Purpose
To report the first use of in vitro fertilization (IVF) and preimplantation genetic diagnosis to achieve an unaffected pregnancy in an autosomal-recessive retinal dystrophy.
Design
Case report.
Methods
An affected male with Stargardt disease and his carrier wife underwent IVF. Embryos obtained by intracytoplasmic sperm injection underwent single-cell DNA testing via polymerase chain reaction and restriction enzyme analysis to detect the presence of ABCA4 mutant alleles. Embryos were diagnosed as being either affected by or carriers for Stargardt disease. A single carrier embryo was implanted.
Results
Chorionic villus sampling performed during the first trimester verified that the fetus possessed only 1 mutant paternal allele and 1 normal maternal allele, thus making her an unaffected carrier of the disease. A healthy, live-born female was delivered.
Conclusion
IVF and preimplantation genetic diagnosis can assist couples with an affected spouse and a carrier spouse with recessive retinal dystrophies to have an unaffected child.
Stargardt disease is the most common type of hereditary recessive macular dystrophy. The estimated incidence for the disease is 1 in 10 000 live births, and it characteristically presents in juveniles and young adults. Patients begin to experience a bilateral, gradual decline in their vision between the ages of 6 and 20 years, and can present with visual acuity ranging from 20/20 to 20/200. Their prior visual acuity is often normal, though their final acuity is often 20/200 or worse.
Stargardt disease, similar to age-related macular degeneration (AMD), causes central visual impairment. Though the clinical picture is highly variable, some characteristics can include the presence of orange-yellow flecks distributed around the macula and the mid-retinal periphery and localized to the retinal pigment epithelium (RPE) on fundus photography. These changes may not be visible on initial presentation, however, as the first sign can often be disappearance of the foveolar reflex. Later stages can include an area of atrophic RPE ranging from 2 disc diameters horizontally to 1.5 disc diameters vertically in the macula, giving the appearance of “bull’s eye” maculopathy.
Stargardt disease is caused by mutations in the photoreceptor-specific ABCA4 (formerly known as ABCR ) gene on human chromosome 1p13-p21 (STGD1). Variants in this gene have also been linked to the development of autosomal-recessive cone-rod dystrophy and retinitis pigmentosa. Over 500 disease-associated alleles have been identified, with exceptional allelic heterogeneity, making genetic analysis of the disease challenging. Conventional mutation detection techniques have been able to detect only 25% to 60% of all expected mutations, while direct sequencing could identify 66% to 80%. A study by Jaakson and associates demonstrated the benefits of using an ABCR400 genotyping microarray, which was shown to be over 99% effective in screening for all known ABCR gene mutations and was able to detect approximately 70% to 75% of all expected mutations.
Preimplantation genetic diagnosis (PGD) is a technique introduced in the early 1990s that involves analysis of embryos created in vitro for genetic defects and only implanting those embryos that are free of defects. Traditionally, groups with indications for such interventions have included those with high risk of having children with genetic disease who have opted to terminate pregnancies based on prenatal tests, who have had recurrent miscarriages, who have objections to abortion, and/or who have concurrent infertility and those who are being treated with in vitro fertilization (IVF) and in whom low rate of success with this method can be attributed to chromosomal aneuploidies in the embryos. The uses of this technology have expanded, and reports of its successful use in cases of retinoblastoma and X-linked retinoschisis have been published.
Preimplantation genetic diagnosis involves collection of single cells (blastomeres) through biopsies that can be performed on polar bodies, at the cleavage stage, and at the blastocyst stage, which is the latest stage at which the embryo can be biopsied. After cells are obtained, there are several techniques available for DNA analysis. Polymerase chain reaction (PCR) is used to amplify DNA from the polar body or blastomere while fluorescence in situ hybridization (FISH) is used to analyze the chromosomal complement of blastomeres. Embryos without aberrances are then isolated and used for the pregnancy. The first application of this technique was for patients with carriers of an X-linked disease, but advancements in single-cell analysis expanded the technique for use in cases of many monogenic diseases. Here, we present a couple’s experience with preimplantation genetic diagnosis for Stargardt disease, resulting in the successful delivery of a live-born child without the disease. To our knowledge, this is the first report of the application of preimplantation genetic diagnosis in the case of an autosomal-recessive retinal dystrophic disease.
Methods
Patient Description
A 29-year-old man affected with Stargardt disease (visual acuity 20/70 in both eyes, Figures 1 and 2 ) and his 29-year-old wife sought genetic counseling regarding their desire to conceive in the midst of concerns over having an affected child. Although the frequency of disease-causing mutations in the general population is low (approximately 5%), the couple were advised to have genetic testing for the wife. Genetic testing performed on both the patient and his wife confirmed his possession of 2 ABCA4 mutations (c5018+2C>T and c5882G>A). The c5018+2C>T variant is a relatively rare splice site mutation that has been associated with Stargardt disease in at least 2 studies. The c5882G>A substitution, resulting in the G1961E amino acid change, is an extensively characterized and one of the most frequent STGD mutations.
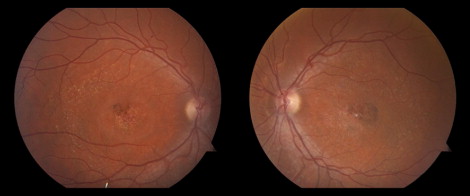
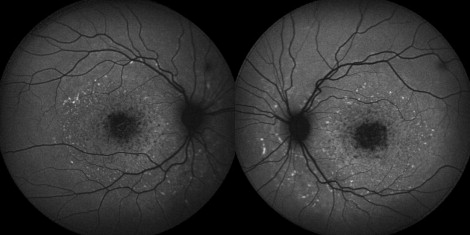
Testing of the wife revealed 1 possibly pathogenic ABCA4 mutation (c455G>A). The c455G>A variant, resulting in R152Q protein change, has been described in at least 3 studies. In 1, the variant was described as a “rare variant” since it was also detected in controls. In the 2 others, it was defined as a disease-causing mutation. This variant exemplifies the difficulty of unambiguous assignment of pathogenicity to very rare ABCA4 missense alleles where supportive evidence, such as segregation with the disease in families and frequency in the general population, is hard, if not impossible, to obtain.
In this particular case, the R152Q variant was considered possibly pathogenic to avoid the potential disease expression in compound heterozygous state. Because the risk of having an affected child was now 50%, the couple was offered and accepted the option of undergoing IVF with PGD.
Mutation Analyses
A blood sample was obtained from the husband, affected with Stargardt disease, and his wife and an ABCA4 mutation screening with ABCR500 chip was performed. Specifically, PCR amplification of the genomic DNA with specific primers for exons 1 through 49, and flanking intronic sequences, followed by purification of PCR products and array-based primer extension with dideoxy terminators was performed, using primers to detect, at that time, 441 known mutations for Stargardt disease. The current array detects 519 mutations (Asper Biotech, Tartu, Estonia). Results showed that she was a carrier of the c455G>A (R152Q) ABCA4 variant. The same testing on the affected husband found 2 Stargardt disease–associated mutations, the splice site–affecting c5018+2C>T mutation and the c5882G>A (G1961E) mutation, thereby confirming the clinical diagnosis of STGD.
For the embryos, DNA obtained from biopsied cells underwent PCR amplification of the genomic DNA with primers for known mutations for Stargardt disease, just as the procedure was performed on blood samples from the parents. Controls included maternal and paternal genomic DNA as well as standard DNA with blanks to demonstrate lack of exogenous DNA contamination of the samples.
The patient’s wife underwent chorionic villus sampling (CVS) at 11 weeks gestation. Direct DNA sequence analysis was performed on the sample to test for mutations in exons 5, 35, and 42 of the ABCA4 gene. The Amplistr Identifiler kit (Applied Biosystems, Life Technologies Corp., Foster City, California, USA) was used to compare 16 microsatellite markers in the maternal DNA with the chorionic villus sample in order to evaluate for maternal DNA contamination of the CVS sample. Results demonstrated that the fetus was a carrier for Stargardt disease, as expected, possessing only the paternal c5018+2C>T mutation.
In Vitro Fertilization and Embryo Biopsy
The experimental nature of the procedure was discussed with the couple, who agreed verbally and in writing that they wished to complete the procedure in order to reduce the risk of their fetus’ having Stargardt disease. Controlled ovarian stimulation was carried out using 1 mg/d of leuprolide acetate initiated in the mid-luteal phase. Injectable gonadotropins (follicle-stimulating hormone [FSH] and human menopausal gonadotropin [hmG]) were administered in a 2:1 dosing ratio starting on day 3 of the ensuing period, with a concurrent halving of the leuprolide acetate dose to 0.5 mg/d. Results of the methods described above for oocyte retrieval, fertilization, and biopsy of embryos are presented in the Table . This cycle yielded 17 oocytes, 16 of which were fertilized by intracytoplasmic sperm injection (ICSI). Of these, 15 were biopsied, with 6 demonstrating 1 maternal and 1 paternal mutant allele and thus labeled as affected with Stargardt disease. For 3 of the 15, molecular data were inconclusive, leaving 6 that were identified as having normal (unaffected) maternal alleles. Of these 6, 2 were cryopreserved, 3 were discarded, and 1 was transferred into the uterus on day 5, resulting in a singleton pregnancy.



