Purpose
To evaluate status of the external limiting membrane (ELM) as a contributor of visual acuity (VA) in age-related macular degeneration (AMD).
Design
Hospital-based, cross-sectional study.
Methods
We retrospectively reviewed spectral-domain optical coherence tomography images of 158 patients with AMD who had undergone photodynamic therapy and classified them based on the status of the ELM: absent, discontinuous, or complete. We simultaneously assessed foveal thickness, presence or absence of subretinal fluid/mass, presence or absence of subretinal pigment epithelium fluid/mass, status of the inner segment/outer segment (IS/OS) junction, and status of the intermediate line between the IS/OS junction and retinal pigment epithelium. Correlation coefficients between each parameter and VA were analyzed.
Results
There was a strong correlation between ELM status and VA (r = −0.75, P < .001), and that was higher than that of the IS/OS (r = −0.69, P < .001). Multivariate analysis showed that ELM status is the most important factor for VA. Other parameters that correlated with VA included age, status of the intermediate line, and presence of subretinal or subretinal pigment epithelium fibrosis. Foveal thickness showed V-shaped correlation, with the dividing line around 200 μm.
Conclusion
ELM status may be more useful than is IS/OS status in evaluation of retinal morphology and function in patients with AMD.
Exudative age-related macular degeneration (AMD) is a condition that is characterized by abnormal choroidal neovascularization (CNV). This CNV causes hemorrhage and exudation, either of which can lead to photoreceptor cell death. Despite new treatment strategies, including use of anti–vascular endothelium growth factor (VEGF) agents and photodynamic therapy (PDT), the disease remains a major cause of acquired blindness in developed countries.
Great strides have been made recently in the diagnosis and management of AMD. Optical coherence tomography (OCT), which allows for noninvasive visualization of normal retina as well as of pathologic conditions, is now widely accepted as a standard tool in clinical practice and in the management of AMD.
Although resolution of the older OCT devices was limited, currently available spectral-domain OCT (SD-OCT) machines achieve up to 5 μm resolution; indeed, newer SD-OCT devices have allowed layer-by-layer evaluation of the retina.
Among the features depicted with OCT, outer nuclear layer thickness and status of the inner segment/outer segment (IS/OS) junction are popular hallmarks for assessing photoreceptor integrity and have been correlated with visual function in various macular pathologies. In fact, previous studies showed that continuity of the IS/OS line is important for good visual acuity (VA) in AMD patients who were treated with PDT or with anti-VEGF agents. Although the IS/OS line, which is detectable even with previous models of OCT, such as Stratus OCT (Carl Zeiss, Dublin, California, USA), is certainly correlated with VA, presence of the IS/OS line often cannot be confirmed in advanced stages of AMD. For example, the IS/OS line was not detected in 55% to 65% of eyes in previous reports. Although complete loss of the IS/OS line indicates severe retinal damage and is informative, another parameter is needed to evaluate changes that occur after its disappearance. It remains unclear whether or not there is a more optimal parameter for assessing retinal damage in patients with AMD.
The external limiting membrane (ELM) is a candidate for assessing retinal integrity, and the relationship between ELM status and VA has been reported for central serous chorioretiopathy and for retinal vein occlusion. Although resolution of previous models of OCT limited detailed observation of the ELM, improved resolution now facilitates visualization and evaluation of the ELM. In the study described herein, we evaluated the status of the ELM as a predictor of VA, and also looked at several other factors, including retinal thickness, intraretinal/subretinal fluid, and status of the IS/OS line, in order to define which parameter has the highest correlation with VA in AMD patients.
Subjects and Methods
We retrospectively reviewed the clinical records of patients who were examined with Spectralis OCT (Heidelberg Engineering, Dossenheim, Germany) more than 6 months after the last PDT at Kobe City Medical Center General Hospital. When a patient underwent PDT in both eyes, only the right eye was included in this study. Concerning OCT images, when appropriate eye tracking and averaging of more than 40 images could not be performed, the image was excluded from the study. Clinical and OCT data were gathered in May 2009; the latest OCT image of each patient at that point and visual acuity measured on the same day were analyzed. Initial and follow-up fluorescein angiography (FA) and indocyanine angiography (IA) were performed with the HRA2 (Heidelberg Engineering). PDT with verteporfin (Visudyne, Novartis AG, Basel, Switzerland) and a 689-nm laser system (Carl Zeiss, Dublin, California, USA) was carried out according to a standardized protocol. When exudative changes, such as retinal edema or subretinal fluid, were observed on periodic FA/IA and/or OCT, the patient underwent re-treatment.
SD-OCT images were obtained with Spectralis (Spectralis Family Acquisition Module, version 4.0.2.0, Heidelberg, Germany) with Heidelberg Eye Explorer (version 1.6.1.0, Heidelberg, Germany). Horizontal scans of the macula were recorded for each eye. The measurements were performed under pupillary dilation. The eye tracking system of the device was used to assure that the scans made were in the correct position; the position of the fovea was manually detected during examination. More than 40 scans were averaged for each record.
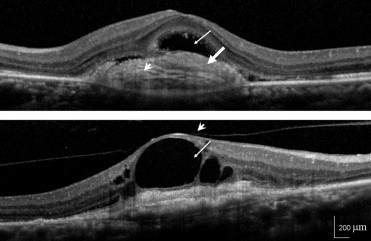
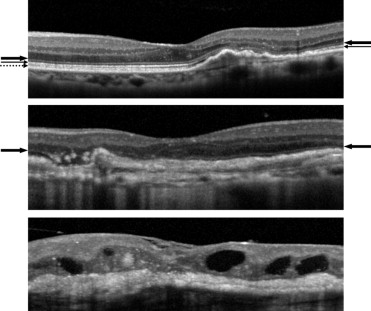
We judged the presence or absence of intraretinal fluid, subretinal fluid, subretinal fibrosis, subretinal pigment epithelium (sub-RPE) fluid, sub-RPE fibrosis, and vitreous adhesion for each image ( Figure 1 ). The judgment was performed for a 2-mm-diameter area, which was based on the diameter of physiologic fovea being 1.85 mm. The status of foveal ELM, IS/OS, and the intermediate line were judged for each image as absent, discontinuous, or complete ( Figure 2 ). Foveal thickness was defined as the distance between the vitreoretinal border and the edge of the RPE. When retinal detachment or subretinal fibrosis was seen, the inner border of the subretinal fluid or fibrosis was used arbitrarily as the outer boundary. As controls, we measured retinal thickness of contralateral eyes that did not have any retinal disease or condition, such as soft drusen, AMD, diabetic retinopathy, or retinal vessel occlusion. Two of the authors (A.O., M.H.), who were masked as to VA of the study participants, performed all of these measurements. The average of 2 measures was taken as the retinal thickness. When there were discrepancies in the judgments of the parameters, another author (M.S.) made the final decision. Clinical characteristics, including age and sex, were also reviewed and analyzed.
The statistical program SPSS (version 11.0.1, SPSS Japan, Tokyo, Japan) was used to analyze the sample data. Descriptive analyses are reported as means ± standard deviation unless otherwise specified. Visual acuities were measured with a Landolt C chart and then converted to logarithm of the minimal angle of resolution (logMAR) equivalents. Bivariate relationships were examined using the Spearman correlation coefficient. Measurement values of the groups were compared using one-way analysis of variance (ANOVA) with Bonferroni correction. To investigate which parameter is important for VA, multivariable stepwise logistic regression analysis was performed setting VA as a dependent variable. P values of less than .05 were considered to be statistically significant.
Results
A total of 158 eyes of 158 patients with AMD met the inclusion criteria. The mean age of the enrolled patients was 74.1 ± 8.9 years; there were 112 men and 46 women. Pretreatment CNV type was predominantly classic in 31 patients, minimally classic in 78 patients, and occult with no classic in 49 patients. Seventy-six patients were diagnosed as having polypoidal choroidal vasculopathy and 7 were diagnosed with retinal angiomatous proliferation. The participants had undergone relatively small numbers of PDT an average of 1.8 ± 0.8 times, and their logMAR VA was 0.71 ± 0.51. Foveal thickness was 167.6 ± 107.2 μm, whereas foveal thickness data obtained from 81 healthy fellow eyes was 203.2 ± 17.2 μm.
The correlation coefficients between each parameter and the logMAR VA are shown in the Table . Status of the ELM, IS/OS, and intermediate line, as well as presence of subretinal fibrosis, showed a relatively strong correlation. Age, intraretinal fluid, sub-RPE fluid, and sub-RPE fibrosis were only mildly correlated with logMAR VA.
| Age | Intraretinal Fluid | ELM | IS/OS | Intermediate Line | Subretinal Fibrosis | Sub-RPE Fluid | Sub-RPE Fibrosis | Sex | Subretinal Fluid | Vitreous Adhesion | |
|---|---|---|---|---|---|---|---|---|---|---|---|
| +:37 −:121 | +:46 ±:57 −:55 | +:15 ±:44 −:99 | +:0 ±:24 −:134 | +:80 −:78 | +:35 −:123 | +:118 −:40 |
| +:37 −:121 | +:28 −:130 | |
| r | 0.29 | 0.28 | −0.75 | −0.69 | −0.47 | 0.59 | −0.19 | 0.20 | −0.08 | −0.13 | −0.10 |
| P | <.001 | <.001 | <.001 | <.001 | <.001 | <.001 | .015 | .008 | .346 | .102 | .210 |
The most important multivariate predictor of VA was ELM status (r 2 = 0.541) followed by age (ELM status and age: r 2 = 0.572). The correlation was strengthened when adding subretinal fibrosis (ELM status, age, and subretinal fibrosis, r 2 = 0.600) and IS/OS (ELM status, age, subretinal fibrosis, and IS/OS, r 2 = 0.610) ( P < .001, P = .001, P = .001, P = .024 for ELM, age, subretinal fibrosis, and IS/OS, respectively).
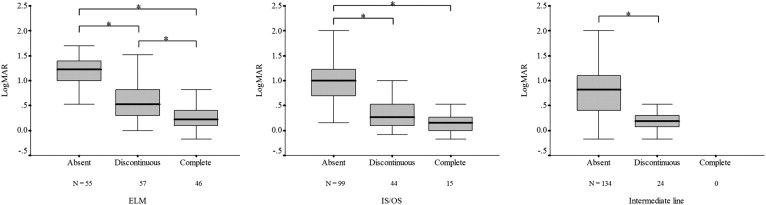
Figure 3 shows logMAR VA and status of the ELM ( Figure 3 , Left), IS/OS ( Figure 3 , Middle), and intermediate line ( Figure 3 , Right). Note that a relatively small percentage of patients showed complete IS/OS and no patient showed complete intermediate line. The absence or disruption of the line was associated with poor logMAR VA when the ELM was considered, but a difference was seen only between absent and the 2 other groups when the IS/OS was considered. The significant difference was also found between absent and discontinuous intermediate line groups.