Purpose
To describe the characteristics and course of late varicella-zoster virus (VZV) dendriform keratitis in patients with histories of herpes zoster ophthalmicus (HZO); to describe responses of corneal lesions to antiviral treatment; and to investigate risk factors for recurrence.
Design
Retrospective case series.
Methods
Included were patients known to have 1 or more episodes of dendriform lesions beginning at least 2 weeks after HZO in 2 academic practices. Epithelial lesions were evaluated for the presence of VZV DNA by a polymerase chain reaction assay. Demographic, medical, and ophthalmic data were collected for each episode. Responses to treatment with antiviral medications were evaluated. Cumulative risk of recurrence was determined using Kaplan-Meier analysis; potential risk factors for recurrence (age, systemic disease, lesion characteristics, corticosteroids) were evaluated using univariate Cox proportional hazard models.
Results
We identified 20 patients (14 women; median age, 65 years) who met inclusion criteria. Dendriform lesions were pleomorphic with thickened, opaque epithelium. Seven patients had systemic diseases characterized by altered immune function. VZV DNA was identified in 15 of 16 cases tested, and all lesions responded to antiviral therapy. The 1-year incidence of first recurrence was 95.8 lesions per 100 person-years of follow-up. Patients had multiple recurrences, but risk of recurrence appeared to decrease over time. No statistically significant risk factors for recurrence were identified.
Conclusions
Late dendriform lesions associated with HZO are foci of productive VZV infection. Lesions can be treated effectively with topical or systemic antiviral agents. Patients can have multiple recurrences of dendriform lesions despite treatment.
A variety of corneal disorders can occur in patients with herpes zoster ophthalmicus (HZO). Recoverable virus has been demonstrated in dendriform lesions that develop soon after the onset of cutaneous lesions. In contrast, late epithelial lesions, including mucous plaques, have traditionally been considered noninfectious in nature. In 1988, Engstrom and Holland described chronic varicella-zoster virus (VZV) infection of the corneal epithelium in a patient with acquired immunodeficiency syndrome (AIDS). Chern and associates subsequently confirmed the occurrence of such infections and described the characteristics and course of lesions in a series of 16 patients with human immunodeficiency virus (HIV) infection. Pavan-Langston and associates have shown that similar lesions can occur in people without HIV infection; they described 4 patients with “delayed pseudodendrites” that were found to contain VZV DNA and that responded to antiviral therapy. Al-Muammar and Jackson subsequently described 3 patients with histories of HZO and dendriform corneal lesions that responded to treatment with a combination of topical and oral antiviral agents. There is little additional information in the medical literature about such lesions. The purpose of the current study is to describe in greater detail the spectrum of clinical characteristics, the clinical course, and the response to antiviral treatment of late VZV dendriform keratitis in patients with histories of HZO who do not have HIV disease.
Methods
Included were all patients in 2 academic practices (those of G.N.H. and T.P.M.) who had histories of HZO or had histories of HZO sine herpete (ocular disease without skin lesions), and who developed dendriform keratitis at least 2 weeks after the onset of HZO. Also included were all patients who had other epithelial lesions following the onset of HZO, and whose lesions were evaluated with polymerase chain reaction (PCR) techniques for VZV DNA. For purposes of this report, these cases provided a control to investigate whether VZV was associated specifically with dendriform lesions. Excluded were patients who were known to be HIV-infected or who had histories suggestive of HIV disease. HIV testing was not performed routinely on other patients who met inclusion criteria.
As an additional control for the specificity of the PCR assay, we reviewed results for the 23 patients with HSV keratitis reported by Leigh and associates, whose corneal specimens had been tested in our laboratories. All had positive tests for HSV but had been tested for evidence of VZV as well.
Data Collection
Retrospective chart reviews were performed for all patients. For each, the following demographic and medical data were collected: age, gender, and systemic diseases that might be associated with altered immune function. For each examination at which dendriform lesions were identified, the following factors were collected: eye affected and interval from onset of HZO to development of lesions (for first-identified dendriform lesions) or from previous dendriform lesions (for recurrent lesions). The following medical data were collected for each subject throughout the course of follow-up: medications used (corticosteroids, topical and systemic antiviral agents, immunosuppressive drugs) and temporal relationship of medication use to development of first-observed or recurrent lesions. If medical records that identified the date on which first-identified dendriform lesions developed were available from referring physicians, that information was used to calculate the intervals from onset of HZO to development of dendriform lesions and from onset of dendriform lesions to treatment. All other analyses use data only from examinations at our institutions.
The following ophthalmic data were collected for each episode of dendriform lesions: associated symptoms; characteristics of lesions (appearance, presence of fluorescein staining, location [central, midperipheral, limbal]); presence of stromal involvement (infiltrates, scar); and anterior chamber cells. All slit-lamp biomicroscopic examinations had been performed by 1 of 2 authors (G.N.H., T.P.M.).
The following information about treatment for each episode was collected: use of oral or topical antiviral agents; use of topical corticosteroids; and changes in lesions following start of antiviral agents.
All evaluations of corneal scrapings for VZV DNA by PCR-based assays were performed in the Clinical Microbiology Laboratory at the Francis I. Proctor Foundation, University of California, San Francisco, using methods described previously. All specimens were also tested for the presence of herpes simplex virus (HSV) DNA as previously described.
Study Definitions
An epithelial lesion was considered dendriform if it had a linear pattern with multiple branches or components that were identified by epithelial opacity or by fluorescein staining. A lesion was considered central if it involved the apex of the cornea; a lesion was considered limbal if any aspect of the lesion extended to, or involved, the limbal conjunctiva; all other lesions were considered to be midperipheral. Recurrence was defined as a new dendriform lesion after resolution of previous lesions, whether the new lesion was in the same or a different location than the previous dendriform lesions. Active uveitis was defined as the presence of anterior chamber cells. Cells had been assigned semi-quantitative scores, as defined by Hogan and associates.
Data Analysis and Statistical Techniques
We compared the proportion of dendriform lesions found to contain VZV DNA to the proportion of other, nondendriform epithelial lesions found to contain VZV DNA using the Fisher exact test. Cumulative risk of first recurrence was determined by Kaplan-Meier analysis.
Three factors associated with first-observed lesions (age, presence of systemic disease, lesion location) and 3 factors identified at first-observed episode or during follow-up examinations before first recurrence (presence of stromal involvement, use of topical corticosteroids, presence of anterior uveitis) were investigated as potential risk factors for first recurrence using univariate Cox proportional hazard models.
Representative Case Histories
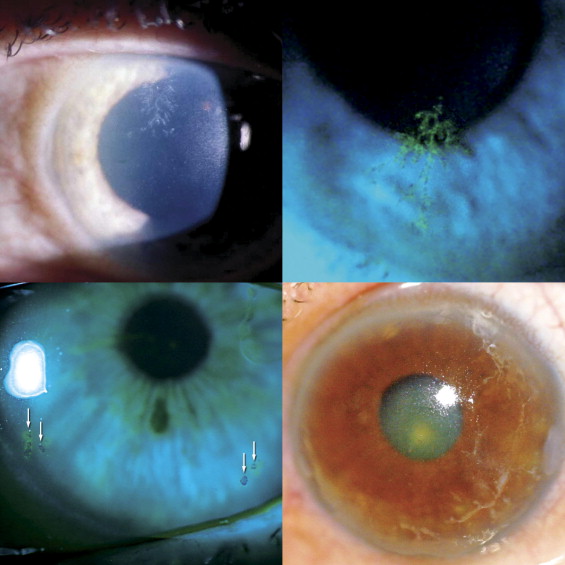
Case histories of 3 representative patients are presented in the Supplemental material (available at ajo.com ). They illustrate the spectrum of clinical characteristics and courses of dendriform keratitis. Corneal lesions for each case are illustrated in Figure 1 .
Results
We identified 20 patients with histories of HZO who developed late dendriform keratitis. Two patients had HZO sine herpete ; diagnosis was suspected on the basis of chronic keratouveitis consistent with herpetic disease (interstitial keratitis, decreased corneal sensation, sectional iris atrophy) and associated facial pain suggestive of post-herpetic neuralgia. We identified an additional 5 patients with histories of HZO who had other corneal epithelial lesions that were evaluated with the PCR assay to rule out the presence of VZV DNA; 2 had nondendriform punctate epithelial keratitis and 3 had persistent epithelial defects associated with underlying stromal keratitis.
Table 1 lists demographic, medical, and ophthalmic characteristics of first-observed lesions for the 20 patients with late dendriform keratitis. The majority of patients were women. Seven of 20 (35%) had a systemic disease that could be associated with altered immune function or were receiving immunosuppressive medications; the specific conditions are listed in Table 1 . Five of 12 patients (42%) who were 65 years of age or younger, including the 2 youngest patients (aged 45 and 51 years), had 1 of these medical conditions associated with altered immune function. In contrast, only 2 of 8 patients (25%) older than 65 years had such medical conditions. We identified no unique disease characteristics in the subgroup of patients with possible alterations in immune function. The median interval from onset of HZO to development of first-observed dendriform lesions was 5 months, but was as long as 15 months in 1 patient. The majority of patients described 1 or more symptoms (18 patients, 90%) and had decreased corneal sensitivity (14 patients, 70%).
| Variable | Value |
|---|---|
| Median age (range) | 65 (45–82) years |
| Female | 14 patients (70%) |
| Systemic diseases a | 7 patients (35%) |
| Median interval from HZO to first-observed dendriform lesions b (range, n = 18 c ) | 5 (0.5–15) months |
| Symptomatic d | 18 patients (90%) |
| Location of lesions e | |
| Central | 5 corneas (25%) |
| Midperipheral | 14 corneas (70%) |
| Limbal | 1 cornea (5%) |
| Anterior chamber cells (n = 17 c ) | 14 eyes (82%) |
| Stromal keratitis (n = 17 c ) | 12 eyes (71%) |
| VZV DNA present f (n = 16 c ) | 15 lesions (94%) |
a Including rheumatoid arthritis being treated with methotrexate (2 patients); non-Hodgkin lymphoma/Waldenstrom macroglobulinemia, history of bladder cancer/breast cancer, history of inflammatory bowel syndrome, non-Hodgkin lymphoma status post stem cell transplantation, and mixed connective tissue disease/history of breast cancer (1 patient each).
b Not included were 2 patients with HZO sine herpete .
c Number of patients/eyes/lesions for whom the factor was known, if less than 20.
d Symptoms included foreign body sensation, photophobia, and tearing.
e Central was defined as involving the apex of the cornea; limbal was defined as crossing the limbus; all other lesions were identified as midperipheral.
VZV DNA was identified by PCR assay in 15 of 16 first-observed lesions tested (94%), including both patients with HZO sine herpete ; in contrast, no VZV DNA was identified in the other epithelial lesions of 5 patients with histories of HZO ( P = .0003, Fisher exact test). All tests for HSV DNA were negative. None of the 23 patients with HSV keratitis reported by Leigh and associates had positive PCR assay results for VZV.
There was a spectrum of clinical features associated with the first-observed dendriform lesions ( Figure 1 ). The epithelial lesions often had multiple components, including a variable mixture of dots, lines, and branching forms with blunt ends. The components could be discontinuous. The epithelium was often thickened and opaque, but linear portions of the lesions were generally delicate in appearance. All lesions were gray/white in color and stained variably with fluorescein, rose bengal, or lissamine green stains. There was a tendency for lesions to be more irregular and their appearance to be either more coarse or more delicate than the discrete dendrites caused by HSV. None of the branches had terminal bulbs, as seen with HSV-associated dendrites. Lesions were either central or midperipheral in 19 cases (95%). Only 1 first-observed lesion involved the limbus; the patient had undergone stem cell transplantation for non-Hodgkin lymphoma and was being treated with prednisolone acetate 1%.
Among 17 patients for whom information about the anterior chamber was available, 14 had active anterior uveitis; cells were scored as 1+ or more in 7 patients (41%) at the time of first-observed dendriform lesions. Stromal involvement, characterized by diffuse stromal haze or by sectoral stromal haze subjacent to epithelial lesions, was present in the majority (71%) of patients (n = 17 eyes); there were no dense focal inflammatory infiltrates.
Among the 19 patients with dendriform lesions who were followed by us (1 patient was seen only once by us for a consultative visit), the mean ± SD duration of follow-up was 2.7 ± 2.6 years (median, 1.6 years; range, 0.06 years [22 days] to 8.7 years). Eight of 19 patients were followed by us for less than 1 year. None of the 5 HZO patients with other lesions developed dendriform lesions during follow-up. Information about disease course is provided in Table 2 .
| Variable | Value |
|---|---|
| Median interval from onset of first-observed lesion to start of treatment (range, n = 9 a ) | 21 (2–52) days |
| Response to treatment (n = 18 a b ) | |
| Resolution of epithelial lesion | 18 eyes (100%) |
| Resolution with residual stromal changes | 3 eyes (17%) |
| Median time to resolution of lesions (range) | 13 (7–35) days |
| Number of eyes with recurrences (n = 19 a c ) | 10 |
| Number of documented episodes per eye, range | 1–5 |
| Median interval between documented episodes (range) | 0.4 (0.1–2.6) years |
a Number of patients/eyes for whom the factor was known, if less than 20.
b Two patients were excluded (1 patient did not have any follow-up examinations, and 1 patient had follow-up only 2 months after the first-observed dendriform lesion, and was therefore censored from this analysis).
c One patient was excluded due to lack of any follow-up data.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


