Purpose
To describe the clinical presentation of uveitis with coincident onset of raised and indurated tattooed skin.
Design
Case series.
Methods
Seven consecutive patients were evaluated at a tertiary ophthalmologic facility with coincident uveitis and cutaneous tattoo induration over an 18-month period. All subjects underwent complete ophthalmic examination and a focused systemic medical evaluation including serologic testing and imaging studies. Two participants underwent biopsy of their tattoos. The patients’ clinical courses and responses to treatment over a follow-up period of 1–20 months are reported (mean follow-up = 9 months). Main outcome measures included degree of intraocular inflammation, ocular complications, visual acuity, clinically observable tattooed skin changes, and biopsy results.
Results
Five of 7 patients had bilateral nongranulomatous anterior uveitis: 4 with chronic and 1 with recurrent disease. The remaining 2 patients had bilateral chronic granulomatous panuveitis. Biopsies of raised and indurated tattoos were performed in 2 patients and demonstrated noncaseating granulomatous inflammation surrounding tattoo ink in the dermis. The skin changes resolved in all patients, with a faster response noted in those treated with high-dose oral prednisone for intraocular inflammation. Five patients subsequently experienced recurrent flares of intraocular inflammation in conjunction with the recurrence of raised and indurated tattoos.
Conclusions
These cases represent a subset of patients in whom skin tattooing may have incited an immune response leading to simultaneous inflammation of the eyes and tattooed skin.
In 1952, Lubeck and Epstein published the first report of a patient with bilateral intraocular inflammation and simultaneous tattoo granulomas in the setting of systemic sarcoidosis. This was followed, in 1969, by the first case series to describe bilateral intraocular inflammation with the simultaneous development of tattoo granulomas in 3 patients felt to have no evidence of systemic sarcoidosis at the time of presentation. The pathologic hallmark of sarcoidosis is the noncaseating granuloma; however, it remains a diagnosis of exclusion because of its lack of pathognomonic histopathology, imaging, or serologic studies. Among patients with sarcoidosis, anywhere from 25% to 80% may suffer from ocular or adnexal involvement, and approximately 25%–35% of patients develop cutaneous findings. Anterior uveitis is the most common ocular manifestation of sarcoidosis, occurring in 65% of patients with ophthalmic involvement.
We present 7 patients with no prior diagnosis of sarcoidosis who developed bilateral uveitis in temporal association with inflammation of tattooed skin.
Methods
A retrospective review of 7 consecutive patients with bilateral uveitis and associated cutaneous changes suggestive of tattoo inflammation evaluated over a 20-month period was conducted at the Division of Ocular Immunology, Wilmer Eye Institute. The study was approved by the Johns Hopkins School of Medicine Institutional Review Board and adhered to all tenets of the Declaration of Helsinki. All patient data were handled in accordance with the Health Information Portability and Accountability Act.
All patients underwent a complete ophthalmologic examination and received a medical evaluation ( Table ) in an attempt to rule out syphilis (fluorescent treponemal antibody-absorption [FTA-ABS] and rapid plasma reagin testing [RPR]) and sarcoidosis (chest x-ray and/or computed tomography [CT] chest, serum angiotensin-converting enzyme [ACE] and/or serum lysozyme). Testing for HLA-B27 positivity and infectious etiologies such as Mycobacterium tuberculosis , Toxoplasma gondii , Bartonella henselae , and Borrelia burdorferi was performed in selected patients. Two of the 7 patients underwent biopsy of their inflamed tattoos. The patients’ clinical courses and responses to treatment were reviewed over a follow-up period of 1–20 months.
| Patients | Demographics | Initial VA | Intraocular Inflammation | Uveitic Evaluation a | Sarcoidosis Evaluation a | Tattoo Findings | Tattoo Biopsy | Ocular Complications | Treatment | Follow-up Duration |
|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 20yo AAM | OD(sc): 20/100, OS(sc): 20/400; PHNI OU | Bilateral granulomatous chronic panuveitis | RPR, FTA-ABS, HLA-B27, IGRA, Lyme serology, Toxoplasma IgG, CMP, CBC | ACE, chest x-ray (×2) | Elevation/induration of skin tattooed with black pigment (predominantly black tattoos on arms, chest, and abdomen) | Noncaseating granulomatous reaction associated with tattoo ink | OU: posterior synechiae, glaucoma s/p Baerveldt glaucoma implants | Mycophenolate mofetil, oral prednisone, topical corticosteroids, and IOP-lowering drops | 13 months |
| 2 | 31yo WM | OU(sc): 20/25; PHNI OU | Bilateral nongranulomatous recurrent anterior uveitis | RPR, FTA-ABS, HLA-B27, PPD, CMP, CBC | ACE, lysozyme, chest x-ray, CT chest, lymph node biopsy b | Elevation/induration of skin tattooed with black pigment (multicolored, extensive tattoos on both arms) | Noncaseating granulomatous reaction associated with tattoo ink | OU: steroid-associated ocular hypertension | Topical corticosteroids, IOP-lowering drop | 17 months |
| 3 | 32yo AAM | OU(sc): 20/25-2; PHNI OU | Bilateral nongranulomatous chronic anterior uveitis | RPR, FTA-ABS, HLA-B27, Lyme serology, CMP, CBC | ACE, chest x-ray | Elevation/induration of skin tattooed with black pigment on both arms (black tattoos on chest never involved) | Not performed | OU: pupillary mebranes, cataracts, CME OD: posterior synechiae OS: iris bombe, uveitic glaucoma | Methotrexate, oral prednisone, topical corticosteroids, IOP-lowering drops | 20 months |
| 4 | 23yo AAF | OD(sc): 20/40, OS(sc): 20/200-2; PHNI OU | Bilateral nongranulomatous chronic anterior uveitis | RPR, FTA-ABS, HLA-B27, Lyme serology, CMP, CBC | Lysozyme, chest x-ray | Elevation, induration, and scaling of tattoos with black ink (multicolored tattoos on face, neck, torso, back, and all limbs) | Not performed | OU: posterior synechiae, pupillary membranes, iris bombe, severe CME OS: uveitic glaucoma | Mycophenolate mofetil, oral prednisone, topical corticosteroids, IOP-lowering drops | 7 months |
| 5 | 23yo AAM | OD(sc): 20/25, OS(sc): 20/20+1; PHNI OU | Bilateral nongranulomatous chronic anterior uveitis | RPR, FTA-ABS, HLA-B27, Lyme serology, | ACE, chest x-ray | Elevation/induration of skin tattooed with black pigment (black tattoos on arms/chest) | Not performed | OS: posterior synechiae | Topical corticosteroids | 4 months |
| 6 | 21yo AAF | OD(sc): 20/100, OS(sc): 20/40; PH 20/80 OD, PHNI OS | Bilateral nongranulomatous chronic panuveitis with hypopyon | RPR, FTA-ABS, HLA-B27, PPD, Lyme serology, Bartonella antibody panel, CMP, CBC | ACE, b chest x-ray | Elevation/induration of skin tattooed with black pigment (multicolored tattoos on back) | Not performed | OU: severe optic nerve elevation and hyperemia with papillomacular exudates, ERM OD: subfoveal RPE detachment | Oral prednisone, topical corticosteroids | 2 months |
| 7 | 42yo AAM | OD(sc): 20/20, OS(sc): 20/40; PHNI OD, PH OS 20/32 | Bilateral nongranulomatous chronic anterior uveitis | FTA-ABS, HLA-B27, CMP, CBC | ACE, lysozyme, b chest x-ray, CT chest | Elevation/induration of skin tattooed with black pigment (arm) | Not performed | OU: posterior synechiae OD: neurosensory retinal detachment OS: severe CME | Oral prednisone; systemic immunosuppression recommended | 1 month (lost to follow-up) |
a All results unremarkable/negative unless otherwise indicated.
b Patient 2 underwent biopsy of an enlarged axillary lymph node, which displayed a noncaseating granulomatous reaction. Patient 6 had an elevated ACE value of 85 (reference range: 9–67 U/L). Patient 7 had an elevated lysozyme value of 32 (reference range: 9–17 μg/mL) and a normal serum ACE value of 47.
Selected Case Report: Patient 1
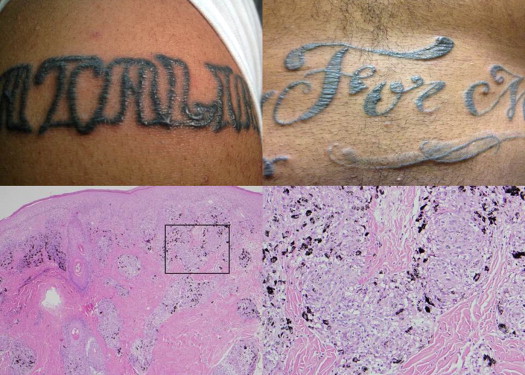
Patient 1 was a 20-year-old African-American man who initially presented for evaluation of a 1-week history of blurred vision, photophobia, and pain in both eyes. He had experienced similar symptoms 6 months earlier, which lasted approximately 1 month before spontaneously resolving. Review of systems was notable for elevation and swelling of 8 tattoos on his arms and chest that occurred in conjunction with his ocular symptoms on both occasions ( Figure 1 ). All of his tattoos were performed during a 1-year period, approximately 6 months prior to his initial ocular complaints.

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


