Purpose
To evaluate efficacy of topical rebamipide for superior limbic keratoconjunctivitis (SLK) in patients with thyroid eye disease.
Design
Retrospective, observational case series.
Methods
Thirty-three eyes from 20 thyroid eye disease patients with SLK who received topical rebamipide (Mucosta ophthalmic suspension unit dose 2%; Otsuka Pharmaceutical Co, Ltd; chemical name, (2RS)-2-(4-chlorobenzoylamino)-3-(2-oxo-1, 2-dihydroquinolin-4-yl) propanoic acid) were included. The following items were evaluated before and 4 weeks after the start of treatments: presence or absence of SLK, rose bengal staining score, area and density classification of fluorescein staining, Schirmer test I results (without topical anesthesia), tear film break-up time, Hertel exophthalmometry values, and margin reflex distances 1 and 2.
Results
Twenty-eight eyes showed complete disappearance of SLK after treatment (84.8%; P < .001). The other 5 eyes (15.2%) demonstrated significant improvement, but had residual punctate rose bengal staining and fluorescein staining near the superior corneal limbus. All 5 eyes exhibited at least 1 of the following findings: proptosis of more than 17.7 mm and upper or lower eyelid retractions or both. Incidence of upper eyelid retraction was significantly higher in eyes with SLK than in those without SLK at the 4-week follow-up ( P = .021). The severity of rose bengal staining and fluorescein staining improved significantly after treatment ( P < .001). Although the Schirmer test results remained constant before and after the treatment ( P = .212), tear film break-up time increased significantly in the posttherapeutic state ( P = .009). No serious adverse events were reported.
Conclusions
Topical rebamipide improved SLK in patients with thyroid eye disease, suggesting a first-line treatment in such patients.
Rebamipide is a quinolinone derivative that increases production of mucin-like substances in the cornea and conjunctiva. It also exerts anti-inflammatory effects, promoting wound healing. Recent studies showed that rebamipide ameliorated corneal and conjunctival epithelial damage and increased tear film stability in patients with dry eye. However, it is still unclear whether rebamipide improves superior limbic keratoconjunctivitis (SLK).
SLK typically is caused by local mucin deficiency in the upper conjunctiva, resulting in abnormal friction and inflammation between the upper eyelid and the superior corneal limbus. This is associated predominantly with thyroid eye disease (TED), in which proptosis and enlarged eyelid fissures aggravate tear deficiency, abnormal friction, and ocular surface inflammation. In general, conservative procedures, such as topical treatment (artificial tears, vitamin A, silver nitrate, α-blocker, tacrolimus, cyclosporine, autologous serum, lodoxamide tromethamine, ketotifen fumarate, and cromolyn sodium), botulin toxin A and triamcinolone acetonide, bandage contact lenses, and punctal plugs, as well as a surgical conjunctival resection partially or completely improve SLK. However, SLK in TED tends to be more refractory, requiring systemic steroids, radiation therapy, blepharoplasty, strabismus surgery, and orbital decompression for treatment.
Because local mucin deficiency and underlying inflammation cause SLK, we speculated that topical rebamipide may improve SLK. SLK in TED usually requires more intense treatment than common SLK. If topical rebamipide improves SLK in TED, instillation as a first-line treatment in the clinic could be applied to such patients. We therefore examined the efficacy of topical rebamipide for SLK in TED patients.
Methods
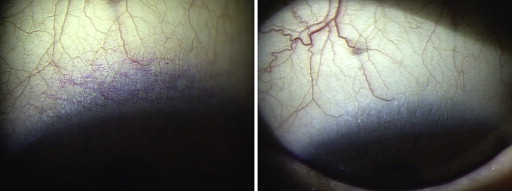
Institutional review board approval was obtained from Aichi Medical University (no. 13-015). We performed a retrospective chart review of all TED patients with SLK who were treated with topical rebamipide from May 2012 through June 2013. The diagnosis of TED was the presence of at least 1 of the characteristic eyelid signs (eyelid fullness, eyelid retraction, and eyelid lag) as well as presence of thyroid autoimmunity. Patients with at least 2 of the following criteria were diagnosed with SLK: blood vessel dilation in the superior bulbar conjunctiva, papillary inflammation of the upper tarsal conjunctiva, punctate rose bengal and fluorescein staining of the superior conjunctiva and of the upper cornea, filaments in the upper cornea, epithelial thickening of the superior bulbar conjunctiva, and redundancy of the superior bulbar conjunctiva. Patients wearing contact lenses or with other treatment for TED, dry eye, or both between pretreatment and posttreatment evaluations were excluded from this study. All patients had received topical rebamipide (Mucosta ophthalmic suspension unit dose 2%; Otsuka Pharmaceutical Co, Ltd, Tokyo, Japan; chemical name, (2RS)-2-(4-chlorobenzoylamino)-3-(2-oxo-1, 2-dihydroquinolin-4-yl) propanoic acid), 1 drop in each eye 4 times daily.
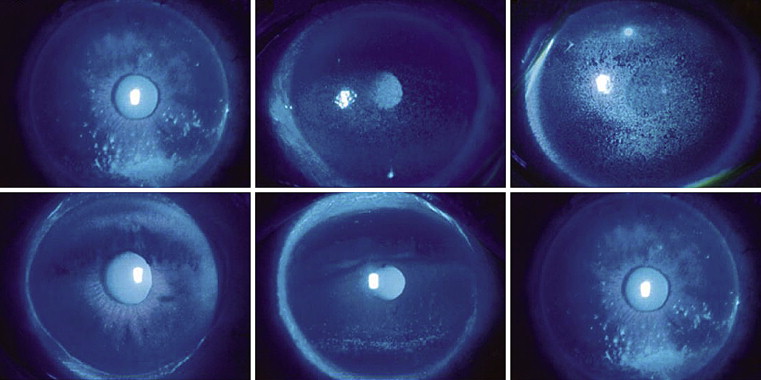
The information collected from the patients’ medical records included patient age, sex, and thyroid function evaluated before treatment. The severity of ocular surface conditions as well as TED conditions before and 4 weeks after the start of treatment were examined because response peak of rebamipide generally is at 4 weeks. The presence or absence of SLK, rose bengal staining score, area and density classification of fluorescein staining, Schirmer test I results, and tear film break-up time (TBUT) were assessed. Rose bengal staining was evaluated in the temporal and nasal conjunctiva and the cornea, then quantified on a scale of 0 (no staining) to 3 (severe staining). Thus, the maximum score that could be obtained from the staining of 1 eye was 9. The evaluation method of fluorescein staining is shown on Figure 1 . The Schirmer test was performed without anesthesia as follows. A Schirmer test strip was placed on the lower conjunctival sac without touching the cornea for 5 minutes, and the length of the wet portion was measured. To determine TBUT, a drop of 2% fluorescein solution was instilled in the lower conjunctival sac. The time from normal blinking to the first appearance of a dry spot in the tear film was measured.
Hertel exophthalmometry values, margin reflex distance (MRD) 1 and MRD-2, and a 7-point scale of the clinical activity score (CAS) for assessment of TED condition also were determined. In Hertel exophthalmometry measurements, distance from the corneal apex to a plane defined by the deepest point on the lateral orbital rim was measured. A base value, the distance between the 2 footplates, was documented at the first measurement and reproduced at the follow-up examinations. MRD-1 and MRD-2 were measured as the distance from the upper (MRD-1) or lower (MRD-2) eyelid margin to the corneal light reflex in the primary eye position. The patient was set in the sitting position with brow fixation and was requested to look at a light source (a pen torch), then the distances were recorded using a millimeter ruler. The CAS consists of 7 parameters, including retrobulbar discomfort, pain on eye movement, eyelid erythema, eyelid swelling, conjunctival injection, chemosis, and swollen caruncle. When the CAS was 4 points or more, it was defined as active TED. All examinations were performed by one of the authors (H.K.).
Patient ages and measurement values were expressed as the mean value ± standard deviation. The presence of SLK was compared before and after treatment using the Fisher exact probability test. The Wilcoxon signed-rank test was used to compare the rose bengal staining scores and the area and density classification scores before and after treatment. The paired t test was used to compare the results of the Schirmer test and TBUT before versus after treatment. We compared Hertel exophthalmometry values after treatment and MRD-1 and MRD-2 between eyes with or without SLK at the 4 week follow-up examination using the Mann–Whitney U test. The presence of proptosis of more than 17.7 mm (the upper limit of the Japanese normal proptosis value) and upper (the upper eyelid margin located above the upper corneal limbus) and lower (the lower eyelid margin located below the lower corneal limbus) eyelid retraction were compared between eyes with or without SLK at the 4-week follow-up examination using the Fisher exact probability test. Statistical analysis was performed using SPSS II software for Windows (SPSS Japan, Inc, Tokyo, Japan). P < .05 was considered statistically significant.
Results
Thirty-three eyes from 20 patients (15 right eyes and 18 left eyes; 4 men and 16 women; mean age, 43.4 ± 11.0 years; range, 26 to 66 years) were included in this study ( Table 1 ). All patients had taken antithyroid drugs before starting rebamipide treatment. Six of 20 patients (30.0%) continued to exhibit signs of hyperthyroidism, whereas the other 14 (70.0%) were considered to be controlled euthyroid patients. Before treatment, 10 (6 patients) of 33 eyes (30.3%) exhibited Hertel exophthalmometry values of more than 17.7 mm. Ten (7 patients) of 33 eyelids (30.3%) and 12 (9 patients) of 33 eyelids (36.4%) showed upper and lower eyelid retraction, respectively. All patients were judged as having inactive TED on the basis of the CAS. These results had not changed at the 4-week follow-up.
| No. of eyes/patients | 33/20 |
| Right/left | 15/18 |
| Male/female | 4/16 |
| Age (range), y | 43.4 ± 11.0 (26 to 66) |
| No. of patients | |
| With hyperthyroidism | 6 |
| With euthyroidism | 14 |
| Hertel exophthalmometry (range), mm | 16.7 ± 2.2 (12.5 to 21.0) |
| MRD-1 (range), mm | 4.9 ± 1.5 (3.0 to 10.5) |
| MRD-2 (range), mm | 5.7 ± 0.9 (3.5 to 8.0) |
| Before Treatment | After Treatment | P Value | |
|---|---|---|---|
| Presence of SLK (no. of eyes) | 33 | 5 | < .001 a |
| Rose bengal staining score (range) | 2.8 ± 1.0 (2 to 6) | 0.8 ± 1.1 (0 to 4) | < .001 b |
| AD classification | |||
| A (range) | 1.4 ± 0.7 (0 to 3) | 0.3 ± 0.5 (0 to 1) | < .001 b |
| D (range) | 1.5 ± 0.8 (0 to 3) | 0.4 ± 0.7 (0 to 2) | < .001 b |
| Schirmer test results (range), mm | 13.2 ± 8.6 (0 to 31) | 14.5 ± 10.4 (0 to 35) | .212 c |
| TBUT (range), s | 2.8 ± 1.4 (1 to 7) | 3.5 ± 2.0 (2 to 8) | .009 c |
a Fisher exact probability test.
Although SLK was present before treatment in all patients, treatment completely resolved signs in 28 eyes (84.8%; P < .001; Figure 2 and Table 1 ). In the other 5 eyes (15.2%), punctate rose bengal staining near the upper corneal limbus remained, but decreased substantially. Each of these 5 eyes exhibited at least 1 of the following findings: proptosis of more than 17.7 mm and upper and lower eyelid retraction. Upper eyelid retraction was more prevalent in eyes with SLK than in those without SLK at the 4-week follow-up ( P = .021; Table 2 ). After treatment, MRD-1 was significantly larger in eyes with SLK than in those without SLK at the 4-week follow-up ( P = .007). The difference in Hertel exophthalmometry values after treatment, MRD-2, and the number of eyes with proptosis of more than 17.7 mm or lower eyelid retraction was not significant between eyes with and without SLK at the 4-week follow-up ( P > .050).