Purpose
To report a novel method for measuring the vertical tilt angle of the optic nerve (ON) head and to investigate the associated factors.
Design
Cross-sectional diagnostic study.
Methods
One hundred and twelve normal, glaucomatous, and glaucoma suspect eyes (99 patients) were enrolled in this study. Subjects underwent a full eye examination, biometry, and spectral-domain optical coherence tomography (SDOCT). The vertical tilt angle was measured on high-resolution cross-sectional SDOCT images passing through the ON head and foveal centers using the inner edges of the Bruch membrane opening as the reference plane. The correlation between the vertical tilt angle with the ovality index and the potential associated factors was estimated with univariate and multivariate linear regression analyses.
Results
The median (interquartile range, [IQR]) axial length and visual field mean deviation were 24.5 (23.8-25.3) mm and −0.9 (−2.76 to 0.26) dB. The median (IQR) tilt angle was 3.5 (1.2-11.2) degrees. There was a moderate correlation between the ovality index and tilt angle (Spearman ρ = 0.351; P < .001). In univariate analyses, axial length, spherical equivalent, and mean deviation were correlated with the tilt angle ( P = .002, P = .011, and P = .013, respectively). Axial length, mean deviation, and their interaction showed a statistically significant correlation with the tilt angle in multivariate analyses ( P = .044 for axial length, P = .039 for mean deviation, and P = .028 for their interaction).
Conclusions
We describe a new method for measuring the ON head vertical tilt angle with high-resolution SDOCT imaging. The ovality index demonstrated only a moderate correlation with the tilt angle measurements and hence is not a good proxy measure for the vertical ON head tilt angle. Axial length and visual field mean deviation are the main factors associated with the ON head vertical tilt angle. The underlying basis for the relationship of vertical tilt angle and glaucoma severity should be further explored.
Evaluation of the optic nerve (ON) head is an essential part of a thorough eye examination. The optic nerve usually follows a slightly oblique course (tilt around the vertical axis) when leaving the eye, and in some eyes—particularly myopic eyes—the vertical tilt of the ON head is significant and can be appreciated ophthalmoscopically. In cases where there is significant vertical tilt, the ON head is seen as vertically oval because of the oblique angle of observation. Although ON head tilt has been described as a congenital anomaly of the optic nerve, there is recent evidence that it may also be acquired secondary to expansion of the posterior sclera in myopic eyes and is commonly associated with significant temporal peripapillary atrophy.
The presence and the degree of the ON head vertical tilt has been traditionally estimated based on subjective clinical evaluation of the optic disc in many published studies. Simple objective methods for measuring the ON head vertical tilt angle have been developed according to optic disc shape and include ovality and tilt indices. We herein report a new method for quantitative measurement of the ON head vertical tilt angle with spectral-domain optical coherence tomography (SDOCT). We also explored factors associated with vertical ON head tilt angle in a series of normal eyes, glaucoma suspects, and eyes with glaucoma.
Methods
Study Subjects
The study subjects of this cross-seectional study were prospectively enrolled from a larger study (UCLA OCT Imaging Study). This study was approved by the Institutional Review Board at University of California Los Angeles (UCLA) and was carried out in accordance with the Declaration of Helsinki. Patients with a definite or suspected diagnosis of primary open-angle glaucoma (POAG) were prospectively identified and invited to be enrolled in the study if they met the following criteria: age ≥30 years, open angles, visual acuity ≥20/80, visual field mean deviation ≥−15 dB, refractive error ≤8.0 diopters (D), and astigmatism ≤3 D. Eyes with evidence of retinal or neurologic diseases or prior glaucoma surgery were excluded. A group of normal subjects recruited through advertising throughout UCLA or spouses of patients visiting the glaucoma clinic at the Jules Stein Eye Institute were also enrolled. The normal subjects were required to have no history of significant eye disease and a normal eye examination, including normal visual acuity (20/25 or better) and normal optic nerve head and visual fields.
Eye Examinations
All subjects underwent a comprehensive eye examination on the day of the imaging, which included the following: visual acuity, automated refraction, intraocular pressure (IOP) measurement, gonioscopy, slit-lamp examination, dilated fundus examination, and achromatic (standard achromatic perimetry, SAP) or short-wavelength automated perimetry (SWAP) fields. The axial length and keratometry were measured with the IOLMaster (Carl Zeiss Meditec, Dublin, California, USA). Central corneal thickness measurements were abstracted from patient charts, if available, or measured with a DGH 55 Pachmate (DGH Technology, Inc, Exton, Pennsylvania, USA). Optic disc photographs were reviewed by 2 experienced clinicians (K.N.M. and J.A.G.) and classified as glaucomatous, indeterminate, or normal. Evidence of glaucoma was based on the appearance of the neuroretinal rim, cup-to-disc asymmetry, retinal nerve fiber layer loss, and presence of disc hemorrhage, if any, but no formal criteria were used by the reviewers. In case of disagreement on classification of individual disc photographs, the final decision was adjudicated by a third reviewer (J.C.).
Visual Field Assessment
The Swedish Interactive Thresholding Algorithm (SITA) standard testing strategy was used for both SAP and SWAP tests. Reliable visual fields were defined as those with a fixation loss or false-negative rate ≤33% and false-positive rate ≤20%. The visual fields were reviewed to exclude lid or lens artifacts. An abnormal SAP or SWAP visual field was defined as presence of a Glaucoma Hemifield Test (GHT) outside normal limits and presence of ≥4 abnormal test locations on the pattern deviation plot with p <5%, both confirmed at least once. These criteria have been shown to be highly specific and sensitive to early glaucomatous visual field loss. Perimetric glaucoma was defined as evidence of reproducible visual field loss on SAP or SWAP regardless of IOP or disc appearance. Eyes with evidence of glaucomatous optic neuropathy based on review of stereoscopic disc photographs with normal or borderline SAP or SWAP visual fields (ie, visual fields that did not meet the criteria mentioned above for abnormality) were considered to be glaucoma suspects.
Imaging and Image Processing Procedures
The following imaging procedures were performed after dilation:
- •
Stereoscopic disc photographs: 35-mm ON head slides were scanned to high-resolution (2400 dpi) digital images with a Nikon slide scanner (Nikon LS-50 ED; Nikon Inc, Shinjuku, Tokyo, Japan).
- •
The HD 5-line raster imaging mode of the Cirrus HD-OCT (Carl Zeiss Meditec, Inc) was used to obtain a high-resolution cross-sectional image of the retina along a 9-mm line passing through the central part of the disc and the fovea. The line extended from the nasal side of the disc to well beyond the fovea. The single-line mode of the HD 5-line raster scan performs 4096 consecutive axial scans along the same predetermined line and the measurements are repeated 4 times and averaged to provide the final image.
Two experienced ophthalmic photographers with extensive experience in imaging with SDOCT performed all the imaging. If the OCT image quality was poor, as judged by the photographer performing the examination, imaging was repeated to obtain a better-quality scan. Inclusion criteria for OCT images were: (1) good linear raster OCT quality (signal strength >6); (2) good-quality en face OCT images so that adequate image registration could be done; (3) no retinal or optic nerve pathology or anomaly (other than possible vertical disc tilt); and (4) no motion artifacts on en face or linear raster OCT image. All the images were reviewed afterwards by one of the investigators (H.H.) and images with a signal strength of <6, obvious artifacts, or significant retinal pathology were excluded.
Tilt Index and Tilt Angle Measurements
The digitized disc photographs were exported to Microsoft Office PowerPoint software (Microsoft Corporation, Redmond, Washington, USA) and an ellipse of best fit was defined for each disc while viewing the stereoscopic photographs. The vertical and horizontal diameters of the fitted ellipse were recorded in pixels. The “ ovality index ” was calculated by dividing the vertical disc diameter (ie, the disc diameter within 20 degrees of the vertical midline) by the horizontal disc diameter.
The tilt angle was measured using cross-sectional HD 5-line raster image of Cirrus OCT as described here:
- 1)
Color fundus photographs were manually registered to en face SDOCT images with Adobe Illustrator CS4 software (Adobe Systems Incorporated, San Jose, California, USA). Transparency of the color fundus photographs was set to 50% to allow visualization of the underlying en face image. Retinal vessels were used as guidelines to make a precise overlay image.
- 2)
The corresponding cross-sectional linear SDOCT scan was then aligned under the overlay image with the blue-green scan line on the en face image (green line on Figure 1 A). In this triple overlay image corresponding points on the color fundus photograph or en face OCT image are aligned with those on the linear scan.
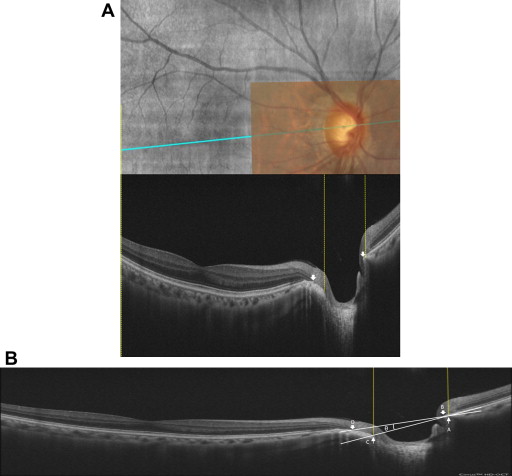
Figure 1
Methods used to estimate the vertical optic nerve head tilt angle with spectral-domain optical coherence tomography (SDOCT). (A) The triple overlay image used for marking the landmarks on the linear SDOCT scan consisted of a color fundus photograph, the en face SDOCT image, and the corresponding cross-sectional linear SDOCT image. By aligning the 3 images, we were able to mark the main landmarks on the linear SDOCT images. The yellow lines mark the clinical boundary of the disc and were continued downward to locate the respective points on the SDOCT image. The arrows show the inner edges of the Bruch membrane on each side of the optic nerve head. (B) The line BD, connecting the inner edges of the Bruch membrane on each side of the optic nerve head, was defined as the r eference plane . The line AC connecting the 2 points marking the clinical disc margin on the SDOCT image (points A and C) was considered as the optic nerve head plane . The vertical tilt angle was defined as the angle between the reference and the optic nerve head planes (θ).
- 3)
The triple registered image was then exported to PowerPoint and while viewing stereo fundus photographs, the locations where the scan line crossed the temporal and nasal disc borders were identified and vertical lines were dropped down to determine the anatomic location corresponding to the temporal and nasal clinical disc borders on the cross-sectional linear SDOCT scan ( Figure 1 A and B).
- 4)
The HD5 images were imported into ImageJ software (version 1.43u, National Institutes of Health, Bethesda, Maryland, USA; http//rsb.info.nih.gov//ij ) and rescaled.
- 5)
A line (line BD) connecting the inner tips of the Bruch membrane on each side of the ON head on the cross-sectional SDOCT image (points B and D, Figure 1 B) was drawn and set as the reference plane.
- 6)
A line (line AC) connecting the 2 points marking the clinical disc margin along the SDOCT scan was considered the ON head plane ( Figure 1 B). The disc border points (points A and C in Figure 1 B) were where the yellow lines intersect the inner surface of the disc ( Figure 1 B).
- 7)
The vertical tilt angle (angle θ) was defined as the angle between the reference plane (line BD) and ON head plane (line AC). Angle measurements were performed with the “angle tool” in the ImageJ software. Based on our method, a positive tilt angle represents vertical tilt as it is understood clinically, that is, the temporal edge of the disc is located more posterior than the nasal edge.
Statistical Analyses
The distribution of continuous parameters was verified with normal quartile plots and the Wilk-Shapiro test. Correlations between tilt angle and potential associated factors such as age, ovality index, axial length, mean deviation (MD), spherical equivalent, and IOP were explored using bivariate scatterplots and univariate analyses. Multivariate linear regression analyses were performed to determine factors affecting the tilt angle in the study sample, taking into account the correlation of the 2 eyes from patients who had both eyes included. Statistical analyses were performed with Stata software (version 11.2, Stata Corp, College Station, Texas, USA). P values less than .05 were considered to be statistically significant.
Results
One hundred and twelve eyes (from 99 patients) were included in this study. Table 1 shows the demographic and baseline characteristics of the enrolled patients. There were 39 normal eyes, 40 glaucoma suspects, and 33 glaucoma eyes. The median (interquartile range [IQR]) axial length and spherical equivalent were 24.5 (23.8-25.3) mm and −0.25 (−2.35 to +0.50) D, respectively.
| Variables | |
|---|---|
| Number of eyes (patients) | 112 (99) |
| Laterality (right/left) | 92/20 |
| Age (mean ± SD, y) | 64.2 ± 9.3 |
| Sex (female/male) | 65/34 |
| Ethnicity | |
| White, n (%) | 69 (69.7%) |
| Asian | 13 (13.1%) |
| African American | 9 (9.1%) |
| Hispanic | 6 (6.1%) |
| Other | 2 (2.0%) |
| Diagnosis (eyes), n (%) | |
| Normal | 39 (34.8%) |
| Glaucoma suspect | 40 (35.7%) |
| Glaucoma | 33 (29.5%) |
| Phakic/pseudophakic (eyes) | 89/23 |
| Visual acuity (median and IQR, logMAR) | 0.10 (0-0.10) |
| Spherical equivalent (median and IQR, diopters) | −0.25 (−2.4 to +0.5) |
| Axial length (median and IQR, mm) | 24.5 (23.8-25.3) |
| Central corneal thickness, (mean ± SD, μm) | 557 ± 41 |
| Keratometry reading (median and IQR, diopters) | 43.5 (42.5-45.0) |
| Mean deviation (median and IQR, dB) | −0.9 (−2.76 to 0.26) |
| Pattern standard deviation (median and IQR, dB) | 2.0 (1.6-3.1) |
| Intraocular pressure on the examination day (mean ± SD, mm Hg) | 14.2 ± 3.3 |
| Tilt angle (median and IQR, degrees) | 3.5 (1.2-11.2) |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


