Purpose
To measure the sparkle of the human eye evaluated by the intensity of corneal light reflection in normal subjects and dry eye patients to investigate whether ocular surface wetness has an impact on the sparkle of the eye.
Design
Prospective case-control study.
Methods
We examined a consecutive series of eight dry eye patients with Sjögren syndrome (SS, 15 eyes), as well as eight normal subjects (16 eyes). The specular corneal surface light reflection was quantitatively measured with an ophthalmic slit-lamp microscope and image capturing system under fixed conditions of light source, incident angle, and detector sensitivity. The intensity of images from subjects’ corneal light reflection was quantified with image analysis software along with the measurement of grade of self-reported brilliancy of the eye, corneal fluorescein staining score, tear film break-up time, and Schirmer test value. The intensity of corneal light reflection was also compared before and after dry eye treatment.
Results
The mean intensity of corneal light reflection was significantly lower in dry eye patients (125.0 ± 40.1) than normal subjects (167.6 ± 36.6, P = .004). Grade of self-reported brilliancy of the eye, corneal fluorescein staining scores, tear film break-up time, and Schirmer test values showed good correlation to the intensity of corneal light reflection. After punctal plug treatment, the intensity of corneal light reflection significantly increased from 125.0 ± 40.1 to 167.2 ± 45.0 ( P < .0001).
Conclusions
The intensity of corneal light reflection representing the sparkle of the eye was significantly more intense in normal subjects compared to dry eye patients, and was increased after punctal plug treatment. The intensity of corneal light reflection appeared to correlate well with tear film stability, volume, and ocular surface desiccation. We showed that tears contributed not only to ocular surface wetness but also to the extent of the light reflection from the eye.
The first image-forming eye appeared around 543 million years ago. From that time, the eye has seen and has been looked at. The eyes are the most expressive part of the human face. The eyes have been called the gateway to one’s soul. Therefore, to have a sparkle in one’s eye is often found to be attractive to others. Wooing people with heart-felt compliments like “Your eyes are sparkling tonight” or “I’m drowning in the pools of light in your eyes” is common, and Ingrid Bergman’s eyes in “Casablanca” stole the hearts of many people.
Although the mechanism of the generation of the sparkle of the eye is still not fully understood, it is possible that pooling of tear over the ocular surface may be associated with increased light reflection from the cornea. Under daily situations the major observable reflections from the eye are Purkinje-Sanson (PS) images. PS I image comprises approximately 97% brightness of all PS images. This is why PS I image has long been employed in the ophthalmic examinations of the anterior segment and cornea using techniques such as Krimsky test, Hirschberg test, keratometry, and corneal topography. Thus, the sparkle of the eye could be assessed by measuring the corneal light reflection, that is, by visualization of the PS I images.
This PS I image has been considered to be generated at the corneal surface. However, the human corneal surface is actually covered by the tear film. Tears are secreted from the lacrimal gland to provide a smooth optical surface, nutrition to the ocular surface epithelium, and a first line of defense against infections. Tears are also distributed over the ocular surface by each eyelid blink to provide wetness. In human visual optics, the refractive indices change most at the air–tear film interface, which affects light refraction and also light reflection. Thus, PS I image is actually generated in the reflection at the surface of the tear film.
In general, the intensity of light reflected from surfaces is dependent on factors like refractive index difference at the interface, smoothness, and wetness of the surface. In the human eye, dry eye disease results in abnormalities of ocular surface smoothness and wetness. Recent dry eye research further revealed corneal surface irregularity and impaired visual function in dry eye states. Thus, we hypothesized that desiccation caused by dry eye disease can lead to a decrease in corneal light reflection, resulting in the reduction of the sparkle of the eye.
In the present study, the intensity of corneal light reflection in normal subjects and dry eye patients was quantitatively measured to investigate whether ocular surface wetness has an impact on the sparkle of the eye.
Methods
Quantification of the Intensity of Corneal Light Reflection
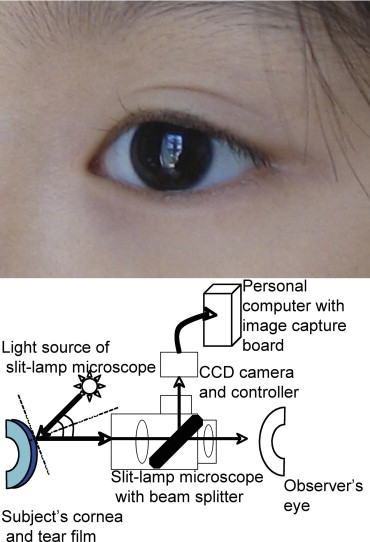
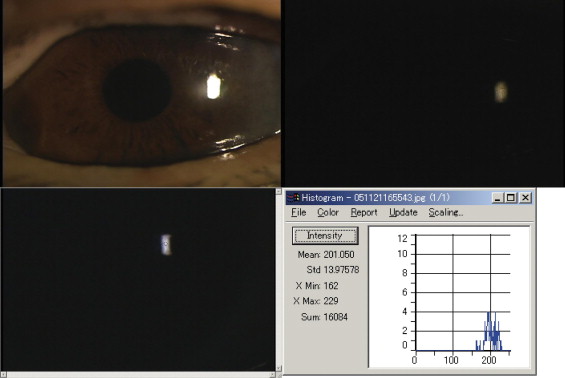
The corneal light reflection ( Figure 1 , Top) was quantitatively measured in a dark room with no other sources of light using an ophthalmic slit-lamp microscope (SL130; Zeiss, Oberkochen, Germany, magnification fixed to 12.72×) attached with a CCD camera (SP-321; JFC Sales Plan Co, Tokyo, Japan) and a digital image capturing system (P4m/MaxFile; P4 Medic Co, Kobe, Japan). The slit-lamp microscope with a fixed light source intensity and with a fixed angle of incidence (22.5 degrees) was set to record the image of the specular corneal surface light reflection ( Figure 1 , Bottom). The light source intensity was decreased and fixed to a minimum so that the images were not oversaturated by light ( Figure 2 , Top left to top right). The sensitivity of the CCD camera was also fixed using constant aperture and gain setting during all examinations. The current image-capturing system was calibrated using the luminance power meter (ADCE 8230E; Advantest, Tokyo, Japan) with acceptable reproducibility. The uniformity of the light source intensity, room illumination, and detector sensitivity were checked each time the measurements were performed. After capturing the RGB (red, green, blue) image of the corneal light reflection, the intensity of corneal light reflection in the central area of the image (diameter 10 pixels) was quantified in the range of 0 to 255 using image analysis software (ImagePro; Mediacybernetics, Silver Spring, Maryland, USA) by the RGB-HIS (hue, intensity, saturation) conversion function ( Figure 2 , Bottom left and bottom right). The mean value of intensity histogram was used for the analysis. Briefly, in the RGB color system, black color corresponds to (0, 0, 0) and white color corresponds to (255, 255, 255). The rest of the colors are produced with each red, green, blue value in the additive color mixing. After the conversion from RGB system to HIS system, darkest intensity corresponds to intensity value 0 and brightest intensity corresponds to intensity value 255. The images of the intensity of corneal light reflection were captured three seconds after the natural blinking in all subjects. None of the subjects received any eye drop instillations at least six hours before the measurements. All the examinations were performed early in the afternoon at the same room temperature (25°C) and humidity (50%).
Participants and Assessment of Tears and Ocular Surface
We examined a consecutive series of eight dry eye patients with Sjögren syndrome (SS, 15 eyes, all female, mean age: 63.5 ± 12.1 years), as well as eight normal subjects (16 eyes, all female, mean age: 65.9 ± 10.9 years). SS patients were diagnosed according to the criteria of Fox and associates. The Japanese dry eye criteria were used for the diagnosis of dry eye. One eye with a history of corneal perforation was excluded from the study. All subjects in this study were female. None of the patients used contact lenses and patients with a history of ocular surgery were also excluded from the study.
The intensity of corneal light reflection was assessed as described above before any invasive procedure. Then, self-reported brilliancy of the eye was graded as follows: grade 1, dull; grade 2, normal brilliancy; grade 3, very brilliant. The corneal epithelial damage was then examined by fluorescein staining. A 2-μL volume of preservative-free solution consisting of 1% fluorescein dye was applied to the conjunctival sac. The intensity of fluorescein staining of the cornea was rated from a minimum of 0 points to a maximum of 3 points, in each upper, middle, and lower cornea. Thus, the maximum total staining score was 9 points. Tear film stability assessed by tear film break-up time (TBUT) was measured three times, and the measurements were averaged. Tear secretion volume was then measured by Schirmer-I test. The intensity of corneal light reflection, as well as other tests, was compared between dry eye subjects and normal controls.
Change of the Intensity of Corneal Light Reflection After Punctal Plug Insertion
All dry eye patients received treatment with nonpreserved artificial tears and 0.1% nonpreserved hyaluronic acid eye drops as necessary for at least one month. All dry eye subjects were refractory to this treatment protocol and underwent punctal plug insertion (Flex plugs, Eagle Vision, Memphis, Tennessee, USA) for both upper and lower puncta. The intensity of corneal light reflection was compared before and three weeks after punctal plug insertion with the above dry eye examinations. No auto-extrusion of the punctal plugs was observed during the study period.
Statistical Analysis
All data are shown as mean ± standard deviation. The Mann-Whitney test was applied to the comparisons of the intensity of corneal light reflection, grade of self-reported brilliancy of the eye, fluorescein staining score, TBUT, and Schirmer test value between dry eye and normal subjects. Linear regression analysis was applied to test the correlations of the intensity of corneal light reflection between grade of self-reported brilliancy of the eye, fluorescein staining score, TBUT, and Schirmer test value. Wilcoxon matched pairs test was applied to the comparisons before and after punctal plug treatment. A level of P < .05 was accepted as statistically significant. Graphpad Instat 3.0 (Graphpad Software, Inc, San Diego, California, USA) was used for statistical analysis.
Results
The mean intensity value of corneal light reflection in normal subjects was significantly more intense (167.6 ± 36.6) compared to dry eye patients (125.0 ± 40.1, P = .004, Table 1 ). Representative cases are shown in Figure 3 (Top and middle). The mean grade of self-reported brilliancy of the eye was significantly higher in normal subjects (2.4 ± 0.7) compared to dry eye patients (1.1 ± 0.4, P = .0001). The mean corneal fluorescein staining score was significantly lower (0.1 ± 0.3) in normal subjects compared to dry eye patients (4.9 ± 2.1, P < .0001). Similarly, TBUT in normal subjects was significantly longer (7.1 ± 2.1 seconds) than in dry eye patients (0.9 ± 0.8 seconds, P < .0001). Schirmer test value was 9.6 ± 10.8 mm in normal subjects, and was significantly higher than in dry eye patients (1.7 ± 1.1 mm, P = .001).
| Intensity of Corneal Light Reflection (0–255) | Grade of Self-Reported Brilliancy of the Eye (1–3) | Fluorescein Staining Score (0–9) | TBUT (sec) | Schirmer Test Value (mm) | |
|---|---|---|---|---|---|
| NL | 167.6 ± 36.6 | 2.4 ± 0.7 | 0.1 ± 0.3 | 7.1 ± 2.1 | 9.6 ± 10.8 |
| Dry eye | 125.0 ± 40.1 | 1.1 ± 0.4 | 4.9 ± 2.1 | 0.9 ± 0.8 | 1.7 ± 1.1 |
| P | .004 | .0001 | <.0001 | <.0001 | .001 |
| r a | NA | 0.69 | −0.44 | 0.49 | 0.51 |
| P ′ a | NA | <.0001 | .01 | .005 | .004 |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


