Purpose
To evaluate EyeCam in detecting changes in angle configuration after laser peripheral iridotomy (LPI) in comparison to gonioscopy, the reference standard.
Design
Prospective comparative study.
Methods
Twenty-four subjects (24 eyes) with primary angle-closure glaucoma (PACG) were recruited. Gonioscopy and EyeCam (Clarity Medical Systems) imaging of all 4 angle quadrants were performed, before and 2 weeks after LPI. Images were graded according to angle structures visible by an observer masked to clinical data or the status of LPI, and were performed in a random order. Angle closure in a quadrant was defined as the inability to visualize the posterior trabecular meshwork. We determined the number of quadrants with closed angles and the mean number of clock hours of angle closure before and after LPI in comparison to gonioscopy.
Results
Using EyeCam, all 24 eyes showed at least 1 quadrant of angle widening after LPI. The mean number of clock hours of angle closure decreased significantly, from 8.15 ± 3.47 clock hours before LPI to 1.75 ± 2.27 clock hours after LPI ( P < .0001, Wilcoxon signed rank test). Overall, gonioscopy showed 1.0 ± 1.41 (95% CI, 0.43-1.57) quadrants opening from closed to open after LPI compared to 2.0 ± 1.28 (95% CI, 1.49-2.51, P = .009) quadrants with EyeCam. Intra-observer reproducibility of grading the extent of angle closure in clock hours in EyeCam images was moderate to good (intraclass correlation coefficient 0.831).
Conclusions
EyeCam may be used to document changes in angle configuration after LPI in eyes with PACG.
Laser peripheral iridotomy (LPI) is the recommended first-line intervention in both acute and chronic forms of primary angle-closure glaucoma (PACG). LPI eliminates pupil block, the primary underlying mechanism for the condition; causes flattening of iris convexity; and may cause widening of the anterior chamber angle.
Gonioscopy, the current reference standard for assessing angle structures, is limited by its dependency on single-observer interpretation and is difficult to perform in a reproducible fashion. Gonioscopy requires the placement of a contact lens on the eye of the patient, and gonioscopic findings may vary with the type of lens used as well as ambient lighting conditions. Although 1 study found that one may document angle opening after LPI with gonioscopy, this is difficult to do in an objective manner. Imaging devices such as ultrasound biomicroscopy (UBM) and anterior segment optical coherence tomography (ASOCT) have been used to measure quantitative changes in angle parameters after LPI, but these were based on angle measurements.
The EyeCam (Clarity Medical Systems, Pleasanton, California, USA) is a new technology that was originally designed to obtain wide-field photographs of the fundus. With recent modifications of the lens angulation, the device can be used to visualize structures in the angle in a manner similar to direct gonioscopy. The EyeCam is able to record images that can be saved on a computer, thus allowing comparisons to be made over time. This may be useful to track angle changes with disease progression as well as after treatment. In this study, we evaluated the use of EyeCam in detecting changes in angle configuration after LPI in PACG eyes in comparison to gonioscopy, the reference standard.
Methods
We recruited 24 consecutive PACG patients from glaucoma clinics of the Singapore National Eye Centre who were undergoing LPI. All eyes had angle closure (defined as the presence of at least 180 degrees of angle in which the posterior pigmented trabecular meshwork was not visible on non-indentation gonioscopy in the primary position) with glaucomatous optic neuropathy (GON) (defined as the presence of vertical cup-to-disc ratio ≥0.7 or cup-to-disc asymmetry ≥0.2 or focal neuroretinal rim notching, with corresponding visual field changes). A glaucomatous visual field defect was defined if the following were found: 1) glaucoma hemifield test (GHT) outside normal limits, and 2) a cluster of 3 or more, non-edge, contiguous points, not crossing the horizontal meridian with a probability of <5% of the age-matched normal on the pattern deviation plot on 2 separate occasions. Exclusion criteria were a history of previous cataract surgery or any corneal opacities or abnormalities that precluded EyeCam imaging, as well as eyes with secondary angle closure. Sequential argon-yttrium-aluminum-garnet (YAG) LPI was performed in all cases with standardized settings (argon laser 0.7-1.0 W, spot size 50 μm, duration 0.1 seconds, 10-30 shots followed by neodymium (Nd)-YAG laser 2-5 mJ, 3-5 shots).
EyeCam Imaging
EyeCam imaging was performed before and approximately 2 weeks after LPI. Patients lay flat on a couch, and after application of topical anesthetic drops, coupling gel was applied to the lens probe and images of the superior, inferior, nasal, and temporal quadrants of the angle were obtained (4 images per eye). The lens probe was placed on a coupling gel without compression of the cornea, minimizing alteration of angle configuration. The probe was positioned at the limbus opposite to the angle being photographed, and light from the fiberoptic probe was directed into the angle of interest and then tilted downward to bring the angle structures into view. The patient looked away from the probe to improve visualization of angle structures and all imaging was performed in the dark.
Gonioscopy was performed in the dark in all cases by a single glaucoma-fellowship trained examiner (S.A.P.) who was masked to EyeCam findings. A 1-mm light beam was reduced to a narrow slit and the vertical beam was offset horizontally for assessing superior and inferior angles and was offset vertically for nasal and temporal angles. Static gonioscopy was performed using a Goldmann 2-mirror lens at high magnification (×16), with the eye in the primary position of gaze. If there was any doubt as to the state of the angle or any suspicion of peripheral anterior synechiae (PAS), this was confirmed on indentation gonioscopy with a Sussman lens. Care was taken to avoid light falling on the pupil and to avoid accidental indentation during examination. Slight tilting of the gonioscopy lens was permitted to gain a view over the convexity of the iris.
Both gonioscopy and EyeCam were performed on the same days both before and after LPI (which was confirmed to be patent by transillumination in all cases). The light intensity at various instances of examination was examined using a lux meter (Sekonic, Studio Deluxe III, L-398A; Sekonic Corporation, Tokyo, Japan). The following luminance levels were found in this study: dark room, 0 lux; slit-beam illumination during gonioscopic examination, 32.28 lux; EyeCam illumination at the time of image capture, 129.12 lux; and standard room illumination, 430.4 lux.
Grading of Images
EyeCam images were graded at the end of the study by an independent observer (M.B.) masked to gonioscopic data and the status of LPI, and were performed in a random order. However, status of LPI could not be completely masked since a patent LPI was seen in some of the images. Images were graded for their quality as follows: grade 1 if the angle details were clear and well focused in all quadrants; grade 2 if angle images were blurred in any quadrant but some details discerned; grade 3 if the angle structures were blurred in at least 1 quadrant such that no details could be discerned; and grade 4 if the structures were blurred in all 4 quadrants and no angle details were discerned. Images were excluded if they were assessed to be grade 3 or 4.
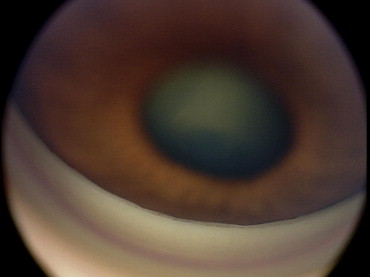
The angle-grading scheme for each quadrant was the same for both gonioscopy and EyeCam images and was based on anatomic structures observed in the angle. Angle closure in a quadrant was defined as the inability to visualize the posterior trabecular meshwork ( Figure 1 ) in that quadrant. For EyeCam images, we further quantified the extent of angle closure in a quadrant by number of clock hours.
In order to assess for intra-observer reproducibility, 30 pre- and post-LPI EyeCam images were randomly selected and graded by the same examiner twice over 2 sessions. These images were graded for angle closure status, angle structures visible, and the extent of angle closure in clock hours. Inter-observer reproducibility was assessed after grading of these 30 images by another glaucoma fellowship–trained examiner (R.S.K.).
Statistical Analysis
Statistical analysis was performed using Medcalc version 10. 0 (Medcalc, Mariaklerke, Belgium). The extent of angle closure before and after LPI was compared using Wilcoxon signed rank nonparameteric test for paired samples. Extent of angle widening between quadrants was compared using Kruskal-Wallis test. Post-LPI angle status for number of quadrants open with gonioscopy and EyeCam was compared using Mann-Whitney test. Intra- and inter-observer reproducibility was analyzed using weighted kappa statistic (for angle structure grading) and intraclass correlation coefficient (for extent of angle closure). Statistical significance was reported if P < .05.
Results
Twenty-four subjects (24 eyes) with PACG were recruited. There were 23 Chinese and 1 Indian subjects, with a mean age of 61.8 ± 7.9 years, and 62.5% (15/24) were women.
A total of 192 EyeCam images (96 quadrants each, before and after LPI) were recorded. Images were either grade 1 (66.7% [128/192]) or grade 2 (33.3% [64/192]) in quality, and all angle images could be analyzed.
Using EyeCam, all 24 eyes showed at least 1 quadrant of angle widening after LPI ( Figure 2 ) . Of these, 12 of 24 eyes had 4 quadrants of angle widening after LPI, 6 of 24 eyes had 3 quadrants, 4 of 24 eyes had 2 quadrants, and 2 of 24 eyes had 1 quadrant of angle widening after LPI. No quadrants became narrower after LPI. The mean (± SD) number of clock hours of angle closure decreased significantly, from 8.15 ± 3.47 before LPI to 1.75 ± 2.27 after LPI ( P < .0001, Wilcoxon signed rank test). There was no significant difference in the change in clock hours of angle closure between the superior, inferior, nasal, and temporal quadrants after LPI ( P > .5; Kruskal-Wallis test). While the pre-LPI apposition in clock hours between quadrants was found to be similar ( P = .5; Kruskal-Wallis test), post-LPI apposition between the inferior compared to the rest of the quadrants showed a significant difference ( P = .0006; Kruskal-Wallis test). This suggested maximum apposition in the inferior quadrant both before and after LPI.
Comparison of Angle Status After Laser Peripheral Iridotomy by Gonioscopy Versus EyeCam
Table 1 shows the number of eyes and quadrants that were open using EyeCam and gonioscopy. The angle status of 22 eyes was more open in at least 1 quadrant after LPI, and remained unchanged (and closed) in 2 eyes with gonioscopy, whereas with EyeCam, all angles opened up at least 1 quadrant. Overall, gonioscopy showed 1.0 ± 1.41 (95% CI, 0.43-1.57) quadrants opening from closed to open after LPI compared to 2.0 ± 1.28 (95% CI, 1.49-2.51, P = .009) quadrants with EyeCam. Gonioscopy consistently revealed more closed quadrants than EyeCam, before and after LPI ( Table 1 ).
| Closed Before LPI | Closed After LPI | Widened From Closed to Open After LPI | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Gonioscopy | EyeCam | P Value a | Gonioscopy | EyeCam | P Value a | Gonioscopy | EyeCam | P Value a | |
| Median (range) | 4 (2 to 4) | 3 (0 to 4) | .0035 | 4 (0 to 4) | 1 (0 to 4) | .0002 | 0 (0 to 4) | 2 (0 to 4) | .005 |
| Number of Quadrants | Number of Eyes (n=24) | ||||||||
| 0 | 0 | 1 | — | 4 | 10 | — | 13 | 2 | — |
| 1 | 0 | 0 | — | 1 | 8 | — | 5 | 8 | — |
| 2 | 1 | 6 | — | 1 | 2 | — | 2 | 4 | — |
| 3 | 0 | 6 | — | 5 | 3 | — | 1 | 7 | — |
| 4 | 23 | 11 | — | 13 | 1 | — | 3 | 3 | — |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


