8 FUNGAL INFECTIOUS DISEASE
Fungal Keratitis
Nicky R. Holdeman
ICD-9: 370.05
 THE DISEASE
THE DISEASE
Pathophysiology
Fungal keratitis results from invasion of the cornea by a fungal organism. While fungi are ubiquitous, they are responsible for a relatively small percentage of overall corneal infections worldwide. Unfortunately, however, because of the difficulty in diagnosing and treating these infections, they often result in devastating ocular consequences. The incidence of fungal keratitis has risen substantially in the last 20 to 30 years, probably due to the increased use of topical corticosteroids and broad spectrum antibiotics and due to better diagnostic techniques.
Etiology
Fungal organisms include single cell yeasts, such as Candida, and multicellular filamentous fungi, such as the Fusarium species. Fungi do not invade the cornea easily and seem to require epithelial trauma, contact lens wear, ocular surface disease, corneal surgery, chronic keratitis, or immunosuppression for infection. The most common organism responsible for fungal keratitis on a worldwide basis is Aspergillus; however, keratomycosis is climate specific. In the southern United States, Fusarium is the most common cause of keratomycosis, whereas Candida and Aspergillus are isolated most frequently in the northern states. Up to 70 different fungi have been implicated as etiologic agents of fungal keratitis (Figs. 8-1 and 8-2).
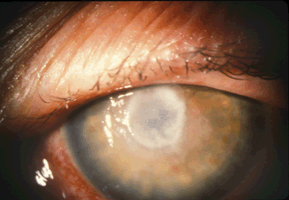
Figure 8-1. Fusarium keratitis.
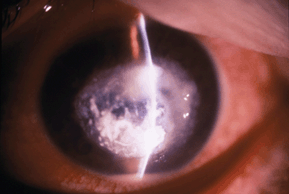
Figure 8-2. Fusarium keratitis with hypopyon.
The Patient
The clinical presentation of keratomycosis may vary—the findings in a filamentous fungal keratitis may be somewhat different than those seen in a yeast infection. The patient’s immune status, duration of involvement, and prior treatment may also modify the findings.
Clinical Symptoms
- Pain
- Conjunctival redness
- Light sensitivity
- Tearing/discharge
- Foreign body sensation
Clinical Signs
- Conjunctival injection (but may be minimal)
- Epithelial defect (or less commonly an intact and slightly elevated epithelium)
- Gray or grayish-white leukocytic stromal infiltrate often with an irregular feathery border
- Anterior chamber reaction; possibly hypopyon with fibrinoid aqueous
- Dry, rough, or gritty texture in the area of involved cornea
- Satellite lesions surrounding the primary infiltrate
- Endothelial plaque
Note: While some of these findings may be useful in raising ones level of suspicion for a fungal infection, in actuality, fungal keratitis has no pathognomonic appearance. It is often difficult to clinically differentiate between fungal and bacterial keratitis.
- Dry, rough, or gritty texture in the area of involved cornea
Demographics
While keratomycosis may affect either sex, there seems to be a higher incidence in men, especially in farm workers and other outdoorsmen. In the southern United States, there is a bimodal distribution of occurrence with greater frequencies in the spring and late fall to early winter.
Incidence is estimated to be approximately 1,500 cases per year in the United States, accounting for up to 5% to 10% of all corneal infections.
Significant History
The history should cover the known risk factors associated with fungal keratitis. The following information should be obtained:
- Has the patient sustained corneal trauma, especially with organic material? (Infection usually occurs 36 to 48 hours after trauma, often slowly progressive.)
- Is the patient systemically or topically immunocompromised?
- Does the patient have any chronic systemic diseases, especially diabetes mellitus?
- Does the patient wear extended contact lenses or a therapeutic bandage lens? (Fungal infection has been reported in contact lens wearers, but bacterial keratitis is more common in these patients.)
- Does the patient have a chronic preexisting ocular surface disorder that may compromise the epithelium (e.g., exposure keratitis, keratitis sicca, herpes simplex keratitis, prior keratoplasty, etc.)?
Ancillary Tests
Diagnosing keratomycosis is often difficult. The primary obstacle in many cases is a failure to suspect a fungal etiology. It is therefore important for a clinician to perform a prompt and thorough laboratory investigation. One should complete the same culture procedure as previously described in the section on bacterial keratitis; however, several points should be emphasized.
1. Scraping the cornea with a sharpened Kimura spatula or a No. 15 scalpel blade is required to enhance the retrieval of fungal elements. The base and leading edge of the infiltrate should be vigorously scraped and then incubated on blood agar, thioglycolate broth, and Sabouraud’s agar (without cyclohexamide) without breaking the surface of the media. (Cyclohexamide is an inhibitant of saprophytic fungi, which are considered contaminants elsewhere in the body, but can be potential pathogens of the cornea.)
- Growth of fungi in culture is usually identifiable within 2 to 7 days, but cultures should be held for 3 weeks before discarding them as negative.
- Occasionally, patients will have a mixed bacterial-fungal, herpetic-fungal, Acanthamoeba-fungal, or mixed fungal keratitis.
- If keratomycosis is the suspected diagnosis, yet the cultures are negative at 48 to 72 hours and the patient is not improving on antibacterial therapy, confocal microscopy or a corneal biopsy may be necessary to identify the infection deep in the stroma. If biopsy fails to confirm keratomycosis and the ulcer is progressing, an anterior chamber paracentesis may be considered to analyze the hypopyon, but this procedure is rarely indicated.
2. Scrapings should also be used to make thin smears for Gram, Giemsa, or Gomori methenamine silver stains. Gram stains may help to identify yeast forms of fungi (e.g., Candida), while Giemsa stain is more likely to define filamentous fungi (e.g., Fusarium, Aspergillus, Cephalosporium). Occasionally, specialized stains (i.e., potassium hydroxide with calcofluor white; acridine orange; etc.) and media (i.e., brain-heart infusion broth) are required to identify the more fastidious organisms.
Note: Diagnosis requires laboratory confirmation and should never be made solely on the basis of the history or the appearance of the cornea. DNA amplification using polymerase chain reaction–based assay is a useful method for rapid and sensitive diagnosis of fungal keratitis, although specificity and availability may be an issue.
- Confocal microscopy may also be used to facilitate the diagnosis.
3. Sensitivities of isolated fungi to various antifungal agents can only be performed in a few specialized laboratories, such as the CDC in Atlanta. It is recommended that isolated organisms should not be discarded so that additional studies could be performed at one of these sites in the event the patient does not respond to therapy.
The Treatment
Typically, most infectious corneal infiltrates and ulcers are treated empirically with broad spectrum antibacterial therapy unless fungal elements are seen on smears or fungi are isolated on cultures. Interestingly, certain topical antibiotics (i.e., chloramphenicol, moxifloxacin, and tobramycin) as well as BAK have a modest effect on Fusarium and Aspergillus. Antifungal therapy of a corneal ulcer is usually not used until a definitive diagnosis is made.
Specific medical therapy for keratomycosis is somewhat limited by FDA-approved topical antifungal agents and by the poor penetration into ocular tissues. If studies verify a fungal etiology, typical management often includes the following measures:
1. Currently, natamycin, 5% suspension (Natacyn), is the only commercially available, FDA-approved antifungal agent for topical use. It is a polyene agent that is most effective against filamentous fungi such as Fusarium but is also active against some yeast. A typical regimen would be one drop q1–2h for 1 to 4 days at which time it can usually be reduced to one drop six to eight times daily depending on clinical response. Several months of therapy may be required to assure that the organism has been eliminated—the standard treatment course is about 12 weeks. While natamycin is well tolerated by the eye, refractory cases may require the addition of other topical, subconjunctival, intrastromal, or systemic antifungal drugs (e.g., amphotericin B, flucytosine, itraconazole, fluconazole, econazole, voriconazole, miconazole, clotrimazole, or ketoconazole). Targeted delivery of voriconazole by intrastromal injection may be beneficial in the treatment of recalcitrant fungal keratitis. Systemic antifungal agents are typically employed in patients with severe keratitis, scleritis, impending perforation, and endophthalmitis.
2. Epithelial debridement and debulkment of necrotic tissue often aids drug penetration into the cornea. However, excessive scraping may be associated with worse outcomes in regards to BCVA following resolution of the infection.
3. Cycloplegics (e.g., scopolamine 0.25% t.i.d.) are used to prevent synechiae formation, reduce inflammation, and increase patient comfort.
4. Intraocular pressures should be monitored and secondary glaucoma controlled as needed (see glaucoma section).
5. Topical corticosteroids are contraindicated during early therapy of a fungal ulcer as they may exacerbate the infection, cause an inflammatory rebound, and ultimately worsen the prognosis. Topical antifungal agents are typically fungistatic and efficacy may vary. After several weeks of effective antifungal therapy and documented clinical improvement, topical steroids are sometimes judiciously employed to decrease corneal inflammation and scarring with the continued use of antifungal agents. However, most clinicians would agree that steroids are best avoided in a confirmed case of fungal keratitis, unless the benefits clearly outweigh the substantial risks.
- Clinical signs of response to treatment are initially an arrest of progression, decreasing infiltrate size and opacity, blunting of the leading edge of the infiltrate, and resolution of a hypopyon.
- Unfortunately, even with early, appropriate, and aggressive treatment, patients with fungal keratitis sometimes proceed to corneal perforation or develop keratoscleritis or endophthalmitis. Since these patients have a higher risk of graft rejection than patients with corneal opacification due to noninflammatory conditions, keratoplasty should be considered early in patients not responding to aggressive medical therapy to try and prevent these sight-threatening complications.
- Lamellar keratoplasty (LK) may be an option if the ulcer does not involve all corneal layers. Penetrating keratoplasty (PK) is indicated when there is a full-thickness corneal infection, corneal perforation, or recurrence after LK. If PK is performed, the excision should encompass the entire infiltrate plus 1 mm of clear cornea.
Note: Cyclosporine A (Restasis) has been shown to possess antifungal activity and may allow some degree of steroid-free inflammation control in a patient with a sight-threatening fungal keratitis. Topical cyclosporine may also help prevent allograft rejection in patients incurring corneal transplant after mycotic infections.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


