Purpose
To analyze a single center’s experiences with ocriplasmin on vitreomacular traction (VMT) and the rate of VMT release, full-thickness macular hole (full-thickness MH) closure, and best-corrected visual acuity (BCVA) changes.
Design
Retrospective interventional case series.
Methods
Single-center study of 58 eyes of 56 patients who received intravitreal ocriplasmin for VMT with or without full-thickness MH. VMT release, full-thickness MH closure, visual acuity changes, and anatomic characteristics on spectral-domain optical coherence tomography (SD OCT) were analyzed.
Results
VMT resolved in 29 of 58 eyes (50%) and nonsurgical closure of full-thickness MH was achieved in 4 of 15 eyes (27%). Mean logMAR BCVA among all treated eyes improved from 0.51 (20/65) at baseline to 0.36 (20/46) at final follow-up ( P = .0018) with mean follow-up of 8.7 months. When compared to eyes without VMT release, eyes with successful vitreomacular release had a better pretreatment BCVA (20/48 vs 20/89, P = .004) and final follow-up BCVA (20/31 vs 20/68, P = .0001). Improvement in BCVA was significant in eyes with VMT release ( P = .0001). Transient ellipsoid zone changes were noted in 26% of treated eyes (n = 15), of which 14 had successful VMT release. Transient subfoveal fluid accumulation was noted in all these patients with vitreomacular release. Mean time to resolution of ellipsoid zone changes was within 38 days.
Conclusion
In clinical practice, intravitreal injection of ocriplasmin achieved VMT release in approximately one half of treated eyes, with a 27% closure rate for full-thickness MH. Transient ellipsoid changes were evident in 26% of treated eyes, more common in eyes with successful VMT release.
Separation of the vitreous body from the internal limiting membrane of the retina is a common event as a person ages. This separation is facilitated by degradation of a rich extracellular matrix between the inner limiting membrane and posterior vitreous cortex, a matrix that is composed of fibronectin, laminin, and other extracellular components. When this matrix fails to completely dissolve, the incomplete vitreoretinal separation and persistent attachment at the vitreomacular interface produces vitreomacular adhesion (VMA), which can progress to the vitreomacular traction (VMT) if anatomic distortion of the fovea is present. This can lead to a full-thickness macular hole (full-thickness MH).
Natural history studies indicate a spontaneous release rate of VMT in 11%–47% of cases over a mean time frame of 8–60 months. Even with spontaneous release, abnormal structural changes in the macula and decreased visual acuity can persist, especially in more chronic or severe cases of VMT. For VMT associated with full-thickness MH, spontaneous closure rates are much lower, occurring in only 3%–11% of cases. Most macular holes enlarge, with a progression rate of 71%–75% from stage II to stage III/IV. Full-thickness macular holes can result in significant decreases in visual acuity that may persist and be irreversible if left untreated for a long time frame.
Traditional treatment for VMT and full-thickness MH includes surgical disruption of the vitreoretinal interface via pars plana vitrectomy (PPV) by mechanically removing the vitreous and relieving its attachment to the macula. Closure rates for macular holes with current vitrectomy techniques are typically 88% or higher. Ocriplasmin (Jetrea; ThromboGenics, Iselin, New Jersey, USA) is a recombinant human serine protease with proteolytic activity against various components of the vitreous and vitreoretinal interface, thereby facilitating chemical separation of the vitreous from the retina. In phase III testing, the efficacy of ocriplasmin for VMT release was reported to be 26.5%, but ranges can be as high as 41%–75%, depending on the presence of positive predictive criteria, including age less than 65 years, focal adhesions less than or equal to 1500 μm, presence of full-thickness MH, phakic status, and absence of epiretinal membrane. In this same report, cases with VMT associated with full-thickness MH treated with ocriplasmin had hole closure rates of 40%.
To date, the literature is limited with regard to real-world experience with ocriplasmin after FDA approval and commercialization of the drug. This study examines a single center’s clinical experience with use of ocriplasmin for VMT with or without macular hole.
Methods
Patient Selection and Diagnosis
The Wills Eye Hospital Institutional Review Board approved a retrospective chart review for this retrospective interventional case series of consecutive patients who received intraocular ocriplasmin between January 14, 2013 and March 15, 2014 at Mid Atlantic Retina and the Retina Service of Wills Eye Hospital. Patient charts were reviewed for data collection and all spectral-domain optical coherence tomography (SD OCT) tests were reviewed before and after treatment. Subjects were excluded if they did not have SD OCT evidence of VMT, if they had less than 1 month follow-up, or if they received ocriplasmin without diagnosis of VMT. All patients must have received a single intravitreal injection of ocriplasmin.
Charts were reviewed for patient age; lens status; date of injection; indication for injection; date of noted VMT release, if applicable; date of any vitrectomy surgery, if applicable; presence of full-thickness MH; and closure of the macular hole, if applicable. Visual acuities recorded were best available spectacle-corrected (with and without pinhole) Snellen visual acuity and were noted at time of injection, at 1 week, at 1 month, and at last follow-up. SD OCTs were also concurrently reviewed for presence of VMT and confirmation of release, as well as for subretinal fluid or changes to the ellipsoid junction. Past ocular history was reviewed for accompanying ocular comorbidities, including diabetic retinopathy, age-related macular degeneration, or retinal vein occlusion. Adverse events and complications were reviewed after injection for dyschromatopsia, visual dimming, progression of cataracts, pain, photophobia, and new flashes or floaters.
Ocriplasmin Injection Protocol
Patients with VMT with or without full-thickness MH were treated with a single, intravitreal 125 μg dose of ocriplasmin (Jetrea; ThromboGenics, Iselin, New Jersey, USA). Standard intravitreal injection protocols were used, including topical proparacaine and 5% betadine, lid retraction, no talking or use of a mask, and injection through the pars plana (3.5 mm or 4 mm from limbus for pseudophakic and phakic patients, respectively). Patients were observed for up to 30 minutes following injection and discharged with intraocular pressure of less than 30 mm Hg. Patient head positioning and location of pars plana injection were determined by individual injecting physician discretion and was, therefore, not standardized.
Detection of Vitreomacular Traction and Measurement of Central Retinal Thickness Using Spectral-Domain Optical Coherence Tomography
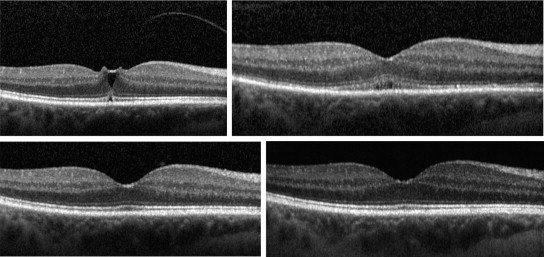
The Heidelberg SD OCT (Heidelberg Engineering, Heidelberg, Germany) was used for all imaging evaluations. The internal limiting membrane, the retinal pigment epithelium, and Bruch’s membrane were identified on all scans centered through the fovea, as determined by the red-free image on the OCT scanner. The presence of VMT was defined as partial attachment of the posterior hyaloid to the internal limiting membrane in the central macula ( Figure 1 ). All SD OCT images were examined qualitatively for the presence or absence of full-thickness macular hole, intra- and subretinal fluid, pigment epithelial detachment, and ellipsoid zone changes. The central retinal thickness was obtained from the center subfield of the macular thickness map. All scans were analyzed by 4 independent masked observers (P.S., A.J., M.F., and S.K.H.); any discrepancies were resolved by an open discussion.
Statistical Analysis
Snellen visual acuities were collected from patients wearing their most recent or best distance correction or best pinhole correction and converted into a logarithm of the minimal angle of resolution (logMAR) score for statistical analysis.
Dependent t test analysis with P < .05 was used to compare differences within groups and independent t test and Fisher exact test was used to compare differences between groups. Clinical outcome measures included SD OCT analysis for vitreomacular interface, subretinal and subfoveal fluid, intraretinal fluid, ellipsoid zone changes, central retinal thickness, mean change from baseline visual acuity, proportion of eyes losing <3 Snellen visual acuity lines, and proportion of eyes gaining ≥3 Snellen visual acuity lines.
Results
Baseline Characteristics
Between January 14, 2013 and March 15, 2014, 67 eyes of 65 patients received a single intravitreal injection of ocriplasmin. Two eyes were excluded that were treated for isolated full-thickness MH without evidence of VMT on SD OCT, and 7 more were excluded for having less than 1 month of follow-up. In total, 58 eyes (38 female, 20 male) of 56 patients were included in this study (30 right eyes and 28 left eyes). The mean age of the patients was 72 years (range 59–94 years). Fifteen eyes had VMT with full-thickness MH. Thirty-seven of the 58 eyes were phakic. Comorbidities found in this cohort includes 23 patients with epiretinal membrane, 12 with diabetic retinopathy (6 with nonproliferative diabetic retinopathy, 2 with proliferative diabetic retinopathy, and 4 without diabetic retinopathy), 8 with age-related macular degeneration (6 with the dry variant and 2 with the wet variant), 1 with central retinal vein occlusion, and 1 with branch retinal vein occlusion. The mean logMAR visual acuity at baseline was 0.51 (20/65, ± 0.367); eyes with full-thickness MH had a logMAR of 0.87 (20/148, ± 0.395) and eyes with isolated VMT had a logMAR of 0.39 (20/49, ± 0.262, P = .0001 in baseline differences between 2 groups).
Spectral-Domain Optical Coherence Tomography and Visual Acuity Outcomes
Ocriplasmin treatment success was stratified into 2 groups: successful release of VMT and closure of full-thickness MH, if present at baseline. Twenty-nine eyes (50%) had VMT release, with a mean and median time to release of 12 and 7 days, respectively (range, 1–48 days). Twenty-six eyes (90%) had resolution of VMT within 28 days. One eye had clinical improvement of VMT in 13 days after the injection, with complete release evident at day 48. Two eyes had a late release of VMT after injection, occurring at 4 months and 6.5 months, respectively.
The mean and median follow-up for all eyes was 258 and 210 days, respectively (range: 35–620 days). At final follow-up, the mean logMAR visual acuity was 0.36 (20/46, ± 0.360, P = .0018 compared to baseline, Table ); full-thickness MH patients had a last follow-up logMAR visual acuity of 0.40 (20/50, ± 0.243, P = .0002 between baseline and follow-up) and patients with isolated VMT had a last follow-up logMAR visual acuity of 0.34 (20/44, ± 0.300, P = .26 between baseline and follow-up). Visual acuity differences between those with macular holes (delta logMAR 0.468, ± 0.362) and those without (delta logMAR 0.044, ± 0.254) were statistically significant ( P = .0001).
| Patient Cohort | VA at First Injection, logMAR (Snellen) | VA at Last Follow-up, logMAR (Snellen) | P Value | Follow-up | Vision Change | Result | |
|---|---|---|---|---|---|---|---|
| All patients (n = 58) | All patients (n = 58) | 0.51 (20/65) | 0.36 (20/46) | .0018 | 1 week (n = 54) | Gain ≥2 lines | 11/54 (20%) |
| Gain ≥3 lines | 9/54 (17%) | ||||||
| Loss ≥2 lines | 7/54 (13%) | ||||||
| Loss ≥3 lines | 5/54 (9%) | ||||||
| Patients with released VMT (n = 29) | 0.38 (20/48) | 0.19 (20/31) | .0001 | 1 month (n = 51) | Gain ≥2 lines | 16/51 (32%) | |
| Gain ≥3 lines | 10/51 (20%) | ||||||
| Loss ≥2 lines | 7/51 (14%) | ||||||
| Loss ≥3 lines | 6/51 (12%) | ||||||
| Patients without released VMT (n = 29) | 0.65 (20/89) | 0.53 (20/68) | .119 | At most recent follow-up (n = 58) (mean 258 days, range 35–620 days) | Gain ≥2 lines | 24/58 (41%) | |
| Gain ≥3 lines | 20/58 (34%) | ||||||
| Loss ≥2 lines | 7/58 (12%) | ||||||
| Loss ≥3 lines | 3/58 (5%) |
In the 29 eyes with VMT release, the pretreatment logMAR visual acuity was 0.38 (20/48, ± 0.259) with a final follow-up logMAR visual acuity of 0.19 (20/31, ± 0.152, P = .0001 compared to baseline, mean follow-up time 8.3 months [248 days] ± 5.0 months [151 days], Table ). Eyes with VMT release with absent macular holes (n = 23) had a mean visual acuity of 0.28 (20/38, ± 0.170) at baseline and 0.16 (20/28, ± 0.147, P = .0018, mean follow-up 7.7 months [231 days] ± 5.3 months [160 days]) at last follow-up. Patients with macular holes and VMT release (n = 6) had a mean visual acuity of 0.75 (20/112, ± 0.209) at baseline and 0.31 (20/41, ± 0.11, P = .0015, mean follow-up 10.5 months [314 days] ± 3.3 months [98 days]) at last follow-up.
The remaining 29 eyes that did not have successful VMT release after injection had a pretreatment logMAR visual acuity of 0.65 (20/89, ± 0.41) and a final logMAR visual acuity of 0.53 (20/68, ± 0.269; P = .119, Table ). However, there was a significant difference in mean visual acuity between eyes that had VMT release and those that did not at baseline (logMAR 0.38 vs 0.65, P = .004) and at final follow-up (logMAR 0.19 vs 0.53, P = .0001). Mean follow-up was 8.9 months (267 days) ± 5.5 months (164 days).
Factors Associated With Vitreomacular Release With Ocriplasmin
Several possible predictors of VMT release were analyzed as established by prior studies. Though statistical significance was not achieved, the absence of epiretinal membrane, phakic lens status, and patient age ≤65 years had higher release rates. Thirty-seven phakic eyes had higher release rates than 21 pseudophakic eyes (57% vs 38%, P = .27). Thirty-five eyes without epiretinal membrane had higher rates of VMT release than the 23 eyes with an epiretinal membrane (57% vs 39%, P = .28). Eleven patients ≤65 years old had greater success with the drug than the 47 patients >65 years old (73% vs 45%, P = .18). All patients in this study had focal VMT, another positive predictor of successful release.
Other factors including macular hole size, sex, and initial visual acuity were also examined. Eyes with macular holes ≤400 μm had release rates of 43% (6 of 14) vs 0% in those with holes >400 μm (0 of 1). Further analysis showed that macular holes ≤250 μm had a release rate of 43% (2 of 6) vs a 50% rate for those between 250 and 400 μm (4 of 8). Overall, successful vitreous release in patients with full-thickness MH was 40% (6 of 15) vs 53% in patients without a full-thickness MH (23 of 43). Male (55%, 11/20) and female subjects (47%, 18/38, P = .78) showed similar release rates. Patients with an initial BCVA ≥ 20/25 had a release rate of 67% (4 of 6) compared to 48% (25 of 52) for those with initial BCVA < 20/25.
Full-thickness MH closure after ocriplasmin injection was also analyzed. Of the 15 eyes that had full-thickness MHs, 6 eyes (40%) measured less than or equal to 250 μm, 8 eyes (53%) were between 250 and 400 μm, and 1 eye (7%) was >400 μm. Four eyes (27%) had complete hole closure following ocriplasmin treatment; 2 were ≤250 μm and 2 were 250–400 μm in size. Ten of the 11 patients (91%) who failed to close underwent vitrectomy for surgical repair with successful closure (mean time to surgery was 52 days, ranging from 22 to 80 days), with the remaining patient scheduled to have surgery at the time of this manuscript preparation. Patients with VMT release after ocriplasmin injection and concurrent pretreatment full-thickness MH (n = 6) had a hole closure rate of 67% (4/6).
The most common adverse events reported after ocriplasmin injection were photopsia and floaters (31% and 26%, respectively). Other reported adverse events include blurriness (n = 7), photophobia (n = 3), distortion (n = 2), and dimming of vision (n = 2). All events were transient and resolved within 1 month. One eye developed mild anterior uveitis that resolved with topical corticosteroid treatment, and 2 eyes developed posterior subcapsular cataracts within 3 months of injection, both of which went on to cataract extraction.
Ellipsoid zone changes in the macula on SD OCT testing was observed in 15 eyes, 14 of which had successful release of VMT and 1 that did not ( Figure 1 ). Mean logMAR visual acuity decreased from 0.43 (20/54, ± 0.339) at baseline to 0.54 (20/69, ± 0.488) at the 1 week follow-up visit, but this was not statistically significant ( P = .49). Eyes with ellipsoid zone changes gradually improved to a visual acuity of 0.22 (20/33, ± 0.192) at last follow-up ( P = .007, mean time of follow-up 7.2 months [216 days], ± 3.8 months [114 days]). All eyes with release of VMT had a concomitant transient development of or increase in subfoveal fluid ( Figure 1 ). All macular ellipsoid zone changes and subretinal fluid were transient and resolved by 3 months (mean of 37 days), with some resolving as early as 2 weeks (as observed on SD OCT at follow-up visits, Figure 1 ).
Of the 54 eyes with a documented visual acuity measurement exactly 1 week after ocriplasmin injection, 7 (13%) had ≥2 lines of visual acuity loss. Of these eyes, 5 (9%) had ≥3 lines of vision acuity loss. Seven of 58 eyes (12%) continued to have ≥2 lines of vision loss at last recorded follow-up, with 3 eyes (5%) continuing to have ≥3 lines of vision loss at last follow-up. Out of the 7 eyes (12%) that continued to have ≥2 lines of vision loss at last recorded follow-up, 5 of the eyes’ vision loss was attributed to failed VMT release, increased macular edema, or worsening of a comorbidity; however, it was impossible to rule out injection-related visual loss in 2 of the eyes. Eleven of 54 (20%) gained ≥2 lines of vision or better within 1 week, of which 9 (17%) gained ≥3 lines of vision. Twenty-four of 58 (41%) gained ≥2 lines of vision or better at final follow-up, of which 20 (34%) gained ≥3 lines of vision ( Table ).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


