Purpose
To investigate the stability of corneal astigmatism and higher-order aberrations after combined femtosecond-assisted phacoemulsification and arcuate keratotomy.
Design
Retrospective, interventional case series.
Methods
Surgery was performed using a VICTUS (Bausch & Lomb Inc, Dornach, Germany) platform. A single, 450-μm deep, arcuate keratotomy was paired at the 8-mm zone with the main phacoemulsification incision in the opposite meridian. The keratotomy incisions were not opened. Corneal astigmatism and higher-order aberration measurements obtained preoperatively and at 2 months and 2 years postoperatively were analyzed.
Results
Fifty eyes of 50 patients (mean age 66.2 ± 10.5 years) were included. The mean preoperative corneal astigmatism was 1.35 ± 0.48 diopters (D). This was reduced to 0.67 ± 0.54 D at 2 months and 0.74 ± 0.53 D at 2 years postoperatively ( P < .001). There was no statistically significant difference between postoperative corneal astigmatism over 2 years ( P = .392). Both magnitude of error and absolute angle of error were comparable between the 2 postoperative time points ( P > .283). At postoperative 2 months and 2 years, 72% and 70% of eyes were within 15 degrees of preoperative meridian of astigmatism, respectively. All wavefront measurements increased significantly at 2 months and 2 years ( P < .007), except spherical aberration ( P > .150). There was no significant difference in higher-order aberrations between 2 months and 2 years postoperatively ( P > .486).
Conclusions
Our study showed the stability of femtosecond-assisted arcuate keratotomy. Further studies using other platforms and nomograms are needed to corroborate the findings of this study.
Femtosecond laser technology allows the creation of arcuate keratotomy incisions for the management of corneal astigmatism. Femtosecond-assisted keratotomy incisions demonstrate favorable accuracy, safety, and reproducibility in the reduction of naturally occurring astigmatism, astigmatism associated with keratoplasty, and residual astigmatism after cataract and refractive surgeries compared to manual incisions. Recently, we reported the outcomes of femtosecond-assisted arcuate keratotomy during cataract surgery. Undercorrection of corneal astigmatism was observed 2 months after surgery. Overall, the studies investigating the efficacy of femtosecond-assisted arcuate keratotomy are limited by a short-term follow-up ranging from 1 to 6 months. Furthermore, evidence regarding corneal higher-order aberration after combined femtosecond-assisted arcuate keratotomy and cataract surgery is lacking in the relevant literature.
The current study investigated the long-term stability of corneal astigmatism and higher-order aberrations after combined femtosecond-assisted phacoemulsification and arcuate keratotomy over 2 years. A single penetrating arcuate keratotomy was paired with an opposite phacoemulsification incision along the steep axis in eyes with low to moderate corneal astigmatism.
Methods
This was a retrospective, interventional case series performed at the Hong Kong Laser Surgery Centre in Hong Kong. Consecutive patients who underwent combined femtosecond-assisted phacoemulsification and arcuate keratotomy between September 2013 and February 2014 were included. The Joint Chinese University of Hong Kong–New Territories East Cluster Clinical Research Ethics Committee approved the study protocol. The study was conducted in accordance with the tenets of the Declaration of Helsinki.
All patients underwent a detailed preoperative ophthalmologic assessment including slit-lamp and fundus examination. Patients with cataract and coexisting corneal astigmatism <2.5 diopters (D) were selected for surgery. Keratometry and biometry were performed by using partial-coherence interferometry (IOLMaster; Carl Zeiss Meditec Inc, Dublin, California, USA). A single reference point at the temporal limbus was marked with the patient sitting upright. Three additional points at 4, 8, and 12 o’clock were also marked on the limbus in order to identify the cornea center by drawing an equilateral triangle. The steep axis was identified with corneal topography (Nidek OPD-Scan III; Nidek Technologies, Aichi, Japan) immediately before the surgery. The angle between the steep axis and the reference point measured at the cornea center was recorded. The patient was then transferred to the femtosecond laser platform. The temporal limbus was used as a reference point for the zero degree mark on the Wallace Mendez degree gauge (Duckworth & Kent Ltd, Hertfordshire, United Kingdom). The steep axis was located with the angle derived from the OPD-Scan III.
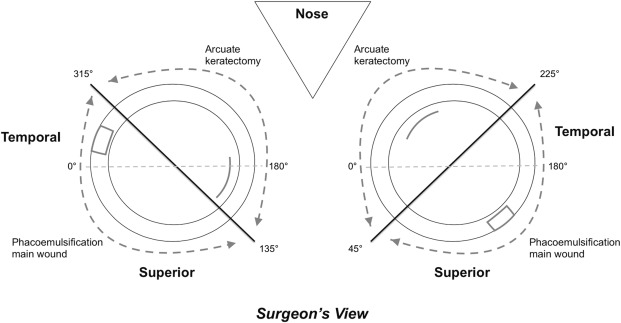
A combined phacoemulsification and arcuate keratotomy was performed using VICTUS (Bausch & Lomb Inc, Dornach, Germany) femtosecond-laser platform. A single arcuate keratotomy incision was paired in the opposite meridian with the main corneal incision for phacoemulsification. The phacoemulsification incision was fashioned between the superior and temporal peripheral cornea, as shown in Figure 1 . The depth of astigmatic keratotomy was set at 450 μm with a 90-degree side-cut angle. The optical zone diameter was set at 8 mm. The range of the angular arc length of the keratotomy incision was between 30 and 80 degrees according to the surgeon’s nomogram, which was modified from the Wallace Limbal Relaxing Incision Nomogram ( Table 1 ). The incisions were created with a programmed energy setting of 1.7 μJ and a spot/line separation of 6 × 4 μm. The main corneal incision had a triplanar configuration with a width of 3.0 mm and a length of approximately 1.8–2.0 mm. Two 1.5-mm-wide peripheral incisions with a triplanar configuration were fashioned 60 degrees apart from the main corneal incision.
| Intended Astigmatic Correction (Diopters) | Arc Length at 8-mm Optical Zone (Degrees) |
|---|---|
| ≤1.00 | 30 |
| >1.00 to ≤1.25 | 40 |
| >1.25 to ≤1.50 | 50 |
| >1.50 to ≤2.00 | 70 |
| >2.00 to ≤2.50 | 80 |
The same surgeon (G.C.) performed all surgeries under topical anesthesia. After the successful docking of the suction ring, a femtosecond laser was used to create the anterior capsulotomy, lens fragmentation, corneal incisions, and arcuate keratotomy in this sequence. After the removal of the docking cone and the suction ring, phacoemulsification was performed. The arcuate keratotomy incisions were not opened after the procedure. Postoperatively, a combination of topical dexamethasone 0.1% (Alcon Laboratories Inc, Forth Worth, Texas, USA) and tobramycin 0.3% (Alcon Laboratories Inc) eye drops was used 4 times a day for 1 month.
Corneal astigmatism and higher-order aberration measurements were obtained at the 6-mm zone from corneal topography (Nidek OPD-Scan III; Nidek Technologies) and analyzed. Vector analysis was performed to evaluate the effective correction of astigmatism. The target-induced astigmatism vector (TIA) is the intended astigmatic change after surgery. The TIA is equivalent to preoperative corneal astigmatism. The surgically induced astigmatism vector (SIA) is the astigmatic change actually induced after surgery. The difference vector (DV) is the induced astigmatic change that would enable the initial surgery to achieve its intended goals. The DV is equivalent to postoperative corneal astigmatism. The magnitude of error (ME) is the arithmetic difference between the SIA and TIA. The angle of error (AE) is the angle described by vectors of SIA vs TIA. The correction index (CI) is calculated as the ratio of SIA to TIA. It indicates an overcorrection if it is more than 1 or an undercorrection if it is less than 1.
IBM/SPSS software version 21 (IBM/SPSS Inc, Chicago, Illinois, USA) was used to perform the statistical analyses. A paired t test was used to compare the continuous variables. Bonferroni correction was applied for multiple comparisons. Pearson correlation was used for continuous variables. P < .05 was considered statistically significant.
Results
Fifty eyes of 50 patients were included in this study. The mean age was 66.2 ± 10.5 years at the time of surgery. The mean preoperative corneal astigmatism or TIA was 1.35 ± 0.48 D (range: 0.55–2.46 D). This was significantly reduced to 0.67 ± 0.54 D at 2 months and 0.74 ± 0.53 D at 2 years postoperatively ( P < .001). No difference was found between postoperative corneal astigmatism or DV measurements over 2 years ( P = .392). Both ME and absolute AE were comparably similar between the 2 postoperative time points ( P > .283) ( Table 2 ). At the end of 2 months and 2 years, 72% and 70% of the eyes were within 15 degrees of the preoperative meridian of astigmatism, respectively. The CI at 2 months and 2 years was 0.78 ± 0.52 and 0.85 ± 0.48, respectively. The flattening index (FI) quantifies the proportion of SIA that is effective to reduce astigmatism at the intended meridian. The ideal value of FI is 1. About half of the cases of corneal astigmatism were effectively reduced by SIA postoperatively as a result of misalignment represented by the absolute AE ( Table 2 ). The index of success (IS), which is the ratio of DV to TIA, indicated a success rate of 49%–59% over 2 years postoperatively ( Table 2 ). A double-angle plot of preoperative and postoperative corneal astigmatism is shown in Figure 2 .
| 2 Months | 2 Years | P Value | |
|---|---|---|---|
| TIA | |||
| Arithmetic mean ± SD (diopters) | 1.35 ± 0.48 | / | |
| Range a (D) | 1.33 to 1.37 | ||
| SIA | |||
| Arithmetic mean ± SD (diopters) | 1.16 ± 0.55 | 1.23 ± 0.58 | .283 |
| Range a (D) | 1.13 to 1.17 | 1.21 to 1.26 | |
| DV | |||
| Arithmetic mean ± SD (D) | 0.67 ± 0.54 | 0.74 ± 0.53 | .392 |
| Range a (D) | 0.65 to 0.69 | 0.72 to 0.76 | |
| ME | |||
| Arithmetic mean ± SD (D) | −0.20 ± 0.58 | −0.12 ± 0.56 | .283 |
| Range a (D) | −0.22 to −0.18 | −0.14 to −0.09 | |
| Absolute AE | |||
| Arithmetic mean ± SD (degrees) | 13.4 ± 18.0 | 14.0 ± 15.5 | .794 |
| Range a (degrees) | 12.7 to 14.0 | 13.4 to 14.6 | |
| CI | |||
| Geometric mean ± SD | 0.78 ± 0.52 | 0.85 ± 0.48 | / |
| Range a | 0.76 to 0.80 | 0.83 to 0.87 | |
| FI | |||
| Geometric mean ± SD | 0.58 ± 0.81 | 0.46 ± 0.64 | / |
| Range a | 0.55 to 0.61 | 0.44 to 0.49 | |
| IS | |||
| Geometric mean ± SD | 0.41 ± 0.51 | 0.51 ±0.53 | / |
| Range a | 0.39 to 0.43 | 0.49 to 0.53 | |
A high correlation was noted between preoperative TIA and postoperative SIA at 2 months (r = 0.322, P = .022) and 2 years (r = 0.428, P = .002) ( Figure 3 ). Moreover, a higher TIA correlated with a lower CI (r = −0.393, P = .005 at 2 months; r = −0.319, P = .024 at 2 years) ( Figure 4 , Left), as well as a lower IS (r = −0.359, P = .011 at 2 months; r = −0.351, P = .013 at 2 years) ( Figure 4 , Right). The spread of absolute AE was broad, especially for corneas with a low TIA ( Figure 5 , Left). A strong correlation was noted between absolute AE and IS (r = 0.700, P < .001 at 2 months; r = 0.766, P < .001 at 2 years), thus suggesting that treatment misalignment was a major influential factor in astigmatism correction ( Figure 5 , Right).

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


