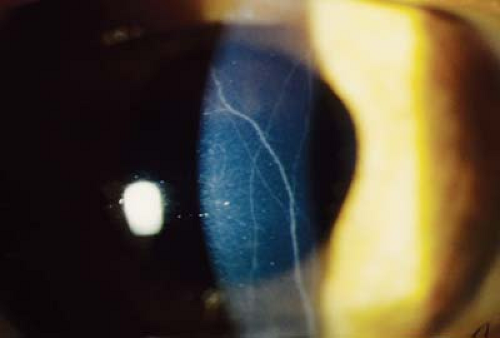
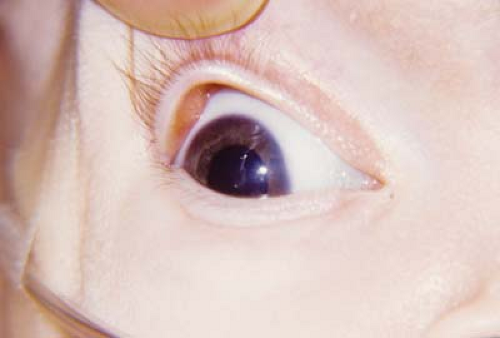
Cornea
Alex V. Levin
Thomas W. Wilson
David Rootman
Jerome Kazdan
The cornea develops from surface ectoderm (corneal epithelium) and neural crest cells (corneal stroma and endothelium). Developmental anomalies can result from inherited or spontaneous genetic mutations and insults during embryogenesis. Acquired disease can result from infection or other environmental or local contiguous processes. Multiple genes are involved in corneal formation. Mutations in these genes may result in isolated corneal malformation or associated abnormalities of the anterior and posterior segment.
As the most important refracting portion of the eye, corneal disease is likely to have a significant effect on vision. In the developing visual system of a child, superimposed amblyopia will almost certainly accompany most corneal disease. As the cornea has afferent neural pain fibers carried by the trigeminal nerve, photophobia and pain are also common symptoms of corneal disease. Its location does allow for topical treatment to be effective in many types of disease, but some corneal problems are not amenable to medical therapy. Corneal transplantation is available to clear the visual axis and relieve symptoms, but this process requires long-term follow-up and treatment, which itself can be uncomfortable and amblyogenic. In the setting of congenital obstruction of the visual axis, the poor success of infantile corneal transplantation has to be carefully weighed against the value of clearing the visual axis as soon as possible.
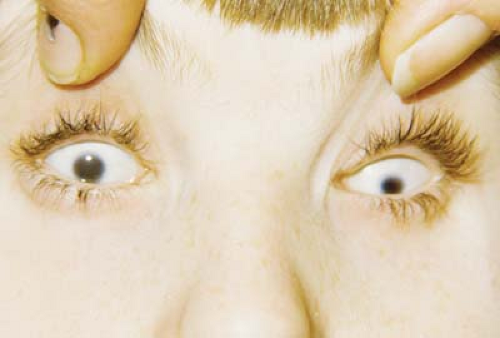
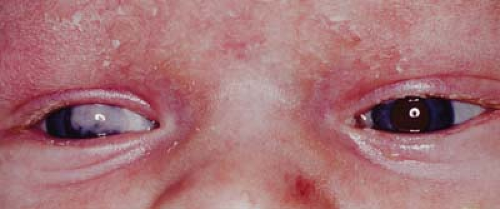 Figure 5.3 Corneal Dermoid Corneal dermoids are round or oval vascular masses attached to the corneal surface. They often protrude, as seen here. They consist of ectodermally derived tissue and may contain hair and sweat glands within the corneal stroma. Therefore, these lesions are classified as choristomas. The lesions are most commonly located at the inferotemporal limbus but may also occur in the conjunctiva or central cornea. Astigmatic or occlusion amblyopia is a concern. Systemic associations include Goldenhar syndrome (Chapter 14: Craniofacial, Figs. 14.18, 14.19, 14.20 and 14.21). Lamellar keratoplasty and penetrating keratoplasty are performed for superficial and deep lesions, respectively. When isolated, this is usually a sporadic nongenetic anomaly. |
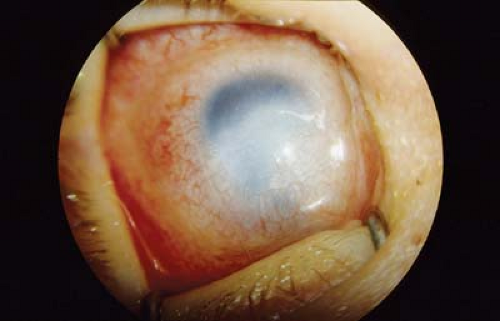
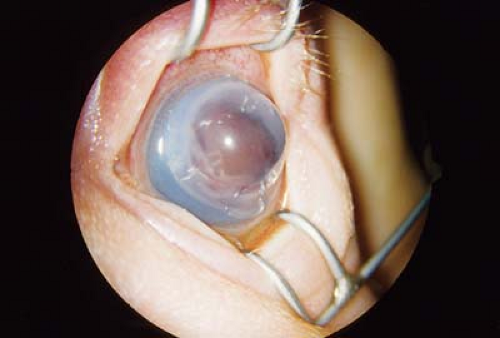 Figure 5.6 Congenital Cornea Ectasia Congenital corneal ectasia is a thinning and protrusion of the central cornea, if not a descemetocele or frank perforation at birth. Uveal tissue often lines the endothelial surface of the abnormal cornea. There is typically microphthalmia and increased intraocular pressure due to angle anomalies. Ectasia may be a manifestation of Peters anomaly (Fig. 5.1), congenital infections (e.g., cytomegalovirus, Chapter 19: Infectious Diseases, Figs. 19.9, 19.10 and 19.11), or an isolated ocular anomaly. Treatment includes urgent penetrating keratoplasty for tectonic support. Given the young age at which this procedure is required, the success rate is low. |
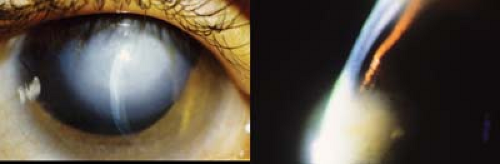
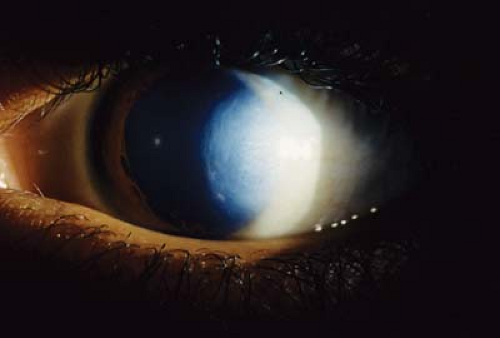 Figure 5.9 Cornea Plana Cornea plana is an abnormally flat anterior corneal surface with corneal curvatures less than 40 diopters and often less than 36. The peripheral cornea is similar to sclera and may be more opaque than usual with features of sclerocornea (Fig. 5.2). Central cornea may also have decreased clarity. Most cases are sporadic, although autosomal dominant and autosomal recessive forms due to mutations in the keratocan gene at 12q also occur, as does association with systemic syndromes such as Ehlers-Danlos and Marfan. |
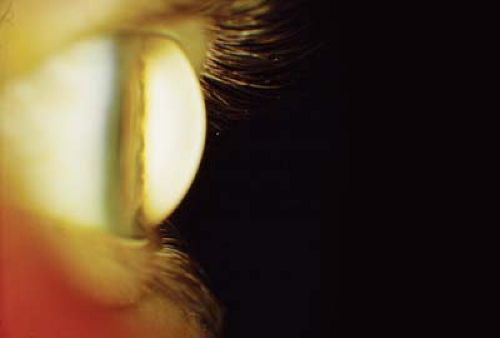
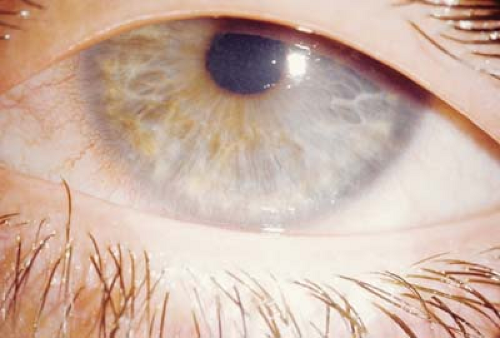 Figure 5.10 Meesman Corneal Dystrophy
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|