Purpose
To evaluate the asymmetry of bilateral orbital development in Chinese children with congenital microphthalmia and to provide a criterion for tailoring treatment timing and therapy.
Design
Retrospective cohort study.
Methods
By combining multisection helical computerized tomography imaging with a computer-aided design system, we measured 38 children between 0 and 6 years of age with congenital microphthalmia and 70 normal children of the same age group. Variables were measured, including orbital volume, depth, width, and height and eyeball volume. Displacement of the orbital rims was calculated by mirroring the unaffected orbit across the midsagittal plane of body.
Results
Significant differences were observed between the orbital volume, eyeball volume, orbital width, and orbital height of the affected and unaffected sides of children with congenital microphthalmia ( P < .001). The difference between the orbital depth of the affected and unaffected sides was not significant ( P = .055). Growth of the inferior and lateral rims retarded by an average of 3 mm, whereas that of the medial and superior rims retarded by less than 1 mm.
Conclusions
The amount of decrease in orbital volume of children with congenital microphthalmia is related to the severity of the disease (decrease in size of the eye), rather than to age. Retarded orbital development is evident primarily in the inferior and lateral rims, correlating mostly with zygomatic and then maxilla and frontal bone. The growth of the affected orbit slows down or even stagnates by 3 years of age. Intervention therapy before 3 years of age was critical.
Congenital microphthalmia is a genetic disease that can lead to abnormal ocular and facial development. Diagnosis usually is made based on the dimension of cornea and diameter of the globe. Microphthalmia usually is defined as a corneal diameter of less than 10 mm and an anteroposterior globe diameter of less than 20 mm, excluding the short axial length resulting from eyeball atrophy. The prevalence of congenital microphthalmia in China is reported to be up to 9 cases per 100 000 people, whereas the incidence from other countries varies between 8 and 32 cases per 100 000 people. It is the leading cause of blindness among congenital eye diseases. No significant gender difference is noted in patients with congenital microphthalmia. In patients with congenital microphthalmia, 43.9% have unilateral microphthalmia, whereas 72.9% of patients with isolated microphthalmia have unilateral disease. In cases of unilateral defect, the orbit is affected. In addition, the growth of the face can be affected without proper stimulation from a normal globe. The condition eventually can lead to severe facial asymmetry, which subsequently results in tremendous physical and psychological impact on the affected child. At present, treatments in such cases focus on orbital development and cosmesis, but not on sight recovery. Therefore, the purpose of this study was to explore the development of the orbit by measuring orbital volume, global volume, and various orbital diameters in both patients and normal children and to provide clinical evidence for the management, timing, and efficacy of intervention.
Methods
Demographics
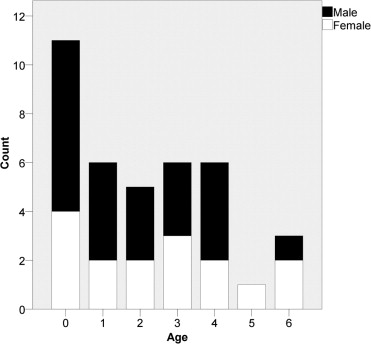
A retrospective cohort study was performed in the patients who were diagnosed with congenital microphthalmia between January 2007 and December 2009 in Beijing Tongren Hospital. The study enrolled 38 pediatric patients of Chinese descent (age range, 0 to 6 years; 22 males and 16 females; Figure 1 ). All of the subjects were diagnosed with unilateral congenital microphthalmia before study enrollment. Study data were collected before any treatment. Controls included 70 patients of the same ethnic group (age range, 0 to 6 years). Those patients underwent computerized tomography (CT) scanning in our hospital between March 2008 and August 2010 as part of routine medical care. Control patients with any structural abnormalities, such as craniofacial deformities, tumors, orbital trauma, or nasosinusitis, were excluded from the study. The controls were divided into 7 age groups, with 10 subjects in each group.
Methods
Examination Method
Each patient was placed in a supine position and scanned using a Brilliance 64-slice spiral CT scanner (Royal Dutch Philips Electronics Ltd, Eindhoven, The Netherlands), with the orbitomeatal line as the baseline. The following criteria were used for the CT scans: 120 Kv, 200 mA, 0.625 mnd64i, and 512 × 512 pixel matrixes. Output of the CT scan was imported to a computer-aided design system (iPlan Cranial Software, version 2.5; BrainLAB, Munich, Germany), which then produced 3-dimensional reconstructions of the orbit.
Orbital Volume Measurement
The entire orbit was contained in approximately 70 layers of horizontal CT slices. The surface of the orbit was examined layer by layer in the horizontal plane. The outline of the orbit was drawn on the first and eighth layer of the horizontally cut CT. The surface area of the orbit on the first and eighth layers was calculated with iPlan Cranial software. Then, the outlines of the 6 intervening layers were divided evenly and were generated automatically using the same software. The same measuring method was applied to the entire patient population ( Figure 2 ).
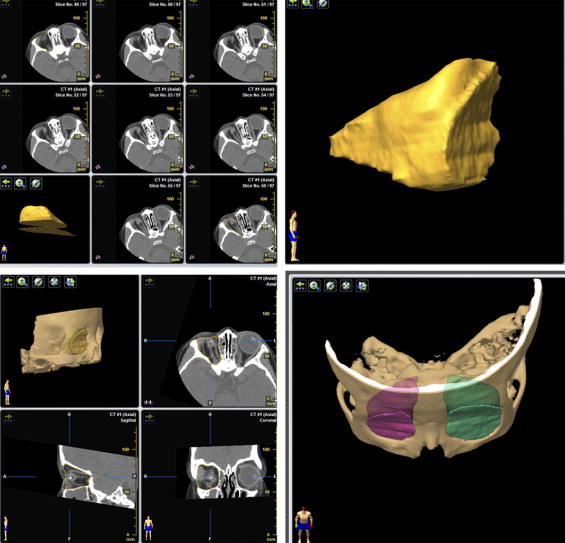
Global Volume Measurement
Method 1 for the measurement of the healthy eye was as follows. The slice with the greatest area on the horizontally cut CT was found, and the distance between the corneal peak and the posterior pole of the eyeball was measured. Thus, the anteroposterior diameter was obtained. The maximum horizontal distance perpendicular to the anteroposterior diameter on the horizontal cut CT is the transverse diameter. The unaffected eyeball was approximated to be a sphere, so the volume was obtained using the cubature formula:
V = 4 / 3 π r 3 ,
Method 2 for the measurement of the healthy eye was as follows. To obtain the volume, the eyeball was outlined in each slice on the horizontally cut CT, and the volume was obtained using iPlan Cranial software (same as the method used to measure orbital volume).
Measurement of the affected eyeball was as follows. Because of its irregular shape, this volume could not be calculated using the cubature formula as previously stated. For this reason, the orbit was outlined in each slice to obtain the volume.
The ball-to-orbit ratio was calculated using the formula below:
B a l l – t o – o r b i t r a t i o = G l o b a l V o l u m e O r b i t a l V o l u m e .
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


