Purpose
To report 1-year results of reduced-fluence photodynamic therapy (PDT) for polypoidal choroidal vasculopathy (PCV) in Japanese patients.
Design
Prospective interventional case series.
Methods
In the present study, 28 treatment-naïve eyes of 28 consecutive patients underwent PDT with a reduced laser fluence of 25 J/cm 2 . Patients were followed up at baseline and 1 week and 3, 6, 9, and 12 months after PDT. Choroidal perfusion changes were evaluated by indocyanine green angiography (ICGA) and leakage from PCV lesions and exudative changes by fluorescein angiography and optical coherence tomography. Treatment safety was assessed according to visual acuity (VA) and adverse events. The best-corrected VA (BCVA) obtained by Landolt ring tests was converted into the logarithm of the minimal angle of resolution (logMAR).
Results
At baseline, the mean logMAR BCVA was 0.45 (geometric mean: 7/20). At 12 months, the mean logMAR BCVA significantly improved to 0.29 (geometric mean: 10/20) ( P = 0.0001). The logMAR BCVA was stable or improved by ≥0.2 in 26 eyes (93%) at 1-year follow-up. In 10 eyes with VA better than 20/40 at baseline, the mean logMAR BCVA was significantly improved compared with baseline at 12 months. Although 16 of 28 eyes (57%) showed mild to moderate nonperfusion of choriocapillaris in early ICGA at 1 week, 27 eyes (96%) showed recovery to pretreatment levels at 3 months. Mean number of treatment sessions during the 12 months was 1.3. No severe side effects related to treatment were encountered.
Conclusions
Reduced-fluence PDT is an effective treatment for PCV and could improve vision even in eyes with VA better than 20/40.
Verteporfin therapy reduces the risk of vision loss in patients with subfoveal choroidal neovascularization (CNV) in age-related macular degeneration (AMD). The Japanese Age-Related Macular Degeneration Trial (JAT) showed superior efficacy of photodynamic therapy (PDT) for Japanese patients compared with the Treatment of Age-Related Macular Degeneration with Photodynamic Therapy (TAP) study, which mainly investigated Caucasians. Guidelines for the use of verteporfin in Japan demonstrated that verteporfin was effective in maintaining visual acuity (VA) for 12 months for all lesion types, as demonstrated previously in the JAT, and a significant improvement in VA was observed for eyes with polypoidal choroidal vasculopathy (PCV) ( P < .001), the prevalence of which is postulated to be higher in Asian populations than in Caucasians. However, a decline in VA was observed for eyes with VA better than 20/40.
On the other hand, several studies have shown that PDT damages the physiological choriocapillary layer beyond the irradiated area, and repeated PDT leads to persistent choriocapillary nonperfusion in most eyes. Choroidal ischemia consecutively induces a secondary angiogenic response with increased expression of vascular endothelial growth factor (VEGF). The influence of verteporfin therapy on the physiological choroid may be the reason for further vision loss and the need for repeated treatment. The Visudyne in Minimally Classic Choroidal Neovascularization (VIM) Study Group showed there was no difference in the proportion of patients having acute severe vision decrease in the reduced-fluence group as compared with the standard-fluence group. Michels and associates reported that reduced-fluence treatment leads to much less damage of the choriocapillaris when compared to standard-fluence. Thus, since the efficacy of PDT was reported in eyes with PCV, we aimed to study the effect and safety of reduced-fluence PDT for PCV in Japanese patients.
Methods
Twenty-eight eyes of 28 consecutive patients (24 men, 4 women) who had been diagnosed with PCV and had no previous treatment of any type for PCV were enrolled in this prospective study between July 1, 2007 and March 31, 2008. All 28 patients were Japanese and the median patient age was 73.5 years (range, 47–85 years). The prospective interventional case-control study was approved by the Institutional Review Board of Kagawa University Faculty of Medicine.
Patients received verteporfin (Visudyne; Novartis Pharma, Tokyo, Japan) injection at 6 mg/m 2 body surface area over 10 minutes and then underwent PDT with a light fluence of 25 J/cm 2 using a Visulus PDT system 690S (Carl Zeiss Meditec AG, Jena, Germany) 5 minutes after the completion of infusion. The laser spot size was chosen to cover the entire PCV vascular lesions, including the polypoidal lesions and branching vascular network vessels, as shown on indocyanine green angiography (ICGA), plus an extra margin of 1000 μm.
Patients were seen for regular follow-up visits within 7 days before PDT (baseline) and at 1 week and 3, 6, 9, and 12 months after PDT. Best-corrected VA (BCVA) and optical coherence tomography (OCT) using an OCT3000 or Cirrus HD-OCT system (Carl Zeiss Meditec, Dublin, California, USA) were performed at each visit. Fluorescein angiography (FA) using the TRC50IX system with ImageNet2000 (Topcon, Tokyo, Japan) and ICGA using a Heidelberg Retina Angiograph 2 (HRA2) (Heidelberg Engineering GmbH, Heidelberg, Germany) were performed before PDT, and at 1 week and 3 months after PDT. We evaluated choroidal perfusion changes by ICGA, leakage from polypoidal vascular lesions by FA, and exudative changes by OCT. Grading of effect on choriocapillaris was based on a report by Michels and associates.
The PDT endpoint was achieved when complete absence of leakage was seen on FA, or when the absence of exudative changes including pigment epithelial detachment, serous retinal detachment, and retinal edema was seen on OCT. Rendering disappearance of polypoidal vascular lesions on ICGA was unnecessary. Eyes with no exudative changes on OCT were observed rather than treated, even though there was minimal leakage.
Safety of treatment was assessed based on BCVA and adverse events. The BCVA obtained by Landolt ring tests was converted into the logarithm of the minimal angle of resolution (logMAR), with a change of 0.2 or more in logMAR VA considered significant. Improvement in BCVA was defined as an increase of ≥0.2 logMAR units, and worsening in BCVA was defined as a decrease of ≤0.2 logMAR units. For comparison of BCVA outcomes to baseline, the paired t test was used.
Results
Patient characteristics are shown in the Table .
| Case No. | Age | VA | ICGA Findings at Month 3 | Choriocapillary Nonperfusion After PDT a | No. of Treatments | |||
|---|---|---|---|---|---|---|---|---|
| At Baseline | 12 Months | Branching Vascular Network | Polypoidal Vascular Lesions | Week 1 | Month 3 | |||
| 1 | 61 | 20/250 | 20/120 | persistent | disappeared | no | no | 1 |
| 2 | 77 | 20/30 | 20/20 | disappeared | disappeared | not significant | no | 1 |
| 3 | 82 | 20/60 | 20/25 | persistent | disappeared | moderate | no | 1 |
| 4 | 47 | 20/20 | 20/10 | disappeared | disappeared | moderate | no | 1 |
| 5 | 59 | 20/30 | 20/20 | disappeared | disappeared | no | no | 1 |
| 6 | 59 | 20/200 | 20/100 | persistent | disappeared | moderate | no | 1 |
| 7 | 85 | 20/200 | 20/100 | persistent | disappeared | no | no | 1 |
| 8 | 73 | 20/50 | 20/100 | persistent | recurrent | no | no | 3 |
| 9 | 77 | 20/50 | 20/22 | persistent | disappeared | not significant | no | 1 |
| 10 | 75 | 20/40 | 20/60 | persistent | disappeared | moderate | no | 2 |
| 11 | 71 | 20/40 | 20/22 | disappeared | disappeared | moderate | not significant | 2 |
| 12 | 76 | 20/25 | 20/28 | persistent | disappeared | not significant | no | 3 |
| 13 | 84 | 20/200 | 20/200 | persistent | persistent | no | no | 2 |
| 14 | 55 | 20/30 | 20/16 | persistent | disappeared | not significant | no | 1 |
| 15 | 77 | 20/30 | 20/25 | persistent | disappeared | not significant | no | 1 |
| 16 | 71 | 20/40 | 20/30 | persistent | disappeared | no | no | 2 |
| 17 | 64 | 20/28 | 20/30 | persistent | disappeared | no | no | 1 |
| 18 | 77 | 20/40 | 20/25 | persistent | disappeared | not significant | no | 1 |
| 19 | 68 | 20/28 | 20/16 | persistent | disappeared | no | no | 1 |
| 20 | 75 | 20/28 | 20/28 | persistent | disappeared | moderate | no | 1 |
| 21 | 79 | 20/120 | 20/120 | persistent | disappeared | no | no | 1 |
| 22 | 68 | 20/50 | 20/28 | persistent | disappeared | no | no | 1 |
| 23 | 70 | 20/60 | 20/28 | persistent | disappeared | moderate | no | 1 |
| 24 | 83 | 20/60 | 20/28 | persistent | disappeared | no | no | 1 |
| 25 | 78 | 20/50 | 20/22 | persistent | disappeared | moderate | no | 1 |
| 26 | 70 | 20/200 | 20/120 | disappeared | disappeared | no | no | 1 |
| 27 | 71 | 20/100 | 20/50 | persistent | disappeared | moderate | no | 1 |
| 28 | 74 | 20/30 | 20/50 | persistent | disappeared | moderate | no | 2 |
a Based on grading of verteporfin therapy’s effect on the choriocapillaris as documented by indocyanine green angiography.
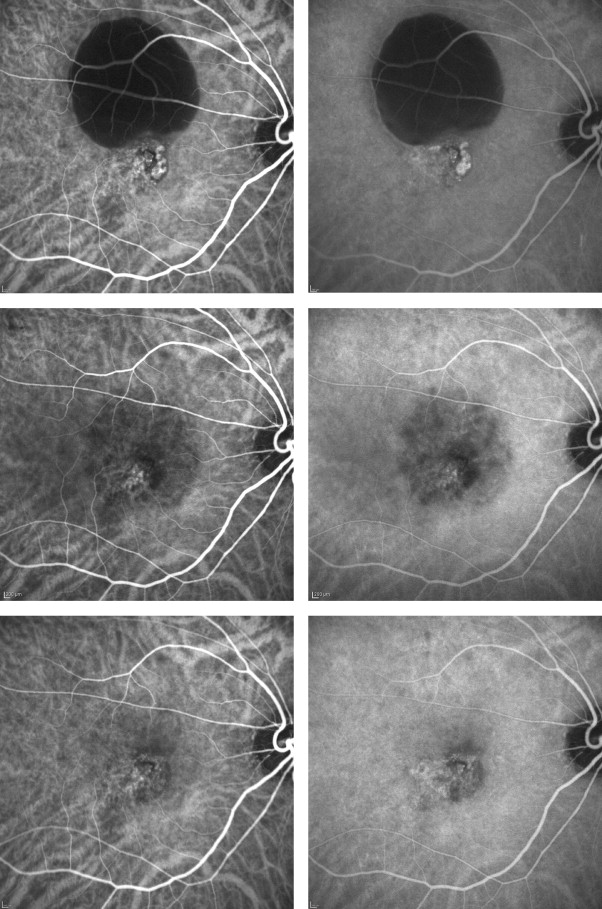
PDT-Induced Choroidal Perfusion Changes
Sixteen of 28 eyes (57%) showed mild (not significant) to moderate nonperfusion of choriocapillaris in early ICGA at 1 week, but 27 of 28 eyes (96%) showed recovery to pretreatment levels at 3 months ( Figure 1 , Table ). Only 1 eye showed mild choriocapillary nonperfusion at 3 months.