Purpose
To examine the risk of age-related macular degeneration (AMD) with oral bisphosphonates.
Design
Three study designs were used: (1) disproportionality analysis; (2) case-control study; (3) self-controlled case series (SCCS).
Methods
setting : (1) Food and Drug Administration (FDA) Adverse Event Reporting System (FAERS) Database; (2) 2 patient cohorts from British Columbia, Canada. study population : (1) All reports of AMD to the FDA with oral bisphosphoantes; (2) patients with wet AMD in British Columbia (2009–2013) and 1 million controls (2000–2007). intervention : Oral bisphosphonates. main outcome measures : (1) Reports of AMD to the FDA; (2) first diagnosis of wet AMD verified by a retina specialist in British Columbia.
Results
In the disproportionality analysis there were 133 cases of AMD reported with alendronate, 20 with ibandronate, and 14 with risedronate. The reported odds ratios (RORs) for alendronate, ibandronate, and risedronate were 3.82 (95% CI: 2.94–4.96), 2.40 (95% CI: 1.49–3.86), and 2.87 (95% CI: 1.58–5.19), respectively. In the case-control analysis there were 6367 cases and 6370 corresponding controls. The adjusted OR for wet AMD among regular users of bisphosphonates in the 1, 2, and 3 years prior to the index date were 1.24 (1.12–1.38), 1.38 (1.22–1.56), and 1.59 (1.38–1.82), respectively. In the SCCS analysis there were 198 cases of wet AMD on continuous bisphosphonate therapy. The rate ratio for wet AMD for continuous bisphosphonate use was 1.99 (95% CI: 1.41–2.79). We did not have information on intravenous bisphosphonates.
Conclusions
Continuous users of oral bisphosphonates are at a higher risk of developing wet AMD. Given the observational nature of this study and limitation of the data, future studies are needed to confirm these findings.
Bisphosphonates are one of the most prescribed classes of drugs, mainly used for the prevention of osteoporosis. They are complex molecules with proinflammatory properties, which might explain the mechanism behind some of their adverse events. For example, zolendronic acid, an intravenous bisphosphonate, has been linked to both early and delayed flu-like symptoms owing to the release of inflammatory mediators such as interleukins, cytokines, and C-reactive proteins (CRPs). Similarly, oral and intravenous bisphosphonates have been shown to increase the risk of ocular inflammatory conditions such as scleritis, uveitis, and optic neuritis. A case-control study using the Age-Related Eye Disease Study has shown that CRP, an inflammatory marker associated with coronary artery disease, might also be associated with age-related macular degeneration (AMD) .
Age-related macular degeneration is an incurable disease that continues to be the leading cause of blindness in older adults. There are 2 main types: dry and neovascular (also referred to as wet) AMD. Intravitreal injections of anti–vascular endothelial growth factor (VEGF) are the mainstay treatment for wet AMD. Large epidemiologic studies have identified several risk factors that might be important in the pathology of AMD, including genetics, smoking, and obesity. However, the effects of chronic use of prescription drugs, especially those that can promote inflammation like bisphosphonates, are unknown. We hypothesized that long-term use of oral bisphosphonates can increase the risk of neovascular or wet AMD in older adults and conducted a pharmacoepidemiologic study.
Methods
Setting and Study Population
We used 3 distinct study designs in this study: disproportionality analysis, case-control study, and a self-controlled case series (SCCS).
For the disproportionality analysis we used data from the Food and Drug Administration (FDA) Adverse Event Reporting System (FAERS) database, which captures all spontaneous adverse drug reactions reported to the FDA. Data were available from the fourth quarter of 2004 to the second quarter of 2014.
For the case-control and SCCS studies, we used the British Columbia (BC) Ministry of Health Databases. The databases are composed of health-related information for approximately 4.8 million residents of BC. Specifically, the data capture all hospitalizations through the Discharge Abstract Database, all physician visits through the Medical Services Plan (MSP) data file, and all prescription drugs (including date of dispensation, day supply, and quantity dispensed) through PharmaNet. The BC Provincial Retinal Disease Treatment Program, part of the BC Ministry of Health, provides anti-VEGF therapies (bevacizumab or ranibizumab) to older adults with wet AMD. Data for all AMD patients are recorded by a retina specialist and inputted to a comprehensive database that captures all intravitreal injections, including type of anti-VEGF used and the date of injection from 2009 to 2013. These data have been used in several epidemiologic studies. Ethics approval was obtained from the University of British Columbia Clinical Ethics Board.
Study Design
Disproportionality Analysis
Disproportionality analysis is a signal detection technique that examines the risk of an adverse event with a target drug by comparing the number of cases of the adverse event reported with the drug in question against the number of cases of the same adverse event reported with all other drugs in the database. This technique uses information from adverse drug reaction databases such as the FAERS database. It allows researchers and drug regulatory agencies to screen potential “signals” for adverse drug reactions.
Case-Control Study
Cases were identified as those with the first incidence of wet AMD, defined as the first intravitreal injection of anti-VEGF therapies (mainly bevacizumab or ranibizumab), from 2009 to 2013 in the BC AMD database. This date was deemed the index date. Controls were selected from a smaller subset of the BC Ministry of Health database, which included approximately 1 million subjects who had visited an ophthalmologist in BC from 2000 to 2007. Controls had the same opportunity of being diagnosed for AMD by an ophthalmologist as the cases, thus minimizing detection bias. Controls were selected if they did not have an International Classification of Diseases, ninth revision (ICD-9) code for any retinal disease (362.00) or had not received verteporfin therapy and were alive and at risk of developing AMD at the index date. We matched each case with 10 controls by age, follow-up time, and calendar time to control for prescribing trends.
Self-controlled Case Series
The SCCS is similar to a retrospective cohort study but only analyzes person-time among the cases. Exposed person-time on bisphosphonate therapy (risk period) is compared to the period without bisphosphonate use in the same subject, controlling for time-fixed confounders. Thus the main advantage of the SCCS study is that it eliminates intersubject variability that might lead to bias. In the SCCS design, confounders that change over time, such as age, were modeled in increments of 1-year age bands.
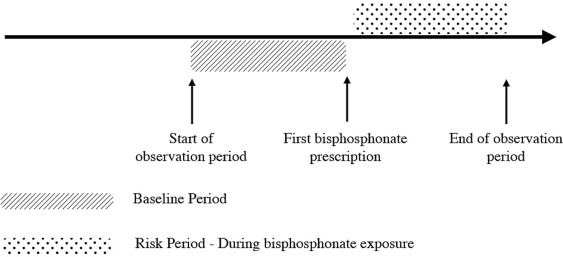
Among the 7752 incident wet AMD patients identified from the BC Ministry of Health Database, we first identified all those with at least 1 prescription of an oral bisphosphonate available in Canada, including alendronate, etidronate, and risedronate. From this cohort we further identified continuous users of a bisphosphonate, defined as an AMD subject with no discontinuation periods longer than 15 days between 2 bisphosphonate prescriptions. Subjects were censored at the time of a prescription termination or the end of the study period. Since the time to onset of AMD with bisphosphonates is unknown, we followed bisphosphonate users to the first AMD injection date to avoid exposure misclassification. The period prior to the first bisphosphonate prescription was designated as the unexposed period ( Figure ) and was thus used as the comparator period.