Assessment of Ocular Health
Shoshana Bell-Craig
Robert H. Duckman
A high incidence of ocular disease is found in the pediatric population and, therefore, a thorough assessment of ocular health is imperative (1). To prevent vision conditions that have the potential to cause permanent vision loss, it is important to diagnose and treat them early. An evaluation of ocular health should include careful inspection of the anterior segment, pupil reflexes and intraocular pressure, and assessment of the posterior segment with dilation (2).
It is always easier to examine a patient who can respond to questions clearly and who can follow instructions during an examination. Most children will cooperate and testing used to assess the ocular health of adults can be used in the pediatric population. Standard procedures, however, may not be applicable to those who are very young or unable to communicate. We can put this population at some ease by making a number of modifications (2).
Evaluating the External Eye
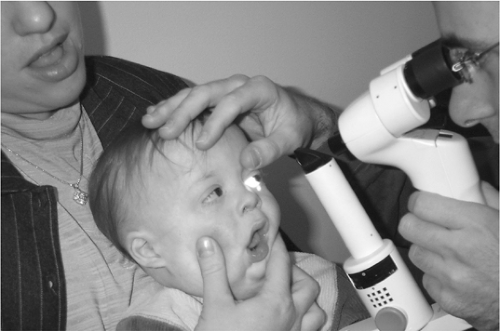
The standard fixed biomicroscope can be used to evaluate the anterior segment by having the infant or child propped up by the parent (Fig. 11.1). Children 2 years of age and older can usually stand on the footrest of the chair or kneel on the chair. For infants and children younger than 2 years, a portable slit lamp can be utilized. The most useful position for infants when using a portable slit lamp is to have them face up on the parent’s lap with their head on the parent’s knees and their legs under the parent’s armpits (3).
Portable slit lamps are available from the following manufacturers.
Clement Clarke Portable Slit Lamp 904
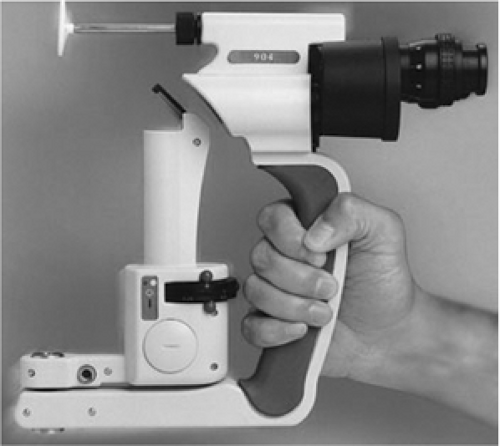
The Clement Clarke portable slit lamp with its head and chinrest assembly, can be used for traditional style examinations or as a handheld slit lamp (Fig. 11.2). The portable slit lamp’s power source is a rechargeable battery pack, enabling the examiner to be more mobile. It provides three slit widths (0.12 mm, 0.25 mm, and 0.5 mm), four slit heights (3 mm, 5 mm, 8 mm, and 14 mm), and two color filters (blue and yellow). Its standard magnification is 10× with the availability of optional 16× lenses.
Kowa SL–15 Portable Slit Lamp
The Kowa SL-15 (Fig. 11.3) is a cordless, rechargeable unit that has a halogen illumination source with a spot and three slit widths as well as a built-in cobalt blue filter. Magnification settings are the same as for the Clement Clarke, with a range from 10 to 16. The stand doubles as a battery charger and permits long-term continuous lighting for approximately 40 minutes. An optional headrest is also available to improve stability. The illumination can be reduced to one sixteenth of the maximum and may be beneficial for use with children to reduce
discomfort. (The original SL-14 model has been discontinued.)
discomfort. (The original SL-14 model has been discontinued.)
Heine HSL 150 Pocket Slit Lamp
The Heine HSL 150 pocket slit lamp (Fig. 11.4) does not provide as many slit sizes as the Clement Clarke and Kowa, but it does have an adjustable slit image with slit size available from 0.2 mm × 10 mm to 4 mm × 14 mm. Unlike the Clement Clarke and Kowa, the blue filter is available as an option for corneal evaluation and does not provide as much magnification. A 6 magnification with 20-D loupe is available and, when combined with the 10-D loupe, can provide 10 magnification. It is beneficial because it increases the working distance from the patient and offers a large field of view.
Zeiss HSO 10 Hand Slit Lamp
The Zeiss HSO 10 hand slit lamp (Fig. 11.5) can be converted into an indirect ophthalmoscope.
The illumination unit can be moved with one hand and set in any position on the clamping lever so that one hand is available to hold open eyelids or improve fixation with finger puppets. The equipment includes either a power supply unit or a rechargeable battery unit so the examiner can move around freely.
The illumination unit can be moved with one hand and set in any position on the clamping lever so that one hand is available to hold open eyelids or improve fixation with finger puppets. The equipment includes either a power supply unit or a rechargeable battery unit so the examiner can move around freely.
In addition to using a slit lamp to evaluate the integrity of the cornea, companies have developed handheld keratometers, which are extremely patient friendly.
Portable keratometers are available from the following manufacturers.
Marco Handheld Automatic Keratometer KM-500
The KM-500 allows the examiner to observe the targeted eye from any distance. It will fire automatically when focused properly. Two rechargeable batteries provide 60 minutes of continuous use. The measurable range of corneal curvature is 33 to 67.50 D.
Nidek Handheld Auto Refractor/Keratometer ARK-30
The Nidek ARK-30 is lightweight and portable and is capable of taking measurements with an infant or child lying on a parent’s lap because of its 90° correction function. It is wireless and comes with a built-in forehead rest. Nidek has also developed an autorefractor or keratometer and noncontact tonometer in one unit called the TONOREF RKT-7700. It allows the examiner to evaluate the external eye and obtain intraocular pressure readings without changing instruments. This unit, however, does require that the patient keep his or her chin in a chinrest.
Pupil Reflexes
A penlight or transilluminator is typically used to assess pupils in both the pediatric and adult population. Testing should be done with normal room illumination so as not to increase
anxiety. Keep in mind, very young patients have more miotic pupils, which do not reach normal size until about the age of 6 months (Jennings 1996). Have the infant or child sit on a parent’s lap and direct their fixation onto a distant target, if possible. It may be necessary to hold the eyelids open while testing for direct and consensual pupillary responses. It is increasingly difficult to determine the presence of a relative afferent defect without accurate fixation so toys set up across the room that make noise and light up are excellent targets.
anxiety. Keep in mind, very young patients have more miotic pupils, which do not reach normal size until about the age of 6 months (Jennings 1996). Have the infant or child sit on a parent’s lap and direct their fixation onto a distant target, if possible. It may be necessary to hold the eyelids open while testing for direct and consensual pupillary responses. It is increasingly difficult to determine the presence of a relative afferent defect without accurate fixation so toys set up across the room that make noise and light up are excellent targets.
Intraocular Pressure
Tonometry indirectly measures intraocular pressure (IOP) by determining the resistance of the cornea to indentation. The most commonly used devices are indentation (Schiotz) tonometers, applanation (Goldmann) tonometers, noncontact tonometers (pneumotonometry), and electronic indentation tonometers (3). Assessment of IOP is important, but can be difficult to obtain in a very young patient. A baseline measurement is valuable and IOP should be assessed, particularly when ocular signs and symptoms of or risk factors for glaucoma exist. Testing under sedation or anesthesia may be appropriate if IOP cannot be assessed under ordinary conditions.
Contact Tonometers
Currently, two methods are used to measure IOP in which the instrument touches the cornea—indentation and applanation. The indentation method indents and distorts the cornea using varied weights and a 3-mm plunger to indent the cornea. The device is known as the Schiotz tonometer and, although outdated, is still used in some clinical settings. This device has many drawbacks including the rigidity of the cornea and resistance to indentation, rigidity of the globe, and the possibility of injury and abrasion to the cornea. The more accepted method is applanating or flattening the cornea (1).
Tonometry is usually performed with the standard Goldmann applanation tonometer mounted on a slit lamp biomicroscope. It is the standard against which all tonometers are compared, and it is the preferred method to diagnose and treat glaucoma (4). Children who are able to cooperate by sitting still and fixating on a target can be evaluated using the standard Goldmann applanation tonometer. A drawback in using it with the pediatric population is that the patient must be in a horizontal plane with the tonometer. It helps to have the child kneel on the chair or stand while taking IOP measurements (1). Further drawbacks include the necessity of instilling fluorescein and an anesthetic eye drop.
Several companies (e.g., Haag-Streit, Clement Clarke, Nikon, and R. H. Burton) manufacture Goldmann-type tonometers for the slit lamp. The measurement of IOP in school-aged children is generally successful with applanation (2). Evaluation, however, has become much easier with the advent of portable instrumentation, such as handheld applanation and noncontact tonometers. The Perkins tonometer is very useful for this population.
Handheld Applanation Tonometers
Given that the standard Goldmann tonometer is mounted on a slit lamp, it is relatively nonportable. Handheld tonometers can be easily transported and do not require the patient to be positioned in an instrument. They may be less alarming to children and allow them to sit on their parent’s lap or lie down. Although less frightening, most of them require both fluorescein and anesthetic ocular drops. Many companies manufacture handheld tonometers and multiple studies have been performed to assess their reliability when compared with a Goldmann tonometer. Some of these are discussed below.
Clement Clarke-Perkins MK2 Applanation Tonometer
The Clement Clarke-Perkins MK 2 applanation tonometer (Fig. 11.6) utilizes Goldmann applanation and a counterbalance system, and can, therefore, take measurements with the patient in any position, which is very beneficial in the pediatric population. As a standard, spares and
accessories are supplied and the battery handle detaches for the installation and removal of batteries. Four AA batteries can be used. A rechargeable battery handle is interchangeable with the standard handle and can be left overnight to charge in the unit. The Perkins examination telescope (PET) allows magnified viewing of the fluorescein “semicircles” at arm’s length. A sterile disposable prism can be used for each patient to reduce risk of contamination.
accessories are supplied and the battery handle detaches for the installation and removal of batteries. Four AA batteries can be used. A rechargeable battery handle is interchangeable with the standard handle and can be left overnight to charge in the unit. The Perkins examination telescope (PET) allows magnified viewing of the fluorescein “semicircles” at arm’s length. A sterile disposable prism can be used for each patient to reduce risk of contamination.
Medtronic Solan’s Tono-Pen Xl
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree