Purpose
To investigate the effectiveness and complications associated with the use of bevacizumab, an anti–vascular endothelial growth factor agent, in the treatment of prethreshold retinopathy of prematurity (ROP).
Design
A multicenter, retrospective case series.
Methods
Data from patients who had received intravitreal bevacizumab (IVB) injections for the treatment of ROP were collected from 4 medical centers in Taiwan. The main outcome measures were the regression of ROP and the complications that were associated with the IVB injections.
Results
In total, 162 eyes from 85 patients were included in the study. After receiving IVB injections, 143 eyes (88%) exhibited ROP regression. Fourteen eyes (9%) required additional laser treatment for ROP regression after the absence of a positive response to the IVB injections. Three eyes (2%) progressed to stage 4 ROP and required vitrectomies to reattach the retinas. Two eyes (1%) received 1 additional IVB injection to decrease persistent plus disease. All of the eyes (100%) had attached retinas after the various treatments that they received. The major ocular complications that were associated with IVB injections included vitreous or preretinal hemorrhage in 2 eyes (1%); cataract in 1 eye (1%); and exotropia in 1 eye (1%). No notable systemic complications related to the IVB injections were observed.
Conclusions
IVB injection seems to be an effective and well-tolerated method of treating prethreshold ROP. Laser therapy may still be required as a backup treatment for patients who do not respond to an IVB injection or for those in whom ROP worsens after an IVB injection.
Retinopathy of prematurity (ROP) remains one of the leading causes of childhood blindness. In later stages of ROP, neovascularization of the retina develops as a result of retinal immaturity. Neovascularization in turn leads to retinal traction, retinal detachment, hemorrhage, and the development of a funnel configuration of the retina, which eventually affects visual function. Neovascularization is driven mainly by vascular endothelial growth factor (VEGF). Currently, the recommended treatment for type 1 ROP is laser ablation in the periphery. The timing of treatment has been moved to an earlier stage of the disease, which was documented by the Early Treatment for Retinopathy of Prematurity Study. Although laser treatment effectively prevents stage 3 ROP from progressing to stage 4 ROP in 90% of patients, ablative laser treatments actually destroy approximately two thirds of the retina, and some patients still progress to retinal detachment despite receiving laser or cryotherapy. Moreover, the functional outcomes in stage 4B or stage 5 ROP still are not satisfactory, even after the patient has been treated with a vitrectomy or scleral buckle. Therefore, a new treatment that could decrease the need for either laser treatment or vitreoretinal surgery is necessary.
Bevacizumab (Avastin; Genentech Inc, San Francisco, California, USA) is a humanized anti-VEGF monoclonal antibody. It is the first antiangiogenic agent to be approved for the treatment of metastatic colorectal cancer. It also has been shown to produce favorable outcomes in the treatment of many retinopathies that are associated with VEGF upregulation, including age-related macular degeneration, diabetic retinopathy, vitreous hemorrhage, neovascular glaucoma, and retinal vascular occlusion. Previous studies have shown that VEGF levels in the vitreous fluid often are highly elevated in ROP patients. These results suggest that bevacizumab is a potential candidate for use in the treatment of ROP.
Previously, Mintz-Hittner and associates published the results of a randomized trial of ROP therapies (Bevacizumab Eliminates the Angiogenic Threat of Retinopathy of Prematurity [BEAT-ROP] study) and found that bevacizumab was effective in the treatment of ROP; it was more effective than laser treatment in zone 1 ROP cases in particular. We also published the results of a multicenter study in Taiwan in which 27 patients (49 eyes) were enrolled. Thus far, however, the number of studies on the use of bevacizumab in the treatment of ROP remains limited. The present study aimed to update the findings of our previous study in Taiwan by including more patients and monitoring those patients for a longer follow-up period. Patients with prethreshold ROP (as defined by criteria that were established in the Early Treatment for Retinopathy of Prematurity Study) who were treated with bevacizumab (patients with stage 4 and stage 5 ROP were excluded) were included in this study. Refraction data, which were collected after the injection of bevacizumab and after the regression of ROP in some patients, were analyzed. Treatment effects, ocular complications, and systemic complications also were analyzed.
Methods
This was a multicenter, retrospective study of the use of bevacizumab in the treatment of patients with ROP. The data were collected from medical centers in 4 cities across Taiwan: the National Taiwan University Hospital in Taipei, the Changhua Christian Hospital in Changhua, the Chang Gung Memorial Hospital in Kaohsiung, and the Chang Gung Memorial Hospital in Taoyuan. The data were collected between January 2006 and February 2011. Data from patients with prethreshold ROP (ROP that had not yet reached stage 4 or 5) who were treated with an intravitreal bevacizumab (IVB) injection were collected from each center and were pooled for analysis. The indications for treatment were patients whose retinopathy met the criteria that were established by the Early Treatment for Retinopathy of Prematurity Study. Patients whose disease progression and treatment outcomes were monitored for fewer than 6 months were excluded. Numerical variables are presented as means ± standard deviations.
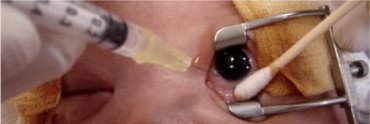
Eyes were prepared in a standard fashion using 5% povidone–iodine and topical antibiotics, after which 0.625 mg (0.025 mL) bevacizumab was injected intravitreally via the pars plicata under intravenous sedation. The injection was performed with a 30-gauge needle that initially was directed along an angle that was perpendicular to the globe and that then was redirected slightly toward the center of the eyeball after the needle had passed the equator of the lens. This technique was used to avoid damaging either the lens or the retina ( Figure 1 ). This technique was different from the technique that we used to perform intravitreal injections in adults. After the injection had been administered, the intraocular pressure and retinal artery perfusion of the injected eye were checked, and patients received topical antibiotics for 7 days. If the patients did not respond positively to the IVB injection or if the ROP worsened, the patients were treated using conventional laser treatment or an additional IVB injection. A positive response included the disappearance of the tunica vasculosa lentis, pupil dilation, the disappearance of or a decrease in retinal vessel tortuosity and neovascularization, and the presence of vessels that continued to vascularize toward the peripheral retina. The worsening of ROP was defined as follows: the reappearance of plus disease, the persistence or reappearance of neovascularization arising from the retinal vessels, and progression to retinal detachment. All of these conditions required retreatment. After treatment, patients were monitored every 1 or 2 weeks until full vascularization of the retina was observed. Full vascularization was defined as follows: vascularization as far as it would develop without an active component or clinically significant tractional elements. All of the screeners and treating physicians were retina specialists. In certain cases, photographs were obtained before and after the injection of bevacizumab using the RetCam Imaging System (Clarity Medical System, Pleasanton, California, USA). In some patients, examinations were performed under anesthesia after the IVB injection. In these examinations, intraocular pressure, corneal size, and axial length were measured, and slit-lamp ophthalmoscopy, indirect ophthalmoscopy, and cycloplegic refraction were performed. The cycloplegic agent that was used was either 1% cyclopentolate or 1% tropicamide.
Results
The current study is an extension of a prior study that enrolled more patients and involved a longer follow-up period. The patients with prethreshold disease (excluding stage 4 and 5 ROP) who had received an IVB injection in the prior study (41 eyes of 23 patients) were pooled together with the 121 eyes of 62 new patients in the current study for the outcome analysis. In total, 162 eyes from 85 patients (57 male and 28 female) were included in the study. Data were collected from 15 patients from the National Taiwan University Hospital in Taipei, 14 patients from the Changhua Christian Hospital in Changhua, 23 patients from the Chang Gung Memorial Hospital in Kaohsiung, and 33 patients from the Chang Gung Memorial Hospital in Taoyuan. The mean gestational age and birth weight of the entire cohort were 26.3 ± 2.6 weeks and 930.1 ± 359.3 g, respectively. All of the treated eyes had prethreshold ROP without retinal detachment.
Among the treated eyes, 160 eyes had stage 3 ROP (99%), and 2 eyes (1%) had stage 2 ROP. In addition, 17 eyes (10%) had zone 1 ROP, and 145 eyes (90%) had zone 2 ROP. Among the eyes with stage 2 or 3 ROP, bevacizumab was used as the primary treatment for ROP in 147 eyes (91%), and it was used as a salvage treatment in 15 eyes (9%) after a lack of response to prior laser treatment. Patients who had undergone previous laser treatment had undergone either 1 or 2 treatment sessions (4 eyes [27%] had undergone 2 laser treatment sessions, and 11 [73%] eyes had been treated only once). Among eyes with prethreshold ROP, the mean age at injection was 36.6 ± 3.2weeks postmenstrual age (PMA). One to 3 days after the injection, the tunica vasculosa lentis had diminished, and pupil dilation was noted. Decreased vessel tortuosity was observed in most eyes within 1 week of receiving an IVB injection. The regression of neovascularization took anywhere from several weeks to months. After the regression of neovascularization, the continuation of normal vascularization toward the periphery of the retina could be observed. Of the 162 eyes, the use of bevacizumab in the treatment of ROP resulted in the regression of ROP after a single IVB injection in 143 eyes (88%; Figure 2 ). Additional laser treatment was required to regress ROP in 14 eyes (9%), in which either no positive response to IVB injection or worsening of the ROP was observed. The additional laser treatment occurred at a mean age of PMA 40 ± 2.8 weeks (range, 36 to 44 weeks PMA). The average time between laser treatment and IVB injection was 6 ± 3.4 weeks. Three eyes (2%) progressed to stage 4 ROP and required vitrectomies to reattach the retinas. The time to vitrectomy was 35, 41, and 69 weeks PMA in these 3 eyes. Two eyes (1%) received 1 additional IVB injection at 39 and 41 weeks PMA to decrease persistent plus disease. If we pooled all of the cases with a worsening of ROP after IVB, the average time between retreatment (including laser, vitrectomy, additional IVB injection) and initial IVB injection was 7.6 ± 9.4 weeks. On average, patients were monitored for 13.7 ± 5.8 months. All of the eyes (100%) had attached retinas at the final follow-up appointments.
Examinations under anesthesia were performed on 28 patients (33%). All of the eyes had normal intraocular pressure, corneal size, and clear media, except one, who had a cataract. Refraction data were available in 53 eyes from 28 patients with regressed ROP after receiving an IVB injection. The mean spherical power was 0.8 ± 2.6 diopters (D; range, −6.3 to 7.3 D), the mean cylindrical power was −2.1 ± 1.1 D (range, −5.3 to −0.3 D), and the mean axial length was 20.7 mm (range, 19.8 to 22.3 mm). The mean spherical equivalent of refractive error among these patients was −0.1 ± 1.8 D (range, −8.75 to 6.55 D). Only 4 eyes (8%) had spherical equivalents that were more severe than −5 D. Most eyes (42/53; 79%) had with-the-rule astigmatism. The mean age at examination was 17.8 ± 7.6 months (range, 8 to 35 months).
Major ocular complications that were associated with IVB injection included vitreous or preretinal hemorrhage, which occurred in 2 eyes (1%); cataract, which occurred in 1 eye (1%); and exotropia, which occurred in 1 eye (1%). Vitreous or preretinal hemorrhage eventually resolved in all of the eyes. The cause of cataract in 1 patient was not related to the trauma caused during the intravitreal injection. That patient underwent cataract surgery at the age of 19 months. No notable systemic complications that were related to the IVB injection were observed during the follow-up period.
Results
The current study is an extension of a prior study that enrolled more patients and involved a longer follow-up period. The patients with prethreshold disease (excluding stage 4 and 5 ROP) who had received an IVB injection in the prior study (41 eyes of 23 patients) were pooled together with the 121 eyes of 62 new patients in the current study for the outcome analysis. In total, 162 eyes from 85 patients (57 male and 28 female) were included in the study. Data were collected from 15 patients from the National Taiwan University Hospital in Taipei, 14 patients from the Changhua Christian Hospital in Changhua, 23 patients from the Chang Gung Memorial Hospital in Kaohsiung, and 33 patients from the Chang Gung Memorial Hospital in Taoyuan. The mean gestational age and birth weight of the entire cohort were 26.3 ± 2.6 weeks and 930.1 ± 359.3 g, respectively. All of the treated eyes had prethreshold ROP without retinal detachment.
Among the treated eyes, 160 eyes had stage 3 ROP (99%), and 2 eyes (1%) had stage 2 ROP. In addition, 17 eyes (10%) had zone 1 ROP, and 145 eyes (90%) had zone 2 ROP. Among the eyes with stage 2 or 3 ROP, bevacizumab was used as the primary treatment for ROP in 147 eyes (91%), and it was used as a salvage treatment in 15 eyes (9%) after a lack of response to prior laser treatment. Patients who had undergone previous laser treatment had undergone either 1 or 2 treatment sessions (4 eyes [27%] had undergone 2 laser treatment sessions, and 11 [73%] eyes had been treated only once). Among eyes with prethreshold ROP, the mean age at injection was 36.6 ± 3.2weeks postmenstrual age (PMA). One to 3 days after the injection, the tunica vasculosa lentis had diminished, and pupil dilation was noted. Decreased vessel tortuosity was observed in most eyes within 1 week of receiving an IVB injection. The regression of neovascularization took anywhere from several weeks to months. After the regression of neovascularization, the continuation of normal vascularization toward the periphery of the retina could be observed. Of the 162 eyes, the use of bevacizumab in the treatment of ROP resulted in the regression of ROP after a single IVB injection in 143 eyes (88%; Figure 2 ). Additional laser treatment was required to regress ROP in 14 eyes (9%), in which either no positive response to IVB injection or worsening of the ROP was observed. The additional laser treatment occurred at a mean age of PMA 40 ± 2.8 weeks (range, 36 to 44 weeks PMA). The average time between laser treatment and IVB injection was 6 ± 3.4 weeks. Three eyes (2%) progressed to stage 4 ROP and required vitrectomies to reattach the retinas. The time to vitrectomy was 35, 41, and 69 weeks PMA in these 3 eyes. Two eyes (1%) received 1 additional IVB injection at 39 and 41 weeks PMA to decrease persistent plus disease. If we pooled all of the cases with a worsening of ROP after IVB, the average time between retreatment (including laser, vitrectomy, additional IVB injection) and initial IVB injection was 7.6 ± 9.4 weeks. On average, patients were monitored for 13.7 ± 5.8 months. All of the eyes (100%) had attached retinas at the final follow-up appointments.
Examinations under anesthesia were performed on 28 patients (33%). All of the eyes had normal intraocular pressure, corneal size, and clear media, except one, who had a cataract. Refraction data were available in 53 eyes from 28 patients with regressed ROP after receiving an IVB injection. The mean spherical power was 0.8 ± 2.6 diopters (D; range, −6.3 to 7.3 D), the mean cylindrical power was −2.1 ± 1.1 D (range, −5.3 to −0.3 D), and the mean axial length was 20.7 mm (range, 19.8 to 22.3 mm). The mean spherical equivalent of refractive error among these patients was −0.1 ± 1.8 D (range, −8.75 to 6.55 D). Only 4 eyes (8%) had spherical equivalents that were more severe than −5 D. Most eyes (42/53; 79%) had with-the-rule astigmatism. The mean age at examination was 17.8 ± 7.6 months (range, 8 to 35 months).
Major ocular complications that were associated with IVB injection included vitreous or preretinal hemorrhage, which occurred in 2 eyes (1%); cataract, which occurred in 1 eye (1%); and exotropia, which occurred in 1 eye (1%). Vitreous or preretinal hemorrhage eventually resolved in all of the eyes. The cause of cataract in 1 patient was not related to the trauma caused during the intravitreal injection. That patient underwent cataract surgery at the age of 19 months. No notable systemic complications that were related to the IVB injection were observed during the follow-up period.
Discussion
In this study, we found that using an IVB injection (0.625 mg) as either a primary treatment or salvage treatment after laser therapy resulted in the regression of neovascularization and full vascularization of the retina in 88% of eyes with prethreshold ROP. Nine percent of eyes showed no response to bevacizumab or worsening in the degree of ROP after receiving an IVB injection and required additional laser treatment. In addition, 2% of eyes progressed to stage 4 ROP and required vitrectomies to reattach the retinas; 1% of eyes required a second bevacizumab injection to decrease the plus disease. Ocular complications did occur in some patients (preretinal or vitreous hemorrhage, 1%; cataract, 1%; and exotropia, 1%), but in none of the patients did endophthalmitis or corneal opacities develop that required corneal transplants in the laser treatment arm, as was reported in the BEAT-ROP study. No apparent systemic toxicity that was related to the injection was found between the injection date and the date of the last follow-up examination. These data were consistent with the data in our previous publication. Because VEGF concentrations are highly elevated in advanced ROP and because VEGF has been found to be a driving force for neovascularization, blocking VEGF with anti-VEGF agents, such as bevacizumab, seems to be a reasonable approach to the treatment of ROP. Increasingly, more patients worldwide have received anti-VEGF treatment for ROP, and therefore, data on the effectiveness and complications of this treatment method are urgently needed.
Mintz-Hittner and Kuffel showed that a single injection of bevacizumab prevented progression to retinal detachment in all eyes with posterior zone 1 ROP, even when laser ablation was not necessary. In their recent randomized trial, the BEAT-ROP study, Mintz-Hittner and associates found that compared with conventional laser therapy, there was a significant benefit of IVB monotherapy in infants with stage 3+ retinopathy for zone 1 disease, but not for patients with zone 2 disease. The development of peripheral retinal vessels continued after treatment with IVB, whereas conventional laser therapy led to permanent destruction of the peripheral retina. The results are encouraging, because approximately 27% to 47% of posterior zone 1 patients progress to retinal detachment even with the application of laser ablation in the peripheral retina. In our case series, 17 eyes (10%) with ROP were classified as having zone 1 disease. None of these eyes progressed to retinal detachment after receiving IVB. These results seem to reflect a better outcome after IVB injection as compared with laser treatment in zone 1 ROP patients. Other potential benefits of anti-VEGF therapy relative to ablative treatments include a simpler procedure that requires less time to complete, no need for the special equipment that is required for laser or cryotherapy, a procedure that is less destructive to the retina, the regression of tunica vasculosa lentis and the dilation of pupils (which facilitates subsequent treatments or follow-up examinations easier), and the elimination of various complications that are associated with ablative treatments, such as refractive errors or visual field loss. However, long-term study is necessary to establish the validity of these advantages.
The injection site, depth, and angle that were used in pediatric eyes are different from those that have been used in adult eyes. These modifications seek to avoid damaging either the lens or the retina ( Figure 3 ). The injected volume that is required for treating infants also is much lower than the appropriate volume for adults. Surgeons need to be very familiar with the various injection techniques before applying this treatment to newborns. Infants need to be monitored closely for potential complications that are associated with intravitreal injection, including cataract, endophthalmitis, and retinal detachment, after receiving an IVB injection.




