Purpose
To determine the success rate of the initial fundus photography session in producing gradable images for screening diabetic retinopathy in children <18 years of age with type 1 diabetes (T1D), and to analyze outcome-associated factors.
Design
Retrospective observational cohort study.
Methods
Mydriatic red-free monochromatic 60-degree digital fundus images centered on the macula and optic disc of 213 patients were graded. Photography success was classified as “complete” if both images of both eyes were gradable, “partial” if both images of 1 eye were gradable, “macula-centered image(s) only” if only the macula-centered image of one or both eyes was gradable, and “unsuccessful” if neither macula-centered image was gradable.
Results
Complete success was reached in 97 (46%; 95% confidence interval [CI], 39–52) patients, at least partial success in 153 (72%; 95% CI, 65–78) patients, success of macula-centered image(s) only in 47 (22%; 95% CI, 17–28) patients, and in 13 (6%; 95%CI, 3–10) patients fundus photography was unsuccessful. Macula-centered images were more often gradable in both eyes than optic disc–centered images ( P < .001). Success of photography did not differ between right and left eye. Sex, age at diagnosis of T1D, and the duration of diabetes, age, and glycemic control at the time of initial photography were unassociated with complete success. Partial success tended to decrease with increasing age category ( P = .093), and the frequency of gradable macula-centered image(s) only increased with increasing age ( P = .043).
Conclusions
Less than half of the children achieved complete success, but in only 6% initial fundus photography was unsuccessful, indicating its value in assessing retinopathy in the pediatric setting.
The worldwide incidence of type 1 diabetes (T1D) in children has increased dramatically during the last 3 decades: The Diabetes Mondiale Study spanning the 1990s showed that the yearly incidence of T1D varied from 0.1 per 100 000 in China and Venezuela to 40.9 per 100 000 in Finland, which had the highest incidence of all 57 countries studied.
In Finland, the incidence of T1D in children <15 years of age was even higher, 64.2 per 100 000 per year during the period from 1980 to 2005, growing fastest in the age group of 0–4 years. A new annual peak incidence of 64.9 per 100 000 was observed in 2006, but since then the incidence has reached a plateau. It has been estimated that over half a million Finns suffer from diabetes and that approximately 40 000 of them have T1D.
Diabetic retinopathy (DR) is the most common complication of T1D. Almost all patients with an onset of T1D under the age of 30 years have some type of DR 20 years from diagnosis. DR is the leading cause of acquired visual impairment in the working age group in Finland. Because DR can progress despite being asymptomatic for a long time, regular screening of the ocular fundi to detect the onset and to follow the progression of DR is important.
Mydriatic fundus photography is the most effective screening method for DR, with a sensitivity exceeding 80%. Screening is often carried out with a 45-degree fundus camera. However, stationary 60-degree cameras can also be used for better coverage of the fundi. A green filter and monochromatic photography enhance the detection of hemoglobin-containing changes, as compared with color images.
The American Academy of Ophthalmology and Diabetes Association recommend that clinical ophthalmic examinations as a screening method for DR be started 3–5 years after a diagnosis of T1D, followed by annual reviews for pediatric patients older than 9 years. The National Health Service in the UK recommends both clinical fundus examination and fundus photography annually for all T1D patients aged 12 years and older. In Finland, photographic screening of children with T1D is recommended to commence at the age of 10 years regardless of the duration of T1D. This age was chosen as a compromise as compared to an individual onset of photography at the beginning of puberty, which is when DR usually starts to occur. DR has, however, been reported in prepubertal children. If no DR is detected, imaging should be performed at 2-year intervals and annually after DR is detected or if images are ungradable. Fundus photography as a part of regular follow-up visits at the Children’s Hospital in Helsinki was established in 1997, and the present digital camera has been in operation since 2005.
It is presently unknown how often the first fundus photography session is successful in children, in terms of providing gradable fundus images in a clinical setting. We assessed this as a part of a study of DR in children with T1D. Our hypotheses were that (1) fundus photography is more difficult to perform in younger as compared with older patients, and (2) macula-centered (MC) images are more often gradable than optic disc–centered (DC) images. Furthermore, we assessed whether girls cooperate better than boys, whether those with better glycemic control cooperate better than those with worse control, and whether a younger age at the onset of T1D, or a longer duration of diabetes, was associated with imaging success.
Methods
Results of success in terms of providing gradable fundus images in children during their first-ever fundus photography session were reviewed as a retrospective, observational cohort study. The study was approved by the Coordinating Ethics Committee of the Hospital District of Helsinki and Uusimaa, and it was performed in accordance with the Declaration of Helsinki.
Eligibility Criteria
The children who were eligible for inclusion in the study had been diagnosed with T1D during the period from 2000 to 2013 at Children’s Hospital, Helsinki, Finland; were under the age of 16 years; resided in Helsinki; and underwent initial fundus photography during the period 2009–2013 when they were 9–17 years of age. The search for eligible patients was carried out at Children’s Hospital, where all new T1D patients are registered. A total of 213 patients were identified, and all were enrolled in this study.
Fundus Photography and Classification of Photographic Success
Two 60-degree fundus images of each eye, 1 centered on the macula (MC) and the other on the optic disc (DC), were taken after pupillary dilation with 0.5% tropicamide drops during regular outpatient visits by 1 of 3 trained nurses. All images were taken with a digital Canon CF-60UD fundus camera (Canon Inc, Tokyo, Japan). Images were monochromatic (black-and-white), obtained with a green filter (ie, red-free), and stored using IMPAX Client software (Agfa HealthCare, Greenville, South Carolina, USA). Photographic success was graded by 1 observer (T.G.) using a slightly modified classification of the Atherosclerosis Risk in Communities (ARIC) Study ( Supplemental Table ; Supplemental Material available at AJO.com ). For each patient, all 4 images were graded separately and evaluated in terms of focus and clarity, consistency with aimed field definitions, visibility of the principal structures (ie, the macula and optic disc), and image artifacts. Typical reference images are shown in Figure 1 .
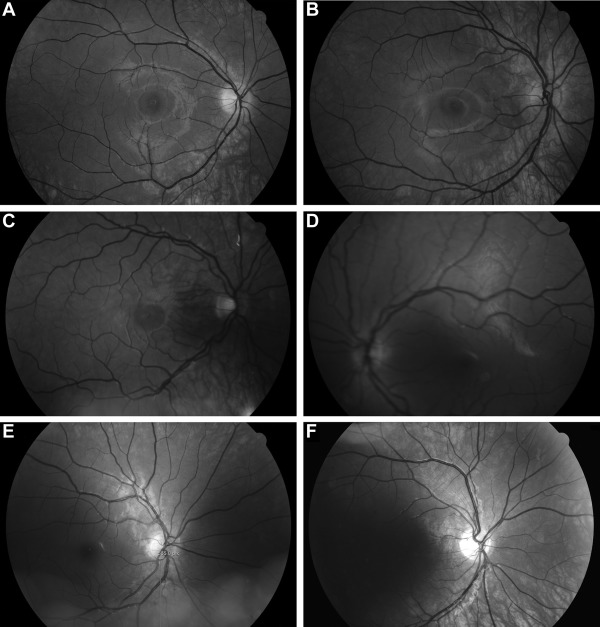
A single fundus image was classified as “excellent” when it had good focus and clarity, it adhered to the field definitions, the macula and optic disc were fully visible and gradable, and there were no artifacts ( Supplemental Table ). An image was classified as “gradable” when it was at least of fair quality with regard to field definitions, focus, and clarity, allowing for minor artifacts but no obscuration of the macula or optic disc. An image was considered “ungradable” if the above criteria were not met. Furthermore, if the macula was not visible owing to more nasal centralization in an otherwise “gradable” DC image, it was classified as “partially gradable.”
Photography was graded as a “complete success” if both images of both eyes were gradable and as “partial success” when the 2 images of only 1 eye were gradable. When at least 1 MC image was gradable, photography was graded “macula-centered image(s) only,” and when neither of the MC images was gradable, photography was considered to have been “unsuccessful.” In addition, an alternative grading of “qualified complete success” was achieved when the outcome was “complete success” except for the DC image(s) being “partially gradable.”
Grading of photographic success did not specify other situations in which the DC image of 1 eye was gradable in addition to the MC image of the other eye. Rather, these images were labeled as “macula-centered image(s) only.” Furthermore, if the DC images of both eyes but no MC images were gradable, photography was classified as “unsuccessful.”
Baseline data (sex, date of birth, date of diagnosis of T1D, and glycohemoglobin 1A [HbA1c] level at the time of the initial photography session) were entered from patient charts into an Excel file (Microsoft, Seattle, Washington, USA). The date of the initial fundus photography session was taken from the IMPAX Client database.
Statistical Methods
Data were imported from Excel and analyzed using statistical IBM SPSS software for Windows (version 22; SPSS Inc, Chicago, Illinois, USA). Continuous variables are expressed as median and range. Exact binomial 95% confidence intervals (CI) are given for the main findings. The association between age and the outcome of fundus photography was evaluated using age as a continuous variable or, alternatively, by dividing the study population in 3 age groups on the basis of age at the initial photography session. The Pearson χ 2 test and the Kruskal-Wallis test were used to compare unordered and singly ordered contingency tables, respectively. The Mann-Whitney U test was used to compare the distribution of continuous variables. Differences between 2 dependent categorical variables were assessed with the McNemar test. The Bonferroni correction was used when appropriate to adjust for multiple comparisons. A P value of < .05 was considered statistically significant.
Results
Of the 213 patients, 121 (57%) were male. The median age of all patients at the time of the T1D diagnosis was 8.7 (range, 1–15) years. Age at the time of the initial fundus photography was 11.2 (range, 9–17) years. At this time, the median duration of T1D was 2.3 (range, 0.2–9.6) years, and the median HbA1c was 8.5% (6.3%–13.8%). The number of patients in the 3 defined age groups of 9–10, 11–12, and 13–17 years was 96 (45%), 57 (27%), and 60 children (28%), respectively.
Success of Fundus Photography
Complete success with the initial fundus photography was obtained in 97 patients (46%; 95% CI, 39%-52%), whereas partial success was achieved in 56 patients (26%; 95% CI, 21%-33%). Thus, at least partial success was reached in 153 patients (72%; 95% CI, 65%-78%). Macula-centered imaging was successful in 47 cases (22%; 95% CI, 17%-28%), so at least 1 gradable MC image was obtained in 200 patients (94%; 95% CI, 90%-97%). In 13 patients (6%; 95% CI, 3%-10%), the initial fundus photography session was unsuccessful. At least qualified complete success was reached in 136 patients (64%; 95% CI, 57%-70%).
Univariate analysis did not show an association between the presence or absence of complete success vs sex, age at diagnosis, HbA1c level, duration of diabetes, and age at photography ( Table 1 ).
| All Patients | Complete Success of Photography | Not Complete Success of Photography | P Value | |
|---|---|---|---|---|
| Number of patients | 213 | 97 | 116 | |
| Sex | ||||
| Male, n (%) | 121 (57) | 59 (61) | 62 (53) | .28 NS a |
| Female, n (%) | 92 (43) | 38 (39) | 54 (47) | |
| Age at diagnosis of T1D | ||||
| Median y | 8.7 | 8.3 | 8.8 | .77 NS b |
| Range (y) | (1.0–16.0) | (1.3–16.0) | (1.0–15.6) | |
| Age at the first photography | ||||
| Median y | 11.2 | 11.2 | 11.2 | .55 NS b |
| Range (y) | (9.5–17.9) | (9.7–17.3) | (9.5–17.9) | |
| Duration of T1D at the initial photography | ||||
| Median y | 2.3 | 2.3 | 2.2 | .82 NS b |
| Range (y) | (0.2–9.6) | (0.7–9.6) | (0.2–9.4) | |
| HbA1c | ||||
| Median % | 8.5 | 8.3 | 8.6 | .41 NS b |
| Range (%) | (6.3–13.8) | (6.3–13.1) | (6.3–13.8) | |
The percentages of gradable MC and DC images of the right and left eye for the 3 age categories were comparable ( Table 2 ). MC images of both eyes were gradable in 78 patients in the youngest group (81%), 47 in the intermediate group (82%), and 52 patients in the oldest group (87%), and the MC image of 1 eye only was gradable in 10 (10%), 9 (16%), and 4 patients (7%), respectively. DC images of both eyes were gradable in 46 (48%), 28 (49%), and 29 patients (48%) in the 3 age groups, and both DC images were ungradable in 19 (20%), 14 (25%), and 22 patients (37%), respectively.
| Image | Age Group | |||
|---|---|---|---|---|
| 9-10 Years, N (%; 95% CI) | 11–12 Years, N (%; 95% CI) | 13–17 Years, N (%; 95% CI) | Total N (%; 95% CI) | |
| RMC | 83 (86; 78–93) | 51 (89; 78–96) | 53 (88; 77–95) | 187 (88; 83–92) |
| RDC | 68 (71; 61–80) | 35 (61; 48–74) | 36 (60; 47–72) | 139 (65; 58–72) |
| LMC | 83 (86; 78–93) | 52 (91; 81–97) | 55 (92; 82–97) | 190 (89; 84–93) |
| LDC | 55 (57; 47–67) | 36 (63; 49–76) | 31 (52; 38–65) | 122 (57; 50–64) |
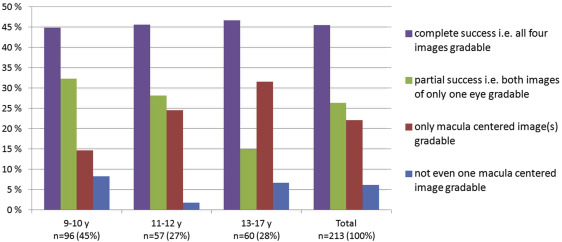
Complete success was reached equally often in the 3 age categories (43 [45%], 26 [46%], and 28 patients [47%], respectively) ( Figure 2 ). No difference in the percentages of patients with unsuccessful photography (8%, 2%, and 7%, respectively) was apparent. However, 32% of patients in the youngest age group reached partial success, as compared with 28% in the intermediate and 15% in the oldest group ( P = .093, Kruskal-Wallis test with Bonferroni correction for 4 comparisons; Figure 2 ). The frequency of gradable MC image(s) only increased with increasing age (15%, 25%, and 32%, respectively; P = .043, Kruskal-Wallis test).
Quality of Macula-Centered Versus Optic Disc–Centered Images
MC image field definition reached good grade in both eyes of 192 patients (90%), and no one had a poor grade field in either eye ( Table 3 ). Furthermore, the macula was fully visible and gradable in both eyes of 201 patients (94%), and the optic disc was free of obscurations in both eyes of 206 patients (97%). The focus and clarity grade was good in both eyes of 131 patients (62%), and in 1 eye only of 55 patients (26%). At least fair focus and clarity grade were achieved in both eyes of 184 patients (86%). Artifacts in the MC images of both eyes were seen in 43 patients (20%), and of 1 eye only in 65 patients (31%).
| Photographic Parameter | Focus: Good Field: Good Artifacts: No Mac O/M: No Disc O/M: No N (%) | Focus: Fair Field: Fair N (%) | Focus: Borderline Field: Poor Artifacts: Yes N (%) | Focus: Inadequate Mac O/M: Yes Disc O/M: Yes N (%) | Cannot Grade N (%) | Missing Image N (%) |
|---|---|---|---|---|---|---|
| Right macula-centered image | ||||||
| Field | 205 (96) | 8 (4) | 0 (0) | – | 0 (0) | 0 (0) |
| Focus | 156 (73) | 39 (18) | 16 (8) | 2 (0.9) | 0 (0) | 0 (0) |
| Disc o/m | 210 (97) | – | – | 3 (1) | – | 0 (0) |
| Macula o/m | 207 (97) | – | – | 6 (3) | – | 0 (0) |
| Artifacts | 136 (64) | – | 77 (36) | – | – | 0 (0) |
| Right optic disc–centered image | ||||||
| Field | 37 (17) | 152 (71) | 7 (3) | – | 1 (0.5) | 16 (8) |
| Focus | 117 (55) | 59 (28) | 19 (9) | 2 (0.9) | 0 (0) | 16 (8) |
| Disc o/m | 186 (87) | – | – | 11 (5) | – | 16 (8) |
| Macula o/m | 158 (74) | – | – | 39 (18) | – | 16 (8) |
| Artifacts | 106 (50) | – | 91 (43) | – | – | 16 (8) |
| Left macula-centered image | ||||||
| Field | 199 (93) | 12 (6) | 0 (0) | – | 1 (0.5) | 1 (0.5) |
| Focus | 161 (76) | 32 (15) | 14 (7) | 5 (2) | 0 (0) | 1 (0.5) |
| Disc o/m | 209 (98) | – | – | 3 (1) | – | 1 (0.5) |
| Macula o/m | 204 (96) | – | – | 8 (4) | – | 1 (0.5) |
| Artifacts | 138 (65) | – | 74 (35) | – | – | 1 (0.5) |
| Left optic disc–centered image | ||||||
| Field | 52 (24) | 133 (62) | 8 (4) | – | 2 (0.9) | 18 (8) |
| Focus | 120 (56) | 60 (28) | 13 (6) | 2 (0.9) | 0 (0) | 18 (8) |
| Disc o/m | 182 (85) | – | – | 13 (6) | – | 18 (8) |
| Macula o/m | 133 (62) | – | – | 62 (29) | – | 18 (8) |
| Artifacts | 94 (44) | – | 101 (47) | – | – | 18 (8) |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


