Purpose
To identify whether and how outcomes of macular hole (MH) surgery are influenced by the extent of internal limiting membrane (ILM) peeling.
Design
Randomized clinical trial.
Methods
This study involved 65 eyes from 65 patients who underwent surgery for idiopathic MH. ILM was peeled with a radius of either 0.75 disc diameter (small-extent group, SEG) or 1.5 disc diameter (large-extent group, LEG), according to the randomization. Anatomic success, visual acuity, and metamorphopsia score (M-score) were measured at 2- and 6-month postoperative visits. The distance between the foveal center and the parafoveal edge of the outer plexiform layer on optical coherence tomography was measured in 4 directions, and further distance increases in certain directions were defined as asymmetric elongation of foveal tissue.
Results
Complete closure of the MH was observed after initial operation in 97.0% of eyes in both groups. The mean visual improvement at 6 months after surgery was 20.4 ± 12.8 and 19.1 ± 10.8 ETDRS letters in SEG and LEG, respectively ( P = .452). The mean amount of improvement in M-score was 0.26 ± 0.55 in SEG and 0.50 ± 0.53 in LEG ( P = .039). There was a difference in the mean degree of asymmetric elongation between the 2 groups (22.5% ± 10.8% in SEG vs 13.4% ± 5.8% in LEG, P = .001). And there was inverse correlation between the mean degree of asymmetric elongation and the amount of improvement in M-score at 6 months postoperatively ( P < .001).
Conclusion
Larger extent of ILM peeling during MH surgery is beneficial with respect to reduction of metamorphopsia, alleviating asymmetric elongation of foveal tissue.
Since Kelly and Wendel introduced the vitrectomy technique to reattach the macular hole (MH), considerable advances in surgical treatment have been achieved. As a consequence, MH has now become a surgically treatable disease with standardized techniques incorporating vitrectomy, induction of posterior vitreous detachment, internal limiting membrane (ILM) peeling, and gas tamponade. Although there was a debate on ILM peeling in the past, ILM peeling has been established to improve surgical success rates. In addition, retinal ILM peeling has been facilitated by staining dye such as indocyanine green.
The rationale for ILM peeling is that MH can occur and enlarge owing to contraction of perifoveal vitreous and cellular constituents with myofibroblastic differentiation on the surface of the ILM. Although ILM has no inherent contractile properties, it does act as a scaffold for contractile tissue to exert tangential traction on fovea.
Several studies using optical coherence tomography (OCT) have reported the dynamic sealing process after MH surgery. Foveal tissue elongation and macular migration have been noted following ILM peeling after surgery for MH and diabetic macular edema. In addition, there is a significant correlation between these morphologic changes and visual function such as metamorphopsia.
Although ILM peeling has become a widely accepted surgical technique since the introduction of MH surgery, the optimal extent of ILM peeling is not known and the anatomic and functional outcomes according to peeling extent have not been investigated. The purpose of this study was to investigate the influence of the extent of ILM peeling on anatomic and functional outcomes of MH surgery.
Methods
This prospective randomized clinical trial was performed at a single center according to the tenets of the Declaration of Helsinki. The study protocol ( Supplementary Text ; Supplemental Material available at AJO.com ) was approved by the institutional review board and ethics committees (Samsung Medical Center IRB no. 2013-07-083, ClinicalTrials.gov identifier NCT02010138 ). Subjects were recruited between July 12, 2013 and March 23, 2015. Trial follow-up of the last enrolled subject was completed in November 2015. All patients provided written informed consent before enrollment.
The study population consisted of subjects 18 years of age or older diagnosed with idiopathic MH before undergoing vitrectomy. Idiopathic MH was defined as a defect of the foveal retina involving its full thickness from the ILM to the outer segment of the photoreceptor layer without other accompanying ophthalmic disorders.
Exclusion criteria included eyes with traumatic MH, evidence of ocular inflammation, diabetic retinopathy, hypertensive retinopathy, retinal vasculitis, media opacity that would influence visual acuity or preclude acquisition of clear spectral-domain OCT images, −6.0 diopters or more of spherical equivalent, presence of staphyloma, history of intraocular surgery other than uncomplicated cataract surgery, and other ocular diseases that could influence macular microstructure or visual function. Patients who declined to participate in the study were also excluded.
At baseline, a detailed demographic and medical history was collected, and all subjects underwent a complete preoperative evaluation, including examination for best-corrected visual acuity (BCVA) using the Early Treatment Diabetic Retinopathy Study (ETDRS) chart (Lighthouse International, New York, New York, USA), M-chart (Inami Co, Tokyo, Japan) test, anterior segment examination, and dilated fundus examination with a 90 diopter lens. Horizontal and vertical OCT scans through the fovea were performed with a combined confocal scanning laser ophthalmoscope and spectral-domain OCT (Spectralis HRA-OCT; Heidelberg Engineering, Heidelberg, Germany). Metamorphopsia score (M-score) measurement was performed using the M-chart according to a previously described method.
Randomization and Treatment
The block randomization method was designed by an independent clinical trial consultant. Subjects were randomized based on preallocated codes placed in sealed envelopes that were opened during the randomization visit by a trial coordinator. Based on the code, each subject was randomized to either the small-extent group (SEG) or the large-extent group (LEG). Participants and examiners who were assessing outcomes were masked to the assignment of groups.
A standard 3-port pars plana vitrectomy was performed by a single surgeon (S.W.K.) using the Constellation (Alcon Laboratories Inc, Fort Worth, Texas, USA) or Associate (Dutch Ophthalmic Research Center, Inc, Zuidland, The Netherlands) 23 gauge vitrectomy system. After core vitrectomy, the posterior hyaloid membrane was removed using the vitreous cutter. In cases without posterior vitreous detachment, partial posterior hyaloidectomy was performed to prevent the risk of triggering peripheral break. Then, peeling of the retinal ILM was performed using vitreous forceps with the assistance of indocyanine green dye staining. Scrapers were never used. With reference to the size of the optic nerve, the ILM was pinched with end-gripping forceps (Grieshaber Maxgrip 723.13; Alcon Laboratories Inc, Fort Worth, Texas, USA) at the point of desired radius (0.75 or 1.5 disc diameter). Then, the strand of ILM was peeled off radially toward the foveal center. Then another short strand of ILM was peeled off circumferentially toward the initial pinching point to create an L-shaped slit for starting round-shaped laminorrhexis ( Supplemental Figure ; Supplemental Material available at AJO.com ). The operator then pulled the ILM flap and lifted several times at its mid-edge, paying special attention to create a round-shaped laminorrhexis ( Figure 1 ). This was followed by a complete fluid–gas exchange using either 25% sulfur hexafluoride gas or 14% perfluoropropane gas. The selection of gas was dependent on the size and duration of MH. That is, we used 25% sulfur hexafluoride gas if the MH was smaller than 400 μm with a symptom duration shorter than 3 months. Otherwise, we used 14% perfluoropropane gas. Combined cataract surgery was conducted in patients with visually significant cataracts or incipient cataracts in subjects older than 60 years. All patients were encouraged to maintain a face-down position for at least 5 days postoperatively. Subjects with persistent MH at the first postoperative visit or reopened MH were supposed to undergo additional fluid–gas exchange along with intravitreal injection of autologous platelet concentrate.
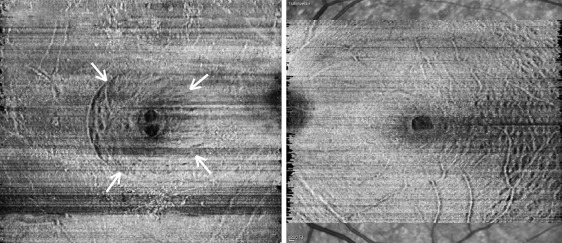
Outcome Measures
Postoperative measurements of BCVA and M-score were conducted at 2- and 6-month follow-up visits by independent, masked observers. The amount of improvement in BCVA and M-score values between the preoperative visit and the postoperative 6-month follow-up were defined as the Δ BCVA and Δ M-score, respectively.
The first postoperative OCT scanning was usually conducted 1–2 weeks after operation according to intraocular gas status. After that, OCT scans were conducted at follow-up visits 2 and 6 months postoperatively. The same experienced examiner conducted all OCT scans on all subjects.
OCT images of 1:1 μm setting, rather than 1:1 pixel setting, were used for measurement. The measurements were performed manually using the contained Heidelberg Eye Explorer software (version 1.5.12.0; Heidelberg Engineering). MH size was calculated as the mean of the horizontal and vertical diameters. Two independent observers (K.B., J.M.Y.) analyzed the images in a masked fashion.
To evaluate postoperative elongation of the foveal tissue, the distance between the edges of the outer plexiform layer (OPL) was measured and defined as the inter-OPL distance. The difference in inter-OPL distance between horizontal and vertical images was defined as horizontal-vertical asymmetry. The horizontal-vertical percent asymmetry (H-V % asy) was calculated as (horizontal inter-OPL distance − vertical inter-OPL distance) × 100/(horizontal inter-OPL distance + vertical inter-OPL distance). The absolute value of H-V % asy was used for analysis. To evaluate asymmetric elongation of foveal tissue on the same horizontal or vertical plane, we measured the distance from the foveal center to the edge of the OPL as nasal, temporal, superior, and inferior foveal length, according to the direction. To determine the accurate “foveal center,” 4–6 OCT scans were usually performed. The localization of the foveal center was facilitated by the outer foveolar defect, which was usually detected in the few months after surgery. The image with the largest outer foveolar defect was taken as an image scanning foveal center. If there was no outer foveolar defect, the thinnest foveal location was considered the foveal center. The asymmetry of both horizontal and vertical planes was evaluated on the basis of postoperative 6-month OCT scan. The horizontal percent asymmetry (Hor % asy) was calculated as (nasal foveal length − temporal foveal length) × 100/(nasal foveal length + temporal foveal length). The vertical percent asymmetry (Ver % asy) was also calculated as (superior foveal length − inferior foveal length) × 100/(superior foveal length + inferior foveal length). The absolute value of Hor % asy or Ver % asy was used for analysis, except for correlation analysis with outer macular thickness. The mean % asy in each eye was calculated as (absolute value of Hor % asy + absolute value of Ver % asy)/2.
Infrared images linked to the OCT scans have also been used to assess morphologic changes around the removed ILM margin. Points in an imaginary circle with the radial length of approximately 1.25 disc diameter from the foveal center, which encounters retinal vascular landmarks such as the intersection of retinal vessels, were set as a paramacular reference spot (PRS). The distance from the foveal center to the PRS was measured by the innate caliper function of the Heidelberg Eye Explorer software (version 1.5.12.0; Heidelberg Engineering) and was defined as nasal length, temporal length, superior length, and inferior length according to the direction. The distance between the edges of the PRS was measured and defined as the vertical or horizontal inter-PRS distance. Analysis was performed using the increment ratio of distance at first postoperative visit and 2-month and six-month postoperative visits on the basis of preoperative distance, as the PRS was an arbitrarily determined point that could not be compared as an absolute numerical value. The absolute value of the degree of mean percent increment of horizontal and vertical inter-PRS was used for analysis.
An ETDRS-style topographic map of macular thickness was generated automatically by built-in segmentation software. The mean thicknesses of the macular inner ring segments (0.5–1.5 mm from foveal center) and macular outer ring segments (1.5–3.0 mm from foveal center) in the nasal, temporal, superior, and inferior directions were measured on the basis of the result of 20 × 15-degree raster scans consisting of 19 horizontal scans.
Sample Size Calculations and Data Analysis
The primary outcome measure in this study was the amount of improvement in metamorphopsia (Δ M-score) 6 months after intervention. In our initial proposal, we had estimated that the group receiving large-extent ILM removal would show a 100% improvement in metamorphopsia score compared with the group receiving small-extent ILM removal. The necessary sample size was calculated from the results of our previous study. Based on the continuous endpoint, 2-sided, 2-sample t test with an α-error of .05 and a power of 90% was conducted. Allowing for a dropout rate of 10%, 64 patients (32 per group) were calculated to be recruited with an allocation ratio of 1:1.
The primary analysis was conducted to identify the difference in functional and anatomic outcomes between the 2 groups. Subsequent analysis was performed to reveal the relationship between functional and anatomic outcomes. That is, comparison of anatomic closure rate, BCVA, M-score, Δ BCVA, and Δ M-score were made between the 2 groups. Then, associations of horizontal inter-OPL distance, vertical inter-OPL distance, H-V % asy, mean % asy, mean percent increment of inter-PRS, and retinal thickness profile with changes in ETDRS visual acuity and M-score were analyzed. The frequency of additional treatment and complications were also evaluated.
Statistical analyses were performed by an independent statistician using SAS version 9.3 (SAS Inc, Cary, North Carolina, USA). The χ 2 test was used for categorical variables, and the Wilcoxon rank sum test and t test were used for comparison of continuous variables. Appropriate parametric analyses were performed when the data were normal. Associations of mean inter-OPL distance or mean inter-PRS distance with preoperative MH size, visual acuity, and M-score were determined using Spearman correlation analyses. A P value less than .05 was considered significant.
Results
Sixty-five patients were randomized to either the SEG (n = 33) or LEG (n = 32) group. Complete closure of macular hole after initial operation was noted in 32 of 33 eyes (97.0%) in SEG and in 31 of 32 eyes (96.9%) in LEG. One patient of each group experienced persistent MH after initial operation and was excluded, and 4 patients were lost to follow-up before 6 months post-surgery. Those persistent MHs were closed by additional fluid–gas exchange along with autologous platelet concentrate injection. Finally, complete closure of MH was noted in all 65 eyes. Other serious postoperative complications, such as recurrence of MH, intractable increase in intraocular pressure, rhegmatogenous retinal detachment, and endophthalmitis were not observed. Thus, 30 SEG patients and 29 LEG patients were ultimately included in the study ( Figure 2 ).
Table 1 outlines the baseline characteristics of the patients. There were no significant differences in baseline characteristics, including the size and stage of MH, BCVA, or M-score, between the groups ( Table 1 ). The 25% sulfur hexafluoride gas was applied on 17 eyes in SEG and 16 eyes in LEG, and the 14% perfluoropropane gas was applied on 13 eyes in SEG and 13 eyes in LEG. In terms of lens status, 26 eyes (86.7%) in SEG and 27 eyes (93.1%) in LEG were phakic preoperatively. Combined cataract extraction was performed for 6 eyes (20.0%) in SEG and 9 eyes (31.0%) in LEG. After macular hole surgery, 12 eyes (40%) in SEG and 11 eyes (37.9%) in LEG underwent cataract surgery during the follow-up period. Thus, 22 eyes (73.3%) in SEG and 22 eyes (75.9%) in LEG were pseudophakic at 6 months postoperatively. Preoperative and postoperative lens statuses were not different between the 2 groups.
| Characteristics | Small-Extent Group (n = 30) | Large-Extent Group (n = 29) | P Value |
|---|---|---|---|
| Baseline | |||
| Age, mean ± SD, y (range) | 64.3 ± 7.7 (47∼78) | 63.7 ± 8.1 (39∼78) | .742 |
| Sex (M/F), n | 7/23 | 6/23 | .807 |
| Lens status, n (%) | .671 | ||
| Phakic | 26 (86.7%) | 27 (93.1%) | |
| Pseudophakic | 4 (13.3%) | 2 (6.9%) | |
| Stage, n (%) | .771 | ||
| 2 | 19 (63.3%) | 18 (62.1%) | |
| 3 | 7 (23.3%) | 5 (17.2%) | |
| 4 | 4 (13.3%) | 6 (20.7%) | |
| MH size, a μm, mean ± SD (horizontal × vertical) | 321.3 ± 144.4 (333.4 × 309.1) | 335.3 ± 158.8 (342.4 × 328.2) | .723 |
| BCVA, mean ± SD, letters (range) | 50.2 ± 13.0 (22∼71) | 49.7 ± 10.9 (28∼71) | .862 |
| M-score, mean ± SD (range) | 0.79 ± 0.51 (0.0∼2.0) | 0.85 ± 0.63 (0.0∼2.0) | .767 |
| Postoperative 6 months | |||
| Lens status, n (%) | .825 | ||
| Phakic | 8 (26.7%) | 7 (24.1%) | |
| Pseudophakic | 22 (73.3%) | 22 (75.9%) | |
| BCVA, mean ± SD, letters (range) | 70.6 ± 11.4 (35∼85) | 68.8 ± 10.4 (39∼81) | .622 |
| M-score, mean ± SD (range) | 0.53 ± 0.44 (0.0∼1.8) | 0.34 ± 0.34 (0.0∼1.3) | .091 |
| ΔBCVA, mean ± SD, letters (range) | 20.4 ± 12.8 (−15∼44) | 19.1 ± 10.8 (−1∼50) | .676 |
| ΔM-score, mean ± SD (range) | 0.26 ± 0.55 (0.1∼1.7) | 0.50 ± 0.53 (−0.4∼1.6) | .039 |
a Minimum hole dimension (maximal hole diameter at narrowest point) was used for measuring the size of MH.
The mean BCVAs measured at baseline and at 2 and 6 months postoperatively were 50.2 ± 13.0, 63.9 ± 11.7, and 70.6 ± 11.4 ETDRS letters in SEG and 49.7 ± 10.9, 62.6 ± 11.5, and 68.8 ± 10.4 letters in LEG, respectively. The M-scores measured at baseline and at 2 and 6 months postoperatively were 0.79 ± 0.51, 0.56 ± 0.49, and 0.53 ± 0.44 in SEG and 0.85 ± 0.63, 0.44 ± 0.50, and 0.34 ± 0.34 in LEG, respectively. During each follow-up period, BCVA, M-score, and ΔBCVA showed no significant difference between the 2 groups. ΔM-score values, the mean amount of improvement in metamorphopsia between the preoperative visit and the postoperative 6-month follow-up, were 0.26 ± 0.55 in SEG and 0.50 ± 0.53 in LEG, and the difference was significant ( P = .039) ( Table 1 , Figure 3 ). In the additional analysis, baseline BCVA, size of MH, stage of MH, preoperative outer foveal changes on OCT, and choice of gas tamponade during surgery were not correlated with ΔM-score ( Supplemental Tables 2–4 ; Supplemental Material available at AJO.com ).
Degree of Asymmetric Elongation of the Fovea and its Influence on Visual Acuity and Metamorphopsia
Table 2 shows the changes in mean horizontal and vertical inter-OPL distance during the study period. Elongation of both vertical and horizontal inter-OPL distance was observed in all 59 eyes during the follow-up period. The SEG tended to have larger inter-OPL distances over the entire period. However, the vertical and horizontal distances at postoperative 6 months were not significantly different between the 2 groups ( P = .097 and P = .101, respectively). At 6 months postoperatively, the mean absolute value of H-V % asy was 12.6% in SEG and 12.0% in LEG ( P = .921).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


