Purpose
To evaluate the association between improvement of photoreceptor integrity and visual acuity (VA) after anti–vascular endothelial growth factor (anti-VEGF) injections in neovascular age-related macular degeneration (AMD).
Design
Retrospective, cross-sectional study.
Methods
Eighty-seven eyes of 84 patients who were newly diagnosed with neovascular AMD and treated with anti-VEGF injections were reviewed retrospectively. Using spectral-domain optical coherence tomography, the status of the inner segment/outer segment photoreceptor junction (IS/OS) was graded and classified into 3 groups at baseline and 1 and 2 months after 3 monthly injections. The proportion of the improved IS/OS line after treatment was analyzed and correlated with VA.
Results
The number of eyes in the IS/OS+ group, representing disrupted IS/OS line less than 200 μm, was increased from 9 (10%) at baseline to 33 (38%) at 1 month. There was a significant difference in the ratio of IS/OS+ group between baseline and 1 month ( P < .001). Those in the IS/OS± group, showing focal disrupted IS/OS line between 200 and 800 μm, decreased from 29 (33%) to 22 eyes (25%). Improvement of the IS/OS line at 1 month compared to baseline was noted in 43 eyes (49%) and correlated with better VA ( P < .016). No increase of VA was observed in 44 eyes without definite improvement. There was no significant correlation between improvement of the IS/OS line and VA from 1 to 2 months.
Conclusions
Assessing the change of the photoreceptor integrity before and after treatment would be a useful indicator to predict initial response to treatment and visual prognosis in patients with neovascular AMD.
Neovascular age-related macular degeneration (AMD), characterized by abnormal choroidal neovascularization (CNV), is the leading cause of blindness among the aging population in developed countries. Recently, anti–vascular endothelial growth factor (anti-VEGF) therapies have become the treatment of choice for CNV, with a better visual outcome than other well-documented therapies. The PrONTO study, which adopted an as-needed dosing scheme, was based on optical coherence tomography (OCT) findings with favorable results. OCT has become an essential examination to evaluate the necessity of retreatment. These clinical trials showed that visual acuity (VA) continued to improve rapidly during the first 3 months and maintained since 2 months after the third injection.
The introduction of spectral-domain OCT (SD-OCT) has significantly improved the delineation of retinal features including the inner segment/outer segment (IS/OS) photoreceptor junction. The integrity of the IS/OS line was found to correlate with VA in patients with various macular diseases. However, little is known about the association between the IS/OS line and visual outcome in AMD patients after anti-VEGF treatment. Only 1 report has shown that the IS/OS line continuity was required for good VA in 22 patients with AMD who were treated with anti-VEGF injections. The aim of the current study was to document the IS/OS line condition at baseline, then at 1 and 2 months after 3 monthly anti-VEGF injections. The change of the photoreceptor integrity after treatment was followed with SD-OCT, and the correlation between the improvement rate of the IS/OS line and visual gain was evaluated in patients with neovascular AMD.
Methods
We retrospectively reviewed the clinical records of all patients who were diagnosed with neovascular AMD at the vitreoretinal service clinic of the Yonsei University Severance Hospital from May 1, 2009 to July 31, 2010. We used the hospital clinical database (CDR software, Yonsei University Severance Hospital, Seoul, Korea) to identify patients with neovascular AMD who received intravitreal anti-VEGF injections. The eligibility criteria were as follows: 1) age >50 years; 2) neovascular AMD proven by fundus photograph and fluorescein angiography (FA); 3) treatment with intravitreal anti-VEGF monotherapy (ranibizumab or bevacizumab); 4) follow-up for a minimum of 6 months; and 5) availability of results from a SD-OCT examination. The exclusion criteria were as follows: 1) history of vitrectomy or cataract extraction during follow-up; 2) history of previous treatment for AMD, such as verteporfin photodynamic therapy (PDT) or intravitreal anti-VEGF therapy; 3) myopia of more than 3 diopters; 4) CNV caused by any condition (such as angioid streak, choroidal rupture, and ocular histoplasmosis syndrome) other than AMD; and 5) presence of comorbid ocular conditions that might affect VA.
In total, 84 patients (87 eyes) who met the criteria were included for study evaluation. A complete ophthalmologic examination was performed during the initial visit. This included measurements of best-corrected visual acuity (BCVA), intraocular pressure, slit-lamp biomicroscopy with a noncontact lens, and indirect ophthalmoscopy. BCVA was measured with a Snellen chart and Snellen BCVA was converted to logarithm of the minimal angle of resolution (logMAR) scale. Counting fingers VA was assigned a logMAR value of +2.0 (0.01), according to methods used by Holladay.
The diagnoses were verified by FA and indocyanine green angiography, using the Heidelberg Retina Angiograph (Heidelberg Engineering, Heidelberg, Germany). The neovascular complex location was classified into 3 categories: subfoveal, juxtafoveal, or extrafoveal. The lesion compositions were classified into 4 categories: predominant classic, occult (occult with minimally classic), polypoidal choroidal vasculopathy (PCV), and retinal angiomatous proliferation (RAP).
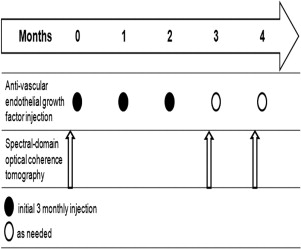
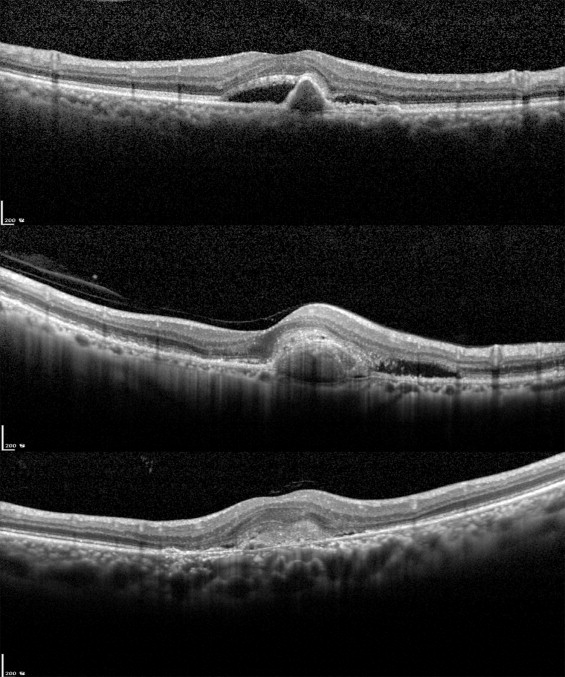
Three consecutive monthly injections of anti-VEGF were performed, followed by an as-needed dosing regimen. SD-OCT was done at baseline and 1 and 2 months after 3 monthly injections ( Figure 1 ) . SD-OCT images were obtained using Spectralis (Heidelberg Engineering, Heidelberg, Germany). Vertical cross-sectional scans were centered on the fovea for analysis and multiple raster scans were also obtained. The eye tracking system was used to ensure that the scans were taken in the correct positions. Central macular thickness, volume within a 1.0-mm-diameter area, and outer nuclear layer (ONL) thickness at foveal center were measured by the calipers of the SD-OCT with manual correction. Baseline levels of intraretinal fluid, subretinal fluid, and pigment epithelial detachment (PED) were analyzed. The photoreceptor IS/OS layer was evaluated 500 μm in either vertical direction from the fovea. The continuity of IS/OS junction was graded and classified into 3 groups. A patient was placed in the IS/OS+ group, which reflected a nearly intact IS/OS line, when the disruption was 200 μm or less. Patients were assigned to the IS/OS± group for focal disruptions between 200 and 800 μm, and the IS/OS- status was assigned to patients for diffuse disruption of more than 800 μm. Figure 2 shows the example of 3 categories of IS/OS line status used in the present study. All grading of the IS/OS junction was performed by trained personnel who were unaware of the VA or other information on the eyes. Every evaluation was done twice by the same personnel.
Statistical analysis was performed using SPSS 18.0 (SPSS, Chicago, Illinois, USA). All values are presented as mean ± standard deviation unless otherwise specified. Bowker’s symmetry test was used to compare the ratio of IS/OS status at baseline and 1 and 2 months after 3 monthly anti-VEGF injections. Bivariate relationships were examined using the Spearman correlation coefficient. A paired t test was used to compare 2 groups, and measurement values of the 3 groups were compared using 1-way analysis of variance (ANOVA) with Bonferroni correction. P values of less than .05 were considered to be statistically significant.
Results
Eighty-seven eyes from 84 patients were included in the analysis. The baseline characteristics of the 84 patients are summarized in Table 1 . The mean age was 72.7 ± 8.2 years. Subjects received a mean of 5.7 injections during a mean follow-up period of 10.4 ± 4.3 months. Ranibizumab was administered in 53 of 87 eyes (61%). Baseline FA revealed a mixture of lesion types (22% classic, 60% occult, 11% PCV, 7% RAP) that were mostly located at the subfovea (68%) or juxtafovea (29%).
| Variables | |
|---|---|
| No. eyes | 87 |
| No. patients | 84 |
| Age, y (range) | 72.7 ± 8.2 (51–93) |
| Sex, no. (%) | |
| Male | 53 (63) |
| Female | 31 (37) |
| Medical history, no. patients (%) | |
| Diabetes | 13 (15) |
| Hypertension | 42 (50) |
| Anti-VEGF treatment, no. eyes (%) | |
| Ranibizumab | 53 (61) |
| Bevacizumab | 34 (39) |
| Follow-up, mo | 10.4 ± 4.3 |
| Injections, no. (total) | 5.7 ± 2.5 |
| 19 (22): 52 (60): 10 (11): 6 (7) |
| 59 (68): 25 (29): 3 (3) |
As shown in Table 2 , the mean baseline VA was 0.88 ± 0.52 logMAR and there was a statistically significant improvement to 0.78 ± 0.50 at 1 month (paired t test, P = .009). At 2 months, VA was 0.78 ± 0.56 logMAR ( P = .030). At baseline, 9 eyes (10%) showed a nearly intact IS/OS line beneath the fovea (IS/OS+ group) and 29 eyes (33%) had focal disruption of IS/OS line (IS/OS± group), whereas 49 eyes (56%) had diffuse disruption (IS/OS- group). When the continuity of the IS/OS line was graded at 1 month, the number of eyes in the IS/OS+ group was 33 (38%); 22 eyes (25%) and 32 eyes (37%) were classified in the IS/OS± and IS/OS− groups, respectively. The percentage of the IS/OS+ group increased from 10% at baseline to 38% after treatment, and this difference was statistically significant under the Bowker symmetry test ( P < .001). Among 9 eyes that were classified as the IS/OS+ group at baseline, 6 eyes had no change of IS/OS integrity, maintaining the same grade at 1 and 2 months. There was aggravation of the IS/OS line in the other 3 eyes after treatment with concomitant decrease of VA. At 2 months, 34 eyes (39%) were classified in the IS/OS+ group, 26 eyes (30%) in the IS/OS± group, and 27 eyes (31%) in the IS/OS- group. There was no significant difference of the IS/OS line between 1 and 2 months.
| Baseline | 1 Month After 3 Monthly Injections | 2 Months After 3 Monthly Injections | |
|---|---|---|---|
| BCVA (logMAR) | 0.88 ± 0.52 | 0.78 ± 0.50 | 0.78 ± 0.56 |
| IS/OS+ a | 9 (10%) | 33 (38%) | 34 (39%) |
| IS/OS± b | 29 (33%) | 22 (25%) | 26 (30%) |
| IS/OS− c | 49 (56%) | 32 (37%) | 27 (31%) |
a Eyes in which the disruption of IS/OS line is less than 200 μm.
b Eyes in which the disruption of IS/OS line is between 200 and 800 μm.
c Eyes in which the disruption of IS/OS line is more than 800 μm.
The correlation between the continuity of the IS/OS line and mean VA change for 6 months was analyzed using a linear mixed model. The IS/OS line status 1 and 2 months after treatment exhibited a relatively strong correlation with mean VA change (r = 0.50, P < .001 and r = 0.38, P < .001). However, there was no correlation between the IS/OS line measured at baseline and change in VA status. There was no significant relationship observed between the VA change and other covariates (age, sex, intraretinal cysts, intraretinal or subretinal fluid, PED, ONL thickness, central macular thickness, and volume).
The investigation of the improvement of the IS/OS line after therapy is represented in Table 3 . One month after anti-VEGF injections, improvement of the IS/OS line was observed in 43 eyes (49%), and there was no change in the IS/OS line of 35 eyes (40%). A significant increase of VA was found in 43 eyes that showed the improvement of the IS/OS line ( P < .016). Eighteen eyes were assigned from the IS/OS± to IS/OS+ group and 16 eyes from the IS/OS- to IS/OS± group. The number of eyes that showed improvement from the IS/OS- to IS/OS+ group was 9 eyes at 1 month. Forty-four eyes that did not show definite improvement of the IS/OS line were lacking a significant increase of VA. At 2 months, only 11 eyes (13%) showed further improvement of the IS/OS line and no change of the IS/OS line was noted in 72 eyes (83%). There was no significant correlation of VA to the improvement of the IS/OS line during the second month. Among the 11 eyes that showed improvement of the IS/OS line, a fourth anti-VEGF injection was performed in 9 eyes because of still-active CNV upon SD-OCT examination, and 2 eyes showed resolution of fluid after just 3 monthly injections. Four eyes were classified from the IS/OS± to IS/OS+ group and 7 eyes from the IS/OS- to IS/OS± group at 2 months.
| 1 Month After 3 Monthly Injections | 2 Months After 3 Monthly Injections | |
|---|---|---|
| Improvement of IS/OS line | 43 (49%) | 11 (13%) |
| No change of IS/OS line | 35 (40%) | 72 (83%) |
| Aggravation of IS/OS line | 9 (11%) | 4 (4%) |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


