Summary
Blunt trauma to the head and face may impact the orbital rim, transmitting avulsive force to the eye muscle pulleys and then to the eye muscles themselves. This may result in damage to the pulleys and muscles, leading to strabismus. These muscle traumas were termed “flap tears” by this author due to the flaplike appearance of the avulsed portion of muscle in the early cases. The muscles seemed to have been “sliced” as if by a knife, although no orbital penetration had occurred. Other types of appearance of muscle avulsion have since been identified.
The onset of strabismus is usually delayed by several weeks, becoming manifest during formation of scar tissue. Symptoms may be delayed by years if fusional vergence amplitudes allow the patient to maintain alignment despite the abnormal restriction to motility. Patients often forget the trauma that precipitated the problem.
The most commonly involved muscle is the inferior rectus, and therefore the classic presentation of flap tear has been hyperdeviation greater on downgaze after orbital floor fracture. Exotropia is also common after flap tear, particularly with convergence insufficiency, and esotropia is also seen.
Penetrating trauma to the eye muscles and iatrogenic eye muscle trauma following sinus surgery, retinal detachment repair, glaucoma valve placement, and inadvertent local anesthetic into a muscle, and muscle loss and rupture during strabismus surgery are also discussed.
20 Traumatic Strabismus: Direct Orbital and Muscle Trauma and Flap Tear
20.1 Introduction
Trauma may cause strabismus by damaging the central nervous system (CNS) and/or the cranial nerves (CNs), which control eye movements. (Surgical intervention for CN palsy and CNS abnormalities is addressed in Chapter 18 Cranial Nerve Palsies.) It can also cause direct mechanical damage to the eye muscles, their pulley system (which is essential for proper muscle function) 1 , and the bony orbit. Combined CNS damage and direct muscle injury is certainly possible, and has been observed. Distinguishing between neural and mechanical damage requires sophisticated diagnostic acumen. By correctly pinpointing the etiology of strabismus, the surgical correction will be more precise and lasting.
20.2 Blunt Trauma
20.2.1 Partial Avulsion of a Rectus Muscle (Flap Tear)
A partial tear of a rectus muscle can result indirectly from blunt trauma to the orbital rim and/or face, as well as direct muscle trauma during sports, retinal detachment surgery, or penetrating trauma. 2 , 3 , 4 The resultant motility defect results from restriction of movement created by scarring of the avulsed section of muscle (the flap) to the surrounding orbital tissues (Fig. 20‑1). Displacement or disruption of the orbital pulleys may also contribute to the motility abnormality. 5 The direction of healing taken by the avulsed tissue determines the resultant motility defect. Understanding of this complex condition is simplified by dividing it into the following components:
Type/appearance of tear: longitudinal, lamellar, beveled, retracted (Fig. 20‑2, Fig. 20‑3, Fig. 20‑4, Fig. 20‑5, Video 20.1, Video 20.2).
Location of tear: avulsed from insertion (Fig. 20‑6), avulsed from musculotendinous junction (Fig. 20‑7), or deep muscle belly rupture (Fig. 20‑8).
Muscle(s) involved: inferior rectus (IR), medial rectus (MR), superior rectus (SR), and lateral rectus (LR), in order of decreasing frequency.
Mechanism of strabismus and direction of healing of flap: tether, dragging, pulley displacement.

Fig. 20.1 Flap tear of left inferior rectus muscle. 
Fig. 20.2 (a) Longitudinal flap tear of left inferior rectus (LIR) muscle. (b) Black dotted lines outline intact portion of LIR muscle, on Green hook. White dotted lines outline avulsed “flap” of muscle, fibers coursing under Desmarres retractor. (c) Same muscle after repair. 
Fig. 20.3 (a) Lamellar flap tear of left medial rectus (LMR) muscle. Muscle may look deceptively normal, but it is devoid of its capsule and orbital layer, beginning about 4 mm behind the insertion. (b) Black dotted lines outline area of intact muscle, blue dotted lines indicate the denuded section, and white dotted lines show the path of the avulsed flap, behind Desmarres retractor. (c) Flap after retrieval, suspended on suture. 
Fig. 20.4 (a) Beveled flap tear of left inferior rectus. (b) Remaining attached portion of muscle is thicker temporally (black arrow) than nasally (blue arrow). Avulsed flap indicated by dotted black lines. 
Fig. 20.5 (a) Retracted flap tear of right inferior rectus. Flap is not visible, and has retracted between orbital septal layers. (b) Same muscle, after retrieval and reattachment of flap. 
Fig. 20.6 (a) Flap tear (longitudinal) of left medial rectus, flap avulsed from insertion. (b) Missing muscle section outlined by black dotted line. (c) Same muscle, repaired. 
Fig. 20.7 (a) Flap tear (beveled) of right inferior rectus, avulsed from musclulotendinous junctions. This is an atypical medial tear. (b) Black dotted line outlines the edge of defect. Medial edge is thicker (white arrow) than inner edge (black arrow), making this a beveled flap. (c) Avulsed flap has been retrieved, and is suspended on suture (arrows). (d) Same muscle, repaired. 
Fig. 20.8 Flap tear (lamellar) with deeper origin. Edge of tear indicated with black arrows. Deeper tears than this have been observed.
20.2.1.1 Background
Ipsilateral hyperdeviation following orbital floor fracture was traditionally attributed to palsy of the branch of the third cranial nerve (CN III) to the IR. 6 , 7 Anatomically, that would require the trauma to sever the muscle belly, as the course of the inferior division of CN III is short, dividing within the muscle cone to the inferior oblique (IO) and IR muscle branches. This conundrum led to exploration of the IR in one such case in 1994, over 1 year following the patient’s orbital fracture repair. The muscle was found attached at the insertion, not severed horizontally into two halves as had been anticipated, but its anatomy was distorted. There was a mass of scarred tissue external to the muscle cone, and several hours of gentle dissection within surgical planes led to freeing of the abnormal tissue. A flap of muscle came forward to fill the defect in the attached portion of muscle, and the anatomy became clear. The distal part of the flap had been adherent toward the orbital rim, and had acted as a tether restricting downgaze. The IR was repaired, and the motility improved. Over several years, four similar cases were identified and repaired. This led to a report of five cases of hyperdeviation following orbital floor fracture repair. 8 Initially it was incorrectly hypothesized that the orbital surgeon had created the damage by slicing the IR during surgery. The missing portion of muscle looked like a “flap” that had been sliced away from the remaining attached IR. A few cases then presented with the identical IR appearance without any prior orbital surgery. It became clear that the original blunt trauma had caused a portion of the IR to avulse. The fracture site was usually far posterior to the location of the muscle tear, which was usually at or near the insertion. Over time it was found that avulsion injury to the extraocular muscles and/or pulleys can also occur without identifiable orbital fracture, and that these smaller, more occult injuries are common.
20.2.1.2 Presenting Strabismus
The classic presentation is a hyperdeviation greater on downgaze and ipsilateral side gaze (without torsion) following orbital floor fracture (Fig. 20‑9). When this pattern is present, flap tear may be diagnosed with certainty. The cause is the tether created by the outwardly flapped avulsed segment of IR. Associated small exodeviation is common, and will often resolve with flap tear repair alone.
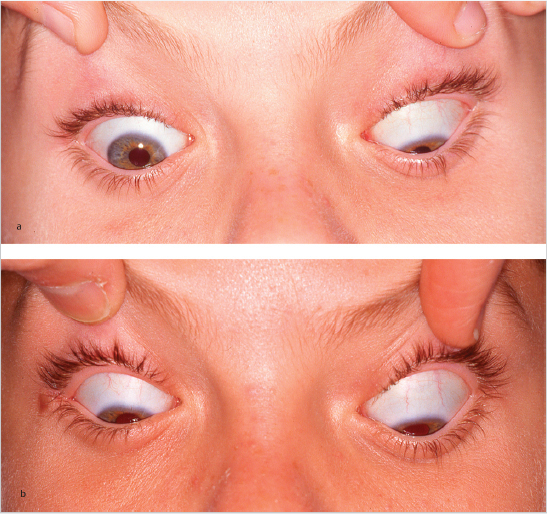
It also became clear that other strabismus patterns were possible and actually more common than hypertropia. MR and/or IR flap tear can present with exotropia, and convergence insufficiency is frequent. Esotropia was originally diagnosed with rare LR tears, but more recently has been identified together with IR tears, in which the flaps were healed nasalward. This may prove to be a common result of IR flap tear.
Head trauma and facial trauma may be combined after a single event, such as an automobile accident with cranial trauma from the initial impact and facial trauma due to air bag deployment.
20.2.1.3 Mechanism of Tear
Blunt trauma to the face is the usual cause of flap tear, especially when the impact is to the orbital rim. Anatomical studies have shown elastin penetrations into the orbital layer of each rectus muscle, causing the muscle’s orbital layer to insert onto the pulley rather than the scleral insertion (Fig. 20‑10). Traction from a bending or fracturing orbital wall could be transmitted to the outer muscle fibers (Fig. 20‑11, Fig. 20‑12, Fig. 20‑13, Fig. 20‑14), causing the orbital layer of the muscle to tear away from the global layer. This would result in a lamellar flap tear.





Achilles tendon ruptures can be caused by tension from a strong contraction of the gastrocnemius/soleus complex in a healthy individual. Perhaps a similar contraction of the IR occurs during trauma, which could explain longitudinal-type tears.
Some partial avulsions have been caused by direct but nonpenetrating trauma, such as poking actions, or an object striking directly over the muscle insertion without penetrating the conjunctiva.
Retinal detachment surgery can cause lamellar flap formation due to the common practice of blunt stripping of connective tissue off the surface of the muscle prior to scleral buckle placement.
20.2.1.4 Flap Tear Appearance/Types
Normal inferior rectus and medial rectus muscle appearances are compared to the four types of flap tear in Video 20.1 and Video 20.2.
20.2.1.4.1 Longitudinal
Most partial avulsions assume a longitudinal splitting configuration, resulting in a narrowed appearance to the remaining attached portion of muscle. Longitudinal flaps of the IR are almost always temporal in location, and can vary from a tiny sliver of muscle to a large tear with most of the muscle avulsed off its insertion (Fig. 20‑15, Fig. 20‑16). The capsule usually avulses with the muscle flap, but sometimes the capsule is intact, partly disguising the extent of the injury. A muscle hook placed under the insertion will show the defect. MR flaps are usually inferior in location, but superior MR flaps have been seen. SR flap tear is rare, and has usually been associated with major head trauma with superior orbital fracture. Two cases were seen of SR partial avulsion due to direct nonpenetrating trauma over the muscle insertion. LR avulsions are very rare, and the only two seen were each the result of direct pulling trauma at the lateral orbital rim, such as with wrestling.


20.2.1.4.2 Lamellar
Another configuration is a lamellar tear, with separation of the orbital from the global layers of the rectus muscle, causing a thinned, capsule-denuded appearance (Fig. 20‑13, Fig. 20‑17). The MR muscles seem to be the most prone to present with full-width thin lamellar flaps. These are the most difficult flaps to locate and repair. The hypothesized mechanism of this tear, which is often, but not always, seen in combination with longitudinal flap of the IR, is illustrated in Fig. 20‑12. Although seemingly insignificant, as the muscle tissue itself seems uninvolved, these may cause profound exotropia (Case 4 Large Angle Exotropia Corrected with Flap Tear Repair Alone, Video 20.3, Chapter 29 Traumatic Strabismus Repair (Flap Tear, Slipped and Lost Muscles)). There may be a genetic component to this defect, as many of these patients have shallow-appearing orbits, and some have no or minimal history of trauma. Three infants with this defect have been identified to date. 9

20.2.1.4.3 Beveled
A beveled appearance of the flap is probably due to a combination of the lamellar and longitudinal tear mechanisms. The orbital (or external) layer of the muscle always has the greatest tissue loss, and the global layer is more or fully intact.
20.2.1.4.4 Retracted (Turtleneck)
Some flaps retract within their sheath and may be difficult to trace. The capsule appears intact, but the muscle is deficient in width. It would seem that these flaps cause less difficulty with tether formation and may not cause as much disturbance of motility. It is likely that the associated pulley disruptions or displacements may be the main source of strabismus with these tears.
20.2.1.5 Point of Flap Disinsertion
20.2.1.5.1 Avulsion from Insertion
Many flaps avulse from the muscle insertion, leaving a narrowed insertion. For IR tears the avulsion is almost always temporal in location, and MR tears are usually inferior, but superior segment MR tears have been seen (Fig. 20‑1, Fig. 20‑6, Fig. 20‑16, Fig. 20‑18).

20.2.1.5.2 Avulsion from Musculotendinous Junction
Some flaps disinsert posterior to the insertion, usually at the musculotendinous junction. These can appear deceptively normal on quick inspection due to the normal width and capsule at the insertion. The abnormality becomes clear when the Desmarres retractor is placed, because adhesions prevent full exposure of the muscle. The proximal capsule disruption and distorted pulleys also help diagnose the tear (Fig. 20‑2, Fig. 20‑7, Fig. 20‑19).

20.2.1.6 Strabismus Mechanism
The direction in which the flap heals determines the motility defect, if any. Presumably, many flaps heal back to the muscle or into a motility-neutral position and cause no trouble.
20.2.1.6.1 Tether
Some tears flap directly away from the muscle cone toward the orbital periphery, creating a tether and a motility defect toward the direction of action of that muscle. This would simulate a weakened muscle, and has usually been mistaken for partial CN palsy. Force generation testing, however, usually reveals the muscle strength to be good, and the forced duction test usually demonstrates mechanical restriction. With this mechanism, IR flap tear causes a hyperdeviation greater on downgaze, and MR flap tear would cause exotropia and convergence insufficiency. Both presentations have been regularly seen clinically. LR flap tear could therefore conceivably cause esotropia, and SR flap tear could cause a hypotropia. These are both rare conditions, but they have been demonstrated and successfully repaired.
20.2.1.6.2 Dragging
The IR muscle is by far the most prone to partial avulsion, presumably due to anatomical connections to the inferior orbital wall, which is the most common site of orbital fracture. Most flaps occur at the temporal side of the IR, and this finding correlates with the anatomical separation of the IR into nasal and temporal compartments as discussed in Chapter 4. When the flap and connected pulley tissues are dragged into a temporal direction, the deviation tends to be outward. This is especially true for bilateral IR flap tear, in which the bilateral hyperdeviations cancel each other out and become asymptomatic. The exoshift becomes the clinical problem. If the flap is dragged nasalward, esotropia could develop, and this phenomenon has only recently been discovered.
20.2.1.6.3 Pulley Displacement and Pulley Tear
Temporal displacement of the flap is usually associated with temporal displacement of the muscle pulleys, further reducing the strength of the IR. It may also place traction on the pulleys of adjacent muscles. Inferior displacement of the MR pulley could conceivably occur from traction from the temporally displaced IR pulley. Distortion of the MR path could contribute to exotropia after flap tear. Inferior displacement of the belly of the MR has been seen in some flap tear cases, and responds well to simple myopexy or pulley fusion (Chapter 19, Chapter 30).
Pulley tear with subsequent scarring may also impair muscle function without muscle tear or displacement (Video 29.17).
20.2.1.7 Muscles Involved
Flap tear most commonly involves the IR, followed by the MR. This is presumably due to their proximity to the maxillary and ethmoid sinuses, with their thin adjacent orbital walls. Combined inferior and medial rectus tears are not infrequent. Superior and lateral rectus flap tears are rare (Fig. 20‑20), but have been reported. The superior orbital fractures needed to cause SR avulsions have usually been associated with severe skull trauma. The several LR tears were due to direct trauma (e.g., pulling force at the lateral canthus during wrestling), rather than indirect blunt trauma. Bilaterality is common with inferior and medial rectus avulsions, with about the same frequency as unilaterality. IO involvement has been rare. In one case the lamellar IR flap had wrapped around the IO, distorting its path, converting it to a depressor on downgaze. Two cases have been documented with IO rupture. One was combined with severe IR flap tear, and the other was isolated to the IO (Case 6, Video 20.4). Disinsertion of the trochlea may occur in combination with flap tear if there is a partial penetration of a blunt object (as has happened with a handlebar of a bicycle in one case [Fig. 20‑21, Fig. 20‑22], and a finger-poking incident in another).



20.2.1.8 Diagnosis—History
The patient’s history is critical to diagnose and predict the presence of a flap tear, even if the specific trauma is no longer recalled. When there is no family history of strabismus and the strabismus had a subacute onset, a precipitating event may have occurred. Questioning should probe for possible trauma. Were sports ever played that included facial impact? Was there ever an air bag deployment? Has the patient ever experienced ecchymosis?
20.2.1.8.1 Early Childhood
Early childhood onset does not preclude flap tear. Young children often fall flat on their faces when learning to walk, and their delicate tissues may be easily traumatized by a seemingly minor impact. A history of ecchymosis is suggestive, but not a prerequisite (Fig. 20‑23). Head-banging behaviors, seen in autism as well as in some nonautistic children, can cause flap tear. Running into a wall or an edge of a coffee table, and falling off a bicycle, swing, or tree are activities that have caused rectus muscle trauma.

20.2.1.8.2 Adults
Adults do not always connect the onset of strabismus with the precipitating injury. Strabismus develops as scar tissue begins to strengthen and contract, usually over 3 weeks after trauma. If this is accompanied by strong fusional vergence ability there may be no symptoms for years, until tissues stiffen and vergence amplitudes begin to break down with age.
This author repaired flap tears in a Korean War veteran, whose injury was caused by a concussive blast while sitting on a tank, and a Vietnam War veteran, who received blows to his face from the butt of a rifle of a fellow soldier. Both were able to maintain fusion for years until reaching their 50s. The Korean War veteran received several routine surgeries over 10 years by the author, which helped temporarily, but strabismus recurred regularly until recognition of the true etiology with definitive repair.
20.2.1.8.3 Combined Trauma
Motor vehicle trauma can cause CN palsy due to the head injury as well as partial avulsion due to the facial trauma. A severe beating could also do the same. The resulting strabismus patterns can be complex and perplexing, such as bilateral superior oblique (SO) palsy with large extorsion and V pattern, but exotropia and convergence insufficiency due to bilateral IR flap tear. This exact combination has been seen and fully corrected with flap tear repair and bilateral SO advancement (Case 2). A history of loss of consciousness will alert the examiner to possible CN palsy, and questioning about facial bruising, laceration, swelling, or orbital fracture would point to flap tear.
20.2.1.8.4 Predisposing Visual Abnormalities
Patients with preexisting sensory abnormalities (poor vision or weak fusion) may have a greater predisposition to developing strabismus following blunt trauma. Someone with normal vision and fusion will fight to maintain alignment during the healing process, and perhaps this will help the eye to heal near primary position. If a small residual angle of strabismus is present, fusional vergence may allow the patient to remain asymptomatic. When fusion is absent there is no ability to counteract the mechanical forces caused by the trauma and subsequent healing with scar contracture. Perhaps this scenario explains some cases of acquired sensory exotropia (Case 3).
20.2.1.9 Examination—Office
Clues to the presence of flap tear are usually discernable during the office examination. Examine the ocular adnexa carefully, and measure for orbital asymmetry and possible enophthalmos, indicating possible occult trauma. Gaze restriction is usual, and a hyperdeviation greatest on gaze to the side ipsilateral to the higher eye is a classic finding. Exotropia with convergence insufficiency is also common. Pseudo-SO overaction is a typical finding. The adducting (uninvolved) eye appears to overdepress, but this is an illusion caused by the tethered (torn) IR of the abducting eye. The key to distinguishing this from true SO overaction is to examine the retinas for torsion. True SO overaction should be accompanied by intorsion in the primary position on fundus examination. Torsion is atypical with flap tear alone, and when present could point to pulley displacement or primary or secondary oblique dysfunction.
In-office forced duction may reveal restriction into the field of action of the involved muscle(s), and force generation testing usually proves active contractile force of the muscle. There have been exceptions to both these rules, but if one encounters strong contractility of a seemingly “paretic” muscle combined with mechanical restriction into that muscle’s gaze direction, one can be certain of the presence of a partial avulsion.
20.2.1.10 Diagnosis—Imaging
High-resolution magnetic resonance imaging (MRI) with the use of surface coils has successfully demonstrated flap tear, 10 , 11 , 12 but the lower-resolution imaging available to most of us is usually nonspecific. There may be irregularity of the IR and associated pulley displacements. In the primary position, an IR flap may be closely approximated to the muscle, and the separation may not be seen with MRI. The separation would probably become apparent with active contraction of the muscle, which could be achieved by repeating the MRI with the patient in a downgaze position. Hopefully, imaging will become more useful as access to quality scans improves in the future (Fig. 20‑24).

Performing detailed scans in young children is probably not helpful enough to warrant the additional anesthesia, risk, and expense. In adults, this author finds imaging more helpful to identify the associated muscle displacements than the tears themselves. Muscle displacements should also be corrected along with repair of flap tear (Chapter 19, Chapter 30). Fine-cut coronal orbital sections are requested, and the use of contrast is discouraged.
20.2.1.11 Surgical Planning
Although flap tear may be suspected, there needs to be a contingency plan in place in case it is not found. A sample surgical plan for right hypertropia and exotropia possibly due to trauma could read as follows: “Inspect inferior and medial rectus right eye, with repair if defect is found. Possible comparison with muscles left eye. If no defect is found, will recess the right LR 7 mm, resect the right MR 5 mm, and anteriorly transpose the right IO. If defect is found, it will be repaired and the plan adjusted accordingly.” In this case a flap tear of the right IR and possibly the MR could cause such a pattern. Repair would reduce or eliminate the need for additional standard surgery. A decision regarding the need for additional standard strabismus surgery is based upon the forced duction and spring-back balance tests after the muscle or muscles are repaired. For exotropia, recession of a single LR alone is sufficient in most cases after flap tear repair. If alignment looks good, then no recession is required. 15 If flap tear is present based upon the forced duction test and muscle appearance, but the surgeon cannot find it, then resection of the remaining attached portion of muscle is the best approach, as it reduces the tether-restriction of the flap on the muscle. Some surgeons have reported success in restoring motility by simple disinsertion of the flap rather than full repair. 13 , 14
20.2.1.12 Flap Tear Repair
Intraoperative recognition of flap tear and repair technique are detailed in Chapter 29 (Fig. 20‑25).

20.2.1.13 Postoperative Management
Patients are asked to begin active range of motion motility exercise immediately following surgery, and to pursue this hourly if possible. Although the use of topical steroids could potentially reduce adhesions and possible recurrent tethering, it could also impede the healing of the flap itself. Orthopaedists don’t use postoperative steroids following tendon or ligament repair, so steroid use after flap tear is probably not advisable.
20.2.1.13.1 Eye Muscle Physical Therapy
When the eye has not regained full rotation after flap tear repair, aggressive in-office forced duction can expand the range of motion. This is similar to physical therapy after orthopaedic surgery. The conjunctiva is anesthetized topically in a location opposite the direction of limitation (e.g., pull from the superior limbus for deficient depression). It is then grasped with a toothed forceps several millimeters behind the limbus, and the eye is pulled into the direction of gaze limitation with the patient actively looking that way (Fig. 20‑26). The force is gradually increased and held for 20 to 30 seconds. The process is repeated several times per session. Biweekly sessions are performed over several months. Some patients have a dramatic response to one or two stretching sessions and can discontinue stretching earlier. Some patients have excellent alignment after repair alone, and can omit the physical therapy. If stretching is needed in a young child, it is done in the operating room with brief general anesthesia.

20.2.1.13.2 Standard Strabismus Surgery—Ipsilateral Resection/Contralateral Recession and Restrictive Procedures
If residual strabismus remains, standard strabismus surgery is performed at a later date. If orthotropia has been achieved in primary position, then first concentrate on conservative range of motion stretching. If primary position undercorrection exists, this may be due to excessive muscle length. The traumatized muscle may gain length as a result of the injury, particularly if there was posterior damage that could not be repaired. A small resection of the involved muscle is usually effective, and easier to perform if done within a few days after primary repair. Back-to-back surgery dates are usually planned for out-of-town patients to allow for small reoperations.
When combined trauma has occurred, such as fourth CN palsy due to head trauma along with IR flap tears due to facial trauma, combined surgery is done, such as SO advancements combined with IR repair (Case 2).
Overcorrections are rare, but have occurred in a few patients with aggressive healing responses. They respond well to a small recession of the involved muscle, but this should be delayed until a few months after primary repair to allow inflammation to subside and a mature scar to form.
Cases of horizontal strabismus due to flap tear may retain residual deviation due to shortening of the antagonist muscles, or residual tether of the involved muscles due to incomplete repair. Most of these cases come to surgery months to years following trauma, so length changes in antagonist muscles are expected. In exotropia cases, flap tear repair usually replaces the MR resection in the surgical plan, and reduces the amount of total LR recession required. The decision of how much recession to perform is based upon the spring-back and forced duction tests. 15 , 16
When restricted motility persists, a procedure to restrict motility of the fellow eye is possible (Chapter 33).
20.2.1.14 Long-term Stability
Statistical analysis of the long-term reoperation rates after flap tear repair as compared with standard strabismus surgery is not yet available, and probably will not be for at least 5 years. Ongoing data from all flap tear repairs are being collected for future analysis. It is the author’s impression that reoperation within the first year after flap tear repair is commonly required to achieve initial orthotropia and good motility, with about the same frequency as standard strabismus surgery. Once a good result is obtained, however, the results to date seem more stable than after standard strabismus surgery.
20.2.1.15 Myasthenia Gravis and Flap Tear
Myasthenia gravis is an autoimmune disorder in which neuromuscular transmission is impaired due to autoantibodies against the acetylcholine receptors. It may be systemic, but often primarily or exclusively affects the extraocular and/or levator muscles. Some, but not all, ocular myasthenic patients progress to systemic involvement. Additionally, although variability of strabismus, both in degree and in pattern, is the diagnostic hallmark of myasthenia, some patients are surprisingly stable. Their diplopia is often controllable with prisms, and responds well to standard strabismus surgery. 17 , 18 It is difficult to explain why stability would be present in any myasthenic patients, unless coexisting mechanical abnormalities were present. Additionally, pyridostigmine treatment, which is usually effective to treat systemic symptoms, has little effect on strabismus. 18 This feature also argues for an underlying mechanical defect.
One patient (Case 5) developed myasthenia gravis and strabismus recurrence 3.5 years following successfully repaired flap tears and full recovery of motility. The acquisition of myasthenia was test-proven because he tested negative at initial presentation, but then tested positive at 3.5 years. The strabismus due to myasthenia was not fully correctable by surgery. Ocular myasthenia has also been diagnosed in three other flap tear patients. Could exposure to eye muscle antigens by the injury, and again at subsequent repair, cause the antibody formation and secondary development of myasthenia? Could this explain the stability of alignment and favorable surgical outcomes in some? The concept of exposure of extraocular muscle to the patient’s circulation as a possible cause of ocular myasthenia, did not originate with this author. (Personal communication from Michael Kaminski, MD, Nashville, TN) If this supposition is correct, the natural extension of this reasoning would be to recommend the minimizing of direct muscle tissue trauma whenever possible during routine strabismus surgery.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


