Purpose
To analyze retinal thickness and volume measurements of X-linked retinoschisis patients by spectral-domain optical coherence tomography (SD OCT) and correlate these findings with visual acuity and patient age.
Design
Retrospective comparative case series.
Methods
Sixty-three eyes of 33 male patients with X-linked retinoschisis were gleaned from a SD OCT database at the University of Illinois at Chicago. Forty-one eyes of 21 patients with low refractive error, no visual impairment, and no known retinal disease served as age-similar controls. The mean age of the retinoschisis patients was 26.4 years. The mean age of patient controls was 30.0 years. Full-thickness, inner and outer retina thickness, and volume measurements were determined by SD OCT.
Results
Foveal schisis was observed in 81% of retinoschisis patients. Patients with foveal schisis tended to be younger than patients lacking foveal schisis. Inner and outer foveal thickness and volume measurements were increased in retinoschisis patients compared to controls. Outer retinal perifoveal and parafoveal thicknesses and volumes were consistently increased in retinoschisis patients relative to controls. In contrast, inner retinal perifoveal and parafoveal thickness and volume measurements were decreased in retinoschisis patients compared to controls. Worse visual acuity correlated with thinning of the temporal perifoveal inner retina and thickening of the inner fovea. Full-thickness measurements and inner retina and outer retina thickness and volume measurements tended to decrease with patient age.
Conclusion
Increased inner retinal foveal thickness and decreased perifoveal inner retinal thickness correlates with worse visual acuity and overall retinal thickness decreases with age in X-linked retinoschisis.
X-linked retinoschisis has demonstrated variable clinical and imaging findings. Early histologic reports localized the region of schisis to the nerve fiber layer. More recent studies have shown a wide spectrum of optical coherence tomography (OCT) findings in this condition, particularly in terms of location of cystoid macular changes. Additionally, analysis of the extramacular retina has demonstrated peripheral schisis apparent on OCT in many of these patients.
Prior clinical studies have demonstrated a lack of correlation between full retinal thickness at the fovea and best-corrected visual acuity (BCVA). This study aims to determine if there is a correlation between outer or inner retinal thickness and volume measurements by OCT and patient characteristics such as age and visual acuity.
Methods
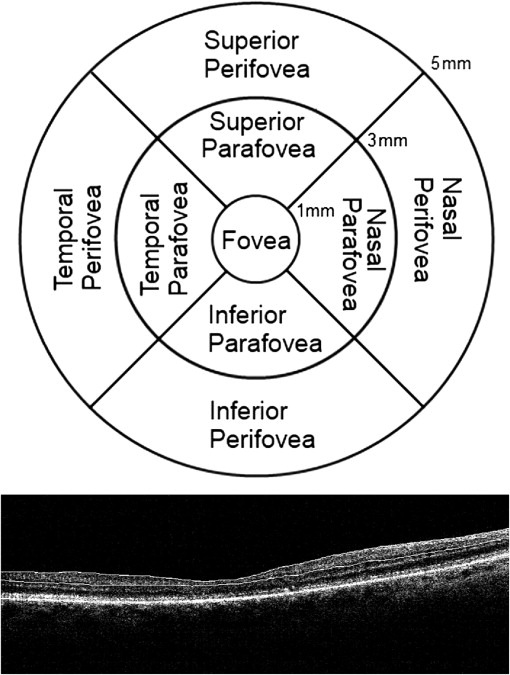
The spectral-domain optical coherence tomography (SD OCT) database was reviewed to identify patients with a diagnosis of X-linked retinoschisis who underwent SD OCT imaging. This retrospective study was approved by the Institutional Review Board at the University of Illinois Medical Center. The diagnosis of X-linked retinoschisis was based on clinical criteria including fundoscopy, electroretinogram results, and OCT findings. Age-similar controls with low refractive error, no visual impairment, and no known retinal conditions were identified in the database as a comparison group. BCVA was determined from the patient records. All OCT scans were obtained using the MM5 protocol consisting of a 5 mm by 5 mm grid of horizontal and vertical scans through the macula on an Optovue RTVue SD OCT system (Optovue Inc, Fremont, California, USA). The automated scans were reviewed and inaccurate segmentation boundaries were corrected manually. The inner retina was defined as retinal nerve fiber layer, ganglion cell layer, and inner plexiform layer for the purposes of this study. Full-thickness, inner and outer retina thickness, and volume measurements in 15 regions of the macula were automatically generated by the Optovue software and were recorded from thickness maps. These measurement regions and inner retinal segmentation boundaries are illustrated in Figure 1 . For thickness and volume measurements, evaluated regions include temporal, superior, nasal, inferior, superior hemisphere, and inferior hemisphere areas of the parafoveal and perifoveal regions, as well as the central foveal zone.
Two-tailed t tests were performed to compare means between the groups. Multiple linear regression analysis was performed to correlate OCT measurements with BCVA. Condition indices less than 15 were considered acceptable collinearity measures. Pearson correlation analysis was generated for patient age in relation to OCT measurements. A P value less than .05 was considered statistically significant.
Results
Sixty-three eyes of 33 male patients identified with X-linked retinoschisis were analyzed. Figure 2 presents the OCT image and corresponding thickness map for a retinoschisis patient with typical schisis cavities. Forty-one eyes of 21 patients served as age-similar controls. The mean age of retinoschisis patients was 26.4 years (range 7–58 years). The mean age of the age-similar controls was 30.0 years (range 11–56 years). There was no statistical difference in age distribution between the cases and controls ( P = .350). The mean logMAR BCVA for the eyes of the cases was 0.5, corresponding to a Snellen acuity of approximately 20/65. Foveal schisis was observed on OCT in 81% of the retinoschisis patient eyes. The mean age of patients without foveal schisis was 40.9 years, which was significantly older than patients with foveal schisis (22.3 years; P < .0001). Five patients required manual re-segmentation. In 2 eyes, automated or manual segmentation was deemed inaccurate owing to severe foveal schisis, and these measurements were excluded from the corresponding statistical analysis.
Figure 3 illustrates the full-thickness retinal measurements for cases and controls. Figure 4 depicts the thickness and volume measurements of the outer retina. Figure 5 summarizes the thickness and volume measurements of the inner retina. Although most of the full-thickness retinal measurements did not differ between the 2 groups, a few select full-thickness measurements, namely foveal thickness, temporal parafoveal thickness, and foveal volume, were greater in the retinoschisis group. In contrast, all of the segmented outer retina and inner retina thickness and volume measurements differed between the case and control groups. The outer retinal thicknesses and volumes were statistically increased in the X-linked retinoschisis group compared to the control group in all instances. The inner foveal thickness and volume measurements were greater in the X-linked retinoschisis patients than in the controls, while the inner retinal measurements in the perifoveal and parafoveal areas were decreased in the retinoschisis patients compared to controls.
Multiple linear regression analysis was performed with logMAR BCVA as the dependent variable and all retinal thickness and volume measurements as the independent variables. The generated regression model (R = 0.552, R 2 = 0.305, adjusted R 2 = 0.279) yielded volume of the inner retina at the fovea (beta = 0.446; P < .0001) and volume of the temporal perifoveal inner retina (beta = −0.551; P < .0001) as statistically significant variables. The standardized beta coefficient suggests an inverse relationship for temporal perifoveal inner retinal volume and visual acuity, suggesting that visual acuity declines as the inner temporal perifoveal retina thins.
Pearson correlation coefficients were calculated to assess the relationship between patient age and retinal thickness or volume measurements. The Table summarizes the statistically significant correlations. In general, full-thickness retinal thicknesses and volumes decreased with age. Several outer retinal perifoveal thicknesses and volumes also declined with age. Overall, the strongest Pearson correlations were for inner retinal thickness and volume measurements, which also diminished with age ( Figure 6 ).
| Variable | Pearson Correlation | P Value |
|---|---|---|
| Full-thickness parafoveal inferior hemisphere thickness | −0.332 | .008 |
| Full-thickness parafoveal nasal thickness | −0.304 | .015 |
| Full-thickness parafoveal inferior thickness | −0.274 | .029 |
| Full-thickness perifoveal thickness | −0.258 | .041 |
| Full-thickness perifoveal inferior hemisphere thickness | −0.376 | .002 |
| Full-thickness perifoveal nasal thickness | −0.473 | <.001 |
| Full-thickness perifoveal inferior thickness | −0.384 | .002 |
| Full-thickness parafoveal inferior hemisphere volume | −0.268 | .034 |
| Full-thickness parafoveal nasal volume | −0.305 | .015 |
| Full-thickness parafoveal inferior volume | −0.270 | .033 |
| Full-thickness perifoveal volume | −0.347 | .005 |
| Full-thickness perifoveal superior hemisphere volume | −0.251 | .048 |
| Full-thickness perifoveal inferior hemisphere volume | −0.428 | <.001 |
| Full-thickness perifoveal nasal volume | −0.500 | <.001 |
| Full-thickness perifoveal inferior volume | −0.435 | <.001 |
| Outer retina perifoveal inferior hemisphere thickness | −0.264 | .036 |
| Outer retina perifoveal nasal thickness | −0.410 | .001 |
| Outer retina perifoveal inferior thickness | −0.292 | .020 |
| Outer retina perifoveal inferior hemisphere volume | −0.264 | .036 |
| Outer retina perifoveal nasal volume | −0.411 | .001 |
| Outer retina perifoveal inferior volume | −0.290 | .021 |
| Inner retina parafoveal thickness | −0.459 | <.001 |
| Inner retina parafoveal superior hemisphere thickness | −0.405 | .001 |
| Inner retina parafoveal inferior hemisphere thickness | −0.483 | <.001 |
| Inner retina parafoveal temporal thickness | −0.471 | <.001 |
| Inner retina parafoveal superior thickness | −0.291 | .020 |
| Inner retina parafoveal nasal thickness | −0.471 | <.001 |
| Inner retina parafoveal inferior thickness | −0.452 | <.001 |
| Inner retina perifoveal thickness | −0.555 | <.001 |
| Inner retina perifoveal superior hemisphere thickness | −0.489 | <.001 |
| Inner retina perifoveal inferior hemisphere thickness | −0.564 | <.001 |
| Inner retina perifoveal temporal thickness | −0.536 | <.001 |
| Inner retina perifoveal superior thickness | −0.421 | .001 |
| Inner retina perifoveal nasal thickness | −0.447 | <.001 |
| Inner retina perifoveal inferior thickness | −0.527 | <.001 |
| Inner retina parafoveal volume | −0.460 | <.001 |
| Inner retina parafoveal superior hemisphere volume | −0.404 | .001 |
| Inner retina parafoveal inferior hemisphere volume | −0.481 | <.001 |
| Inner retina parafoveal temporal volume | −0.471 | <.001 |
| Inner retina parafoveal superior volume | −0.293 | .020 |
| Inner retina parafoveal nasal volume | −0.470 | <.001 |
| Inner retina parafoveal inferior volume | −0.450 | <.001 |
| Inner retina perifoveal volume | −0.554 | <.001 |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


