Purpose
To describe and evaluate the severity of pediatric blepharokeratoconjunctivitis in Asia.
Design
Retrospective case series.
Methods
Clinical records of patients diagnosed with pediatric blepharokeratoconjunctivitis at a tertiary referral center in Singapore from 1991 through 2010 were reviewed. Patients were graded as having mild (corneal involvement without scarring), moderate (corneal scarring), or severe (corneal scarring with thinning or perforation) disease based on recorded clinical findings.
Results
Fifty-one patients were diagnosed with pediatric blepharokeratoconjunctivitis. The mean age at presentation was 10.2 ± 3.6 years, most patients were female (80.4%), and the mean duration of follow-up was 58.9 ± 44.0 months. Chinese (56.9%) subjects made up most of the cases. Most subjects had moderate (56.9%), followed by severe (37.4%) and mild (5.9%), disease. Four patients (7.9%) had an associated dermatologic disease. All patients were treated with topical antibiotics, and 98% were treated with topical steroids. Nineteen (37.3%) patients received systemic antibiotic therapy, and 1 received systemic steroid therapy. Three patients required deep lamellar keratoplasty (2 tectonic and 1 optical), and 2 underwent cornea gluing alone; all 5 of them were Chinese. Patients graded as having severe disease were more likely to undergo surgical intervention (26.3%) than patients who were graded as having moderate (0%) and mild (0%) disease ( P < .05). The main complication of treatment was raised intraocular pressure in 7 (13.7%) patients requiring medical therapy. Overall, best-corrected visual acuity improved by 0.10 logarithm of the minimal angle of resolution units ( P < .001) after appropriate medical and surgical intervention.
Conclusions
Pediatric blepharokeratoconjunctivitis patients in Asia seem to have a more severe clinical presentation and course. Early and adequate management can arrest the disease process and can minimize visual morbidity.
Pediatric blepharokeratoconjunctivitis is an underrecognized and poorly defined syndrome. It is associated frequently with a delay between disease and presentation. Jones and associates demonstrated that a 2-year lag between disease onset and presentation can result in a 0.06 logarithm of the minimal angle of resolution (logMAR)-unit reduction in visual acuity ( P = .054), which highlights that the disease can result in significant visual morbidity.
The management of pediatric blepharokeratoconjunctivitis can be challenging. Currently, there is a lack of an effective, standardized treatment regimen for the disease, with potentially sight-threatening complications like amblyopia, thinning, and perforation and treatment-related complications such as steroid-induced glaucoma and cataracts. Because this disease usually begins early in life, the lifelong burden of the disease also can affect the quality of life of the patient.
Previous studies have described the clinical spectrum, management, and visual outcomes of the disease, and attempts have been made to grade the disease. However, most studies have had small sample sizes with nonstandardized treatments and evaluations. The purpose of our study was to describe and evaluate the clinical spectrum and disease severity of pediatric blepharokeratoconjunctivitis in Asian eyes.
Methods
This study was a retrospective case series. All patients who were diagnosed with pediatric blepharokeratoconjunctivitis at a tertiary referral center in Singapore from 1991 through 2010 were included. Only patients 16 years of age and younger at presentation were included in the study. Blepharokeratoconjunctivitis was defined clinically as the presence of eyelid involvement by lid margin scarring, blepharitis, meibomitis, and chalazion or hordeolum, accompanied by epithelial or stromal keratitis, corneal scarring, vascularization, and thinning or perforation. The demographics, clinical presentation, and management outcomes of each patient were recorded.
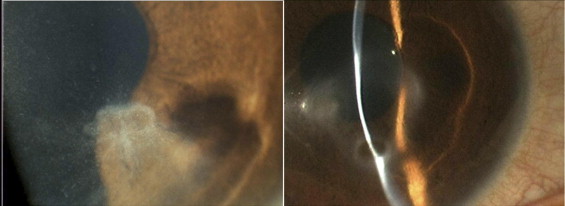
The management protocol of our patients includes daily warm compress and lid hygiene, topical antibiotics, topical steroids, topical immunosuppressant, for example, cyclosporin A 0.5%, and systemic antibiotics and systemic steroids, depending on severity of the disease and response to treatment. Patients were graded based on documented clinical corneal findings at any point during the follow-up period. Those graded with mild disease had only corneal epithelial involvement without stromal scarring, for example, punctate epithelial erosions or superficial punctate keratitis; moderate disease was defined as the additional presence of corneal stromal scarring, with or without vascularization; and severe disease was defined as corneal scarring with significant stromal thinning ( Figure 1 ) . Eye scrapings additionally were performed when an active infectious cause was suspected.
Statistical significance was set at P < .05. The chi-square and Fisher exact test were conducted for analyzing categorical data. The Wilcoxon signed rank test was conducted to compare paired preoperative and postoperative data. SPSS software version 17 (IBM Corporation, Armonk, New York, USA) was used for the analyses. Internal review board approval was secured for the study.
Results
Fifty-one patients were diagnosed with pediatric blepharokeratoconjunctivitis at our center from 1991 through 2010. The mean age at presentation was 10.2 ± 3.6 years. Females made up most of the patients: 41 (80.4%) of 51. The mean duration of follow-up was 58.9 ± 44.0 months (range, 3 to 227 months). Most of the patient were Chinese (29/51; 56.9%), followed by Indian (13/51; 25.5%) and Malay (9/51; 17.6%).
Bilateral disease was seen in most patients (33/51; 64.7%), unilateral disease in the right eye was seen in 27.5% (14/51) of patients, and unilateral disease in the left eye in was seen in 7.8% (4/51) of patients. The most common symptoms experienced were eye redness (35/51; 68.6%), tearing (13/51; 25.5%), and blurred vision (12/51, 23.5%; Table 1 ). All of the patients had lid and corneal changes, and 66.7% (34/51) had conjunctival changes. The most common lid pathologic features were meibomitis (44/51; 86.3%), blepharitis (39/51; 76.5%), and chalazion (23/51; 45.1%), whereas the most common corneal changes were corneal scarring (47/51; 92.2%), superficial vascularization (46/51; 90.2%), and punctate epithelial erosions or superficial punctate keratitis (38/51; 74.5%). Among the 51 patients, 56.9% (29/51) were graded as having moderate disease, 37.3% (19/51) were graded as having severe disease, and 5.9% (3/51) were graded as having mild disease.
| Symptoms and Signs | Number | Percentage |
|---|---|---|
| Symptoms | ||
| Redness | 35 | 68.6 |
| Tearing | 13 | 25.5 |
| Blurred vision | 12 | 23.5 |
| Pain | 11 | 21.6 |
| Irritation | 7 | 13.7 |
| Photophobia | 5 | 9.8 |
| White spot | 4 | 7.8 |
| Swelling | 3 | 5.9 |
| Discharge | 2 | 3.9 |
| Itching | 1 | 2.0 |
| Rubbing | 1 | 2.0 |
| Signs | ||
| Lid | 51 | 100 |
| Meibomitis | 44 | 86.3 |
| Blepharitis | 39 | 76.5 |
| Chalazion | 23 | 45.1 |
| Stye | 12 | 23.5 |
| Telangiectasia | 1 | 2.0 |
| Conjunctiva | 34 | 66.7 |
| Hyperemia | 26 | 51.0 |
| Papillae | 17 | 33.3 |
| Phlyctena | 8 | 15.7 |
| Follicles | 6 | 11.8 |
| Conjunctivitis | 5 | 9.8 |
| Cornea | 51 | 100 |
| Corneal scar | 47 | 92.2 |
| Superficial vascularization | 46 | 90.2 |
| Punctate epithelial erosions or superficial punctate keratitis | 38 | 74.5 |
| Marginal infiltrates | 26 | 50.9 |
| Corneal phlyctena | 19 | 37.3 |
| Thinning | 17 | 33.3 |
| Deep vascularization | 9 | 17.6 |
| Limbitis | 7 | 13.7 |
| Perforation | 2 | 3.9 |
Eye cultures were performed in only 8 patients: 6 were corneal scrapings, 1 was a conjunctival swab, and 1 was an eyelid swab. One cornea specimen isolated Pseudomonas aeruginosa , and the conjunctival swab isolated Acinetobacter baumannii with coagulase-negative Staphylococcus . All other culture results were negative. Four patients (7.9%) were diagnosed with a coexisting dermatologic condition: 3 of them were diagnosed with acne rosacea and 1 was diagnosed with acne vulgaris based on their cutaneous manifestations.
All patients were treated with topical antibiotics, and the 3 most common topical antibiotics prescribed were fucidic acid gel (47/51; 92.2%), levofloxacin (26/51; 51.0%), and tobramycin eyedrops (22/51; 43.1%). All but 1 patient received treatment with topical steroids, and the 3 most commonly prescribed were dexamethasone 1% (45/51; 88.2%), prednisolone 0.12% to 1% (34/51; 66.7%), and fluorometholone 0.1% (19/51; 37.3%). The frequency of topical steroid treatment was tapered based on response to treatment, and the dosing regimen ranged from once every 2 hours to once every other day. The mean duration of topical steroids was 16.0 ± 18.5 months. Topical cyclosporin A 0.5% was administered to 8 children (15.7%). Systemic antibiotic therapy was initiated in 19 patients (37.3%), and the older children received oral doxycycline (16/19; 84.2%), whereas younger children younger than 9 years of age received erythromycin (3/19; 15.8%) or Augmentin (3/19; 15.8%) oral therapy. The mean duration of oral antibiotic administration was 1.9 ± 4.2 months (range, 1 to 23 months). One patient had severe inflammatory disease that required systemic control with oral prednisolone.
Five patients, all of whom were Chinese, required surgical intervention during their course of follow-up. Two patients underwent a deep lamellar keratoplasty for tectonic indications and 1 patient underwent the procedure for optical indications. The case study of a patient who underwent a deep lamellar keratoplasty is shown in Figure 2 . Two other patients with spontaneous corneal perforations ( Figure 3 ) at presentation required cornea gluing, without graft surgery, with Histoacryl topical skin adhesive (B. Braun, Ann Arbor, Michigan, USA), a tissue sealant that consists of n-butyl-2 cyanoacrylate. Patients graded as having severe disease had a 26.3% chance of requiring subsequent surgical intervention for tectonic or optical indications as compared with patients who were graded as having moderate and mild disease ( P < .05, Fisher exact test (2 sided).
Complications of treatment encountered in our study population include that of raised intraocular pressure in 7 (13.7%) patients, cataract in 1 (2%) patient, and gastrointestinal disturbance from oral antibiotics in 1 (2%) patient. Those with raised intraocular pressure were treated medically with good response, and in none of them did glaucoma develop during the course of their follow-up.
At presentation, 17 eyes (33.3%) had poor vision (less than 0.3 logMAR). At final review, 8 (15.7%) of 51 eyes had persistently poor vision ( P < .01). Overall, the best-corrected visual acuity improved by 0.10 logMAR units ( P < .001, Wilcoxon signed rank test [2 sided]) after appropriate medical and surgical intervention, where the final best-corrected visual acuity was 0.2 logMAR.
A subgroup analysis of children by age groups showed that children 6 to 10 years of age required steroids for a longer duration (24.6 ± 23.4 months) than children 11 to 16 years of age (10.6 ± 11.0 months; P = .028), but there were no differences comparing children 0 to 5 years of age (6.5 ± 5.2 months) with the other groups. Subgroup comparisons by age group were not significant for the other variables like visual acuity; disease severity; use of medical treatment like antibiotics, steroids, or cyclosporin A 0.05%; corneal perforation; need for surgical intervention; or treatment-related complications.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


