Purpose
To validate and evaluate the reliability of retinal vessel diameter measurements by optical coherence tomography (OCT). The effects of age and hypertension on vessel diameter were also examined.
Design
Prospective, cross-sectional study.
Methods
Two hundred thirty-eight eyes (238 subjects) with no ocular disease were included. Hypertension was present in 106 subjects and absent in 132 subjects. Spectralis HRA+OCT was used to scan a circular region around the optic disc. Outer and inner diameters of the 4 largest retinal arteries and veins were measured using OCT vascular wall reflections, and vessel wall thickness was calculated.
Results
Intervisit, interexaminer, and interevaluator intraclass correlation coefficients of randomly selected vessel measurements were all greater than 0.90. Mean inner arterial and venous diameters were 87.8 ± 9.4 μm and 113.7 ± 12.5 μm, respectively. The OCT-measured mean inner arterial and venous diameters were significantly correlated to fundus photography caliber measurements ( P = .005 and P = .001, respectively). Arterial and venous wall thicknesses were 17.4 ± 2.4 μm and 13.7 ± 2.1 μm, respectively, both of which were highly correlated with subject age (arterial: r = 0.612, P < .001, venous: r = 0.455, P < .001). Additionally, both mean arterial and venous wall thicknesses were significantly greater in subjects with hypertension than in age-matched subjects without hypertension ( P = .020 and P = .015, respectively).
Conclusions
Retinal vessel diameter measurements obtained with OCT were highly reproducible and vessel wall thicknesses, calculated using outer and inner diameter measurements, were significantly thickened by both aging and systemic hypertension.
The retinal vasculature can be directly and noninvasively visualized through the transparent ocular media. This facilitates assessment of retinal vascular changes resulting from systemic and/or metabolic diseases. Classically, funduscopic findings in the retinal vasculature (ie, arteriolar narrowing, caliber irregularity, light reflex alterations, vessel wall sheathing, arteriovenous crossing phenomena) are categorized according to the Keith-Wagener-Barker and/or the Scheie classification systems, which are used to diagnose systemic arteriosclerosis or hypertension. In addition, recent semi-automated measurement software programs allow precise retinal vessel caliber measurements using digital fundus photographs. Using such measurements, population-based studies have examined risk factors associated with various diseases and have found that increased retinal venous caliber is associated with stroke and ischemic heart disease.
In the past decade, advances in optical coherence tomography (OCT) image resolution and acquisition speed have allowed more detailed observations of the retinal architecture, greatly enhancing our understanding of the pathomorphology of various macular diseases. Unfortunately, features of the retinal vasculature have not been well studied with OCT and the literature is sparse. Recently, Muraoka and associates obtained sectional OCT images of physiologically normal retinal vessels. Vessel cross-sections were usually oval in shape and appeared as 4 distinct hyper-reflectivities arranged in a linear configuration. They concluded that the innermost and outermost hyper-reflectivities represented the vessel wall itself, and that the internal paired hyper-reflectivities represented flowing blood. Because OCT has a higher resolution in the direction of the light beam, OCT should allow for precise measurement of retinal vessel vertical diameter.
In the current study, we used Spectralis HRA+OCT to measure retinal vessel diameter and wall thickness in the region surrounding the optic disc. The repeatability and validity of these measurements was also evaluated in subjects without ocular or systemic disease. The influence of age and hypertension on retinal vessels was also examined using measurements from subjects without systemic hypertension of varying age, and by comparing measurements made in age-matched subjects with and without systemic hypertension.
Methods
The Ethics Committee at Kyoto University Graduate School of Medicine approved this prospective study, which was conducted in accordance with the tenets of the Declaration of Helsinki. Written informed consent was obtained from each subject before any study procedures or examinations were performed.
Patients
This prospective study included 238 eyes from 238 subjects with no ocular disease. Subjects had no systemic diseases, except for 106 subjects who had hypertension. Retinal vessels were examined with the Spectralis HRA+OCT (Heidelberg Engineering, Heidelberg, Germany) at the Kyoto University Hospital Department of Ophthalmology between October 2011 and December 2012. Eyes that had any of the following were excluded from the study: keratoconus, high myopia (more severe than -6 diopters), high astigmatism (more severe than ±3 diopters), best-corrected visual acuity worse than 20/25, prior intraocular surgery, or any coexisting ocular disease (eg, glaucoma, diabetic retinopathy, retinal vein occlusion, age-related macular degeneration, senile cataract that diminished image quality). Subjects with systemic disease (ie, diabetes, dyslipidemia, stroke, ischemic heart disease, collagen disease), except for hypertension, were also excluded.
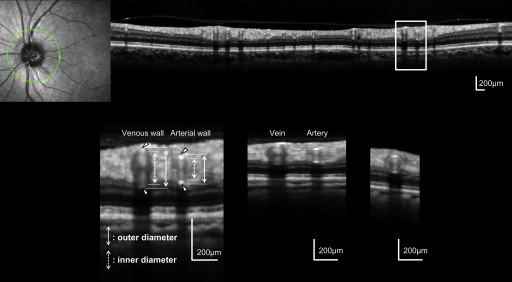
Presence of hypertension was determined based on antihypertensive agent use or by a physician’s diagnosis. After a comprehensive medical interview, refractive error was measured, keratometry was performed, and, after pupil dilation, 45-degree digital fundus photographs were obtained (3216 × 2136 pixels, TRC-50LX; Topcon, Tokyo, Japan). Finally, OCT examination was performed using the Spectralis HRA+OCT. A 3.46-mm-diameter circular scan, centered around the optic disc center, was obtained ( Figure 1 ). Each OCT A-scan had a depth of 2 mm and comprised 512 pixels, providing a depth × transverse digital sampling of 3.87 × 7.50 μm per pixel. One hundred B-scans were obtained at the same location and averaged to provide each cross-sectional image.
Measurement of Retinal Vascular Caliber on Fundus Photographs
We used 45-degree digital fundus photographs, centered 5 degrees nasal to the fovea, to measure retinal vessel caliber, as previously described. Briefly, fundus photographs were imported into computer-imaging software (IVAN; University of Wisconsin, Madison, Wisconsin, USA), and the caliber of each vessel was measured 0.5-1 disc diameters from the optic disc margin (zone B). Measurements were made in a semi-automated fashion.
Measurement of Retinal Vessel Outer and Inner Diameter and Vessel Wall Thickness Using Optical Coherence Tomography
A Spectralis HRA+OCT circular scan, centered on the optic disc, provided cross-sectional images of all major retinal arteries and veins ( Figure 1 ). Major retinal vessels radiate from the optic disc through the peripapillary area, running parallel to the retinal surface. This allows scanning light from the OCT to be projected vertically onto the vessel walls and the lumen. After obtaining an adequate scan, we measured the inner and outer vessel diameters of the 4 largest retinal arteries and veins using the built-in manufacturer’s software (Spectralis Acquisition and Viewing Modules, version 4.0; Heidelberg Engineering). As reported previously, normal vessels had an oval-shaped heterogeneous reflectivity and often had 4 distinct hyper-reflectivities in a linear configuration ( Figure 1 ). When image dimensions were adjusted so that the horizontal-to-vertical ratio was changed back to 1:1, vessel cross-sections became round ( Figure 1 ). Although retinal vessels sometimes showed a circular vascular wall ( Figure 1 ), most appeared only as reflections from the inner (towards the vitreous) and outer (towards the retinal pigment epithelium [RPE]) sides of the vessel wall. Additionally, all flowing blood appeared inside a vessel as a paired, frequently hourglass-shaped, hyper-reflectivity ( Figure 1 ).
Using our OCT measurements, vessel wall thickness was calculated using the following formula: wall thickness = (outer vessel diameter − inner vessel diameter)/2.
Masked retinal specialists measured outer and inner vessel diameter of the 4 largest arteries and 4 largest veins on each OCT scan. Based on inner vessel diameter and vessel wall thickness, the arterial wall-to-lumen ratio was calculated.
Reproducibility of Optical Coherence Tomography Vessel Diameter Measurements
Intervisit reproducibility of OCT vessel diameter measurements was examined in 25 subjects who underwent 2 OCT examinations by the same examiner at 2 different visits. Evaluations were performed between 2 weeks and 3 months apart. Interexaminer reproducibility was examined in 20 subjects who underwent 2 OCT scans on the same day, each by a different independent examiner. Repeatability of vessel diameter measurements was independently examined by having 2 retina specialists measure vessel diameter on the same OCT scan from 50 subjects. The intraclass correlation coefficient (ICC) was used to determine repeatability by using 1 randomly selected artery and 1 randomly selected vein in each subject’s OCT scan. Additionally, mean outer and inner vessel diameters were calculated by averaging OCT measurements from the 4 largest arteries and veins. These were compared with mean vessel caliber, as measured on digital color fundus photographs with assistance from semi-automated computer software.
Effect of Blood Flow on Vertical Vessel Diameter Measurement
The potential effect of blood flow on the OCT representation of retinal vessels was examined in vitro. A fine glass tube with an inner diameter of 140 μm (AS ONE, Osaka, Japan) was connected to a pump to circulate heparinized human blood collected from healthy volunteers. Blood flow rates were selected arbitrarily and the tube was scanned using the Spectralis HRA+OCT. A 25-diopter lens was attached to the OCT machine to focus on the blood flow within the glass tube. Each final OCT image was obtained by averaging 100 scans. Previous studies have shown that flow velocity in the major retinal vessels of healthy eyes is approximately 5-35 mm/s. To be within both physiologically normal and pathologic flow velocity ranges, blood flow rate within the glass tube was varied between 0.0 and 10.0 mL/h (0.0-180.5 mm/s).
Statistical Analyses
Statistical analyses were performed using the PASW Statistics software (version 18.0; SPSS, Chicago, Illinois, USA). Vessel diameter values are presented as mean ± standard deviation and were calculated using 4 selected arteries or 4 selected veins on fundus photographs or OCT sections. Student t tests were used to compare quantitative data with normal distributions and equal variance. Distributions were examined for statistical differences using χ 2 tests and bivariate relationships were analyzed using Pearson correlation coefficient. Statistical significance was defined as a P value <.05.
Results
The current study examined 238 eyes from 238 subjects (133 male, 105 female), both with and without hypertension. Mean subject age was 62.1 ± 15.6 years and ranged between 21 and 92 years ( Table 1 ). The reproducibility and validity of OCT measurements were examined in eyes of healthy volunteers with no systemic disease. Intervisit (n = 25), interexaminer (n = 20), and interevaluator (n = 50) ICCs of randomly selected vessel measurements were all greater than 0.90 ( Table 2 ). Therefore, OCT measurements of vessel diameter in the circular region around the optic disc are highly reproducible.
| Age (y, mean ± SD, range) | 62.1 ± 15.6 (21-92) |
| 20-39 years (n) | 28 |
| 40-59 years (n) | 51 |
| 60-79 years (n) | 142 |
| 80+ years (n) | 17 |
| Sex (male/female) | 133/105 |
| Hypertension (+/−) | 106/132 |
| Refractive error (diopters, mean ± SD) | −0.27 ± 1.94 |
| Keratometer reading (mm, mean ± SD) | 7.65 ± 0.30 |
| Intraclass Correlation Coefficient | |||
|---|---|---|---|
| Intervisit (n = 25) | Interexaminer (n = 20) | Interevaluator (n = 50) | |
| Arterial outer diameter | 0.964 | 0.944 | 0.959 |
| Arterial inner diameter | 0.969 | 0.948 | 0.972 |
| Venous outer diameter | 0.977 | 0.958 | 0.980 |
| Venous inner diameter | 0.982 | 0.961 | 0.978 |
Mean outer and inner artery and vein diameters were calculated from the 4 largest arteries and 4 largest veins identified. Mean arterial and venous outer diameter was 122.5 ± 10.9 μm (range: 93.3-172.6 μm) and 141.0 ± 13.1 μm (range: 110.3-183.5 μm), respectively, and mean inner arterial and venous diameters were 87.8 ± 9.4 μm (range: 65.3-143.4 μm) and 113.7 ± 12.5 (range: 78.8-148.5 μm), respectively. Mean vessel calibers of arteries and veins in zone B (0.5-1 disc diameter from the optic disc margin), as measured on fundus photographs, averaged 102.9 ± 12.0 μm (range: 76.2-158.9 μm) and 123.3 ± 17.1 μm (range: 59.2-169.7 μm), respectively. Table 3 shows the correlation between mean vessel diameter, as measured on OCT scans, and mean vessel caliber, as measured on fundus photographs. Images from 50 randomly selected healthy subjects were used. Optical coherence tomography measurements of vessel diameter were done in the plane vertical to the retinal surface, but fundus photograph measurements were made in the coronal plane. Although these disparate methods measured vessel diameter in different planes, OCT and fundus photograph measurements correlated well for both arterial and venous diameter/caliber measurements.
| r | P Value | |
|---|---|---|
| Mean arterial outer diameter | 0.286 | .044 |
| Mean arterial inner diameter | 0.395 | .005 |
| Mean venous outer diameter | 0.450 | .001 |
| Mean venous inner diameter | 0.455 | .001 |
As described above, vessel wall thickness was calculated from outer and inner vessel diameter measurements. Mean wall thickness was 17.4 ± 2.4 μm (range: 10.3-23.0 μm) in arteries and 13.7 ± 2.1 μm (range: 10.1-21.8 μm) in veins. Additionally, arterial walls generally had a higher reflectivity than venous walls, and arterial walls were significantly thicker than venous walls ( P < .001). The arterial wall–to-lumen ratio was 0.396 ± 0.16 (range: 0.203-0.592).
Using measurements from healthy eyes of subjects with no systemic disease, age-dependent changes in vessels were evaluated ( Figure 2 ). Although mean venous outer and inner diameters were not affected by subject age, mean wall thickness significantly increased with age (r = 0.455, P < .001). Mean arterial inner diameter was also not significantly affected by subject age, but mean outer diameter (r = 0.384, P < .001) and vessel thickness (r = 0.612, P < .001) progressively increased with age. Subjects were then divided into older (≥50 years) and younger (<50 years) groups ( Table 4 ). Arterial outer diameter, arterial wall thickness, arterial wall–to-lumen ratio, and venous wall thickness were significantly greater in older subjects than in younger subjects ( Figure 3 ). Vessel walls were 17% and 22% thicker in veins and arteries, respectively, in older subjects compared with younger subjects.
| <50 Years (n = 35 Eyes) | ≥50 Years (n = 97 Eyes) | P Value | |
|---|---|---|---|
| Age (y, mean ± SD, range) | 31.1 ± 7.7 (21-46) | 66.3 ± 9.1 (51-87) | <.001 |
| Sex (male/female) | 16/19 | 53/44 | .340 |
| Vessel measurements (μm, mean ± SD) | |||
| Mean arterial outer diameter | 115.0 ± 11.3 | 122.8 ± 9.1 | <.001 |
| Mean arterial inner diameter | 86.4 ± 8.8 | 87.7 ± 8.2 | .440 |
| Mean arterial wall thickness | 14.3 ± 2.5 | 17.5 ± 2.0 | <.001 |
| Mean venous outer diameter | 136.8 ± 12.3 | 142.0 ± 12.4 | .036 |
| Mean venous inner diameter | 113.5 ± 11.2 | 114.5 ± 12.5 | .667 |
| Mean venous wall thickness | 11.7 ± 2.0 | 13.7 ± 1.8 | <.001 |




