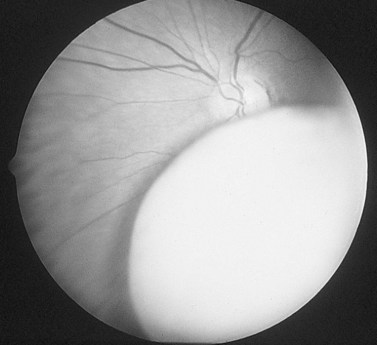
Chapter 67 Pars plana lensectomy for retained intravitreal lens material
Introduction
The most common indication for pars plana lensectomy is crystaline lens or lens fragment dislocation into the vitreous cavity as a complication of cataract extraction1–3. 97% of cataract surgeons in the United States utilize phacoemulsification in cataract surgery, and 74% do not perform planned extracapsular cataract extraction4; thus, complications sustained during phacoemulsification account for the vast majority of retained lens material cases referred to retina surgeons2,5. A comprehensive multicenter study of capsule complications conducted in Sweden demonstrated that previous trauma, white or brunescent cataract, and phacodonesis were significant preoperative risk factors for capsule complications and that loose zonules, use of trypan blue, miosis, and inexperienced surgeons were intraoperative risk factors6. The Swedish used the term capsule complication to include zonular dehiscence, capsule rupture, vitreous loss, and lens remnants lost into the vitreous6. Whereas capsule complications occur in 1–6.1% of all cataract surgeries7,8, retained lens material has been reported to complicate between 0.3% and 1.1% of cataract extractions and occurs more commonly with inexperienced surgeons3,9–13. Other indications for pars plana lensectomy include traumatic cataract, crystalline lens dislocation associated with traumatic injury14, and lens subluxation caused by a variety of systemic conditions including Marfan syndrome, homocystinuria, and PXF syndrome15–17.
Preoperative evaluation
Initial diagnostic examination
The cataract incision should be identified and evaluated for leakage. The intraocular pressure should be assessed, because secondary glaucoma is present in about 50% of patients. Corneal edema may be present as early as the first postoperative day and may result in difficulty visualizing posterior pathology. The application of topical glycerin ophthalmic solution and the reduction of an elevated intraocular pressure may be effective in temporarily reducing corneal edema and facilitating anterior segment and fundus examinations. Anterior chamber inflammation can range from mild cell and flare to a severe fibrinous reaction simulating infectious endophthalmitis18. Slit-lamp biomicroscopy and gonioscopy may identify small lens fragments in the anterior chamber angle19.
Visualization of the crystaline lens or lens fragments within the vitreous cavity by indirect ophthalmoscopy confirms the diagnosis. Cortical material appears white and fluffy (Fig. 67.1), and nuclear material appears yellowish-brown and has sharper borders, unless it is surrounded by cortex (Fig. 67.2). The examination should include indirect ophthalmoscopic examination of the peripheral retina, specifically looking for retinal tears, retinal detachment, and serous or hemorrhagic choroidal effusions. These complications are more likely to occur if the cataract surgeon has attempted to extract posterior lens fragments by irrigation or insertion of instruments into the posterior vitreous20,21.
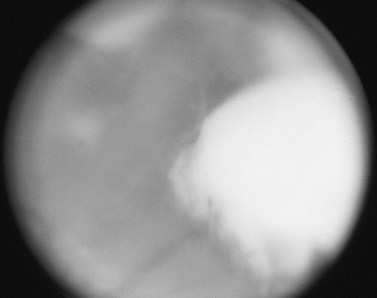
Fig. 67.1 Fundus photograph illustrating retained lens cortex in the mid vitreous following cataract surgery.
Preoperative complications
Corneal edema
Approximately 50% of eyes with retained lens fragments present with corneal edema or corneal decompensation2,5,22–27. This probably results from a combination of surgical trauma, prolonged phacoemulsification times related to the complicated cataract removal, intraocular inflammation, and increased intraocular pressure. Fortunately, the corneal edema is usually transient and resolves with conservative treatment in the majority of affected eyes. Less commonly, retained nuclear fragments sequestered in the anterior chamber may traumatize the corneal endothelium and cause substantial corneal edema and reduced visual acuity, which is reversible following surgical removal of the fragments19. Approximately 3–10% of eyes with retained lens material will develop chronic corneal decompensation and bullous keratopathy that requires penetrating keratoplasty2,12,23.
Uveitis
An inflammatory response to retained lens fragments occurs in 56–87% of eyes with retained lens material2,22,23. Initially, the affected eye may appear quiet, with severe inflammation not developing until weeks later18. Treatment with topical cycloplegic agents and corticosteroids should be instituted preoperatively. Rarely, the uveitis may be so severe that it is clinically confused with infectious endophthalmitis18.
Glaucoma
Secondary glaucoma occurs in approximately 40–50% of eyes with retained lens material2,22–24,26,27. The elevation in intraocular pressure may result from lens fragments, heavy molecular weight soluble lens proteins, and macrophages which obstruct the trabecular meshwork28–30. A steroid-induced elevation in intraocular pressure may be the responsible mechanism in some eyes, creating a confusing clinical picture. Removal of the lens particles usually results in resolution of the secondary glaucoma31. However, as many as one-third of eyes with retained lens fragments treated by vitrectomy and lensectomy demonstrate a persistence of mildly elevated intraocular pressure that requires chronic treatment5.
Retinal detachment
Cataract surgery complicated by vitreous loss is associated with a 5% incidence of retinal detachment at 4 years, which is four to five times greater than the risk following uncomplicated cataract surgery32. In eyes with retained lens fragments, the incidence of retinal detachment is even greater, affecting from 3.8% to 23% of eyes2,12,23,26,33–35. About one-half of the retinal detachments are recognized prior to, or during, vitrectomy and one-half develop postoperatively2,33,34. The development of proliferative vitreoretinopathy may be more common in eyes with retained lens material, requiring the use of silicone oil for repair and limiting the final visual acuity2. Although retinal detachment occurs in the minority of eyes with retained lens material, it is the most common identifiable cause of reduced postoperative visual acuity in several studies22,25,33.
Endophthalmitis
Endophthalmitis may occur concomitantly with retained lens fragments after phacoemulsification23,36. B-scan ultrasonography has proven useful in demonstrating the size and type of retained lens material in eyes with endophthalmitis and opaque media36. Eyes with retained lens fragments and suspected endophthalmitis should be managed with immediate injection of intravitreal antibiotics in conjunction with pars plana vitrectomy and lensectomy or vitreous tap36. The decision of whether or not to perform pars plana lensectomy should be based on the indications for eyes with retained lens material without endophthalmitis. Although 50% of patients with retained lens fragments have been reported to have positive vitreous cultures, routine vitreous cultures are not recommended because they do not identify eyes at risk for endophthalmitis or influence the clinical management37.
Preoperative management
The preoperative management of eyes with retained lens material begins once the surgeon performing the cataract surgery recognizes this complication. After the determination is made that the crystaline lens or lens fragments are posteriorly dislocated into the vitreous cavity, no further attempts should be made to retrieve them. Nuclear fragments remaining in the capsular bag should be phacoemulsified, and residual lens cortex and viscoelastic material should be removed by careful irrigation and aspiration. Anterior vitrectomy may be performed if vitreous has entered the anterior chamber. Attempts to inject fluids or manipulate instruments in the posterior vitreous cavity38 should be avoided because of the risk of inducing retinal tears or detachments and exacerbating the uveitis20,24,39
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree