11 LACRIMAL DISORDERS
Dacryoadenitis
Andrew Mick
ICD-9: 375.00
 THE DISEASE
THE DISEASE
Pathophysiology
Dacryoadenitis is a disease characterized by inflammation and enlargement of the lacrimal gland and surrounding tissues. Depending on the clinical characteristics and etiology, it is classified as acute, chronic, or granulomatous.
Etiology
Underlying causes of dacryoadenitis include infectious diseases, inflammatory disorders, malignancies, and benign enlargements.
Acute Dacryoadenitis
Andrew Mick
ICD-9: 375.01
 THE DISEASE
THE DISEASE
The Patient
Clinical Symptoms
- Sudden onset of pain in the superior temporal orbit
- Upper temporal eyelid is swollen, red, and tender to touch (Fig. 11-1)
- Secondary conjunctival injection and symptoms of eye irritation and tearing
- Double vision in attempted superior gaze in severe cases
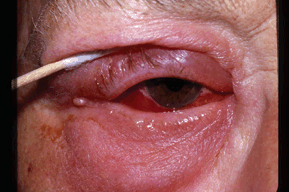
Figure 11-1. Dacryoadenitis.
Clinical Signs
- Unilateral more commonly than bilateral
- Lacrimal gland enlarged and inflamed
- Palpebral, orbital, or both lobes of the lacrimal gland may be involved
- Chemosis of surrounding conjunctiva with an occasional follicular response
- “S-shaped ptosis” due to relative involvement of upper temporal eyelid
- Mucopurulent discharge may be present in bacterial etiologies
- Tender palpable ipsilateral preauricular nodes more common with viral etiologies
- Proptosis, downward displacement of the globe, or mild extraocular muscle (EOM) disruption in severe cases
Demographics
Acute dacryoadenitis is a rare disorder usually of infectious etiology. It is most common in children and young adults, but individuals of all ages can be affected. Route of infection can be blood borne, transconjunctival, transneuronal, or through direct inoculation from trauma. Common causative agents are viruses including mumps, Epstein-Barr (mononucleosis), herpes simplex, herpes zoster, and rarely human immunodeficiency virus (HIV). Bacterial dacryoadenitis is less common and often accompanies traumatic inoculation. Bacterial etiologies include Staphylococcus sp., Streptococcus sp., Haemophilus influenzae, and Neisseria gonorrhoeae. Systemic inflammatory disorders such as sarcoidosis, Wegener’s granulomatosis, and Crohn’s disease usually manifest as chronic or bilateral dacryoadentis but must be ruled out. Rarely neoplastic etiologies including leukemia and lymphoma present as acute dacryoadenitis.
Significant History
- Recent and rapid onset of symptoms
- Occasional fever and leukocytosis
Laboratory Tests
- Complete blood count (CBC) with differential: Leukemia, lymphoma
- Culture any discharge on blood (most bacteria), chocolate (Haemophilus sp., Neisseria gonnorrhoeae), and thioglycollate agar (aerobic and anaerobic bacteria)
- Computed tomography (CT), magnetic resonance imaging (MRI), or orbital ultrasound: Delineates extent of tissue involvement, especially indicated with proptosis, downward displacement of the globe, limited EOM motility, or decreased vision
- Blood titers for appropriate suspected viral etiologies: Mumps, Epstein-Barr, HIV
- Lacrimal gland biopsy: Atypical presentations or lack of appropriate treatment response
The Treatment
Broad-spectrum antibiotics should be initiated until cultures, titers, and laboratories can better direct therapy. Appropriate choices would include
- Amoxicillin/clavulanate 500/125 mg twice daily
- Cephalexin 250 to 500 mg four times daily
- Penicillin/cephalosporin sensitive: Azithromycin: 500 mg daily for 3 days or 250 mg twice a day for 1 day, then once daily for 4 days
- Severe presentations or pediatric cases: Referral for possible hospitalization with intravenous (IV) drug therapy
Viral Etiologies
- Cool compresses
- Topical lubricants
- Appropriate analgesic as needed
- Suspected herpetic: Acyclovir 400 mg five times a day (simplex) or 800 mg five times a day (zoster), Valacyclovir 1,000 mg three times a day, Famciclovir 500 mg three times a day
Chronic/Granulomatous Dacryoadenitis
Andrew Mick
ICD-9: 375.02
 THE DISEASE
THE DISEASE
The Patient
Clinical Symptoms
- Chronic or recurrent swelling and redness of the upper lid
- Bilateral cases more common than with acute dacryoadenitis
- Occasional pain and double vision
Clinical Signs
- Localized mass in the lateral upper eyelid area
- Lacrimal gland enlarged and inflamed
- Proptosis, downward displacement of the globe, or EOM disruption in severe cases
Chronic/granulomatous dacryoadenitits has a variety of etiologies: Inflammatory (sarcoidosis, Wegener’s granulomatosis, Crohn’s disease), infectious (tuberculosis, mumps, HIV, syphilis), and neoplastic (leukemia, lymphoma)
Significant History
- Symptoms/signs of systemic infectious, inflammatory, or neoplastic disease
Laboratory Tests
- Suspected leukemia/lymphoma: CBC with differential
- Suspected sarcoidosis: Chest x-ray, serum angiotensin-converting enzyme (ACE)
- Suspected Wegener’s granulomatosis: Sinus/chest x-ray, antineutrophil cytoplasmic antibody (ANCA) test, erythrocyte sedimentation rate (ESR), C-reactive protein (CRP)
- Suspected Crohn’s disease: History of characteristic symptoms (weight loss, chronic diarrhea, abdominal pain), hematocrit/hemoglobin (gastrointestinal bleeding), ESR, x-ray with barium, abdominal CT
- Suspected tuberculosis: Purified protein derivative with anergy panel
- Suspected syphilis: Rapid plasma reagin or Venereal Disease Research Laboratory and fluorescent treponemal antibody absorption
- Suspected HIV: Serology
- CT, MRI, or orbital ultrasound: Delineates extent of tissue involvement, especially indicated with proptosis, downward displacement of the globe, limited EOM motility, or decreased vision.
- Lacrimal gland biopsy
The Treatment
- Treatment will depend on the underlying cause of the chronic dacryoadenitis and will involve referral to appropriate subspecialist for evaluation.
Dacryocystitis
Andrew Mick
ICD-9: 375.30
 THE DISEASE
THE DISEASE
Pathophysiology
The disorder is characterized by acute or chronic infection or inflammation of the lacrimal sac. Complete or partial obstruction of the nasolacrimal duct is often the precipitating event prior to infection. Obstruction can result from developmental anomalies, nasal/sinus disease, trauma, neoplasm, dacryolith formation (lacrimal calculi), or systemic inflammatory disease.
Etiology
Acute (ICD-9: 375.32)
- Lacrimal stenosis that results in secondary acute and severe infection
- Commonly cultured bacteria are Gram positive (Staphylococcus aureus, Staphylococcus epidermidis, Streptococcus pneumoniae) and Gram negative (Pseudomonas aeruginosa, Escherichia coli)
- Rarely anaerobic bacteria (Actinomyces israelii, Propionibacterium acnes)
- Rarely fungi (Aspergillus sp., Candida sp.)
Chronic (ICD-9: 375.42)
- Partial or complete blockage of the nasolacrimal system that results in secondary chronic infection
- Commonly cultured pathogens include Gram-positive bacteria (Staphylococcus sp., Streptococcus sp.), coagulase-negative staphylococci, Gram-negative bacteria (P. aeruginosa, E. coli), and fungi (Aspergillus sp., Candida sp.)
The Patient
Clinical Symptoms
Acute
- Pain, redness, and swelling around the lacrimal sac
- Tearing and discharge
- Occasional fever
- Tearing may be the only symptom in many cases
- Occasional swelling around the lacrimal sac
- Discomfort with local digital pressure
Clinical Signs
Acute
- Edema and hyperemia around the lacrimal sac
- Swelling concentrated under the medial canthal ligament
- Mucopurulent discharge expressed from the puncta
- Localized abscess with possible breakthrough to the skin surface (Fig. 11-2)
- Occasional preauricular and submandibular swollen lymph nodes
Chronic
- Epiphora
- Local swelling around lacrimal sac
- Mucopurulent material expressed from puncta with digital pressure
Demographics
Acute dacryocystitis occurs in all age groups with highest incidence in middle-aged adults. Women are afflicted more commonly than men and whites more commonly than other races. Chronic dacryocystitis can occur in infancy with congenital nasolacrimal obstruction. More commonly, it presents in elderly patients often due to involutional stenosis or scarring of the nasolacrimal drainage system.
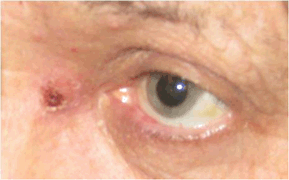
Figure 11-2. Dacryocystitis.
Significant History
- Tearing
- Discharge
- Chronic conjunctivitis
- Chronic sinusitis or current upper respiratory tract infection
Laboratory Tests
- Culture-expressed discharge on blood (all bacteria), chocolate (children: Haemophilus sp.), thioglycollate (aerobic and anaerobic), Sabouraud’s (fungal) agar
- CT scan of orbit and sinuses to rule out widespread pathology or neoplasm: When no immediate improvement occurs with appropriate therapy
The Treatment
Broad-spectrum antibiotics that have coverage for the common bacterial causative agents should be initiated until cultures can better direct therapy. Appropriate choices would include
- Amoxicillin/clavulanate 500/125 mg twice a day
- Cephalexin 250 to 500 mg four times a day
- If penicillin/cephalosporin sensitive: Azithromycin 500 mg daily for 3 days or 250 mg twice a day for 1 day, then once daily for 4 days
- Severe presentations or pediatric cases: Referral for possible hospitalization with IV drug therapy
- Warm compresses
- Analgesic therapy is important because there is often significant pain. Appropriate therapy includes:
1. Mild pain: Acetaminophen 500 mg every 4 to 6 hours, Ibuprofen 400 to 600 mg every 4 to 6 hours, Naproxen 250 to 500 mg two times a day
2. Moderate pain: Acetaminophen with codeine (30 mg codeine) every 4 to 6 hours
- Consider incision for nonresolving dacryocystitis with abscess
- Consider external or endonasal endoscopic dacryocystorhinostomy (DCR) for nonresolving dacryocystitis
- Febrile or pediatric cases with systemic disease should be referred for possible hospitalization with IV drug therapy
Canaliculitis
Andrew Mick
ICD-9: 375.31—ACUTE CANALICULITIS, LACRIMAL
ICD-9: 375.41—CHRONIC CANALICULITIS
 THE DISEASE
THE DISEASE
Pathophysiology
The disorder is characterized by infection or inflammation of the canaliculi.
Etiology
Infectious agents include bacteria (A. israelii, Propionibacterium propionicum), fungi (Candida sp., Aspergillus sp.), and viruses (Herpes simplex). Canaliculitis is rarely associated with intracanalicular punctal plug occlusion.
The Patient
Clinical Symptoms
- Irritation, redness, and swelling over medial portion of eyelids
- Tearing and discharge
Clinical Signs
- Mucopurulent discharge or concretions expressed from punctum
- Concretions felt while probing canaliculus
- Conjunctivitis more severe nasally
- Erythematous area around punctal openings
- Periocular skin vesicles (herpes simplex)
Demographics
Canaliculitis can affect people of all ages but is more common in elderly populations.
Significant History
- Chronic/recurrent conjunctivitis
- Epiphora
- History of herpetic eye disease
Laboratory Tests
- Culture any discharge from punctum on blood (all bacteria), chocolate (children: Haemophilus sp.), thioglycollate (aerobic and anaerobic bacteria), and Sabouraud’s (fungi) agar
The Treatment
- Cultures positive for bacteria: Polymyxin B/trimethoprim solution four times a day or as directed by cultures
- Cultures positive for fungus: Natamycin 5% suspension four times a day
- Suspected herpetic infection: Trifluridine 1% solution four times a day
- Removal of debris in canaliculus with irrigation
- Canaliculotomy or snip punctoplasty may be indicated in nonresponsive canaliculitis
Epiphora
Andrew Mick
ICD-9: 375.20
 THE DISEASE
THE DISEASE
Pathophysiology
The presentation of excessive tearing can be because of lacrimal hypersecretion or failure of the lacrimal system to adequately drain the tears. The four primary mechanisms are as follows:
- Dry eye or other secondary causes of reflex hypersecretion of tears
- Blockage within the lacrimal drainage apparatus or punctal malposition
- Secondary hypersecretion of the lacrimal gland due to mechanical effects
- Primary hypersecretion of the lacrimal gland
Etiology
- Dry eye: Dryness produces ocular irritation that results in subsequent hypersecretion of tears
- Secondary hypersecretion: Environmental irritants (smog, dust, or pollen) and mechanical irritants (trichiasis, entropion, or ectropion) can also produce irritation and induce hypersecretion
- Primary hypersecretion: Many etiologies can produce direct stimulation of the lacrimal gland by infection/inflammation (see “Dacryoadenitis”): Viral infections (mumps, Epstein-Barr, herpes zoster), bacterial infections (Straphylococcus sp., Streptococcus sp., N. gonorrhoeae) inflammatory conditions (sarcoidosis, thyroid ophthalmopathy, Wegener’s granulomatosis, Sjögren’s syndrome)
- Use of topical or systemic parasympathomimetic agents
- Tumors of the lacrimal gland
Blockage of the Lacrimal Drainage System
Blockage of lacrimal drainage can be congenital or acquired and occur proximally or distally within the system.
Congenital Structural Blockage
ICD-9: 375.55 or 743.65
The most common congenital causes of nasolacrimal obstruction include the following:
- Failure of the distal end of the duct to completely canalize during development
- Lack/malformation/membranes of one or more puncta
- Lack/malformation/membranes of the canaliculi
- Congenital tumors of the lacrimal sac:
1. Mucocele
2. Hemangioma
3. Dermoid
- Membrane/cyst in the nasolacrimal duct
Acquired Structural Blockage
ICD-9: 375.56
Acquired nasolacrimal duct obstruction in adults is most often caused by age-related anatomical changes or low-grade infection or inflammation of the lacrimal drainage system.
Proximal end blockage:
- Lid ectropion resulting in eversion of the punctum away from the tear lake: Ectropion can be caused by any chronic inflammation/infection (blepharitis, allergic conjunctivitis), scarring (chemical burns, skin disease), facial nerve palsy, age-related changes to the lid anatomy, or history of blepharoplasty
- Megalocaruncles: Enlarged caruncle that extends to the level of the lower punctum with excess tissue that pushes punctum away from its appositional location with the tear lake
- Punctal stenosis: Scarring/narrowing/occlusion
- Canalicular stenosis: Scarring/narrowing/occlusion, topical and systemic medications can cause scarring (topical timolol, systemic docetaxel, systemic 5-fluorouracil)
Distal end blockage:
- Lacrimal sac and nasolacrimal duct obstructions: Dacryocystitis, dacryolith formation, cysts, mucocele, neoplasms
The Patient
Clinical Symptoms
- Watering of one or both eyes, with or without periocular pain
- Pain, redness, and swelling around lacrimal sac or upper lid
- Foreign body sensation
Clinical Signs
- Negative Jones I or II tests
- Asymmetric dye disappearance test
- Increased lacrimal tear lake
- Lid, punctum, caruncle abnormalities
- Tender swollen lacrimal gland or sac area
- Expression of purulent material from the punctum
Demographics
Epiphora can present in all age groups.
Significant History
- Persistent tearing
- Recurrent sinusitis or dacryocystitis
- Swelling or pain over lacrimal sac
- History of facial trauma or lid surgery
Laboratory Tests
- Culture any discharge if infectious etiology is suspected on blood (all bacteria), chocolate (children: Haemophilus sp.), thioglycollate (aerobic and anaerobic bacteria), and Sabouraud’s (fungi) agar
- Suspected thyroid disease: Serology for T3, T4, TSH
- Suspected sarcoidosis: Chest x-ray, serum ACE
- Suspected Wegener’s granulomatosis: Sinus and chest x-ray, ANCA test, ESR, CRP
- Suspected Sjögren’s syndrome: Consistent history (dry mucus membranes, enlarged salivary, or parotid glands), ESR, CBC, rheumatoid factor, antinuclear antibodies
- Dacryocystography (DCG)
1. Conventional DCG: Contrast medium is passed through canaliculus and nasolacrimal system and imaged with CT, sequential radiographic images, or fluoroscopy
2. Magnetic Resonance DCG: Dilute contrast medium is used and ionizing radiation is avoided
- CT: Axial and coronal views allow visualization of bony lacrimal canal, nasal cavity, and sinuses. Indicated with history of trauma and sinus surgery or concern about the presence of a tumor
Other Diagnostic Tests
- After infectious, inflammatory, or neoplastic lacrimal duct obstruction has been ruled out, further tests are indicated: (See “Lacrimal Tests and Procedures” for more detail.)
1. Dye disappearance test: Confirm asymmetric production/or drainage of tears
2. Tear breakup time (TBUT), Schirmer’s testing, phenol red thread testing, rose bengal dye staining, or lissamine green dye staining: Rule out dry eye or other irritations
3. Careful questioning of the patient regarding environmental irritants and examination of the lids, lashes, and adnexa for signs of secondary causes of hypersecretion: Rule out blepharitis, trichiasis
4. Careful examination of the lid and punctum position in relationship to the globe and tear lake: If no observable cause of hypersecretion is found and the puncta are in apposition to the globe, a diagnosis of lacrimal system blockage is made
5. Jones I test: Negative result confirms, but does not localize the blockage
6. Jones II test: Positive result and dye is retrieved from nasal cavity, the blockage is distal in the lacrimal system. Positive result and clear fluid is retrieved from the nasal cavity, the blockage is at the puncta or canaliculi. Failure to retrieve clear fluid or dye signifies complete blockage
Punctal Malposition
ICD-9: 375.51
- Blepharoplasty: When ectropion or entropion is leading to malposition of the punctum and subsequent epiphora
- Carunculectomy: When underlying cause of punctal malposition is megalocaruncle
Congenital Obstruction
ICD-9: 375.55 or 743.65
- Treat any suspected infection
- Massage lacrimal sac from the common canalicular junction down to the ampulla: Technique is best accomplished while feeding the infant, ten strokes four times a day, most obstructions spontaneously resolve within the first year
- Lacrimal probing between 6 and 12 months of age: Probing after 12 months decreases success rate, probing before 6 months carries inherent risks of anesthesia
- Balloon dacryocystoplasty (DCP), silicone tube intubation, or DCR:
1. Children who do not respond to lacrimal massage and probing
Acquired Obstruction
ICD-9: 375.56
- Treat any active infection with topical or systemic antibiotics (see “Dacryocystitis”/“Canaliculitis”).
- Negative Jones I test: Irrigate lacrimal drainage system to rule out punctal/canalicular stenosis
- Irrigation fails: Initiate further workup or refer patient to oculoplastic surgeon for evaluation.
Hypersecretion
ICD-9: 375.21
- Manage dacryoadenitis if present (see “Dacryoadenitis”)
- Rheumatology consult for suspected sarcoidosis, Wegener’s granulomatosis, or Sjögren’s disease
- Correct any trichiasis
- Manage ocular surface disease, (see “Ocular Surface Disease”), allergic conjunctivitis (see “Atopic Eye Disease”), blepharitis (see “Blepharitis”)
Ocular Surface Disease
Andrew Mick
ICD-9: 375.15
 THE DISEASE
THE DISEASE
Pathophysiology
The ocular surface is maintained by the interaction of sensory receptors and their neural connections to a variety of cells that produce the tear film. The tear film itself has numerous functions including creating a smooth refracting surface, transporting nutrients to the avascular cornea, and protecting tissues from infection. The quality of the tear film is influenced by hormones, systemic medications, emotions, dietary intake (specifically vitamin A), and a variety of environmental factors. The tear film was originally believed to be composed of three layers, but now is generally considered to contain only two. The most superficial is the thin lipid layer, which is secreted by the meibomian glands that are located within the upper and lower lids. The lipid layer serves to decrease the rate of evaporation of the tear film. Under the lipid layer is the thick aqueous-mucin gel layer. The aqueous component of this layer is produced by the main and accessory lacrimal glands. The mucin component of the layer, which is believed to be most concentrated closest to the surface epithelium, is primarily secreted by the conjunctival goblet cells. The aqueous-mucin layer allows for even wetting of the ocular surface in addition to being a barrier to foreign materials. It also contains antimicrobial proteins, nutrients, and growth factors, which further aid the superficial epithelium. The tear film is smoothed and refreshed by the blink of the lids.
While commonly referred to as simply dry eye, any abnormality to the composition or quantity of tears, disruption of the normal eyelid anatomy, or dysfunction of the blink mechanism can result in tissue damage and inflammation. The surface epithelium and tear film of patients with ocular surface disease show unique characteristics. There is an increase of the tear osmolarity as the deficiency of the aqueous component concentrates the tear film. The increased osmolarity and overall dryness results in damage to the cornea and conjunctiva and elicits an inflammatory response. The role of inflammation is evidenced by an increased number of lymphocytes and inflammatory cytokines in the tears of patients with ocular surface disease and is the basis behind the usage of topical steroidal and immunosuppressive therapies in dry eye patients.
Etiology
Ocular surface disease can be classified into two main groups that have different etiologies but often have overlap in the final injury and inflammation pathways. These two categories are evaporative tear loss and aqueous deficiency.
Evaporative Tear Loss
The main cause of evaporative tear loss is blockage or a deficiency in the production of the normal lipid layer by the meibomian glands. With the loss of the stabilizing lipid layer, the aqueous component of the tear film is lost at a higher rate. Meibomian gland dysfunction can occur in isolation but often accompanies dermatologic disorders such as acne rosacea (see “Ocular Rosacea”) and seborrheic dermatitis. Staphylococcal and seborrheic blepharitis (see “Bacterial Blepharitis”/“Meibomianitis”) also can influence the stability of the tear film by producing toxins and lipases that irritate the corneal epithelium and induce an inflammatory response. The lipid layer can also be influenced by the placement of a contact lens into the tear film, abnormalities in the blink mechanism, or prolonged exposure secondary to disrupted lid anatomy.
Aqueous Deficiency
This form of ocular surface disease is primarily caused by a decrease in the secretion from the primary and accessory lacrimal glands and subsequent deficiency in the aqueous component of the tear film. Classically, this condition is caused by Sjögren’s syndrome, but other etiologies exist.
Sjögren’s Syndrome Sjögren’s syndrome is a generalized systemic autoimmune disease characterized by lymphocytic infiltration of the exocrine glands. In the primary form, the glands throughout the body are affected, resulting in keratoconjunctivitis sicca, xerostomia (dry mouth), and dryness to other mucus membranes including the nose and vagina. Secondary Sjögren’s syndrome has the same signs in addition to a systemic autoimmune disorder (see Sjögren’s syndrome).
Non-Sjögren’s Syndrome Other less common causes of decreased aqueous layer production by the lacrimal glands exist. Disruption of the neuronal secretion control can occur after surgical procedures such as laser-assisted in situ keratomileusis. Damage of the accessory conjunctival glands and ducts of the primary gland can result from scarring processes in disorders such as trachoma, ocular cicatricial pemphigoid, Stevens-Johnson’s syndrome, and chemical burns. Infiltrative diseases, such as sarcoidosis and lymphoma, can result in destruction of the glands. Systemic medications such as oral contraceptives, β-blockers, antihistamines, tricyclic antidepressants, and benzodiazepines can depress aqueous tear production as well.
Clinical Symptoms
- Foreign body sensation
- Gritty, burning, or soreness of the eyes
- Red eyes
- Photophobia
- Discharge on the lashes
- Symptoms exacerbated by wind, arid environments, and air conditioning
Clinical Signs
- Conjunctival injection
- Punctate epithelial defects (concentrated inferiorly and in the interpalpebral zone)
- Decreased height of inferior tear meniscus
- Mucus debris in the tear film
- Increased blink rate
- Decreased TBUT
- Fluorescein and vital dye staining
- Positive Schirmer’s test
Demographics
The incidence of dry eye increases with age and is extremely common in the elderly. The condition is more prevalent in women, especially in the postmenopausal period. Dry eye is a common sequela of a variety of autoimmune diseases. Those people who live in dry environments or whose work requires prolonged near or computer tasks are often afflicted. Contact lens wearers also have a higher rate of dry eye symptoms.
Significant History
- Bilateral (may be asymmetrical)
- Long-standing
- Symptoms often worse in the morning
- Symptoms exacerbated by smoke, wind, heat, low humidity, prolonged near or computer work
- Taking systemic β-blockers, antihistamines, tricyclic antidepressants, benzodiazepines, or oral contraceptives
- Additional systemic symptoms that might signal the presence of Sjögren’s syndrome or other autoimmune disease
Ancillary Tests (See Lacrimal Tests and Procedures)
- TBUT
- Fluorescein stain
- Vital dye stain (Rose Bengal, Lissamine Green)
- Schirmer’s test
- Phenol red thread test
The Treatment
After careful examination of the eye and eyelids is undertaken and appropriate additional tests have been performed, treatment should be initiated to address the underlying cause of the ocular surface disease. Any lid anatomical variant or dysfunction in the blink mechanism should be referred to an oculoplastics specialist. Contact lens wearers should consider changing lens materials, changing lens care system, decreasing wear time, or discontinuing wear. Avoidance of contributing environmental factors such as wind, smoke, fumes, and air conditioning should be discussed. If suspected underlying autoimmune disease is present, a rheumatology consult is indicated.
Evaporative Tear Loss
The usual cause of evaporative tear loss is a disorder of the lipid layer and subsequent decrease in the aqueous component of the tear film. The main cause of lipid layer dysfunction is meibomian gland disease and blepharitis. These disorders often respond well to simple lid hygiene and warm compresses, but topically applied antibiotic ointment or oral doxycycline may be required. It has been proposed that oral supplements containing omega-3 fatty acids (flaxseed oil, fish oil) may enhance the quality of the lipid layer, but true efficacy and safety have not been extensively studied.
- Warm compresses and lid hygiene done twice to three times daily
- Artificial tears four times a day. (Nonpreserved formulations are always preferred and should be used if more than four times a day dosing is required to relieve symptoms.) (See “Ophthalmic Lubricants.”)
- Lubricating ophthalmic ointment at bedtime
- Consider erythromycin, bacitracin, or polymyxin B/bacitracin ophthalmic ointment applied to lid margins at bedtime
- Consider topical azithromycin 1% ophthalmic solution (Azasite: Inspire Pharmaceuticals, Durham, NC) twice daily for 2 days then once daily for 2 weeks
- Consider doxycycline 100 mg orally, two times a day for 4 weeks, then taper
- Lubricating ophthalmic ointment at bedtime
Aqueous Deficiency
In this disorder, the main problem is a deficiency in the aqueous component of the tear film. Consequently, the treatment focuses on replacing lost tears, conserving present tears, and controlling the secondary inflammation.
Mild
- Artificial tears four times a day (nonpreserved formulations are always preferred and should be used if more than four times a day dosing is required to relieve symptoms)
- Lubricating ophthalmic ointment at bedtime
Moderate
- Lubricating ophthalmic gels four times a day
- Nonpreserved artificial tears four times a day to every 30 minutes
- Ophthalmic ointment at bedtime
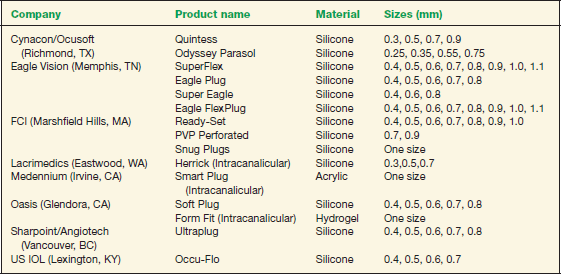
- Consider punctal occlusion (Table 11-1)
Severe Ocular Surface Disease
- Nonpreserved artificial tears every 2 hours to every 30 minutes
- Ophthalmic ointment at bedtime
- Punctal occlusion or cauterization
- Consider time-released dissolvable hydroxypropyl cellulose insert (Lacrisert: Merck, West Point, PA) placed in the lower fornix once daily
- Consider pulsed mild topical steroid: Fluoromethalone alcohol 0.1% suspension: four times a day; Loteprednol etabonate 0.2% or 0.5% suspension (Alrex and Lotemax: Bausch and Lomb, Madison, NJ) four times a day for 1 to 2 weeks
TABLE 11-1 Commercially Available Nondissolving Punctal Plugs (Numerous Companies Have Dissolving Punctal Plugs)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


