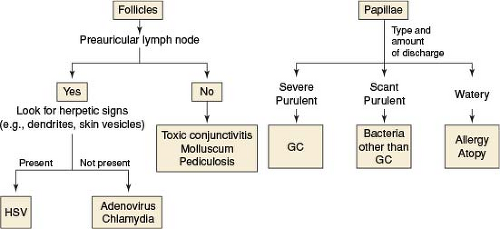
Conjunctiva/Sclera/Iris/External Disease
5.1 Acute Conjunctivitis
Symptoms
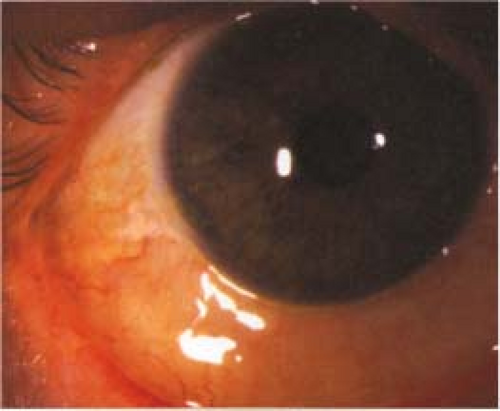
“Red eye” (conjunctival hyperemia), discharge, eyelids sticking or crusting (worse upon awakening from sleep), foreign body sensation, <4-week duration of symptoms (otherwise, SEE 5.2, CHRONIC CONJUNCTIVITIS) (see Figure 5.1.1).
Viral Conjunctivitis/Epidemic Keratoconjunctivitis
Symptoms
Itching, burning, tearing, gritty or foreign body sensation; history of recent upper respiratory tract infection or contact with someone with viral conjunctivitis. Often starts in one eye, and involves the fellow eye a few days later.
Signs
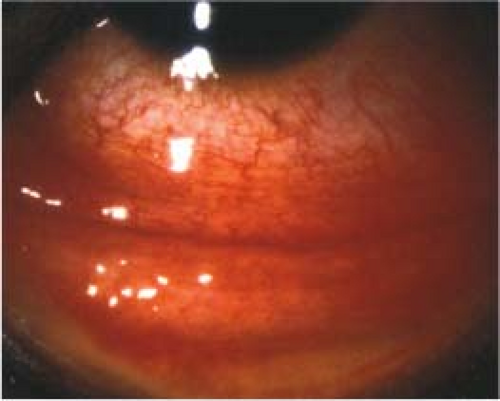
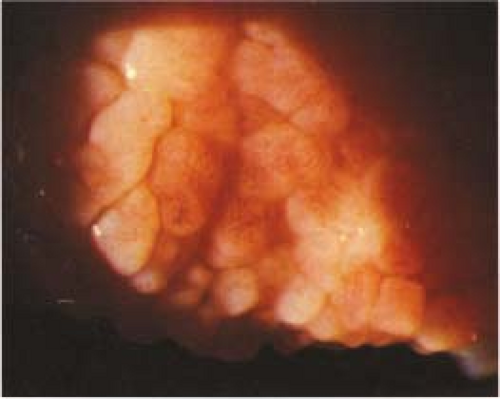
(See Figure 5.1.2.)
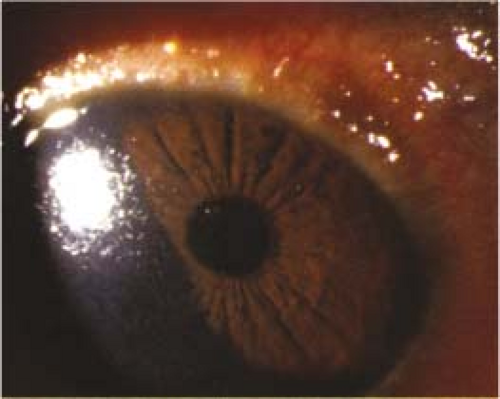
Critical. Inferior palpebral conjunctival follicles (see Figure 5.1.3), tender palpable preauricular lymph node.
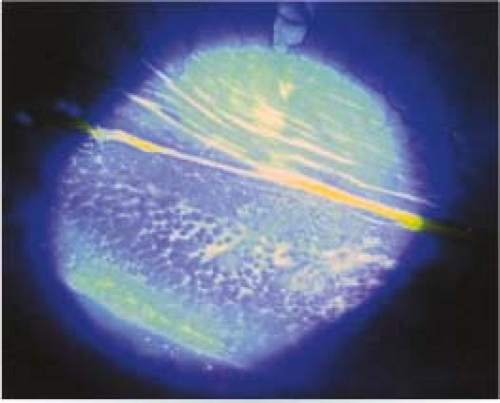
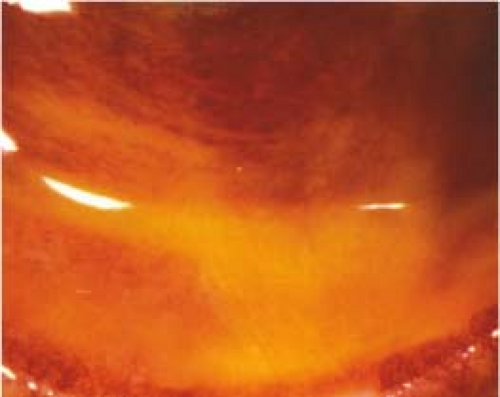
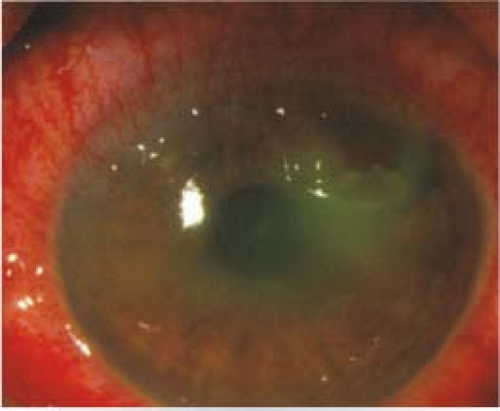
Other. Watery discharge, red and edematous eyelids, pinpoint subconjunctival hemorrhages, punctate keratopathy (epithelial erosion in severe cases), membrane/pseudomembrane (see Figure 5.1.4). Fine intraepithelial microcysts are an early corneal finding which, if present, can be helpful in diagnosis. Subepithelial (anterior stromal) infiltrates (SEIs) can develop a few weeks after the onset of the conjunctivitis.
Etiology and Variants of Viral Conjunctivitis
Most commonly adenovirus. Epidemic keratoconjunctivitis is most commonly caused by subgroup D of serotypes 8, 19, and 37. Pharyngoconjunctival fever is associated with pharyngitis and fever, usually in children, and is most commonly caused by serotypes 3 and 7.
Acute hemorrhagic conjunctivitis: Associated with prominent subconjunctival hemorrhages, usually 1 to 2 weeks in duration. Tends to occur in tropical regions. Caused by enterovirus 70 (rarely followed by polio-like paralysis), coxsackievirus A24, and adenovirus serotype 11.
Work-Up
No conjunctival cultures/swabs are indicated unless discharge is excessive or the condition becomes chronic (SEE 5.2, CHRONIC CONJUNCTIVITIS).
Treatment
Counsel the patient that viral conjunctivitis is a self-limited condition that typically gets worse for the first 4 to 7 days after onset and may not resolve for 2 to 3 weeks (potentially longer with corneal involvement).
Viral conjunctivitis is highly contagious (usually for 10 to 12 days from onset) as long as the eyes are red (when not on steroids) or have active discharge/tearing. Patients should avoid touching their eyes, shaking hands, sharing towels or pillows, etc. Restrict work and school for patients with significant exposure to others while the eyes are red and weeping.
Frequent handwashing.
Preservative-free artificial tears or tear ointment four to eight times per day for 1 to 3 weeks. Advise single-use vials to limit tip contamination and spread of the condition.
Cool compresses several times per day.
Antihistamine drops (e.g., epinastine 0.05% b.i.d.) if itching is severe.
If a membrane/pseudomembrane is present, it should be gently peeled with a cotton-tip
applicator or smooth forceps to enhance comfort, minimize corneal defects, and help prevent symblepharon formation.
If a membrane/pseudomembrane is present or if SEIs reduce vision and/or cause significant photophobia, topical steroids should be initiated. For membranes/pseudomembranes, use a more frequent steroid dose or stronger steroid (e.g., loteprednol 0.5% or prednisolone acetate 1% q.i.d.). Consider a steroid ointment (e.g., fluorometholone 0.1% ointment q.i.d. or dexamethasone/tobramycin 0.1%/0.3% ointment q.i.d.) in the presence of significant tearing to maintain longer medication exposure. For SEIs alone, a weaker steroid with less frequent dosing is usually sufficient (e.g., loteprednol 0.2% or 0.5% b.i.d.). Given the possible side effects, prescription of topical steroids is cautionary in the emergency room setting or in patients with questionable follow-up. Steroids may hasten the resolution of the symptoms but prolong the infectious period. Additionally, steroids often necessitate a long-term taper and delayed SEIs can recur during or after such a taper.
Follow-Up
In 2 to 3 weeks, but sooner if the condition worsens significantly or if topical steroids are prescribed.
Herpes Simplex Virus Conjunctivitis
SEE 4.15, HERPES SIMPLEX VIRUS, for a detailed discussion. Patients may have a history of perioral cold sores. Manifests with a unilateral (sometimes recurrent) follicular conjunctival reaction, palpable preauricular node, and, occasionally, concurrent herpetic skin vesicles along the eyelid margin or periocular skin. Treat with antiviral therapy (e.g., trifluridine 1% drops eight times per day, ganciclovir 0.05% gel five times per day, or oral agents such as acyclovir 400 mg five times a day) and warm compresses. Steroids are contraindicated.
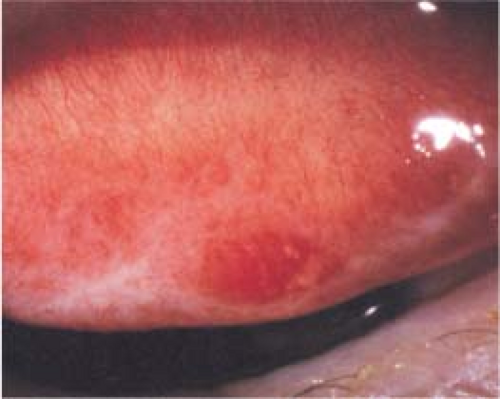
Allergic Conjunctivitis
Symptoms
Itching, watery discharge, and a history of allergies are typical. Usually bilateral.
Signs
Chemosis, red and edematous eyelids, conjunctival papillae, periocular hyperpigmentation, no preauricular node (see Figure 5.1.5).
Treatment
Eliminate the inciting agent. Frequent washing of hair and clothes may be helpful.
Cool compresses several times per day.
Topical drops, depending on the severity.
Mild: Artificial tears four to eight times per day.
Moderate: Use antihistamine and/or mast-cell stabilizer drops. Convenient medications with daily dosing include olopatadine 0.2% or 0.7% and alcaftadine 0.25% drops. Common medications with b.i.d. dosing include olopatadine 0.1%, epinastine 0.05%, nedocromil 2%, bepotastine 1.5%, or ketotifen 0.025% (over-the-counter) drops. Pemirolast 0.1% and lodoxamide 0.1% drops can also reduce symptoms but are recommended at q.i.d. dosing.
Severe: Mild topical steroid (e.g., loteprednol 0.2% or fluorometholone 0.1% q.i.d. for 1 to 2 weeks) in addition to the preceding medications.
Oral antihistamine (e.g., diphenhydramine 25 mg p.o. t.i.d. to q.i.d. or loratadine 10 mg p.o. daily) in moderate-to-severe cases can be very helpful.
Follow-Up
Two weeks. If topical steroids are used, tapering is required and patients should be monitored for side effects.
Vernal/Atopic Conjunctivitis
Symptoms
Usually bilateral but frequently asymmetric itching with thick, ropy discharge. More common in boys. Seasonal (spring/summer) recurrences in vernal conjunctivitis; history of atopy, dermatitis, and/or asthma without seasonal correlation in atopic conjunctivitis. Vernal conjunctivitis is usually seen in younger patients.
Signs
Critical. Large conjunctival papillae seen under the upper eyelid or along the limbus (limbal vernal) (see Figure 5.1.6).
Other. Superior corneal “shield” ulcer (a well-delineated, sterile, gray-white infiltrate with overlying epithelial defect), limbal raised white dots (Horner–Trantas dots) of degenerated eosinophils (see Figure 5.1.7), superficial punctate keratopathy (SPK).
Treatment
Treat as for allergic conjunctivitis except ensure prophylactic use of a mast-cell stabilizer or combination antihistamine/mast-cell stabilizer (e.g., olopatadine 0.2% or 0.7% daily, alcaftadine 0.25% daily, olopatadine 0.1% b.i.d., ketotifen 0.1% b.i.d., lodoxamide 0.1% q.i.d., pemirolast 0.1% q.i.d.) for 2 to 3 weeks before the allergy season starts.
If a shield ulcer is present, add:
Topical steroid (e.g., loteprednol 0.5% or prednisolone acetate 1% drops, dexamethasone 0.1% ointment) four to six times per day.
Topical antibiotic drop (trimethoprim/polymyxin B q.i.d) or ointment (e.g., erythromycin q.i.d., bacitracin/polymyxin B q.i.d.).
Cycloplegic agent (e.g., cyclopentolate 1% t.i.d.).
 NOTE: Shield ulcers may need to be scraped to remove superficial plaque-like material before reepithelialization will occur.
NOTE: Shield ulcers may need to be scraped to remove superficial plaque-like material before reepithelialization will occur.
Cool compresses q.i.d.
Consider cyclosporine 0.05% to 2% b.i.d. to q.i.d. if not responding to the preceding treatment. Inform the patient that maximal effect of this drop is not seen for several weeks.
If associated with atopic dermatitis of eyelids, consider tacrolimus 0.03% to 0.1% ointment q.h.s. or b.i.d. (preferred), pimecrolimus 1% cream b.i.d., or topical steroid ophthalmic ointment (e.g., fluorometholone 0.1% q.i.d.) to the affected skin for 1 to 2 weeks.
Follow-Up
Every 1 to 3 days in the presence of a shield ulcer; otherwise, every few weeks. Topical medications are tapered slowly as improvement is noted. Antiallergy drops are maintained for the duration of the season and are often reinitiated a few weeks before the next spring. Patients on topical steroids should be monitored regularly with attention to IOP, even if used only on the skin.
Bacterial Conjunctivitis (Nongonococcal)
Symptoms
Redness, foreign body sensation, discharge; itching is much less prominent.
Signs
Critical. Purulent white-yellow discharge of mild-to-moderate degree.
Other. Conjunctival papillae, chemosis, preauricular node typically absent (unlike gonococcal in which a preauricular node is often palpable).
Etiology
Commonly, Staphylococcus aureus (associated with blepharitis, phlyctenules, and marginal sterile infiltrates), Staphylococcus epidermidis, Haemophilus influenzae (especially in children and commonly associated with otitis media), Streptococcus pneumoniae, and Moraxella catarrhalis.
Work-Up
If severe, recurrent, or recalcitrant, send conjunctival scrapings for immediate Gram stain (to evaluate for gonococcus) and for routine culture and sensitivities (e.g., blood and chocolate agar).
Treatment
Use topical antibiotic therapy (e.g., trimethoprim/polymyxin B or fluoroquinolone drops or ointment q.i.d.) for 5 to 7 days.
H. influenzae conjunctivitis should be treated with oral amoxicillin/clavulanate (20 to 40 mg/kg/day in three divided doses) because of occasional extraocular involvement (e.g., otitis media, pneumonia, and meningitis).
If associated with dacryocystitis, systemic antibiotics are necessary. SEE 6.9, DACRYOCYSTITIS/INFLAMMATION OF THE LACRIMAL SAC.
Follow-Up
Every 2 to 3 days initially, then every 5 to 7 days when stable until resolved. Antibiotic therapy is adjusted according to culture and sensitivity results.
Gonococcal Conjunctivitis
Signs
Critical. Severe purulent discharge, hyperacute onset (classically within 12 to 24 hours).
Other. Conjunctival papillae, marked chemosis, preauricular adenopathy, eyelid swelling. SEE 8.9, OPHTHALMIA NEONATORUM (NEWBORN CONJUNCTIVITIS), for a detailed discussion of gonococcal conjunctivitis in the newborn.
Work-Up
Examine the entire cornea for peripheral ulcers (especially superiorly) because of the risk for rapid progression to perforation (see Figure 5.1.8).
Send conjunctival scrapings for immediate Gram stain and for culture and sensitivities (e.g., chocolate agar or Thayer–Martin agar).
Treatment
Initiated if the Gram stain shows gram-negative intracellular diplococci or there is a high clinical suspicion of gonococcal conjunctivitis.
A dual treatment regimen of ceftriaxone 1 g intramuscularly (i.m.) PLUS azithromycin 1 g p.o. both in a single dose is recommended. If corneal involvement exists, or cannot be excluded because of chemosis and eyelid swelling, hospitalize the patient and treat with
ceftriaxone 1 g intravenously (i.v.) every 12 to 24 hours in place of i.m. ceftriaxone. The duration of treatment may depend on the clinical response. Consider an infectious disease consultation in all cases of gonococcal conjunctivitis.
If ceftriaxone is not available or unable to be tolerated (e.g., cephalosporin-allergic patients), consider the following treatment regimens:
Gemifloxacin 320 mg p.o. in a single dose PLUS azithromycin 2 g p.o. in a single dose
Gentamicin 240 mg i.m. in a single dose PLUS azithromycin 2 g p.o. in a single dose”
 NOTE: Not only are fluoroquinolones contraindicated in pregnant women and children, but due to increased resistance, they are no longer recommended monotherapy for treatment of gonoccocal infections.
NOTE: Not only are fluoroquinolones contraindicated in pregnant women and children, but due to increased resistance, they are no longer recommended monotherapy for treatment of gonoccocal infections.
Topical fluoroquinolone ointment q.i.d. or fluoroquinolone drop q2h. If the cornea is involved, use a fluoroquinolone drop q1h (e.g., gatifloxacin, moxifloxacin, besifloxacin, levofloxacin, or ciprofloxacin).
Saline irrigation q.i.d. until the discharge resolves.
Treat for possible chlamydial coinfection (e.g., azithromycin 1 g p.o. single dose or doxycycline 100 mg p.o. b.i.d. for 7 days).
Treat sexual partners with oral antibiotics for both gonorrhea and chlamydia as described.
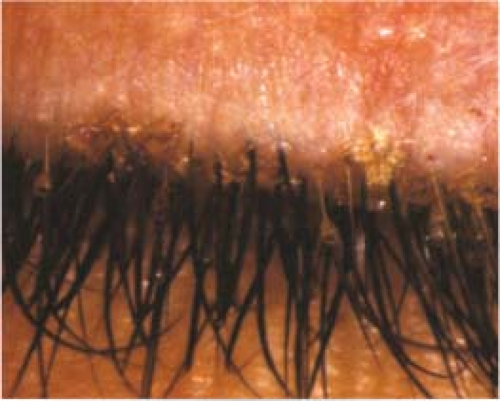
Pediculosis (Lice, Crabs)
Typically develops from contact with pubic lice (usually sexually transmitted). Can be unilateral or bilateral.
Symptoms
Itching, mild conjunctival injection.
Signs
Critical. Adult lice, nits, and blood-tinged debris on the eyelids and eyelashes (see Figure 5.1.9).
Other. Follicular conjunctivitis.
Treatment
Mechanical removal of lice and eggs with jeweler’s forceps.
Any bland ophthalmic ointment (e.g., erythromycin) to the eyelids t.i.d. for 10 days to smother the lice and nits.
Anti-lice lotion and shampoo as directed to nonocular areas for patient and close contacts.
Thoroughly wash and dry all clothes, towels, and linens.
For chlamydial, toxic, and molluscum contagiosum-related conjunctivitis, SEE 5.2, CHRONIC CONJUNCTIVITIS.
5.2 Chronic Conjunctivitis
Symptoms
“Red eye” (conjunctival hyperemia), conjunctival discharge, eyelids sticking (worse on awakening from sleep), foreign body sensation, duration >4 weeks (otherwise SEE 5.1, ACUTE CONJUNCTIVITIS).
Differential Diagnosis
Parinaud oculoglandular conjunctivitis (SEE 5.3, PARINAUD OCULOGLANDULAR CONJUNCTIVITIS).
Silent dacryocystitis (SEE 6.9, DACRYOCYSTITIS/INFLAMMATION OF THE LACRIMAL SAC).
Contact lens-related (SEE 4.20, CONTACT LENS-RELATED PROBLEMS).
Conjunctival tumors (SEE 5.12, CONJUNCTIVAL TUMORS).
Autoimmune disease (e.g., reactive arthritis, sarcoidosis, discoid lupus, others).
Chlamydial Inclusion Conjunctivitis
Sexually transmitted, due to Chlamydia trachomatis serotypes D-K and typically found in young adults. A history of vaginitis, cervicitis, or urethritis may be present.
Signs
Inferior tarsal or bulbar conjunctival follicles, superior corneal pannus, palpable preauricular node, or peripheral SEIs. A stringy, mucous discharge may be present.
Work-Up
History: Determine the duration of red eye, any prior treatment, concomitant vaginitis, cervicitis, or urethritis. Sexually active?
Slit lamp examination.
In adults, direct chlamydial immunofluorescence test, DNA probe, chlamydial culture, or polymerase chain reaction of conjunctival sample.
 NOTE: Topical fluorescein can interfere with immunofluorescence test results.
NOTE: Topical fluorescein can interfere with immunofluorescence test results.
Consider conjunctival scraping for Giemsa stain: Shows basophilic intracytoplasmic inclusion bodies in epithelial cells, polymorphonuclear leukocytes, and lymphocytes in newborns.
Treatment
Azithromycin 1 g p.o. single dose, doxycycline 100 mg p.o. b.i.d., or erythromycin 500 mg p.o. q.i.d. for 7 days is given to the patient and his or her sexual partners.
Topical erythromycin or tetracycline ointment b.i.d. to t.i.d. for 2 to 3 weeks.
Follow-Up
In 2 to 3 weeks, depending on the severity. The patient and sexual partners should be evaluated by their medical doctors for other sexually transmitted diseases. Occasionally a 6-week course of doxycycline may be required.
Trachoma
Principally occurs in developing countries in areas of poor sanitation and crowded conditions. Due to C. trachomatis serotypes A-C.
Signs
(See Figure 5.2.1.)
MacCallan Classification
Stage 1: Superior tarsal follicles, mild superior SPK, and pannus, often preceded by purulent discharge and tender preauricular node.
Stage 2: Florid superior tarsal follicular reaction (2a) or papillary hypertrophy (2b) associated with superior corneal SEIs, pannus, and limbal follicles.
Stage 3: Follicles and scarring of superior tarsal conjunctiva.
Stage 4: No follicles, extensive conjunctival scarring.
Late complications: Severe dry eyes, trichiasis, entropion, keratitis, corneal scarring, superficial fibrovascular pannus, Herbert pits (scarred limbal follicles), corneal bacterial superinfection, and ulceration.
World Health Organization Classification
TF (trachomatous inflammation: follicular): More than five follicles on the upper tarsus.
TI (trachomatous inflammation: intense): Inflammation with thickening obscuring >50% of the tarsal vessels.
TS (trachomatous scarring): Cicatrization of tarsal conjunctiva with fibrous white bands.
TT (trachomatous trichiasis): Trichiasis of at least one eyelash.
CO (corneal opacity): Corneal opacity involving at least part of the pupillary margin.
Work-Up
History of exposure to endemic areas (e.g., North Africa, Middle East, India, Southeast Asia).
Examination and diagnostic studies as above (e.g., chlamydial inclusion conjunctivitis).
Treatment
Azithromycin 20 mg/kg p.o. single dose, doxycycline 100 mg p.o. b.i.d., or erythromycin 500 mg p.o. q.i.d. for 2 weeks.
Tetracycline, erythromycin, or sulfacetamide ointment b.i.d. to q.i.d. for 3 to 4 weeks.
Follow-Up
Every 2 to 3 weeks initially, then as needed. Although treatment is usually curative, reinfection is common if hygienic conditions do not improve.
Molluscum Contagiosum
Signs
Critical. Dome-shaped, usually multiple, umbilicated shiny nodules on the eyelid or eyelid margin.
Other. Follicular conjunctival response from toxic viral products, corneal pannus, SPK. Immunocompromised patients may have larger (up to 5 mm) and more numerous lesions along with less conjunctival reaction. An increased incidence with pediatric atopic dermatitis has been observed.
Treatment
When associated with chronic conjunctivitis, lesions should be removed by simple excision, incision and curettage, or cryosurgery.
Follow-Up
Every 2 to 4 weeks until the conjunctivitis resolves, which often takes 4 to 6 weeks. If many lesions are present, consider human immunodeficiency virus (HIV) testing.
Microsporidial Keratoconjunctivitis
Signs
Diffuse, coarse, raised punctate keratitis and nonpurulent papillary or follicular conjunctivitis not responsive to conservative treatment. In immunocompromised patients, a corneal stromal keratitis resembling HSV or fungal keratitis can occur. Diagnosis is based on scrapings or biopsy of the conjunctiva or cornea; organisms can be identified with Gram stain, Giemsa stain, electron microscopy, and confocal microscopy in vivo.
Treatment
Regimens of antiparasitic and/or antibiotic agents are recommended. Topical fumagillin, polyhexamethylene biguanide (PHMB), and/or oral antiparasitic medications (e.g., itraconazole 200 mg p.o. daily or albendazole 400 mg p.o. b.i.d.) have been used. Epithelial debridement followed by antibiotic ointment (e.g., erythromycin, ciprofloxacin, or bacitracin/polymyxin B t.i.d.) may be useful. Treat any systemic infestation. Consider HIV testing and infectious disease consultation.
Toxic Conjunctivitis/Medicamentosa
Signs
Inferior papillary reaction and/or inferior conjunctival staining with fluorescein from topical eye drops. Most notably from IOP-lowering medications, aminoglycosides, antivirals, and preserved drops (especially those containing benzalkonium chloride). With long-term use, usually more than 1 month, a follicular response can be seen with other medications including atropine, miotics, epinephrine agents, and nonaminoglycoside antibiotics. Inferior SPK and scant discharge may be noted.
Treatment
Usually sufficient to discontinue the offending eye drop. Can add preservative-free artificial tears four to eight times per day. In severe cases, topical steroids can be helpful in quieting the conjunctival inflammation and rendering the eye more comfortable.
Follow-Up
In 1 to 4 weeks, as needed.
Reference
Seize MB, Ianhez M, Cestari Sda C. A study of the correlation between molluscum contagiosum and atopic dermatitis in children. An Bras Dermatol. 2011;86(4):663–668.
5.3 Parinaud Oculoglandular Conjunctivitis
Symptoms
Red eye, mucopurulent discharge, foreign body sensation.
Signs
Critical. Granulomatous nodule(s) on the palpebral and bulbar conjunctiva; visibly swollen ipsilateral preauricular or submandibular lymph nodes.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree