Contact lens wear, especially extended-wear soft lenses
 Corneal trauma, foreign bodies
Corneal trauma, foreign bodies
 Ocular surface disease (e.g., exposure/neurotrophic keratopathy, chronic bullous keratopathy, dry eye syndrome, trichiasis, distichiasis, entropion)
Ocular surface disease (e.g., exposure/neurotrophic keratopathy, chronic bullous keratopathy, dry eye syndrome, trichiasis, distichiasis, entropion)
 Topical immunosuppressive therapy (e.g., corticosteroids)
Topical immunosuppressive therapy (e.g., corticosteroids)
 Immunocompromised patient
Immunocompromised patient
 Postoperative: corneal wound or suture-related (e.g., corneal graft)
Postoperative: corneal wound or suture-related (e.g., corneal graft)
Etiology
 Staphylococcus
Staphylococcus
 Streptococcus
Streptococcus
 Pseudomonas
Pseudomonas
 Moraxella
Moraxella
 Atypical mycobacteria, others
Atypical mycobacteria, others
Symptoms
 Pain, irritation, redness, photophobia, discharge, decreased vision, contact lens intolerance
Pain, irritation, redness, photophobia, discharge, decreased vision, contact lens intolerance
Signs
 Vary according to the severity of the infection and, to a lesser extent, the causative organism
Vary according to the severity of the infection and, to a lesser extent, the causative organism
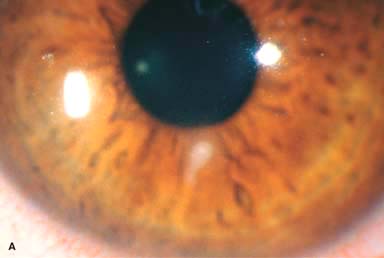
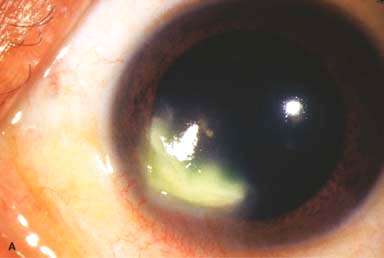
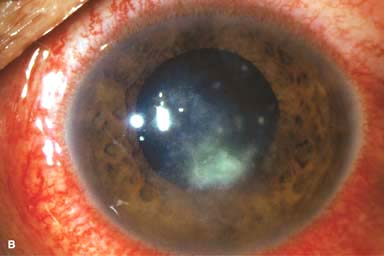
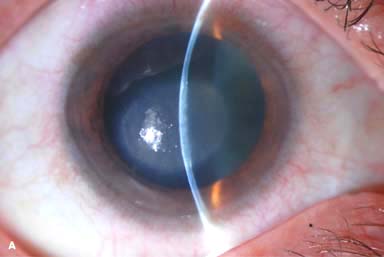
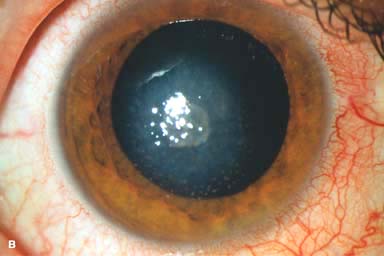
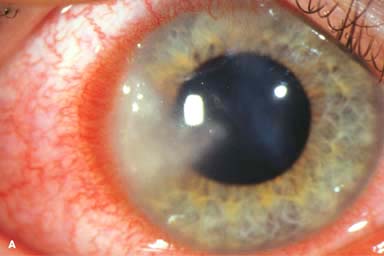
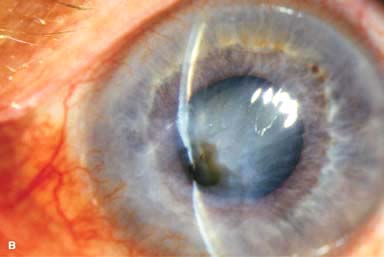
 White stromal infiltrate associated with conjunctival injection and typically with an overlying epithelial defect. There may be stromal loss (ulcer) (Fig. 7-1A and B).
White stromal infiltrate associated with conjunctival injection and typically with an overlying epithelial defect. There may be stromal loss (ulcer) (Fig. 7-1A and B).
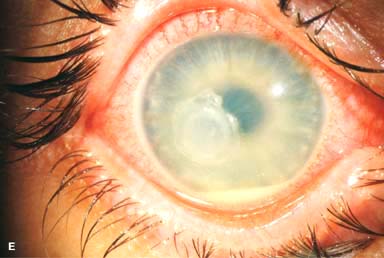
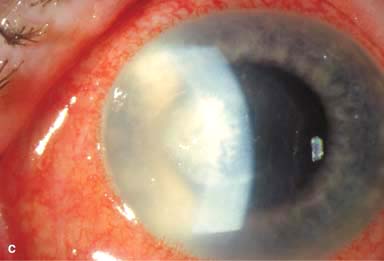
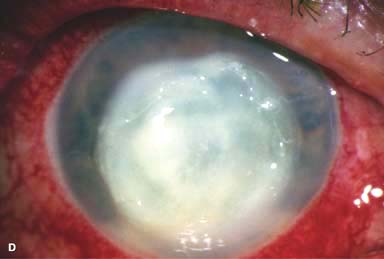
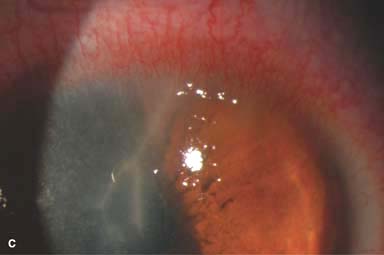
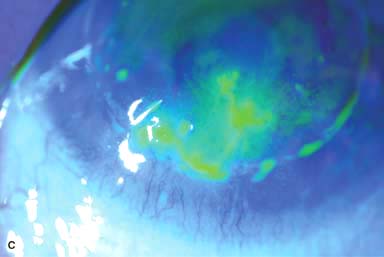
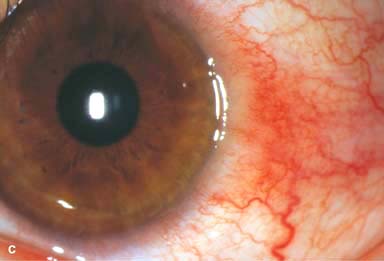
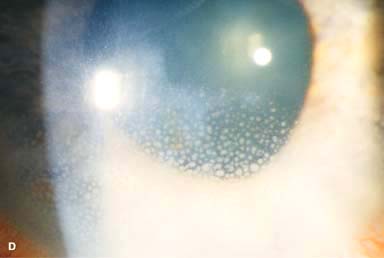
 There may be surrounding stromal edema, Descemet’s folds, secondary reactive iritis, and hypopyon (Fig. 7-1C–H).
There may be surrounding stromal edema, Descemet’s folds, secondary reactive iritis, and hypopyon (Fig. 7-1C–H).
 Staphylococcal keratitis is characterized by a well-defined, white-gray or creamy stromal infiltrate that may enlarge to form a dense stromal abscess.
Staphylococcal keratitis is characterized by a well-defined, white-gray or creamy stromal infiltrate that may enlarge to form a dense stromal abscess.
 Streptococcal keratitis may be suppurative or have a crystalline appearance. Severe anterior uveitis and hypopyon formation are common.
Streptococcal keratitis may be suppurative or have a crystalline appearance. Severe anterior uveitis and hypopyon formation are common.
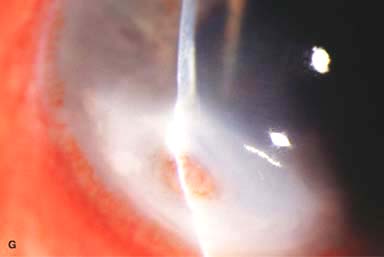
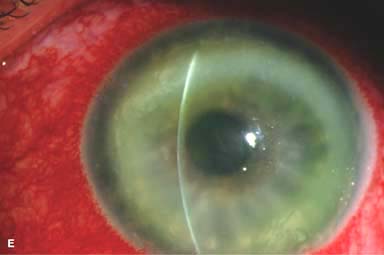
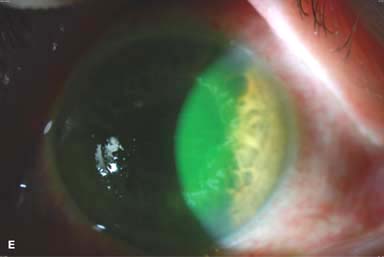
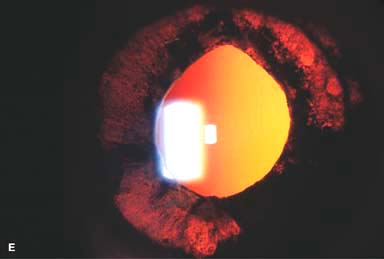
 Pseudomonal keratitis typically presents as a rapidly progressive, suppurative infiltrate associated with hypopyon and a mucopurulent discharge. Corneal perforation may occur (Fig. 7-1G).
Pseudomonal keratitis typically presents as a rapidly progressive, suppurative infiltrate associated with hypopyon and a mucopurulent discharge. Corneal perforation may occur (Fig. 7-1G).
Differential Diagnosis
 Sterile ulcers: vernal shield ulcer, neurotrophic or exposure keratitis, autoimmune keratitis, contact lens–induced sterile keratitis, medicamentosa keratitis. Usually less painful, minimal or no iritis or corneal edema, and culture is negative.
Sterile ulcers: vernal shield ulcer, neurotrophic or exposure keratitis, autoimmune keratitis, contact lens–induced sterile keratitis, medicamentosa keratitis. Usually less painful, minimal or no iritis or corneal edema, and culture is negative.
 Staphylococcal hypersensitivity keratitis: Infiltrates may be bilateral; multiple; peripheral; often located at the 2, 4, 8, or 10 o’clock position; associated with blepharitis; epithelial defect is absent or is smaller than the infiltrate; and there is minimal anterior chamber activity.
Staphylococcal hypersensitivity keratitis: Infiltrates may be bilateral; multiple; peripheral; often located at the 2, 4, 8, or 10 o’clock position; associated with blepharitis; epithelial defect is absent or is smaller than the infiltrate; and there is minimal anterior chamber activity.
 Other microbial (nonbacterial) keratitis: Bacterial cultures are negative. Fungal and special cultures and stains are necessary for diagnosis.
Other microbial (nonbacterial) keratitis: Bacterial cultures are negative. Fungal and special cultures and stains are necessary for diagnosis.
Diagnosis
 Corneal scraping for Gram’s stain, Giemsa stain, calcofluor white stain, cultures, and sensitivity testing. Routine media include blood, chocolate, Sabouraud’s agars, and thioglycolate broths.
Corneal scraping for Gram’s stain, Giemsa stain, calcofluor white stain, cultures, and sensitivity testing. Routine media include blood, chocolate, Sabouraud’s agars, and thioglycolate broths.
 For deep lesions or when repeated cultures are negative in recalcitrant cases, a corneal biopsy may be necessary.
For deep lesions or when repeated cultures are negative in recalcitrant cases, a corneal biopsy may be necessary.
Treatment
 Empirical outpatient treatment with broad-spectrum, topical, nonfortified antibiotic drops may be sufficient for small (2 mm or less) peripheral ulcers with minimal symptoms and minimal anterior chamber activity. Topical fluoroquinolone (e.g., moxifloxacin, gatifloxacin, besifloxacin, levofloxacin, ciprofloxacin, ofloxacin) drops q30–60min around the clock initially, after a loading dose of 1 drop q5min for 15 minutes.
Empirical outpatient treatment with broad-spectrum, topical, nonfortified antibiotic drops may be sufficient for small (2 mm or less) peripheral ulcers with minimal symptoms and minimal anterior chamber activity. Topical fluoroquinolone (e.g., moxifloxacin, gatifloxacin, besifloxacin, levofloxacin, ciprofloxacin, ofloxacin) drops q30–60min around the clock initially, after a loading dose of 1 drop q5min for 15 minutes.
 For larger ulcers or when the ulcers involve the visual axis, or are associated with significant discharge, anterior chamber activity, and hypopyon, treatment may require intensive fortified antibiotic drops. Some patients may need hospitalization. Fortified cefazolin (50 mg/mL) or vancomycin (25 mg/mL) and fortified gentamicin or tobramycin (15 mg/mL). Frequency of instillation: 1 drop q5min for 30 minutes, then q30–60min, of each drop. Wait 5 minutes between administrations of each medication.
For larger ulcers or when the ulcers involve the visual axis, or are associated with significant discharge, anterior chamber activity, and hypopyon, treatment may require intensive fortified antibiotic drops. Some patients may need hospitalization. Fortified cefazolin (50 mg/mL) or vancomycin (25 mg/mL) and fortified gentamicin or tobramycin (15 mg/mL). Frequency of instillation: 1 drop q5min for 30 minutes, then q30–60min, of each drop. Wait 5 minutes between administrations of each medication.
 Subconjunctival antibiotics are necessary only if fortified eye drops cannot be started soon.
Subconjunctival antibiotics are necessary only if fortified eye drops cannot be started soon.
 Oral antibiotics (e.g., moxifloxacin 400 mg q.d., ciprofloxacin 500 mg b.i.d., or levofloxacin 500 mg q.d.) are helpful if the ulcer involves the sclera or has extended into the eye. Systemic antibiotics are also required for Neisseria and Haemophilus infection (e.g., ceftriaxone 1 g IV or IM q12–24h).
Oral antibiotics (e.g., moxifloxacin 400 mg q.d., ciprofloxacin 500 mg b.i.d., or levofloxacin 500 mg q.d.) are helpful if the ulcer involves the sclera or has extended into the eye. Systemic antibiotics are also required for Neisseria and Haemophilus infection (e.g., ceftriaxone 1 g IV or IM q12–24h).
 Cycloplegics are often used to reduce ciliary spasm and to prevent posterior synechiae (e.g., scopolamine 0.25% or atropine 1% t.i.d.).
Cycloplegics are often used to reduce ciliary spasm and to prevent posterior synechiae (e.g., scopolamine 0.25% or atropine 1% t.i.d.).
 Modify regimen according to clinical response and culture and sensitivity results.
Modify regimen according to clinical response and culture and sensitivity results.
 Topical corticosteroids can be used for severe inflammation only after the organism is identified and the infection is under control.
Topical corticosteroids can be used for severe inflammation only after the organism is identified and the infection is under control.
 Urgent corneal transplantation may be necessary in severe cases that are progressing despite aggressive treatment or for ulcers that have perforated.
Urgent corneal transplantation may be necessary in severe cases that are progressing despite aggressive treatment or for ulcers that have perforated.
Prognosis
 Close follow-up is required. Prognosis is very good for small ulcers, good for moderate ulcers, poor for severe ulcers. Better prognosis for ulcers outside the visual axis than ulcers in the visual axis.
Close follow-up is required. Prognosis is very good for small ulcers, good for moderate ulcers, poor for severe ulcers. Better prognosis for ulcers outside the visual axis than ulcers in the visual axis.
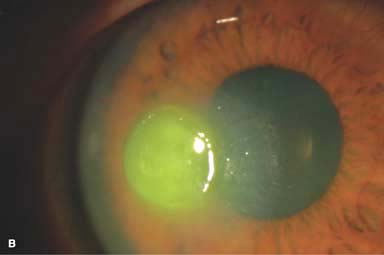
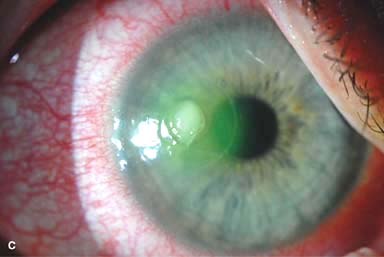
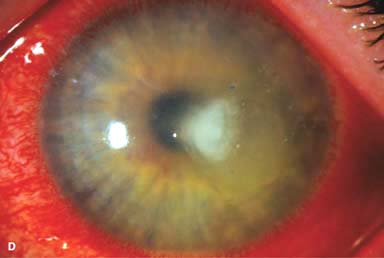
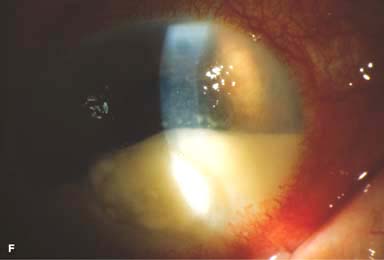
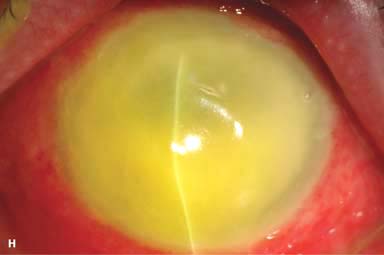
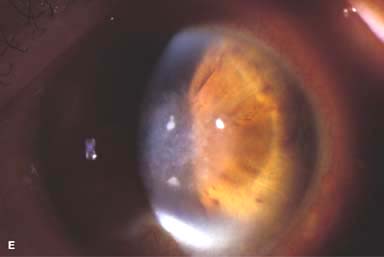
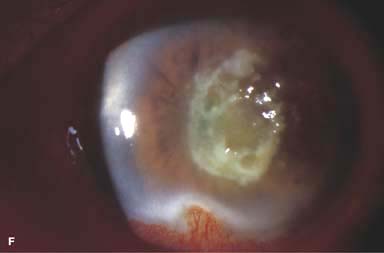
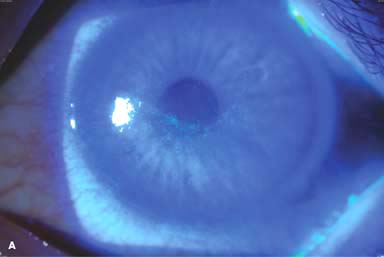
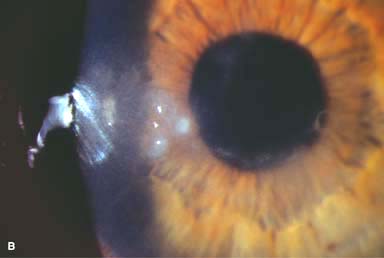
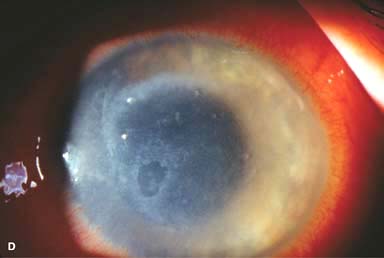
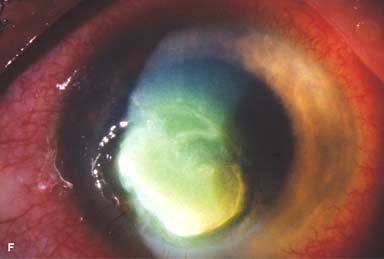
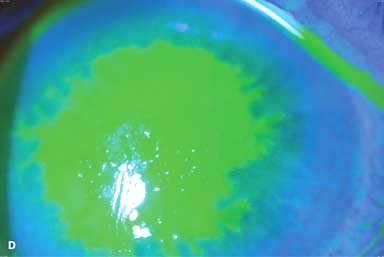
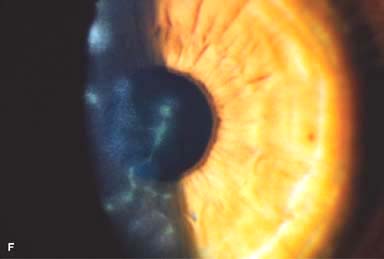
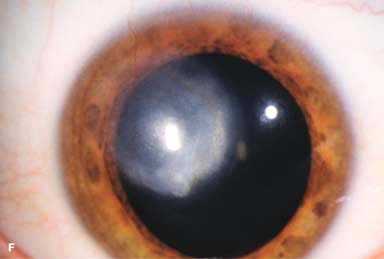
Figure 7-1. Bacterial keratitis. A. This small inferior corneal infiltrate in an overnight soft contact lens wearer has some underlying corneal edema. Because it may be an early infectious keratitis, it should be treated with frequent topical antibiotics and followed closely. B. This moderately large, dense, paracentral, contact lens–related corneal infiltrate has an overlying epithelial defect and surrounding edema. Bacterial keratitis.C. This small to medium-sized paracentral infiltrate is moderately dense. The area of active infiltration is elevated as a result of the inflammatory response. Note also the surrounding edema and the distinct circular immune ring, best seen centrally. D. This dense central corneal ulcer has a large overlying epithelial defect and moderate underlying corneal edema. There is a small hypopyon inferiorly, just blunting the inferior angle. Bacterial keratitis. E. This corneal infection was due to Pseudomonas aeruginosa. There is a large circular corneal ulcer with overlying mucopurulent discharge, underlying corneal edema, and a moderately large hypopyon. F. This large dense corneal ulcer is associated with a hypopyon that fills approximately 50% of the anterior chamber. Bacterial keratitis. G. This infected corneal ulcer caused a perforation. Iris is plugging the wound. The anterior chamber is shallow but formed. H. A total corneal ulceration and epithelial defect is present in this eye. Slit-beam view demonstrates significant central thinning. There is no view of the anterior chamber.
FUNGAL KERATITIS
Fungal keratitis is a very serious, potentially sight-threatening corneal infection that most commonly develops in patients after trauma or in those with a compromised corneal surface.
Etiology
 Nonfilamentous (e.g., Candida): Candida keratitis is a rare, unilateral, insidious fungal infection that usually occurs in eyes with preexisting chronic corneal disease (e.g., dry eyes, herpes keratitis, exposure keratopathy, postkeratoplasty, chronic use of corticosteroid drops) or in severely debilitated patients. Features include a gray-white stromal infiltrate similar to a bacterial ulcer. May have an anterior chamber reaction and hypopyon (Fig. 7-2A and B).
Nonfilamentous (e.g., Candida): Candida keratitis is a rare, unilateral, insidious fungal infection that usually occurs in eyes with preexisting chronic corneal disease (e.g., dry eyes, herpes keratitis, exposure keratopathy, postkeratoplasty, chronic use of corticosteroid drops) or in severely debilitated patients. Features include a gray-white stromal infiltrate similar to a bacterial ulcer. May have an anterior chamber reaction and hypopyon (Fig. 7-2A and B).
 Filamentous (e.g., Aspergillus, Fusarium): Filamentous keratitis is a rare, unilateral, insidious or aggressive fungal infection that frequently affects normal eyes following ocular trauma associated with vegetative matter and in wearers of soft contact lens. Features include a grayish-white infiltrate with indistinct feathery borders, typically surrounded by fingerlike satellite infiltrates in adjacent stroma. The infiltrates may extend beyond the epithelial defect. May have an associated ring infiltrate, anterior chamber reaction, and hypopyon (Fig. 7-2C–F).
Filamentous (e.g., Aspergillus, Fusarium): Filamentous keratitis is a rare, unilateral, insidious or aggressive fungal infection that frequently affects normal eyes following ocular trauma associated with vegetative matter and in wearers of soft contact lens. Features include a grayish-white infiltrate with indistinct feathery borders, typically surrounded by fingerlike satellite infiltrates in adjacent stroma. The infiltrates may extend beyond the epithelial defect. May have an associated ring infiltrate, anterior chamber reaction, and hypopyon (Fig. 7-2C–F).
Symptoms
 Pain, photophobia, tearing, decreased vision; may have a history of trauma, contact lens use or corticosteroid eye drop usage
Pain, photophobia, tearing, decreased vision; may have a history of trauma, contact lens use or corticosteroid eye drop usage
Differential Diagnosis
 Fungal keratitis should be considered in the differential diagnosis of bacterial or herpetic keratitis that does not respond to conventional treatment or that has an unusual history or suspicious appearance.
Fungal keratitis should be considered in the differential diagnosis of bacterial or herpetic keratitis that does not respond to conventional treatment or that has an unusual history or suspicious appearance.
Diagnostic Evaluation
 History of trauma (which is often minor) involving vegetative matter is highly suggestive.
History of trauma (which is often minor) involving vegetative matter is highly suggestive.
 Lack of response to conventional antibacterial therapy
Lack of response to conventional antibacterial therapy
 Corneal scrapings for Gram, Giemsa, calcofluor white, or Gomori methenamine silver stain, and culture (may take up to a week for fungus to grow)
Corneal scrapings for Gram, Giemsa, calcofluor white, or Gomori methenamine silver stain, and culture (may take up to a week for fungus to grow)
 Corneal biopsy may be required if smears and cultures are negative.
Corneal biopsy may be required if smears and cultures are negative.
Treatment
 Topical natamycin 5% (especially for filamentous fungi) and/or amphotericin B 0.15% (especially for Candida) q1h around the clock and taper over 4 to 6 weeks. Patients may require hospitalization initially. Topical voriconazole 1% may also be effective.
Topical natamycin 5% (especially for filamentous fungi) and/or amphotericin B 0.15% (especially for Candida) q1h around the clock and taper over 4 to 6 weeks. Patients may require hospitalization initially. Topical voriconazole 1% may also be effective.
 Oral voriconazole 200 mg b.i.d. or itraconazole or fluconazole 200 to 400 mg loading dose followed by 100 to 200 mg q.d. may be helpful in addition to the intensive topical medications.
Oral voriconazole 200 mg b.i.d. or itraconazole or fluconazole 200 to 400 mg loading dose followed by 100 to 200 mg q.d. may be helpful in addition to the intensive topical medications.
 Cycloplegics (e.g., scopolamine 0.25% or atropine 1% t.i.d.)
Cycloplegics (e.g., scopolamine 0.25% or atropine 1% t.i.d.)
 Corticosteroids are contraindicated.
Corticosteroids are contraindicated.
 Epithelial debridement may facilitate topical therapy by enhancing penetration of antifungals.
Epithelial debridement may facilitate topical therapy by enhancing penetration of antifungals.
 Modify regimen according to clinical response and culture results.
Modify regimen according to clinical response and culture results.
 Therapeutic corneal transplantation may be necessary for unresponsive cases or perforated ulcers. Lamellar keratoplasty is relatively contraindicated because there is a high risk of recurrence of infection.
Therapeutic corneal transplantation may be necessary for unresponsive cases or perforated ulcers. Lamellar keratoplasty is relatively contraindicated because there is a high risk of recurrence of infection.
Prognosis
 Fair for mild to moderate infections; poor for severe infections
Fair for mild to moderate infections; poor for severe infections
Figure 7-2. Fungal keratitis. A. This multilobulated dense infiltrate was caused by a Candida infection. There is an overlying epithelial defect. Peripheral corneal neovascularization suggests that it is a long-standing ulcer. B. This Candida corneal ulcer is slowly improving. The denser infiltrate at the inferior pupillary margin is surrounded by multiple satellite lesions. Fungal keratitis. C. This dense white infiltrate with feathery borders was a result of a Fusarium infection. A ring infiltrate is beginning inferiorly. D. This large central patchy corneal infiltrate and hypopyon enlarged rapidly over several days, leading to an urgent corneal transplant. Histopathology demonstrated numerous filamentous fungi. Fungal keratitis.E. Several months after removal of a corneal foreign body, a patchy central corneal infiltrate is seen. There is also old inferior scarring and neovascularization. Initial cultures were negative. F. Two months later, the eye seen in E has worsened and has a much more dense central infiltrate. Cultures at this point grew Alternaria, which eventually responded to topical and oral voriconazole.
Acanthamoeba Keratitis
Acanthamoeba keratitis is a rare parasitic infection of the cornea associated with the use of soft contact lenses and inadequate contact lens hygiene (e.g., using tap water or home-made saline solution, swimming or hot tub use while wearing contact lenses), and occasionally, trauma. It should be considered in nonhealing, culture-negative keratitis.
Etiology
 Acanthamoeba species
Acanthamoeba species
Symptoms
 Severe pain out of proportion to severity of keratitis, redness, tearing, decreased vision, photophobia, minimal discharge. Symptoms typically develop over a period of weeks, but onset can be more rapid.
Severe pain out of proportion to severity of keratitis, redness, tearing, decreased vision, photophobia, minimal discharge. Symptoms typically develop over a period of weeks, but onset can be more rapid.
 History of soft contact lens use and occasionally trauma
History of soft contact lens use and occasionally trauma
Signs
 Epithelial or subepithelial infiltrates appearing as pseudodendrites early on (Fig. 7-3A and B)
Epithelial or subepithelial infiltrates appearing as pseudodendrites early on (Fig. 7-3A and B)
 Patchy anterior stromal infiltrates may be present early on.
Patchy anterior stromal infiltrates may be present early on.
 Radial keratoneuritis (Fig. 7-3C)
Radial keratoneuritis (Fig. 7-3C)
 A nonsuppurative stromal ring infiltrate, often with variable epithelial breakdown, can develop over weeks. The degree of inflammation is disproportionately mild relative to the amount of pain (Fig. 7-3D–F).
A nonsuppurative stromal ring infiltrate, often with variable epithelial breakdown, can develop over weeks. The degree of inflammation is disproportionately mild relative to the amount of pain (Fig. 7-3D–F).
 In advanced cases, corneal thinning or perforation, scleritis, or hypopyon may develop.
In advanced cases, corneal thinning or perforation, scleritis, or hypopyon may develop.
Differential Diagnosis
 Herpes simplex keratitis
Herpes simplex keratitis
 Fungal keratitis
Fungal keratitis
 Bacterial keratitis
Bacterial keratitis
Diagnosis
 Pain disproportionate to severity of inflammation
Pain disproportionate to severity of inflammation
 Lack of response to antibacterial and antiviral therapy
Lack of response to antibacterial and antiviral therapy
 Ring infiltrate and radial keratoneuritis are highly suggestive.
Ring infiltrate and radial keratoneuritis are highly suggestive.
 Corneal scrapings for Gram, Giemsa, or calcofluor white stain for amoebic cysts
Corneal scrapings for Gram, Giemsa, or calcofluor white stain for amoebic cysts
 Culture on non-nutrient agar with Escherichia coli overlay or special media (e.g., buffered charcoal yeast extract agar).
Culture on non-nutrient agar with Escherichia coli overlay or special media (e.g., buffered charcoal yeast extract agar).
 Corneal biopsy may be necessary if smears and cultures are negative.
Corneal biopsy may be necessary if smears and cultures are negative.
Treatment
 Polyhexamethylene biguanide (PHMB) 0.02% drops q1h. Chlorhexidine 0.02% can be used as an alternative to PHMB.
Polyhexamethylene biguanide (PHMB) 0.02% drops q1h. Chlorhexidine 0.02% can be used as an alternative to PHMB.
 Propamidine isethionate 1% (e.g., Brolene) drops q1h.
Propamidine isethionate 1% (e.g., Brolene) drops q1h.
 Oral voriconazole 200 mg b.i.d. or itraconazole 200 to 400 mg q.d. may be used in addition to the topical medications.
Oral voriconazole 200 mg b.i.d. or itraconazole 200 to 400 mg q.d. may be used in addition to the topical medications.
 Other drops (e.g., clotrimazole 1%) may be added, depending on the severity or treatment response of the infection.
Other drops (e.g., clotrimazole 1%) may be added, depending on the severity or treatment response of the infection.
 Cycloplegics (e.g., scopolamine 0.25% or atropine 1% t.i.d.)
Cycloplegics (e.g., scopolamine 0.25% or atropine 1% t.i.d.)
 Low-dose topical corticosteroids may be helpful in reducing inflammation once the infection appears to be under control.
Low-dose topical corticosteroids may be helpful in reducing inflammation once the infection appears to be under control.
 Oral nonsteroidal anti-inflammatory agents or narcotics for pain relief
Oral nonsteroidal anti-inflammatory agents or narcotics for pain relief
 Modify regimen according to clinical response.
Modify regimen according to clinical response.
 Corneal transplantation may be required if medical therapy fails, but there is risk of recurrence.
Corneal transplantation may be required if medical therapy fails, but there is risk of recurrence.
Prognosis
 Fair to good if diagnosed and treated appropriately within the first month or so of development of symptoms; poor if significant corneal involvement is present
Fair to good if diagnosed and treated appropriately within the first month or so of development of symptoms; poor if significant corneal involvement is present
Figure 7-3. Acanthamoeba keratitis. A. A curvilinear, slightly elevated, “pseudodendritic” epithelial irregularity can be seen in this eye with contact lens–related Acanthamoeba keratitis. B. This early Acanthamoeba infection has several subepithelial infiltrates in a linear pattern reminiscent of a dendrite, hence the term pseudodendrite. There was no frank epithelial defect, but there was epithelial irregularity. Acanthamoeba keratitis. C. Classic radial keratoneuritis is very apparent peripherally in this eye with contact lens–related Acanthamoeba keratitis. D. After several weeks, a ring infiltrate can develop, as can be seen especially superiorly. There is a small epithelial defect inferocentrally. Acanthamoeba keratitis. E. A large ring infiltrate is present in this eye. Despite very aggressive medical treatment, this eye required a corneal transplant. F. After several months of antiacanthamoeba treatment, this dense infiltrate is finally scarring. The active infection eventually resolved, but the eye was left with a significant corneal scar.
HERPES SIMPLEX KERATITIS
Herpes simplex virus (HSV) infection is an extremely common condition that affects a major proportion of the population, although most infections are subclinical. The eyes may be affected in primary ocular herpes or in recurrent disease.
Etiology
 HSV type 1: causes infection above the waist, especially of the face, lips, and eyes. Transmitted by close contact. Much more common in the eye than type 2
HSV type 1: causes infection above the waist, especially of the face, lips, and eyes. Transmitted by close contact. Much more common in the eye than type 2
 HSV type 2: causes infection below the waist, particularly of the genitalia. Transmitted sexually, but neonates can be infected during vaginal delivery. Uncommon in the eye
HSV type 2: causes infection below the waist, particularly of the genitalia. Transmitted sexually, but neonates can be infected during vaginal delivery. Uncommon in the eye
PRIMARY OCULAR HERPES
 Unilateral or bilateral facial and/or eye infection
Unilateral or bilateral facial and/or eye infection
Etiology and Epidemiology
 Primary contact with HSV
Primary contact with HSV
 Usually occurs in children or adolescents
Usually occurs in children or adolescents
Symptoms
 Fever, flulike symptoms
Fever, flulike symptoms
 Facial vesicular rash. Ocular redness, pain, decreased vision, and tearing
Facial vesicular rash. Ocular redness, pain, decreased vision, and tearing
Signs
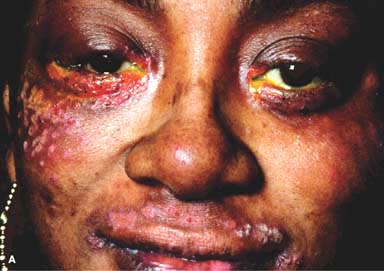
 There may be vesicular blepharoconjunctivitis or periorbital dermatitis. The vesicles usually progress to form crusts (Fig. 7-4). There may be associated acute follicular conjunctivitis with preauricular lymphadenopathy.
There may be vesicular blepharoconjunctivitis or periorbital dermatitis. The vesicles usually progress to form crusts (Fig. 7-4). There may be associated acute follicular conjunctivitis with preauricular lymphadenopathy.
 The cornea may be involved in the form of coarse macropunctate epithelial keratitis or multiple small branching epithelial dendrites without stromal involvement.
The cornea may be involved in the form of coarse macropunctate epithelial keratitis or multiple small branching epithelial dendrites without stromal involvement.
Treatment
 Blepharoconjunctivitis: ganciclovir (e.g., Zirgan) gel, trifluridine (e.g., Viroptic) drops, vidarabine (e.g., Vira-A) ointment, or acyclovir (e.g., Zovirax ophthalmic) ointment five times a day
Blepharoconjunctivitis: ganciclovir (e.g., Zirgan) gel, trifluridine (e.g., Viroptic) drops, vidarabine (e.g., Vira-A) ointment, or acyclovir (e.g., Zovirax ophthalmic) ointment five times a day
 Corneal involvement: ganciclovir (e.g. Zirgan) gel five times a day or trifluridine drops (e.g., Viroptic) nine times a day
Corneal involvement: ganciclovir (e.g. Zirgan) gel five times a day or trifluridine drops (e.g., Viroptic) nine times a day
 Consider acyclovir 200 to 400 mg PO five times a day, valacyclovir 500 mg t.i.d., or famciclovir 250 mg t.i.d. for 7 to 14 days.
Consider acyclovir 200 to 400 mg PO five times a day, valacyclovir 500 mg t.i.d., or famciclovir 250 mg t.i.d. for 7 to 14 days.
 Consider topical antibiotic or acyclovir ointment to help heal skin lesions away from the eyelid margin.
Consider topical antibiotic or acyclovir ointment to help heal skin lesions away from the eyelid margin.
Prognosis
 Good. This is usually a benign and self-limited condition, but the virus subsequently establishes a latent infection in the trigeminal ganglion and may reactivate, especially during periods of physical or emotional stress, causing recurrent disease.
Good. This is usually a benign and self-limited condition, but the virus subsequently establishes a latent infection in the trigeminal ganglion and may reactivate, especially during periods of physical or emotional stress, causing recurrent disease.
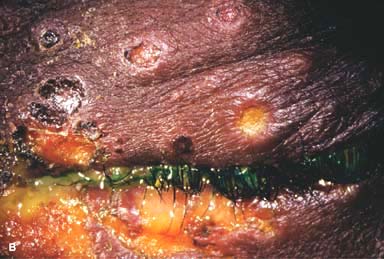
Figure 7-4. Herpes simplex dermatitis. A. This patient had recurrent herpes simplex dermatitis. Note the numerous ulcerated skin lesions around the right eye and cheek. The right eye appears uninvolved, but it should receive prophylactic antiviral treatment because of skin lesions on the eyelid margin. B. Multiple ulcerated skin lesions of herpes simplex can be seen in the upper eyelid. Confluent skin ulcerations are present in the lower eyelid with a mucoid discharge.
RECURRENT OCULAR HERPES SIMPLEX
Recurrent ocular herpes may take the forms of infectious epithelial keratitis, non-necrotizing stromal keratitis (disciform keratitis), necrotizing stromal keratitis, neurotrophic keratitis, and keratouveitis.
Etiology and Epidemiology
 Recurrent HSV is due to a reactivation of latent infection in the trigeminal ganglion, especially during periods of physical or emotional stress.
Recurrent HSV is due to a reactivation of latent infection in the trigeminal ganglion, especially during periods of physical or emotional stress.
 It occurs in children and adults.
It occurs in children and adults.
 It is usually unilateral, but it can be bilateral, especially in immunocompromised patients and those with atopy.
It is usually unilateral, but it can be bilateral, especially in immunocompromised patients and those with atopy.
HSV: EPITHELIAL KERATITIS (DENDRITIC ULCER)
Epithelial keratitis is a common, usually unilateral condition due to the presence of live virus within corneal epithelial cells.
Symptoms
 Unilateral redness, tearing, irritation, decreased vision, photophobia, history of previous episodes
Unilateral redness, tearing, irritation, decreased vision, photophobia, history of previous episodes
Signs
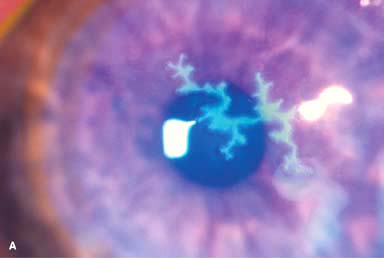
 Single or multiple branching, ulcerating epithelial lesions with raised edges and terminal bulb formation (Fig. 7-5a–C)
Single or multiple branching, ulcerating epithelial lesions with raised edges and terminal bulb formation (Fig. 7-5a–C)
 Enlargement of ulcers can lead to the formation of an amebic-shaped “geographic” ulcer (Fig. 7-5D and E).
Enlargement of ulcers can lead to the formation of an amebic-shaped “geographic” ulcer (Fig. 7-5D and E).
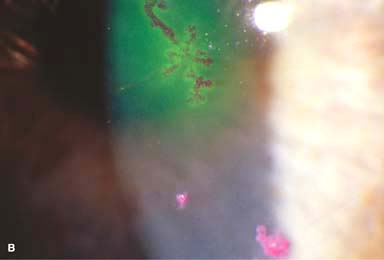
 The ulcer bed stains with fluorescein. The built-up, swollen, opalescent margins of the lesion containing virus-laden cells stain with rose bengal.
The ulcer bed stains with fluorescein. The built-up, swollen, opalescent margins of the lesion containing virus-laden cells stain with rose bengal.
 Anterior stromal haze called “ghost dendrites” may develop below the epithelial lesions (Fig. 7-5F).
Anterior stromal haze called “ghost dendrites” may develop below the epithelial lesions (Fig. 7-5F).
 Corneal sensation is often diminished.
Corneal sensation is often diminished.
Differential Diagnosis
 Herpes zoster keratitis: associated with a history of herpes zoster ophthalmicus with typical skin vesicles found along dermatomal distribution of the face. May have elevated epithelial lesions with tapered ends, which lack terminal bulbs. The entire “mucous plaque dendrite” stains with rose bengal and mildly with fluorescein. Prior to development of the typical zoster rash, early zoster dendrites can look very similar to HSV dendrites.
Herpes zoster keratitis: associated with a history of herpes zoster ophthalmicus with typical skin vesicles found along dermatomal distribution of the face. May have elevated epithelial lesions with tapered ends, which lack terminal bulbs. The entire “mucous plaque dendrite” stains with rose bengal and mildly with fluorescein. Prior to development of the typical zoster rash, early zoster dendrites can look very similar to HSV dendrites.
 Acanthamoeba pseudodendrites
Acanthamoeba pseudodendrites
 Healing epithelial defects
Healing epithelial defects
 Toxic epitheliopathy
Toxic epitheliopathy
Treatment
 Ganciclovir (e.g., Zirgan) gel five times a day, trifluridine (e.g., Viroptic) drops q2h during the day, vidarabine (e.g., Vira-A) ointment five times a day or acyclovir (e.g., Zovirax ophthalmic) ointment five times a day
Ganciclovir (e.g., Zirgan) gel five times a day, trifluridine (e.g., Viroptic) drops q2h during the day, vidarabine (e.g., Vira-A) ointment five times a day or acyclovir (e.g., Zovirax ophthalmic) ointment five times a day
 If the patient is already on corticosteroids, the steroids should be tapered rapidly.
If the patient is already on corticosteroids, the steroids should be tapered rapidly.
 Epithelial debridement can help reduce viral load.
Epithelial debridement can help reduce viral load.
 If there is no response to treatment after 1 week, then poor compliance, resistance to antiviral therapy, antiviral toxicity, or neurotrophic disease should be considered.
If there is no response to treatment after 1 week, then poor compliance, resistance to antiviral therapy, antiviral toxicity, or neurotrophic disease should be considered.
 A short course of systemic acyclovir is unnecessary, because it does not prevent subsequent development of stromal keratitis or uveitis, but it can be used in place of frequent topical antivirals.
A short course of systemic acyclovir is unnecessary, because it does not prevent subsequent development of stromal keratitis or uveitis, but it can be used in place of frequent topical antivirals.
 Consider long-term oral antiviral prophylaxis (e.g., acyclovir 400 mg b.i.d.) if a patient has had multiple episodes of herpetic eye disease.
Consider long-term oral antiviral prophylaxis (e.g., acyclovir 400 mg b.i.d.) if a patient has had multiple episodes of herpetic eye disease.
Prognosis
 Good, but recurrences are common
Good, but recurrences are common
Figure 7-5. Herpes simplex keratitis. A. Fluorescein staining with a cobalt blue light of an active herpes simplex epithelial dendrite. Note the “tree branching” pattern of the dendrite. The central bed stains well with fluorescein, while the elevated edges do not. The ends of the dendrite have classic terminal “end bulbs.” B. Rose bengal dye on this active dendrite stains the heaped-up edges that contain virus-laden cells. Herpes simplex keratitis.C. A recurrent epithelial dendrite is seen in this eye, which is 15 years status post a corneal transplant for herpes simplex keratitis scarring. D. The central area of a very large “geographic” lesion stains readily with fluorescein. The edge of the epithelial defect has herpes simplex dendritic branching and terminal end bulbs. Herpes simplex keratitis.E. Broad slit-beam view of the same eye highlights the classic herpes simplex dendritic features. F. This resolving epithelial dendrite barely stains with fluorescein. There is residual underlying corneal haze in the pattern of the previous dendrite, often termed a “ghost dendrite.”
HSV: NONNECROTIZING STROMAL KERATITIS (DISCIFORM KERATITIS)
Disciform keratitis is a primarily inflammatory condition caused by a hypersensitivity reaction to the herpes simplex viral antigen in the cornea.
Symptoms
 Unilateral redness, tearing, irritation, blurred vision, photophobia, history of previous episodes
Unilateral redness, tearing, irritation, blurred vision, photophobia, history of previous episodes
Signs
 Central disc of stromal and epithelial edema (Fig. 7-6A and B)
Central disc of stromal and epithelial edema (Fig. 7-6A and B)
 Small keratic precipitates localized to the underlying endothelium
Small keratic precipitates localized to the underlying endothelium
 Folds in Descemet’s membrane
Folds in Descemet’s membrane
 Surrounding stromal immune ring (Wessley ring) may be present.
Surrounding stromal immune ring (Wessley ring) may be present.
 The limbal tissue may be thickened and inflamed (limbitis) (Fig. 7-6C).
The limbal tissue may be thickened and inflamed (limbitis) (Fig. 7-6C).
 Anterior uveitis (Fig. 7-6dand E)
Anterior uveitis (Fig. 7-6dand E)
 Intraocular pressure may be elevated.
Intraocular pressure may be elevated.
 Corneal sensation is typically reduced.
Corneal sensation is typically reduced.
Differential Diagnosis
 Herpes zoster disciform keratitis
Herpes zoster disciform keratitis
 Fuchs’ endothelial dystrophy
Fuchs’ endothelial dystrophy
 Acute corneal hydrops of keratoconus
Acute corneal hydrops of keratoconus
 Contact lens overwear
Contact lens overwear
Treatment
 If inflammation is mild and vision is good, the condition can be observed.
If inflammation is mild and vision is good, the condition can be observed.
 In more severe cases, topical corticosteroids (e.g., prednisolone 1%, dexamethasone 0.1%, or loteprednol 0.5% drops q.i.d.) can be started, maintained for several days to weeks, then gradually tapered over weeks or months. Often, a very low dose of topical corticosteroid (once or twice a week) may be required to prevent recurrent inflammation.
In more severe cases, topical corticosteroids (e.g., prednisolone 1%, dexamethasone 0.1%, or loteprednol 0.5% drops q.i.d.) can be started, maintained for several days to weeks, then gradually tapered over weeks or months. Often, a very low dose of topical corticosteroid (once or twice a week) may be required to prevent recurrent inflammation.
 While on corticosteroids more than once a day, concomitant oral antiviral therapy (e.g., acyclovir 400 mg b.i.d.) is often used as prophylaxis.
While on corticosteroids more than once a day, concomitant oral antiviral therapy (e.g., acyclovir 400 mg b.i.d.) is often used as prophylaxis.
 If an epithelial lesion is present, it should be treated before starting corticosteroids.
If an epithelial lesion is present, it should be treated before starting corticosteroids.
 Recommend long-term oral antiviral prophylaxis (e.g., acyclovir 400 mg b.i.d.) if a patient has had multiple episodes of stromal keratitis.
Recommend long-term oral antiviral prophylaxis (e.g., acyclovir 400 mg b.i.d.) if a patient has had multiple episodes of stromal keratitis.
Prognosis
 Good. Stromal scarring may occur and reduce vision (Fig. 7-6F). Often recurs
Good. Stromal scarring may occur and reduce vision (Fig. 7-6F). Often recurs
Figure 7-6. Herpes simplex disciform keratitis. A. This eye has moderate central corneal edema in a circular pattern, hence the term “disciform.” The slit-beam view demonstrates central corneal thickening. This disciform keratitis represents an inflammatory reaction to previous herpes simplex infection. It may resolve spontaneously, but it often responds extremely well to topical corticosteroids with antiviral coverage. B. This eye has severe central corneal edema with underlying keratic precipitates. Herpes simplex limbitis. C. This eye, with a previous history of herpes simplex keratitis, has severe limbal inflammation. Note the thickened, elevated limbal conjunctiva. This limbitis responded to topical corticosteroids and antiviral coverage. Herpes simplex iritis. D. Hundreds of granulomatous keratic precipitates are present in this eye with a history of previous herpes simplex keratitis. Note the faint central corneal scarring of old herpes keratitis. Often the intraocular pressure is elevated in eyes with herpetic iritis. Herpes simplex iritis responds to topical corticosteroids with antiviral coverage. It often benefits from treatment with oral antiviral agents in addition. Herpes simplex keratitis. E. Retroillumination off the retina reveals significant iris stromal atrophy and iris transillumination defects after multiple episodes of herpes simplex keratitis and iritis. F. A large, dense corneal scar with neovascularization remains after repeated episodes of herpes simplex keratitis.
HSV: NECROTIZING STROMAL KERATITIS
Necrotizing stromal keratitis is unusual. It is most likely caused by viral infiltration and inflammation of the corneal stroma.
Symptoms
 Unilateral redness, tearing, irritation, blurred vision, photophobia, pain, history of previous episodes
Unilateral redness, tearing, irritation, blurred vision, photophobia, pain, history of previous episodes
Signs
 Necrotic, cheesy, stromal infiltration, usually associated with an epithelial defect (Fig. 7-7A)
Necrotic, cheesy, stromal infiltration, usually associated with an epithelial defect (Fig. 7-7A)
 The appearance of the infiltrate can be confused with secondary bacterial or fungal keratitis.
The appearance of the infiltrate can be confused with secondary bacterial or fungal keratitis.
 Corneal thinning, stromal neovascularization, scarring, or perforation may develop (Fig. 7-7B).
Corneal thinning, stromal neovascularization, scarring, or perforation may develop (Fig. 7-7B).
 There may be associated keratic precipitates, anterior uveitis, or hypopyon.
There may be associated keratic precipitates, anterior uveitis, or hypopyon.
 Intraocular pressure can be elevated even in the presence of minimal anterior chamber reaction.
Intraocular pressure can be elevated even in the presence of minimal anterior chamber reaction.
Differential Diagnosis
 Primary or secondary bacterial or fungal keratitis: There is generally an overlying epithelial defect. These conditions should be considered when there is lack of response to antiviral treatment, and when there are increased or new signs of infection and inflammation.
Primary or secondary bacterial or fungal keratitis: There is generally an overlying epithelial defect. These conditions should be considered when there is lack of response to antiviral treatment, and when there are increased or new signs of infection and inflammation.
Treatment
 The first priority is to rule out a bacterial or fungal infection and to treat any associated epithelial defect.
The first priority is to rule out a bacterial or fungal infection and to treat any associated epithelial defect.
 Once the epithelium has healed, topical corticosteroids can be judiciously added to reduce stromal and anterior chamber inflammation (e.g., prednisolone 1% or dexamethasone 0.1% drops q.i.d.), combined with topical or oral antiviral prophylaxis.
Once the epithelium has healed, topical corticosteroids can be judiciously added to reduce stromal and anterior chamber inflammation (e.g., prednisolone 1% or dexamethasone 0.1% drops q.i.d.), combined with topical or oral antiviral prophylaxis.
 Corticosteroid drops should be tapered gradually (strength and frequency) over weeks or months, depending on the level of inflammation and the therapeutic response.
Corticosteroid drops should be tapered gradually (strength and frequency) over weeks or months, depending on the level of inflammation and the therapeutic response.
 Cycloplegics (e.g., scopolamine 0.25% or cyclopentolate 1% t.i.d.).
Cycloplegics (e.g., scopolamine 0.25% or cyclopentolate 1% t.i.d.).
 Treat any elevated intraocular pressure. Avoid miotics and prostaglandin analogs.
Treat any elevated intraocular pressure. Avoid miotics and prostaglandin analogs.
 Systemic antiviral medications (e.g., acyclovir 400 mg five times a day for weeks to months) are typically indicated, especially when there is anterior uveitis.
Systemic antiviral medications (e.g., acyclovir 400 mg five times a day for weeks to months) are typically indicated, especially when there is anterior uveitis.
 Corneal transplant during acute stages of the infection is discouraged because of the high failure rates
Corneal transplant during acute stages of the infection is discouraged because of the high failure rates
 Recommend long-term oral antiviral prophylaxis (e.g., acyclovir 400 mg b.i.d.) if a patient has had past episodes of stromal keratitis.
Recommend long-term oral antiviral prophylaxis (e.g., acyclovir 400 mg b.i.d.) if a patient has had past episodes of stromal keratitis.
Prognosis
 Fair. Typically, significant stromal scarring remains, and if it is in the visual axis, it can severely affect vision.
Fair. Typically, significant stromal scarring remains, and if it is in the visual axis, it can severely affect vision.
Figure 7-7. Herpes simplex necrotizing keratitis. A. A necrotizing stromal keratitis can be seen from the 8 o’clock to 10 o’clock positions, reaching into the visual axis. A prominent limbitis is present. Old stromal scarring is present superiorly and centrally. B. This necrotizing herpes simplex keratitis caused a full-thickness corneal melt and perforation. This large perforation required an emergency penetrating keratoplasty.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


