Purpose
To investigate the time-period characteristics associated with morphologic changes in idiopathic central serous chorioretinopathy (CSC) using volume scans acquired by spectral-domain optical coherence tomography (SD-OCT).
Design
Retrospective, observational, cross-sectional case series.
Methods
Patients underwent visual acuity measurements, fundus examinations, fluorescein angiography, indocyanine green angiography, and SD-OCT volume scans. Patients were classified into 5 categories—acute CSC, early chronic (EC) CSC, late chronic (LC) CSC, sequelae of CSC, or recurrent CSC—according to the chronicity and the recurrence. We investigated the relationship between our classification and the detailed morphologic changes of the retinal pigment epithelium and outer retina that were observed in the SD-OCT images.
Results
A total of 76 eyes from 75 patients were included in this study. Serous retinal detachment was relatively higher in acute CSC. Low to flat pigment epithelial detachments (PEDs) were most commonly observed in all stages of CSC, especially in LC CSC, but some semicircular PEDs were occasionally observed in eyes with acute or EC CSC. Retinal dragging with fibrin was most frequently observed in eyes that were in the early stage of acute CSC. A thickened posterior surface of the detached retina was most commonly observed in eyes with acute CSC, whereas a thinned posterior surface of the detached retina was observed in eyes with LC CSC. Hyperreflective dots and subretinal exudates were more commonly observed in eyes with EC and LC CSC than in eyes with acute CSC. In eyes with recurrent CSC, 2 different patterns of SD-OCT findings were observed; these patterns resembled those that were found in either acute CSC or LC CSC.
Conclusions
SD-OCT finding patterns in CSC eyes differ according to the chronicity and the recurrence of the disease. Detailed investigation of the retinal pigment epithelium and outer retina using SD-OCT could be useful for estimating the duration of CSC.
Idiopathic central serous chorioretinopathy (CSC) is a condition that is characterized by a serous detachment of the neurosensory retina at the posterior pole that typically affects young and middle-aged adults. The retinal detachment that is observed in CSC is caused by choroidal vascular hyperpermeability that can be visualized using indocyanine green angiography (IA), and focal leakage at the level of the retinal pigment epithelium (RPE) can be observed using fluorescein angiography (FA).
Spectral-domain optical coherence tomography (SD-OCT) is a noninvasive method that is often used to evaluate the structural abnormalities of CSC in more detail. Many studies have described the detailed morphologic changes that occur in eyes with CSC, particularly the changes that occur in the RPE and the outer retina, including serous retinal detachment (SRD), RPE abnormalities such as pigment epithelial detachment (PED), and small protrusions of the RPE, focal defects in the RPE monolayer at the leaking site, fibrinous exudates in the subretinal space, and subretinal precipitates.
When evaluating CSC, an understanding of the chronicity of the disease is important for determining the treatment plan. Acute CSC usually has a self-limited natural course, whereas chronic CSC with sustained SRD may need an active intervention, such as photodynamic therapy (PDT), to prevent permanent visual disturbance. Therefore, the determination of the chronicity of the disease is important for making an appropriate treatment choice and for predicting the prognosis. However, because there has been no definite objective method for estimating the chronicity of CSC to date, the chronicity of CSC is usually determined from the subjective recall of the patient.
In this study, we classified CSC according to the chronicity and the recurrence of the disease, and we investigated the relationships between our classification criteria and the detailed morphologic changes of the RPE and outer retina that can be observed using SD-OCT. The aim of this study is to propose characteristic time-period-dependent SD-OCT results that are associated with CSC for use as evidence in determining the chronicity of the disease.
Methods
Patients
We retrospectively reviewed the medical records of patients with idiopathic CSC who were examined at the Hanyang University Hospital between October 1, 2008 and November 30, 2011. Data from 76 eyes of 75 patients were included in this study. All of the patients who were included had undergone comprehensive ophthalmic examinations, including FA, IA (F-10; Nidek, Gamagori, Japan), and SD-OCT. Optical coherence tomography (OCT) was performed using a 3D OCT-1000 or -2000 (Topcon, Tokyo, Japan) to perform a volume scan. The volume scan protocol generates a cube of data through a 6-mm-square grid after acquiring a series of 128 horizontal scan lines, each of which is composed of 512 A-scans.
Idiopathic CSC was diagnosed based on the presence of a serous detachment of the neurosensory retina involving the macula that was confirmed by SD-OCT, leakage at the level of the RPE on FA, and choroidal hyperpermeability on IA. Eyes with other retinal abnormalities, such as neovascular maculopathy (ie, polypoidal choroidal vasculopathy, age-related macular degeneration, idiopathic choroidal neovascularization, or retinal vascular diseases), intraocular inflammation, and posterior segmental tumor were excluded from the study. In addition, patients who had steroid-induced CSC, organ transplant–associated CSC, or a history of previous treatment for CSC, such as laser photocoagulation or PDT, were also excluded. In this study, we analyzed only those SD-OCT images that had an image quality factor (the value of the presenting image quality of Topcon SD-OCT images) of more than 45.
Classification of the Disease According to the Chronicity and Recurrence of Central Serous Chorioretinopathy
We classified CSC patients into 5 categories: acute, early chronic, late chronic, recurrent, and sequelae. CSC patients for whom the onset of subjective symptoms such as visual loss, metamorphopsia, chromatopsia, or micropsia had occurred within the past 6 weeks were defined as having acute CSC; symptom onset between 6 weeks and 6 months prior to the patient’s hospital visit was classified as early chronic (EC) CSC; and symptom onset that had occurred 6 months or more prior to the date of the patient’s office visit was considered late chronic (LC) CSC. We only considered the patients with a first episode of CSC as having acute CSC if their disease satisfied both of the following conditions: 1) no recurrent CSC episode was discovered during the subjective recollection of the patient’s history or the review of his or her medical records, and 2) the patient had no background fundus changes that suggested that he or she had recurrent or chronic CSC, such as atrophic retinal and RPE changes, or visible drainage tract or other atypical dye leakage during FA at the initial examination. Patients who had an apparent previous history of CSC in their medical records and remnant symptoms, but no SRD when assessed using SD-OCT, were classified as having sequelae of CSC. Patients who had a reappearance of CSC-related symptoms and SRD that were revealed by means of SD-OCT were defined as having recurrent CSC if there was a previous resolution of CSC that was apparent from their subjective medical history reports or their medical records. We subdivided the patients with recurrent CSC into 2 groups: fresh recurrent CSC and sustained recurrent CSC. Fresh recurrent CSC referred to the cases in which SRD recurred after there was either complete anatomical recovery such as restored photoreceptor layer on SD-OCT from a previous CSC episode or complete disappearance of its symptoms, whereas sustained recurrent CSC was used to describe the cases in which SRD recurred either without complete anatomical recovery from a previous CSC episode or without complete disappearance of its symptoms.
Analysis of Spectral-Domain Optical Coherence Tomography Images
Using SD-OCT images that were obtained at the initial visits of the patients, we investigated various morphologic changes of the RPE and the outer retina in detail. We reviewed both whole OCT scans and scans that were approximately the site of the leakage that was observed during FA. The volume scan protocol that was used here provides a more faithful representation of detailed morphologic changes of the RPE and the outer retina than the raster scan protocol which has a longer spatial interval between each horizontal scan line, and it does so without omission. Thus the volume scan protocol enabled us to detect any tiny alterations of the RPE and the outer retina. Moreover, the volume scan protocol can display a composite fundus image by summing the shadowgrams in the Z direction; this composite image was used to register the location of the leakage point. To determine the corresponding B-scan image that was at or nearest the leakage point, the FA image was superimposed onto this projected fundus image.
Description of Subretinal Pathologies That Were Observed Using Spectral-Domain Optical Coherence Tomography
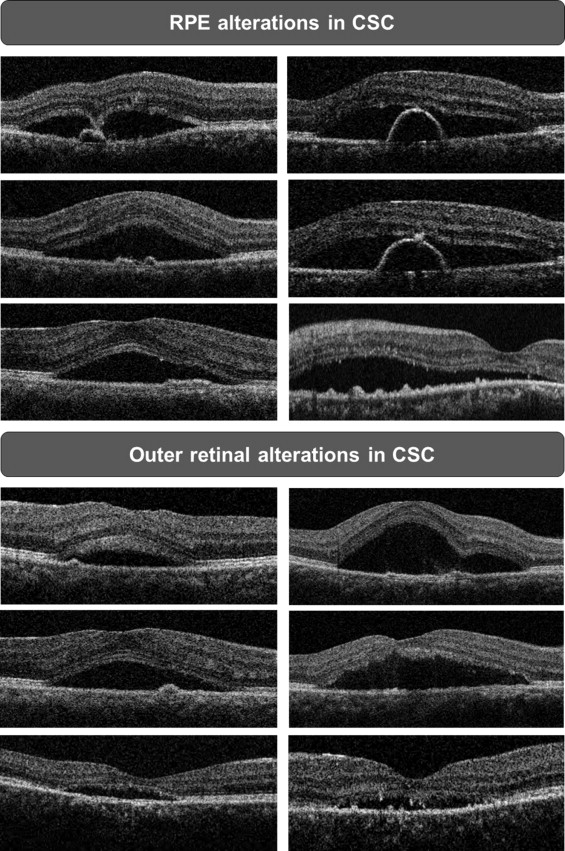
We described the abnormalities of the RPE and outer retina as follows: SRD, PED, RPE protrusion, thickened or thinned posterior surface of the detached retina, granulations of the posterior surface of the detached retina, hyperreflective dots, focal RPE defect within the PED, focal RPE proliferation, and subretinal fibrinous exudates ( Figure 1 ). The height of the SRD was obtained by measuring the distance between the highest points of the SRD and the RPE. The presence of PEDs near leakage sites that were observed during FA was investigated. The morphology of a PED was classified into 1 of 2 types: semicircular PED or low to flat PED. A semicircular PED was defined as a PED that had a typical semicircular pattern of variable size. A low to flat PED was defined as a small PED that had an irregular low or flat pattern. RPE protrusion was defined as the presence of multiple RPE bumps in the absence of optically empty space beneath the RPE layer. Several previous OCT studies have used the term “RPE irregularity” to describe instances in which either a variant of a small PED or irregular RPE thickening appeared near the leakage site that was revealed using FA. However, in our study, the classification of an RPE protrusion was differentiated from that of a PED on the basis of the presence of optically empty space in an SD-OCT image. Retinal dragging with fibrin was defined as the focal dipping or dragging of the detached retina that was accompanied by subretinal fibrin. Thickening or thinning of the posterior surface of the detached retina was described by evaluating the status of the outer photoreceptor layer. A thickened posterior surface of the detached retina was defined as a generalized, smooth thickening of the outer photoreceptor layer, whereas a generalized, smooth thinning of the outer photoreceptor layer was classified as a thinned posterior surface of the detached retina. Granulation of the posterior surface of the detached retina was defined as localized, irregular thickening of the outer photoreceptor layer. Hyperreflective dots were defined when small intense hyperreflective dots were either scattered in the intraretinal area or attached to the posterior surface of the detached retina. Focal RPE defect within the PED at the leakage point on FA was defined only when a high OCT signal was seen in the choroid layer posterior to the defect for preventing confusion from a posterior shadowing effect by a dense structure such as blood vessels. Focal RPE proliferation was defined when a focal hyperreflective mass was present at or near the focal RPE defect within the PED. Subretinal fibrinous exudates were defined as relatively hyperreflective lumps that appeared in the subretinal space.