Fig. 2.1
LipiView scan of the both eyes of a patient with MGD-related dry eyes
The patient underwent a LipiView scan which demonstrated the average interferometry color units (ICU) to be low at 45 in both eyes (normal is >50). The patient has 15 blinks in a 19 s testing interval which is a very high rate with concern for blepharospasm (Fig. 2.1 ). There are also very flat waveforms, unlike the example shown of a normal tear interferometry testing ( Fig. 2.2 ).
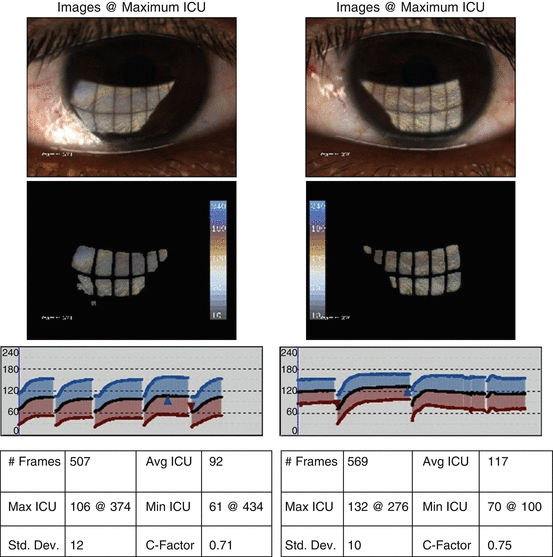

Fig. 2.2
LipiView scan of a normal patient (no dry eyes). In comparing the waveforms between each blink, this normal patient has increasing lipid tear thickness after each blink, not flat or “falling” waveforms
Video imaging also captures the blink mechanism. Incomplete blinking can be observed and this dysfunction will exacerbate evaporation, contributing to symptoms especially in arid climates/conditions. Past contact lens wearers and eyelid surgery patients are at risk for incomplete blink due to loss of feedback with the cornea sensation masked by contact lenses or mechanical inability for the eyelids to meet.
Looking at the Tear Film Interferometry Gives Part of the Picture, but Looking Directly at the Glands Would Help Determine If the Meibomian Glands Are Still Viable. What Technology Can Help Look at Meibomian Glands?
Meibography has been recently available as a clinical tool. In the past, infrared photography could be done, but it was time-consuming. Oculus Keratograph 5 and LipiView II can easily capture the meibomian glands for evaluation of gland architecture and atrophy.
Normal meibography shows long glands, extending across the height of the tarsus, and tiny grape-like clusters of acini around the length of the duct. Curved glands represent atrophy of adjacent glands.
This patient’s meibography shows mild atrophy in both eyelids, up to 25% shortening of the superior and inferior eyelid gland’s length ( Figs. 2.3 and 2.4 ).



Fig. 2.3
Meibography of the right upper and lower lids. The red lines outline the areas where the glands have dropped out

Fig. 2.4
Meibography of the left upper and lower lids. The red lines outline the areas where the glands have dropped out
The Patient Reported Tearing with His Work. How Do You Evaluate This?
A refraction can help determine if ciliary spasm with accommodation could contribute to tearing, in addition to probable reflex tearing from lipid tear deficiency. He has presbyopia and his vision improved to 20/20 with + 1.25 correction at near bilaterally. He was recommended to get a + 1.25 built into his procedural loupes.
Commonly, patients with lipid deficiency would expect to have bursts of reflex tearing that may overwhelm the nasolacrimal system and result in tearing. Epiphora, with tears actually rolling down the cheek, may indicate partial or complete nasolacrimal duct obstruction. Fortunately, this patient does not have epiphora and the tear meniscus is not high.
What Do You Recommend for This Patient?
Basic treatment that can help with meibomian gland deficiency consists of low-cost therapies with low risk of complications. Omega-3 fatty acids can be helpful. The dosing and exact combination of fatty acids has not been established. The NIH Dry Eye Assessment and Management (DREAM) Clinical Trial will give answers on dosing in the future. Commonly 1–2 g of DHA (docosahexaenoic acid) and EPA (eicosapentaenoic acid) are suggested. Caution must be taken when prescribing in the context of blood thinners and risk of prolonging clotting mechanism beyond the 2 g range. Hot compresses are a mainstay of treatment to alleviate gland blockage with incomplete blinking.
How Are Patients Instructed To Do Hot Compresses? Is Eyelid Massage Recommended?
Hot compresses are an economical method of heating the lids that provide some relief and potentially can help warm meibum, making it easier to secrete through the meibomian gland orifices. Wet hot washcloth in the shower can be used for patients with seborrhea debris on the eyelids and lashes, but the intensity of the heat is limited in this application method. A homemade “rice in a gym sock” or commercially available cloth mask filled with polymer beads can be microwaved for 20–30 s (until hot but not burning to touch) and placed over the eyelids for at least 10 min. An AC or USB adaptor plugged-in heated eye masks can be more convenient for business travelers or patients without access to a microwave.
Ten minutes is recommended as a minimum duration since it is recognized that the meibomian glands need this amount of time to release meibum. Cornea ectasia has been reported in patients massaging after heat application. Therefore, at-home lid massage is only recommended with caution. Instead, blinking exercises (described below) may be considered.
The patient spends 4 weeks working on this basic treatment plan but returns with OSDI 40 and still symptomatic. The tearing is better with use of near correction, but he is still symptomatic.
What Other Treatment Can Be Offered?
He declines doxycycline due to problems with his stomach. He tries topical azithromycin but this does not help.
Antibiotics such as tetracyclines and macrolides can be used off-label to improve symptoms of ocular rosacea and dry eye in an economical fashion. Antibiotics are discussed before any out-of-pocket treatment is offered. The patient is an active participant in his/her treatment plan.
The anti-inflammatory effect of inhibition of matrix metalloproteinase-9 can certainly help many rosacea patients and some patients with mild ocular rosacea. Tetracyclines are inexpensive but patients are best warned about gastrointestinal upset, sunburn potential, yeast vaginitis, urinary tract infection, and rarely drug allergy. Most patients need 20–100 mg of doxycycline or minocycline daily for 3 months to see any effect. In patients, where cost is not an issue, the extended release preparations may be better tolerated; otherwise one preferred regimen is doxycycline monohydrate 50 mg twice/day, in part since it is minimizes the dose and is quite affordable (in US pharmacies). Once dry eye symptoms are resolved, then patients can try to stop the drug. Some patients need a 90-day treatment twice a year to maintain their comfort. Some patients prefer dosing every second day.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


