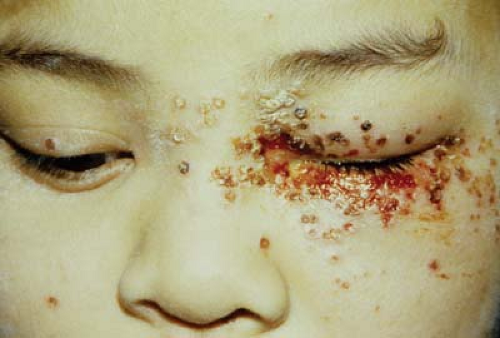 Figure 19.5 Herpes Simplex Herpes simplex virus type I (and less commonly type II) primary infection typically occurs within the first decade following contact with an adult with oral herpes and presents with aphthous stomatitis, dermatitis, or conjunctivitis. The herpes simplex virus becomes latent within the trigeminal ganglion. Factors that may cause recurrence include stress, ultraviolet radiation, menses, fever, and trauma. The skin lesions typically clear within 1 to 2 weeks without significant scarring, although they may become secondarily infected with bacteria and cause a preseptal cellulitis. Approximately 25% of patients with primary herpetic conjunctivitis will develop keratitis including superficial punctate keratitis, subepithelial infiltrates, and possibly dendrites. Patients with primary herpetic conjunctivitis should be treated with topical antiviral ointment or drops.
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|