Purpose
To determine the association between ocular sun exposure measured by conjunctival ultraviolet (UV) autofluorescence and myopic refractive error in young adults.
Design
Cross-sectional study.
Methods
setting : Population-based cohort in Western Australia. study population : Total of 1344 mostly white subjects aged 19–22 years in the Western Australian Pregnancy Cohort (Raine) Eye Health Study. observation procedures : Cycloplegic autorefraction, conjunctival ultraviolet autofluorescence photography, participant questionnaire. main outcome measures : Prevalence of myopic refractive error (spherical equivalent less than −0.50 diopters) and area of conjunctival ultraviolet autofluorescence in mm 2 .
Results
There was an inverse relationship between myopic refractive error and ocular sun exposure, with more than double the prevalence of myopia in the lowest quartile of conjunctival autofluorescence than the highest quartile (33.0% vs 15.6%). Median area of autofluorescence was significantly lower in myopic than in nonmyopic subjects (31.9 mm 2 vs 47.9 mm 2 , P < .001). These differences remained significant after adjustment for age, sex, parental history of myopia, and subject level of education. The use of corrective lenses did not explain the lower conjunctival autofluorescence observed in myopic subjects.
Conclusions
In this young adult population, myopic refractive error was inversely associated with objectively measured ocular sun exposure, even after adjustment for potential confounders. This further supports the inverse association between outdoor activity and myopia.
Myopia is a major health issue worldwide. It contributes to the burden of uncorrected refractive error, which is a leading cause of visual impairment and a significant economic issue with billions of dollars of lost productivity globally. Low levels of myopia may be corrected with glasses, contact lenses, or refractive surgery; however, high myopia is associated with a substantial risk of potentially blinding ocular pathologies including myopic maculopathy, retinal detachment, glaucoma, and cataract.
Prevalence of myopia is increasing worldwide in many populations, with particularly steeper trajectories in east and southeast Asia. This rise in myopia, with corresponding rise in high myopia, is concurrent with myopigenic activities on a background of increasing urbanization of these populations. One activity underlying this association may be a reduction in time spent outdoors, with a recent meta-analysis revealing a reduction in odds of myopia of 2% for every additional hour spent outdoors per week. The protective effect of outdoor activity has also been demonstrated in prospective studies and a randomized clinical trial.
There are currently no widely used interventions to prevent development of myopia, and interventions proposed to reduce progression of myopia are limited by small effect sizes, rebound myopia, and side effects. If the protective association of increased outdoor time and reduced rates of myopia can be confirmed using objective measures of outdoor exposure, it will provide clear evidence of the need for further interventional trials in this area.
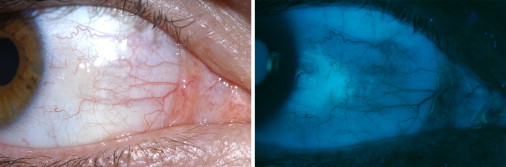
Conjunctival ultraviolet autofluorescence photography is an objective method of assessing ocular sun exposure and correlates strongly with outdoor time. This method avoids the inherent limitations, including subjectivity and recall bias, of measuring outdoor activity using participant recall via questionnaire. Preclinical sun damage on the conjunctiva is known to fluoresce under ultraviolet light, a phenomenon that can be quantified with fixed focal-length photography and digital analysis ( Figure 1 ). Using this technique, an inverse association between conjunctival ultraviolet autofluorescence and myopia was demonstrated in a population cohort from Norfolk Island, although findings were limited by a small sample size, wide age range of participants, and incomplete data on confounding variables. The current study was designed to further investigate the association between conjunctival ultraviolet autofluorescence and myopia in a larger population, and determine whether the association could be explained by confounding factors or the ultraviolet-blocking effect of corrective lenses.
Methods
Participants
This was a population-based cross-sectional study of 1344 participants in the Western Australian Pregnancy Cohort (Raine) Study. Prospective ethical approval was obtained from the Human Research Ethics Committee at the University of Western Australia. The study was conducted in accordance with the tenets of the Declaration of Helsinki and informed consent was obtained from all participants.
The cohort was predominantly of white ethnicity: 90.3% of participants had a white mother, 90.0% had a white father, and for 85.5% of participants both parents were white. Chinese and Indian were the most common nonwhite ethnicities, with small numbers of participants having Indigenous Australian, Torres Strait Islander, Polynesian, or Vietnamese ethnicities. The recruitment and follow-up were performed in Perth, Western Australia, which has a subtropical climate with a latitude of 31°60s south.
Inclusion and exclusion criteria for the initial recruitment of the Raine cohort have been previously published. There were no specific inclusion or exclusion criteria for the 21-year follow-up Raine Eye Health Study. All 2135 active members of the Raine cohort were invited to participate, and of these 1743 (81.6%) agreed to take part in the 21-year follow-up. During the 24-month period from March 2010 to February 2012, 1344 of those 1743 (77.1%) underwent the ophthalmic examination. There was no significant difference in age or sex between those who attended the eye examination and those who did not. Those who attended the eye examination were more likely to be of white ancestry (85.4% vs 80.1%, P < .001).
Conjunctival Ultraviolet Autofluorescence
High-resolution ultraviolet photographs of nasal and temporal conjunctiva were taken using a specially designed camera system. A Nikon D100 (Nikon, Melville, New York, USA) digital camera with 105 mm 147 f/2.8 Micro Nikkor (Nikon, Melville, New York, USA) macro lens was used with an external electronic flash system including ultraviolet transmission filters (transmittance range 300–400 nm, peak 365 nm). The camera, lens, and flash system were mounted on a table with an adjustable subject headrest and joystick-controlled camera positioning assembly. Photographs were taken in a dark room so only ultraviolet fluorescence was recorded by the camera.
Analysis was performed using Adobe Photoshop CS4 Extend (Adobe Systems Inc, San Jose, California, USA). Four photographs were analyzed for each participant (left and right eyes, nasal and temporal conjunctiva). The area of fluorescence in mm 2 for each photograph was determined using Photoshop and added together to produce a total area of fluorescence in mm 2 for each participant.
Myopia and Hypermetropia
Cycloplegic autorefraction was performed using the Nidek ARK-510A (Nidek Co Ltd, Gamagori, Japan) autorefractor. Tropicamide 1% and phenylephrine 10% eye drops were administered for mydriasis. Myopia was defined as spherical equivalent (sum of spherical error and half cylindrical error) less than −0.50 diopters. High myopia was defined as spherical equivalent less than −6.00 diopters. Hypermetropia was defined as spherical equivalent greater than +0.50 diopters. As the correlation between right and left eye spherical equivalent was high (R = 0.955), only right eye spherical equivalent was used in statistical analysis.
Other Variables
Time spent outdoors, level of education (university studies started/completed), parental history of myopia, and use of glasses and contact lenses were determined by questionnaire. Body mass index (BMI) was calculated from height and weight measured at the time of the eye examination.
Statistical Analysis
Total conjunctival ultraviolet autofluorescence was analyzed in quartiles and in increments of 10 mm 2 . Continuous variables were assessed for normality and summarized using mean (standard deviation) or median (interquartile range [IQR]) as appropriate. Differences between categorical variables were assessed with the χ 2 test. Differences between continuous variables were assessed with the Mann-Whitney U test. Trends across categories were assessed using Cuzick’s nonparametric test for trend.
Logistic regression was used to estimate the odds ratio (OR) and 95% confidence interval (95% CI) of myopia. Covariates that were statistically significant ( P < .05) in univariable analyses were included in the multivariable models, in addition to age and sex. Separate multivariable models were constructed containing either total conjunctival ultraviolet autofluorescence or time spent outdoors, owing to the expected collinearity between the 2 covariates. Interaction was evaluated with the likelihood ratio test. All P values were 2-tailed. Statistical analyses were undertaken in Stata 10.1 for Macintosh (Stata-Corp, College Station, Texas, USA; 2009).
Results
Prevalence of Myopia
Of 1344 participants who attended the ophthalmic examination, 13 were excluded owing to absence of cycloplegic autorefraction (refused dilation) and 16 were excluded owing to inadequate or incomplete autofluorescence photographs. Thus, 1315 participants (97.8%) had complete autorefraction and conjunctival ultraviolet autofluorescence data.
Of 1328 participants with compete autorefraction data, mean age was 20.1 years (SD 0.46) and 684 (51.5%) were male. Three hundred eleven participants (23.7%) were myopic (95% CI 21.4–25.9). There was no significant difference between myopia prevalence in male subjects compared with female, 22.7% (95% CI 19.6–25.9) vs 24.6% (95% CI 21.3–28.0), P = .410.
Median conjunctival ultraviolet autofluorescence was lower in myopic subjects than in nonmyopic subjects, 31.9 mm 2 (IQR 10.6–55.9) vs 47.9 mm 2 (IQR 23.2–72.5), P < .001.
Associations With Myopia
Variables associated with myopia are shown in Table 1 . Increasing age, parental myopia, and tertiary education were associated with increased odds of myopia, although owing to the limited age range in the cohort (19–22 years) age only reached statistical significance in the adjusted model. Higher level of conjunctival ultraviolet autofluorescence was associated with decreased odds of myopia, as was participant recall of increased time outdoors during summer and winter. Sex, height, weight, and BMI were not associated with myopia.
| Variable | OR | 95% CI | P |
|---|---|---|---|
| Age (per year) | 1.20 | 0.91–1.60 | .191 |
| Sex (female) | 1.11 | 0.86–1.44 | .410 |
| Parental myopia | |||
| No parents | 1 (ref) | ||
| One parent | 2.17 | 1.57–3.01 | <.001 |
| Both parents | 3.37 | 2.01–5.31 | <.001 |
| Education level | |||
| University started/completed | 1.81 | 1.47–2.39 | <.001 |
| Height (per 10 cm) | 0.94 | 0.82–1.07 | .343 |
| Weight (per 10 kg) | 1.04 | 0.97–1.11 | .296 |
| Body mass index | 1.02 | 0.99–1.04 | .102 |
| Time spent outdoors in summer | |||
| Less than ½ | 2.00 | 1.18–3.42 | .010 |
| ∼ 1/2 | 1.37 | 0.79–2.37 | .265 |
| More than 3/4 | 1 (ref) | ||
| Time outdoors in winter | |||
| Mostly indoors | 1.85 | 1.01–3.39 | .046 |
| 50/50 | 1.18 | 0.63–2.21 | .607 |
| Mostly outdoors | 1 (ref) | ||
| Conjunctival ultraviolet autofluorescence (per 10 mm 2 decrease) | 1.15 | 1.10–1.19 | <.001 |
As they were not significant in the univariable analysis, height, weight, and BMI were not included in the multivariable models ( Table 2 and Table 3 ). Participant recall of time outdoors was not included in the multivariable analysis owing to its collinearity with conjunctival ultraviolet autofluorescence, but when it replaced conjunctival ultraviolet autofluorescence in the multivariable analysis it remained significantly inversely associated with myopia (data not shown). Conjunctival ultraviolet autofluorescence showed a stronger inverse association with myopia than participant recall of time outdoors. There was no interaction between education and conjunctival ultraviolet autofluorescence (p interaction = 0.482) or between parental myopia and conjunctival ultraviolet autofluorescence (p interaction = 0.141).
| Variable | OR | 95% CI | P |
|---|---|---|---|
| Age (per year) | 1.42 | 1.03–1.95 | .03 |
| Sex (female) | 0.87 | 0.65–1.16 | .34 |
| Parental myopia | |||
| No parents | 1 (ref) | ||
| One parent | 1.98 | 1.41–2.78 | <.001 |
| Both parents | 2.98 | 1.80–4.93 | <.001 |
| Education level | |||
| University started/completed | 1.66 | 1.24–2.22 | .001 |
| Conjunctival ultraviolet autofluorescence (per 10 mm 2 decrease) | 1.12 | 1.08–1.19 | <.001 |
| Variable | OR | 95% CI | P |
|---|---|---|---|
| Age (per year) | 1.42 | 1.03–1.96 | .03 |
| Sex (female) | 0.89 | 0.66–1.19 | .43 |
| Parental myopia | |||
| No parents | 1 (ref) | ||
| One parent | 2.01 | 1.44–2.83 | <.001 |
| Both parents | 2.98 | 1.80–4.93 | <.001 |
| Education level | |||
| University started/completed | 1.67 | 1.25–2.23 | .001 |
| Conjunctival ultraviolet autofluorescence | |||
| 4th quartile (>69.8 mm 2 ) | 1 (ref) | ||
| 3rd quartile (44.2–69.8 mm 2 ) | 1.07 | 0.69–1.68 | .760 |
| 2nd quartile (20.2–44.2 mm 2 ) | 1.64 | 1.08–2.51 | .021 |
| 1st quartile (>20.2 mm 2 ) | 2.52 | 1.66–3.81 | <.001 |
Analysis by Increments of 10 mm 2
Prevalence of myopia decreased with increasing conjunctival ultraviolet autofluorescence ( Figure 2 ). For every 10 mm 2 reduction in total conjunctival ultraviolet autofluorescence, odds of myopia increased by 15% (OR 1.15, 95% CI 1.10–1.19, P < .001). This remained significant after adjustment for age, sex, educational level, and parental history of myopia (OR 1.12, 95% CI 1.08–1.19, P < .001).




