Fungal Infectious Disease
Fungal Keratitis
Nicky R. Holdeman
ICD-9: 370.05
THE DISEASE
Pathophysiology
Fungal keratitis results from invasion of the cornea by a fungal organism. While fungi are ubiquitous, they are responsible for a relatively small percentage of overall corneal infections worldwide. Unfortunately, however, because of the difficulty in diagnosing and treating these infections, they often result in devastating ocular consequences. The incidence of fungal keratitis has risen substantially in the last 20 to 30 years, probably due to the increased use of topical corticosteroids and broad spectrum antibiotics and due to better diagnostic techniques.
Etiology
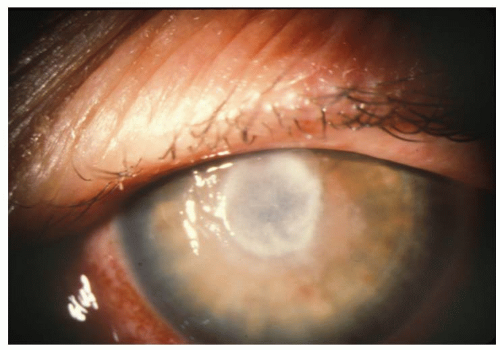
Fungal organisms include single cell yeasts, such as Candida, and multicellular filamentous fungi, such as the Fusarium species. Fungi do not invade the cornea easily and seem to require epithelial trauma, contact lens wear, ocular surface disease, corneal surgery, chronic keratitis, or immunosuppression for infection. The most common organism responsible for fungal keratitis on a worldwide basis is Aspergillus; however, keratomycosis is climate specific. In the southern United States, Fusarium is the most common cause of keratomycosis, whereas Candida and Aspergillus are isolated most frequently in the northern states. Up to 70 different fungi have been implicated as etiologic agents of fungal keratitis (Figs. 8-1 and 8-2).
The Patient
The clinical presentation of keratomycosis may vary—the findings in a filamentous fungal keratitis may be somewhat different than those seen in a yeast infection. The patient’s immune status, duration of involvement, and prior treatment may also modify the findings.
Clinical Symptoms
Pain
Conjunctival redness
Light sensitivity
Tearing/discharge
Foreign body sensation
Clinical Signs
Conjunctival injection (but may be minimal)
Epithelial defect (or less commonly an intact and slightly elevated epithelium)
Gray or grayish-white leukocytic stromal infiltrate often with an irregular feathery border
Anterior chamber reaction; possibly hypopyon with fibrinoid aqueous
Dry, rough, or gritty texture in the area of involved cornea
Satellite lesions surrounding the primary infiltrate
Endothelial plaque
Note: While some of these findings may be useful in raising ones level of suspicion for a fungal infection, in actuality, fungal keratitis has no pathognomonic appearance. It is often difficult to clinically differentiate between fungal and bacterial keratitis.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree