Purpose
To compare a new swept-source optical coherence tomography (SSOCT)-based biometer (OA-2000) with the IOLMaster v5.4 (partial-coherence interferometry) and Aladdin (optical low-coherence interferometry) biometers in terms of axial length measurement and failure rate in eyes with cataract.
Design
Reliability study.
Methods
A total of 377 eyes of 210 patients were scanned with the 3 biometers in a random order. For each biometer, the number of unobtainable axial length measurements was recorded and grouped as per the type and severity of cataract based on the Lens Opacities Classification System III by the same experienced ophthalmologist. The Bland-Altman limits-of-agreement (LoA) method was used to assess the agreement in axial length measurements between the 3 biometers.
Results
The failure rate was 0 eyes (0%) with the OA-2000, 136 eyes (36.07%) with the IOLMaster, and 51 eyes (13.53%) with the Aladdin. χ 2 analyses indicated a significant difference in failure rate between all 3 devices ( P < .001). Logistic regression analysis highlighted a statistically significant trend of higher failure rates with increasing severity of nuclear, cortical, and posterior subcapsular cataracts. Bland-Altman statistics indicated small mean differences and narrow LoA (OA-2000 vs IOLMaster −0.09 to 0.08 mm; OA-2000 vs Aladdin −0.10 to 0.07 mm; IOLMaster vs Aladdin −0.05 to 0.04 mm).
Conclusions
The OA-2000, a new SSOCT-based biometer, outperformed both the IOLMaster and Aladdin biometers in very advanced cataracts of various morphologies. The use of SSOCT technology may be the reason for the improved performance of the OA-2000 and may lead to this technology becoming the gold standard for the measurement of axial length.
Biometry has seen a marked change in recent times. Ultrasound was the technique of choice for axial length determination but has been gradually superseded since 1999 with the advent of the IOLMaster from Carl Zeiss Meditec, with biometry based on partial-coherence interferometry (PCI). In 2009, the Lenstar LS 900 (Haag-Streit) was introduced, another optical biometry device based on optical low-coherence reflectometry (OLCR). The Aladdin optical biometer (Topcon) became available in 2012 and is based on the principle of optical low-coherence interferometry (OLCI). Although a major advantage of PCI-, OLCR-, and OLCI-based devices is that they are noncontact, they also provide much higher degrees of resolution over ultrasound, and devices can measure a number of additional parameters concurrently.
One major limitation of optical biometry is the failure rate with dense or posterior subcapsular cataracts, with one recent study finding failure rates as high as 38% with the IOLMaster (v5.4). However, failure rates will depend on the morphology and severity of cataract. In such cases of failure to acquire an axial length measurement, ultrasound is typically used. However, with the poor resolution known with this modality, errors in axial length measurement are more likely, which is of clinical concern. An axial length measurement error of 1.0 mm can result in a subsequent refractive error of approximately 3.0 diopters (D). As cataract surgery is now seen as a dual refractive and medical treatment procedure, such errors need to be minimized. There have been attempts to improve the failure rate, such as the “Dense Cataract Measurement” mode with the Lenstar and the composite software with the IOLMaster.
Swept-source (SS) optical coherence tomography (OCT) is an alternative implementation of Fourier-domain OCT where the wavelength of the light source is tuned in rapid cycles to sequentially scan the eye. With SSOCT, the signal-to-noise ratio is improved compared with the broadband light source because the reflections of the narrow-bandwidth-wavelength light source are projected to the eye one at a time, which in turn improves image quality and tissue penetration. The OA-2000 (Tomey, Nagoya, Japan) is a new SSOCT-based biometer.
The aim of the present study is to compare this new SSOCT-based biometer to the IOLMaster v5.4 (PCI-based) and Aladdin v1.1.2 (OLCI-based) biometers in terms of axial length measurement and measurement failure rate in eyes with cataract. A further aim was to determine the association between the acquisition rate with the different cataract types and severity.
Methods
This was a prospective device comparison study involving patients undergoing assessment for cataract surgery between June and August 2015 at the Eye Hospital of Wenzhou Medical University, Wenzhou, Zhejiang, China. The cataract patients were invited to participate in the study. Inclusion criteria included cataract in one or both eyes. Exclusion criteria were severe corneal or vitreous opacities, retinal disease, previous cataract surgery, significant systemic disease, or insufficient mental ability to comply with testing. Informed consent was obtained from each patient after the study had been fully explained. Research conformed to the Declaration of Helsinki. The study was approved by the Research Ethics Committee at the Eye Hospital of Wenzhou Medical University.
Each participant underwent a full ophthalmic examination (including pupil dilation with 0.5% tropicamide and 0.5% phenylephrine hydrochloride [Mydrin-P; Santen Pharmaceutical, Osaka, Japan]) and the Lens Opacities Classification System III (LOCS III) was used by the same experienced ophthalmologist (Y.L.) to grade the type and severity of cataract. The LOCS III decimal scale was used for each of the 4 possible components of cataract: nuclear opalescence, nuclear color, cortical, and posterior subcapsular cataract. The scale ranges from 0.1 (clear or colorless) to 5.9 (very opaque, in cases of cortical and posterior subcapsular) or 6.9 (very opaque or brunescent, in cases of nuclear color).
An axial length measurement was attempted with the 3 biometers: the OA-2000 (software version 1.0R), IOLMaster (software version 5.4), and Aladdin (software version 1.1.2) in a random order by the same experienced examiner (W.Z.). The OA-2000 biometer uses Fourier-domain optical interference with a 1060-nm swept-source laser to measure axial length. The IOLMaster v5.4 uses a laser diode emitting a 780-nm infrared beam of short-coherence light. The Aladdin relies on a 830-nm superluminescent diode. Patients were positioned with a chin and forehead rest and were instructed to fixate on the internal fixation target of each device. The OA-2000 uses a 3D eye-tracking system to automatically capture measurements. With the IOLMaster v5.4, the composite-20 method was used, which provides a mean value of 20 measurements, as it has been shown to provide the most consistent success for axial length measurement in comparison to the standard, standard manipulated, and composite-5 methods. With the OA-2000 v1.0R and Aladdin v1.1.2, at least 3 reliable measurements were acquired.
Statistical Analysis
For each biometer, the number of unobtainable axial length measurements was recorded. The Kolmogorov-Smirnov test was used to assess data for normality. χ 2 analyses were used to determine if statistically significant differences in success rates were found between the 3 biometers. The number of unobtainable measurements with each device was then grouped as per the type and severity of cataract (nuclear color, cortical, and posterior subcapsular) and compared. Logistic regression analysis was used to evaluate associations between type and severity of cataract with failure rate. The Bland-Altman limits-of-agreement (LoA) method was used to assess the agreement in axial length measurements between the 3 biometers. Statistics were calculated using Statistical Package for the Social Sciences (SPSS, version 21.0; SPSS Inc, Chicago).
Results
In total, 210 patients were recruited with a mean age of 69.57 ± 9.48 years (range 40–90 years; 112 female). Three hundred and seventy-seven eyes were scanned with each of the 3 biometers. From the 377 scanned eyes, the measurement failure rate was 0 eyes (0%) with the OA-2000 v1.0R, 136 eyes (36.07%) with the IOLMaster v5.4, and 51 eyes (13.53%) with the Aladdin v1.1.2. The Kolmogorov-Smirnov test indicated that data were normally distributed. χ 2 analyses indicated a significant difference in axial length measurement success rate between all 3 devices: OA-2000 v1.0R vs IOLMaster v5.4 (χ 2 = 165.9, P < .001), OA-2000 v1.0R vs Aladdin v1.1.2 (χ 2 = 54.7, P < .001), and IOLMaster v5.4 vs Aladdin v1.1.2 (χ 2 = 51.4, P < .001). Measurement failure rates in relation to the LOCS III cataract grading for the IOLMaster v5.4 and Aladdin v1.1.2 are shown in Table 1 . Logistic regression analysis was used to evaluate the associations between type and severity of cataract with measurement failure rate ( Table 2 ). A Bonferroni correction was applied (0.05/6), with a P value for statistical significance set at .008. This analysis highlighted a statistically significant trend of a higher failure rate with increasing severity of nuclear, cortical, and posterior subcapsular cataracts.
| LOCS III | Cortical | Nuclear Color | Posterior Subcapsular | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Total | IOLMaster | Aladdin | Total | IOLMaster | Aladdin | Total | IOLMaster | Aladdin | |||||||
| Unobtainable Number | Number (%) Unobtainable | Unobtainable Number | Number (%) Unobtainable | Unobtainable Number | Number (%) Unobtainable | Unobtainable Number | Number (%) Unobtainable | Unobtainable Number | Number (%) Unobtainable | Unobtainable Number | Number (%) Unobtainable | ||||
| ≤2.5 | 118 | 35 | 29.66 | 2 | 1.69 | 136 | 18 | 13.24 | 3 | 2.21 | 220 | 37 | 16.82 | 1 | 0.45 |
| 2.5∼3.5 | 164 | 51 | 31.10 | 26 | 15.85 | 164 | 49 | 29.88 | 12 | 7.32 | 85 | 33 | 38.82 | 7 | 8.24 |
| 3.6∼4.5 | 79 | 35 | 44.30 | 9 | 11.39 | 62 | 54 | 87.10 | 22 | 35.48 | 52 | 46 | 88.46 | 26 | 50.00 |
| 4.6∼5.5 | 16 | 15 | 93.75 | 14 | 87.50 | 10 | 10 | 100.00 | 9 | 90.00 | 5 | 5 | 100.00 | 3 | 60.00 |
| >5.5 | 0 | – | – | – | – | 5 | 5 | 100.00 | 5 | 100.00 | 15 | 15 | 100.00 | 14 | 93.33 |
| Total | 377 | 377 | 377 | ||||||||||||
| Cortical | Nuclear Color | Posterior Subcapsular | |
|---|---|---|---|
| IOLMaster | |||
| β | −0.603 | −2.198 | −1.76 |
| P value | .008 | <.001 | <.001 |
| Aladdin | |||
| β | −3.356 | −3.910 | −5.034 |
| P value | .001 | <.001 | <.001 |
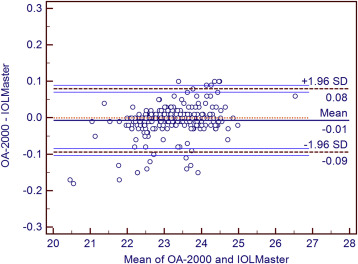
The descriptive statistics, including the mean, maximum, and minimum axial length measurements for the 3 biometers, are shown in Table 3 . The Bland-Altman plots and LoA ( Figures 1–3 ) were used to assess the agreement in axial length measurements with the 3 devices (241 eyes). The mean difference was small (magnitude 0.01 mm and less) and the LoA were narrow for all comparisons, indicating that these devices can be used interchangeably for axial length measurements ( Table 3 ).
| Biometer | Mean Axial Length ± SD | Minimum | Maximum | Mean Difference ± SD | 95% LoA |
|---|---|---|---|---|---|
| OA-2000 (mm) | 23.20 ± 0.84 | 20.36 | 26.56 | −0.01 ± 0.04 (OA-2000 vs IOLMaster) | −0.09 to 0.08 |
| IOLMaster (mm) | 23.21 ± 0.82 | 20.53 | 26.50 | −0.01 ± 0.04 (IOLMaster vs Aladdin) | −0.10 to 0.07 |
| Aladdin (mm) | 23.22 ± 0.82 | 20.55 | 26.50 | 0.00 ± 0.02 (OA-2000 vs Aladdin) | −0.05 to 0.04 |