12 OCULAR TRAUMA
Blunt Trauma
Andrew Mick
 THE DISEASE
THE DISEASE
Pathophysiology
Trauma to the eye from a blunt object results in a concussive shock wave throughout the orbit and globe. The mechanical forces exerted on the globe have the potential to produce damage in all orbital structures.
Common causes include fist fights, airbags, golf balls, baseballs, racquet balls, and bungee cords. Rocks and snowballs are common causes of blunt trauma in children. Greater damage often occurs with smaller objects because the force is more concentrated into the orbital structures. Smaller objects are also able to fit within the protective orbital rim. Larger objects dissipate a large amount of their force into the bones of the face and orbital rim.
The Patient
Significant History
- Recent eye trauma
Clinical Symptoms
1. Pain
- Sharp and sectoral: Corneal abrasion, laceration of the conjunctiva or lid
- Dull aching: Orbital blowout, retrobulbar hemorrhage
- Photophobia: Traumatic iritis
2. Watery discharge
3. Double vision
- Entrapment of extraocular muscles (EOMs)
- Damage to controlling cranial nerve
- Retrobulbar hemorrhage
4. Decreased vision
- Damage to cornea, lens, retina, or optic nerve
- Intraocular bleeding: Hyphema or vitreous hemorrhage
Clinical Signs
1. Reduced visual acuity
2. EOM abnormalities
- EOM restriction: muscle entrapment secondary to an orbital fracture, damage to controlling cranial nerve, retrobulbar hemorrhage
3. Lid involvement
- Ecchymosis and swelling
- Lid lacerations: Injury from a sharp or penetrating object
- Crepitus or subcutaneous emphysema: Introduction of air into periocular tissues suggesting orbital blowout fracture
4. Globe involvement
- Globe rupture: More likely with trauma from smaller, sharp, high speed objects (Fig. 12-1)
- Conjunctival laceration
- Subconjunctival hemorrhage
5. Intraocular pressure (IOP) abnormality
- Low IOP: Ruptured globe, retinal detachment, or iritis
- High IOP: Intraocular hemorrhage, inflammation, lens subluxation into the anterior chamber, retinal detachment, or angle recession
6. Corneal involvement
- Abrasion: Superficial epithelial layer involved
- Laceration: Deeper structures involved without full-thickness wound
- Perforation: Full-thickness wound
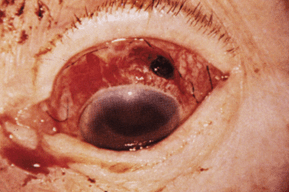
Figure 12-1. Globe rupture.
7. Anterior chamber involvement
- Anterior chamber cell/flare
- Hyphema
- Abnormal anatomical position of tissues
8. Grading anterior uveitis
- Subclinical: No cells or flare
- Trace: Any cells or barely noticeable flare
- Grade 1: 5 to 10 cells per high-power field
- Grade 2: 11 to 20 cells per high-power field
- Grade 3: 21 to 50 cells per high-power field
- Grade 4: Cells too numerous to count, fibrinous/plasmoid aqueous
9. Hyphema (Fig. 12-2)
- Microhyphema
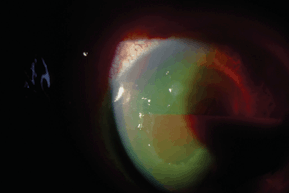
Figure 12-2. Hyphema.
- No layering of red blood cells in the inferior angle
- Visible red blood cells suspended throughout the anterior chamber
- No layering of red blood cells in the inferior angle
- General hyphema
- Grade I: less than 1/3 of the anterior chamber
- Grade II: 1/3 to 1/2 of the anterior chamber
- Grade III: greater than 1/2, but less than total
- Grade IV: Total (100%) hyphema (a.k.a. 8-ball hyphema)
- Grade I: less than 1/3 of the anterior chamber
10. Iris involvement
- Iridodialysis: Iris disinsertion at scleral spur (Fig. 12-3)
- Sphincter or dilator muscle tears
- Transillumination defects: Possible site of intraorbital foreign body entrance
11. Lens involvement
- Subluxation
- Anterior segment displacement
- Opacification: Secondary to blunt trauma or penetrating foreign body
12. Vitreous involvement
- Posterior vitreous detachment
- Vitreous hemorrhage: Increases likelihood of associated retinal detachment/tear
13. Retinal involvement
- Retinal breaks or detachments: Increased risk with preexisting retinal breaks
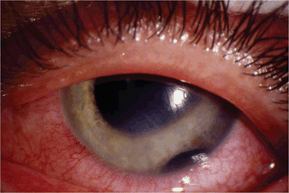
Figure 12-3. Iridodialysis.
- Retinal dialysis: Disinsertion of the sensory retina at the ora serrata
- Traumatic macular hole: Tangential traction at the fovea caused by trauma induced initial equatorial expansion and forward displacement of the posterior pole followed by a rebound to its normal anatomical position
- Commotio retinae: Retinal whitening clinically appearing like edema, representing fragmentation of the photoreceptor outer segments (Fig. 12-4)
14. Choroidal involvement
- Choroidal rupture: Breaks of the inner choroid and overlying RPE, often curvilinear and concentric to optic nerve, may be associated with subretinal hemorrhage or serous detachment of the retina, short- and long-term risk of choroidal neovascular membranes (Fig. 12-5)
- Chorioretinitis sclopetaria: Choroidal rupture caused by shock waves from high velocity, grazing object passing adjacent to the globe
15. Optic nerve involvement
- Traumatic optic neuropathy: Most common injury site is at orbital apex, afferent pupillary deficit (APD), sluggish or absent pupillary responses, decreased vision, color vision abnormality, visual field defects, acutely may be normal but progressive atrophy develops over several weeks, damage can be direct or indirect
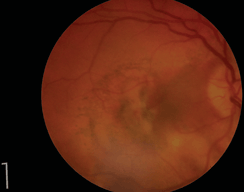
Figure 12-4. Commotio retinae.
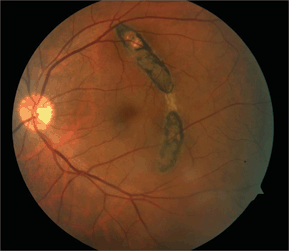
Figure 12-5. Choroidal rupture.
- Direct optic nerve damage: Penetrating objects or bone fractures.
- Indirect optic nerve damage: Mechanical shearing, nerve sheath hemorrhage, orbital/retrobulbar hemorrhage, orbital emphysema, ischemia from damaged blood vessels, secondary inflammation (Fig. 12-6)
- Direct optic nerve damage: Penetrating objects or bone fractures.
- Optic nerve avulsion: Globe rotated and pulled forward resulting in tearing of the lamina cribrosa and nerve fibers at the disc margin, acute partial ring of hemorrhage surrounding the optic nerve, late fibrous proliferation fills area surrounding avulsion site
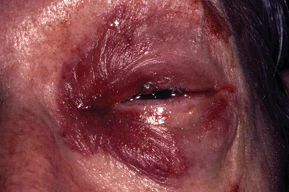
Figure 12-6. Retrobulbar hemorrhage.
Blunt trauma is more common in men than women and has a higher prevalence in the younger age groups. Work environments and recreational activities that put eyes at risk of trauma also increase the prevalence of injuries.
Ancillary Tests
- Binocular indirect ophthalmoscopy: Evaluate the vitreous, retina, choroid, and optic nerve, scleral indentation contraindicated when hyphema and globe rupture are present
- Tonometry: Elevated IOP (intraocular hemorrhage, inflammation, lens subluxation into the anterior chamber, retinal detachment), decreases IOP (globe rupture or retinal detachment)
- Gonioscopy: Rule out angle recession or anterior synechiae formation, contraindicated when hyphema and globe rupture are present
- Sickle cell screening: Black patients with hyphema
- Seidel’s test: Suspicion of penetrating injury to the globe
- Forced duction tests: Differentiate between mechanical and paretic EOM deficits
- Infraorbital nerve testing: Localized anesthesia signals possible orbital fracture
- Computed tomography (CT): Detecting subtle orbital fractures or ruptures of the globe, metallic foreign bodies (Fig. 12-7)
- Magnetic resonance imaging (MRI): Details soft-tissue damage, must rule out the presence of metallic foreign bodies prior to MRI scanning
- Orbital ultrasonography (B-scan): Detecting a ruptured globe or retinal detachment through hazy media or cataract
- Fluorescein angiography: Rule out choroidal rupture
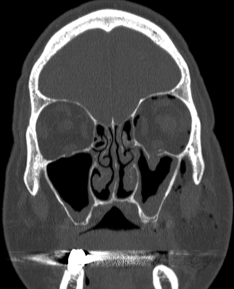
Figure 12-7. Left inferior orbital floor fracture.
The Treatment
1. Corneal abrasion
- Antibiotic coverage
- Noncontact lens wearer: Polymyxin B/trimethoprim solution four times a day
- Contact lens wearer needs antipseudomonal coverage: besifloxacin 0.6% (Besivance: Bausch and Lomb, Madison, NJ): moxifloxacin 0.5% (Vigamox: Alcon, Ft Worth, TX), gatifloxacin 0.3% (Zymar: Allergan, Irvine, CA), ofloxacin, ciprofloxacin, tobramycin four times a day
- Noncontact lens wearer: Polymyxin B/trimethoprim solution four times a day
- Cycloplegia
- Cyclopentolate 1% three times a day
- Scopolamine 0.25% two times a day
- Cyclopentolate 1% three times a day
- Bandage contact lens
- Débridement of loose epithelium
2. Orbital fracture
- Broad-spectrum oral antibiotic therapy
- Amoxicillin/clavulanate 500/125 mg two times a day
- Cephalexin 250 to 500 mg four times a day
- Azithromycin 250 mg twice daily for 1 day and then once daily for 4 days
- Amoxicillin/clavulanate 500/125 mg two times a day
- Cool compresses/ice packs
- Appropriate analgesics
- Mild pain: Acetaminophen 500 mg every 4 to 6 hours, ibuprofen 400 to 600 mg every 4 to 6 hours, naproxen 250 to 500 mg twice daily
- Moderate pain: Acetaminophen with codeine (30 mg codeine) every 6 hours
- Severe pain: Acetaminophen (500 mg) with hydrocodone (5 mg) every 4 to 6 hours, ibuprofen (200 mg) with hydrocodone (7.5 mg) every 4 to 6 hours, acetaminophen (325 mg) with oxycodone (10 mg) every 4 to 6 hours
- Mild pain: Acetaminophen 500 mg every 4 to 6 hours, ibuprofen 400 to 600 mg every 4 to 6 hours, naproxen 250 to 500 mg twice daily
- Refer for surgical evaluation immediately
- Oculocardiac reflex present: Bradycardia, heart block, nausea, vomiting
- Orbital floor fracture with muscle/soft tissue entrapment: High risk of secondary ischemia, especially in children
- Early/severe enophthalmos present or severe facial asymmetry
- Cerebral spinal fluid rhinorrhea
- Large fractures: greater than 1/2 floor or any involving the roof or orbital apex
- Oculocardiac reflex present: Bradycardia, heart block, nausea, vomiting
- Refer for surgical evaluation within 1 month
- Forced duction testing is positive, or the patient experiences persistent diplopia
- There is at greater than 3 mm of persistent enophthalmos present
- Forced duction testing is positive, or the patient experiences persistent diplopia
- Observe
- Diplopia only in extreme gazes
- Minimal cosmetic change
- Diplopia only in extreme gazes
3. Hyphema
- General and microhyphema management guidelines
- Bed rest with only bathroom privileges
- Elevate head to at least 30 degrees at all times, asleep and awake
- No nonsteroidal anti-inflammatory drugs (NSAIDs) or any aspirin-containing medications
- Protective eye shield with holes to allow for detection of decreased acuity
- Topical steroids: Prednisolone acetate 1% four times a day
- Cycloplegic: Scopolamine 0.25% twice daily or atropine 1% daily
- Lab tests for sickle cell in black patients
- Monitor and treat elevated IOP over 24 mm Hg: IOP may be elevated by red blood cell in the trabecular meshwork, inflammatory debris, peripheral synechiae, or pupillary block from central clot. Elevated IOP can result in damage to the optic nerve and blood staining of the cornea. β-Blockers should be the first line of therapy in the absence of contraindications. Prostaglandin analogs should not be used to avoid adding to the inflammatory response. Miotics increase vascular permeability and increase the risk of posterior synechiae. Carbonic anhydrase inhibitors are contraindicated in sickle cell disease due to acidification of anterior chamber
- Daily ocular evaluation: Patient should return immediately if there is a decrease in vision or change in symptoms
- Bed rest with only bathroom privileges
- Severe hyphema or a noncompliant patient may require hospitalization: Activity can be more closely monitored, antifibrinolytic agents (aminocaproic acid 50 mg/kg every 4 hours) may be administered. Patients in whom hospitalization should be considered include the following:
- Patients with large hyphema: greater than 1/3 anterior chamber
- Uncooperative patients
- Children: Amblyopia risk with persistent hyphema
- Patients who have rebleeding
- Patient utilizing anticoagulant therapy
- Sickle cell anemia patients
- Patients with medically uncontrolled IOP
- Patients with large hyphema: greater than 1/3 anterior chamber
- Reasons to refer hyphema patient for consideration of surgical removal of blood
- IOP extremely elevated and not responsive to topical therapy
- Grade III or IV hyphema lasting 6 days: Risk of corneal blood staining
- Children with persistent hyphema: Amblyopia risk
- IOP extremely elevated and not responsive to topical therapy
4. Traumatic uveitis
- Treatment guidelines:
- Subclinical: Cycloplegic such as cyclopentolate 1% four times a day
- Grade 1: Cycloplegic such as homatropine 5% three times a day, topical steroids such as prednisolone acetate 1% three times a day
- Grade 2: Cycloplegic such as homatropine 5% four times a day or scopolamine 0.25% twice a day, topical steroids such as prednisolone acetate 1% four times a day
- Grades 3 and 4: Cycloplegic such as atropine 1% once daily or scopolamine 0.25% twice daily, topical steroids such as prednisolone acetate 1% four times a day, consider longer acting steroid-containing ointment nightly such as sulfacetamide/prednisolone (Vasociden: Novartis, Switzerland) gentamicin/prednisolone (Pred-G: Allergan, Irvine, CA) tobramycin/dexamethasone (Tobradex: Alcon, Ft Worth, TX)
- Presence of elevated IOP associated with iritis: β-blockers are first line of therapy without contraindications, consider α-agonists and topical carbonic anhydrase inhibitors, avoid prostaglandin analogs as they promote inflammation, no miotics as they increase vascular permeability and risk of posterior synechiae formation
- Subclinical: Cycloplegic such as cyclopentolate 1% four times a day
5. Lens subluxation
- Subluxation of the lens into the anterior chamber can cause marked increase in IOP secondary to pupil block. Prior to referral for repositioning or removal of the lens, the following should be done to decrease IOP:
- Cyloplegia with appropriate agent
- Treat elevated IOP with β-blocker, α-agonist, topical or oral carbonic anhydrase inhibitor (acetazolamide 250 four times a day, 500 mg sequel twice a day, methazolamide 25 mg twice a day), or oral hyperosmotic agent (isosorbide 1 to 3 gm/kg, not metabolized to glucose)
- Cyloplegia with appropriate agent
6. Ruptured globe
- Advise patient to not touch or squeeze eyes, position eye shield, advise the patient to not consume any food or water, immediately refer patient to ophthalmic surgeon for surgical repair
7. Commotio retinae
- There is no specific treatment for this condition
- Prognosis with uncomplicated commotio retinae is excellent, vision often returns to normal, more extensive damage to the photoreceptors manifests in RPE mottling and atrophy that may result in functional deficits
8. Retinal tears and detachments
- B-scan ultrasonography: When retina cannot be visualized because of media opacity, an APD may be an early indicator of possible detachment, referral for retinopexy or vitreal-retinal surgery as the extent of damage warrants.
9. Choroidal rupture
- There is no specific treatment for this condition
- Periodic examination for the development of a choroidal neovascular membrane at the site of RPE disruption that can occur months after the injury or years later, immediate referral to a retinal specialist if choroidal neovascular membrane detected
10. Optic nerve trauma
- There is no specific treatment for this condition
- High-dose intravenous steroids administered in the first hours after trauma or surgical decompression of the optic canal have been advocated; treatment therefore will vary with different treating physicians
Corneal Abrasion
Andrew Mick
 THE DISEASE
THE DISEASE
Pathophysiology
The cornea is composed of five distinct layers, including the epithelium, Bowman’s membrane, stroma, Descemet’s membrane, and the endothelium. A defect in the most superficial layer, the epithelium, is classified as a corneal abrasion. Any object that strikes the cornea can produce a superficial abrasion. Common causes are fingernails, tree branches, mascara brushes, and paper cuts.
The Patient
Significant History
- Trauma from vegetative matter: Increased risk of fungal infection
- Contact lens wear: Increased risk of bacterial infection, especially Pseudomonas
- Paper cuts or fingernail injuries: Increased risk of recurrent erosion after resolution
- High-speed foreign body or associated blunt trauma: Increased risk of penetrating injury
Clinical Symptoms
- Pain/foreign body sensation
- Lacrimation
- Light sensitivity
Clinical Signs
- Positive fluorescein staining of defect
- Negative Seidel’s test
- Mild anterior chamber reaction
- Swollen eyelid
The Treatment
- Cycloplegia: Cyclopentolate 1% four times a day or homatropine 5% three times a day, or scopolamine 0.25% twice daily
- Noncontact lens wearers:
- Polymyxin B/trimethoprim solution four times a day
- Polymyxin B/bacitracin ointment nightly
- Polymyxin B/trimethoprim solution four times a day
- Contact lens wearers require anti-Pseudomonas coverage:
- Besifloxacin 0.6% (Besivance: Bausch and Lomb, Madison, NJ), moxifloxacin 0.5% (Vigamox: Alcon, Ft Worth, TX), gatifloxacin 0.3% (Zymar: Allergan, Irvine, CA), ofloxacin, ciprofloxacin, tobramycin four times a day
- Ciprofloxacin, tobramycin ointment nightly
- Consider tight-fitting low-powered soft bandage contact lens: Decreases lid–cornea interaction and facilitate epithelial healing of large or extremely painful abrasions
- Consider topical NSAID to decrease pain: Ketorolac or diclofenac solution
- Appropriate analgesics for pain:
- Mild pain: Acetaminophen 500 mg every 4 to 6 hours, ibuprofen 400 to 600 mg every 4 to 6 hours, naproxen 250 to 500 mg twice a day
- Moderate pain: Acetaminophen with codeine (30 mg codeine) every 6 hours
- Severe pain: Acetaminophen (500 mg) with hydrocodone (5 mg) every 4 to 6 hours, ibuprofen (200 mg) with hydrocodone (7.5 mg) every 4 to 6 hours, acetaminophen (325 mg) with oxycodone (10 mg) every 4 to 6 hours
- Reevaluate until reepithelialized; monitor for infection or recurrent erosion
- Ciprofloxacin, tobramycin ointment nightly
Recurrent Corneal Erosion
Andrew Mick
 THE DISEASE
THE DISEASE
Pathophysiology
Damage to Bowman’s membrane, the basement membrane of the epithelium, prevents normal adherence of the epithelium. This results in a weakened area of epithelium that regularly sloughs off. Bilateral anterior corneal dystrophies (epithelial basement membrane dystrophy, Meesmann’s dystrophy, Reis-Bucklers’ dystrophy) can result in a similar clinical presentation.
Etiology
Erosions are recurrent epithelial defects that are secondary to poor adherence to the underlying basement membrane. They are commonly caused by prior abrasions of the cornea or corneal dystrophies.
The Patient
Significant History
- History of corneal trauma
- Previous episodes of similar symptoms
Clinical Symptoms
- Recurrent pain and foreign body sensation, most prominent upon awakening
- Lacrimation
- Light sensitivity
- Decreased vision
Clinical Signs
- Negative and/or positive corneal staining with fluorescein dye
- Injection of conjunctiva
- Mild anterior chamber reaction
- Presence of anterior corneal dystrophy
Demographics
Recurrent corneal erosions secondary to previous abrasions can occur at any age. The demographics of erosions secondary to different corneal dystrophies vary:
Anterior Corneal Dystrophies
1. Epithelial basement dystrophy (map dot dystrophy)
- Most cases not inherited, but may show autosomal dominant pattern
- Intricate pattern of dots and lines throughout the epithelium
- Most commonly seen in adults between the age of 40 and 70 years
2. Meesmann’s dystrophy
- Autosomal dominant inheritance
- Intraepithelial cysts especially concentrated in the interpalpebral space
- Most commonly presents in first to second decade
- Autosomal dominant inheritance
- Honeycomb appearance of central epithelium
- Usually presents in first to second decade with painful erosions
Ancillary Tests
None.
The Treatment
Initial Therapy
- Cycloplegia: Cyclopentolate 1% four times a day or homatropine 5% twice a day
- Polymyxin B/trimethoprim solution four times a day, polymyxin B/bacitracin ointment nightly
- Copious artificial tears and ophthalmic lubricants
- Consider tight-fitting bandage contact lens if erosion is large or patient is extremely symptomatic
- Follow closely until reepithelialized
After Reepithelialization
- Nonpreserved artificial tears during the day, lubricating ointment nightly
- Consider 5% NaCl ointment nightly for 4 to 6 weeks and then as needed
Failure to Reepithelialize
- Anesthetize and remove abnormal/loose epithelium on edge of erosion with sterile forceps
- Apply bandage contact lens and treat as directed in the “After Reepitheliaztion” section
- Consider oral doxycycline: 50 mg twice a day and mild topical steroid three times a day for 4 weeks: fluorometholone alcohol 0.1% and loteprednol 0.2% suspension (Alrex: Bausch and Lomb, Madison, NJ)
- Continued recurrence
- Consider oral doxycycline 50 mg twice a day and mild topical steroid three times a day for 4 weeks: fluorometholone alcohol 0.1% and loteprednol 0.2% suspension (Alrex: Bausch and Lomb, Madison, NJ)
- Consider micropuncture therapy: Multiple punctures through Bowman’s membrane with 22-guage needle after removal of abnormal epithelium with forceps, large areas of the corneal involvement preferably not in optic axis, after application apply bandage contact lens and treat as directed earlier
Other Treatment Options
- Superficial keratectomy or phototherapeutic keratectomy: When treatment zone is large or if affected area is in the optic axis
Superficial Ocular Foreign Body
Andrew Mick
 THE DISEASE
THE DISEASE
Pathophysiology
A variety of materials in the environment can easily embed themselves into the cornea or conjunctiva. Evaluation of the type of material and its precise location in the eye is necessary to determine appropriate management.
Etiology
Drilling, chopping, and sanding can produce particles that can become entrapped in superficial layers of the eye. Wind-borne particles are another source of this injury.
The Patient
Significant History
- Report of getting something in the eye or employment/environment that entails exposure to debris
Clinical Symptoms
- Foreign body sensation or pain
- Lacrimation
- Photophobia
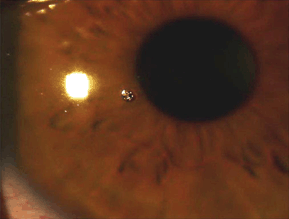
Figure 12-8. Corneal foreign body.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


