Purpose
To study the correlation between the visual fields (VF) and wide-field fundus autofluorescence (FAF) in patients with retinitis pigmentosa (RP).
Design
Retrospective, observational, consecutive case series.
Methods
Twenty-four eyes of 12 patients diagnosed with RP were enrolled. The VFs measured by Goldmann perimetry and wide-field FAF images were compared for each eye. The relationship between the areas of hypoautofluorescence on the wide-field FAF images and scotoma on Goldmann perimetry were evaluated. The VF and FAF images in the central 60 degrees were trimmed and superimposed to calculate the percentage agreement between the hypoautofluorescence and the scotomas and between the isoautofluorescence and hyperautofluorescence and the remaining VFs.
Results
The areas of hypoautofluorescence on the FAF images were correlated significantly (R = 0.86, P < .001) with the areas of the VF defects on Goldmann perimetry. The mean percentage agreement between the hypoautofluorescence and the scotomas was 91.0% ± 7.7% and that of the isoautofluorescence and hyperautofluorescence with the remaining VFs was 84.5% ± 7.4%. The areas of geographic hypoautofluorescence with or without hyperautofluorescent bands reflected the VF defects, while nummular or mottled hypoautofluorescence without VF defects was seen in 7 eyes.
Conclusions
These results suggested that wide-field FAF imaging is useful to evaluate the remaining retinal function in patients with RP. Abnormal fundus autofluorescence precedes loss of retinal function and is helpful for monitoring disease progression.
Retinitis pigmentosa (RP), a progressive, degenerative disorder with a worldwide prevalence of about 1.5 million affected persons, is one of the main causes of acquired blindness in developed countries. Nyctalopia is usually the first sign of RP, followed by concentric visual field (VF) defects and, in advanced cases, central visual loss. The pathogenesis may involve functional impairment of the photoreceptors and retinal pigment epithelium (RPE) and concomitant cell death. There are no clinically available treatments for RP that stop the progression of VF defects or recover vision.
While electroretinography (ERG), fluorescein angiography (FA), and fundus examinations are essential for diagnosing RP, VF tests such as Goldmann perimetry and visual acuity tests have been used conventionally to assess retinal function and disease progression. However, VF tests are subjective and potentially affected by various factors such as patient understanding and attention and investigator skill. Goldmann perimetry is time consuming and can impair patient awareness. VF testing in patients with RP is significantly less reproducible than that in healthy subjects. In contrast, ERG provides objective results of retinal function. However, multifocal ERG has not yet been used for the entire retina, while full-field ERG is often nonrecordable.
Recently, optical coherence tomography (OCT) and fundus autofluorescence (FAF) imaging have been introduced as objective tools to observe microstructural changes such as loss of the photoreceptor and RPE cells associated with visual function. Recent studies have identified a relationship between the abnormal hyperautofluorescence seen on FAF and disruption of the inner and outer segment borderline (IS/OS line) on OCT images. However, conventional FAF imaging and OCT provide significant functional and/or structural information only for the posterior pole of the retina.
More recently, the Optos 200Tx imaging system (Optos, Dunfermline, Scotland) was introduced as a new device to achieve a 200-degree-wide fundus view with 1 image capture in 0.25 second. Previous studies have reported that the ultra-wide-field FA by Optos was more useful for detecting capillary nonperfusion in patients with diabetic retinopathy, uveitis, or branch retinal vein occlusion compared with the panoramic photographs of conventional FA. FAF imaging, FA, and fundus imaging are possible using the Optos instrument.
The goal of this study was to compare wide-field FAF imaging measured with the Optos imaging system and Goldmann perimetry in patients with RP and to evaluate the usefulness of wide-field FAF as an objective technique to monitor the progression of RP.
Patients and Methods
Ethical Review Board approval from Nagoya City University Graduate School of Medical Sciences was retrospectively obtained for this study. This clinical trial is registered in UMIN-CTR (UMIN-ID: UMIN000012558). Patient data in a single hospital were reviewed for this retrospective, observational, consecutive case series. We studied patients with a clinical diagnosis of RP who were referred to Nagoya City University between April 1, 2011 and December 31, 2012. All subjects underwent a slit-lamp examination and fundus photography and, if not performed in other clinics, full-field ERG and FA. The diagnosis of RP was established based on the fundus examination, full-field ERG, and FA. Thirty-six eyes of 18 patients were studied. Eyes were excluded if any factors impaired the resolution of FAF and the reliability of the Goldmann perimetry results, such as dense cataracts, nystagmus, and poor fixation attributable to central visual loss. Goldmann perimetry and wide-field FAF imaging were performed using the Optos imaging system.
Goldmann Perimetry
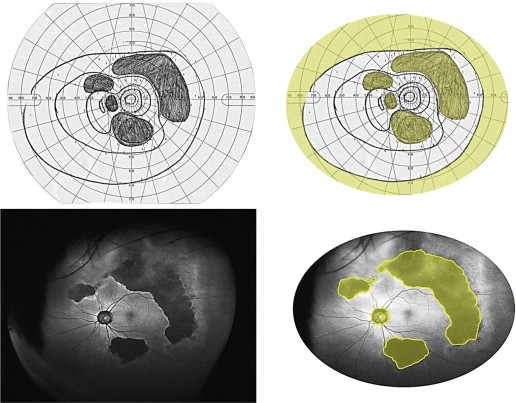
Goldmann perimetry (Haag-Streit, Bern, Switzerland) was performed with the test targets V4e, I4e, I2e, and I1e. The Goldmann perimetry charts were scanned, digitized, and registered using Image J software, version 1.42 (National Institutes of Health, Bethesda, Maryland, USA).
The VFs measured with Goldmann perimetry ( Figure 1 ) were trimmed and evaluated within the area of 60 degrees superiorly, 70 degrees inferiorly, 90 degrees temporally, and 70 degrees nasally, which was considered to be the normal width of the VF in healthy subjects. Scotomatous areas in this VF were calculated manually. In the current study, the most peripheral of the above-mentioned VF was not evaluated because of unstable reproducibility and possible eyelid interference. We defined all defects of the V4e isopter and scotoma of the I4e isopter within the defined area as VF defects.